1. Ectopic Pregnancy
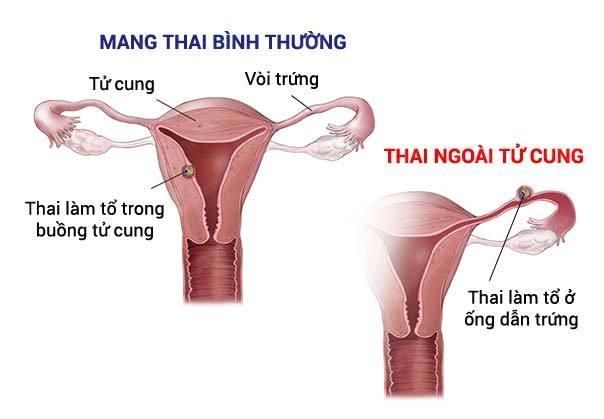
The normal uterus is where the fertilized egg implants and develops into a mature embryo. However, when women encounter issues such as blocked fallopian tubes, adherent ovaries, or narrow fallopian tubes, the fertilized egg may implant outside the uterus, like in the abdomen, the cervix, or inside the fallopian tubes, a condition known as ectopic pregnancy.
These organs cannot nurture the fetus or adjust its size appropriately for development, posing a significant risk. Rupture of the embryo or fallopian tubes, leading to internal bleeding into the abdomen, can occur at any time, threatening the mother's life.
Mothers with ectopic pregnancies may experience typical pregnancy symptoms such as delayed menstruation, abdominal pain, breast tenderness, and nausea. However, it's essential to be cautious of certain signs to distinguish whether one is experiencing an ectopic pregnancy:
- Vaginal bleeding: Many women notice light pink bleeding outside of their menstrual cycle, known as spotting. It's usually lighter in color and duration than normal menstrual bleeding and is rarely accompanied by abdominal pain. However, if bleeding occurs outside of the expected time and persists, appearing darker red, mothers should seek medical attention as it may indicate an ectopic pregnancy.
- Pregnancy symptoms accompanied by abdominal pain: If experiencing lower abdominal cramps, colicky pain resembling constipation, dull, lingering pain, or severe pain and noticing vaginal bleeding, it could be indicative of an ectopic pregnancy. The degree of pain is proportional to the development of the embryo.
- In severe cases, mothers may also experience intense pain, shoulder or arm aches, trembling limbs, sweating, dizziness, or fainting. When encountering these abnormalities, immediate medical attention is necessary. Delaying treatment for an ectopic pregnancy increases the risk as the fetus grows, causing the fallopian tube to rupture, resulting in widespread abdominal bleeding and endangering the mother's life.

2. Pregnancy with birth defects
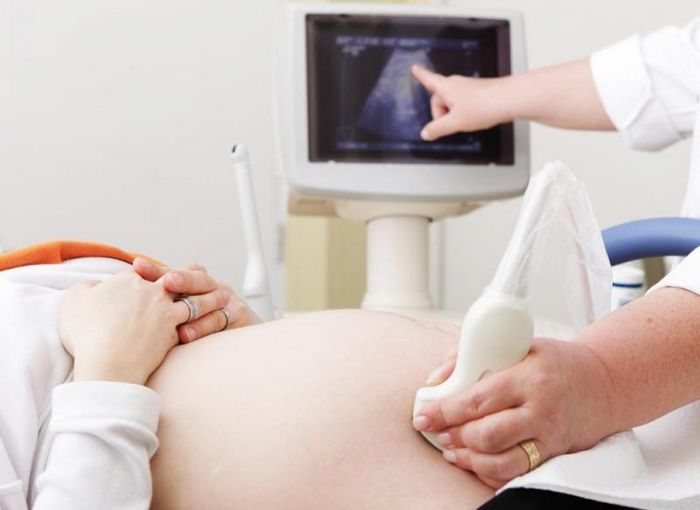
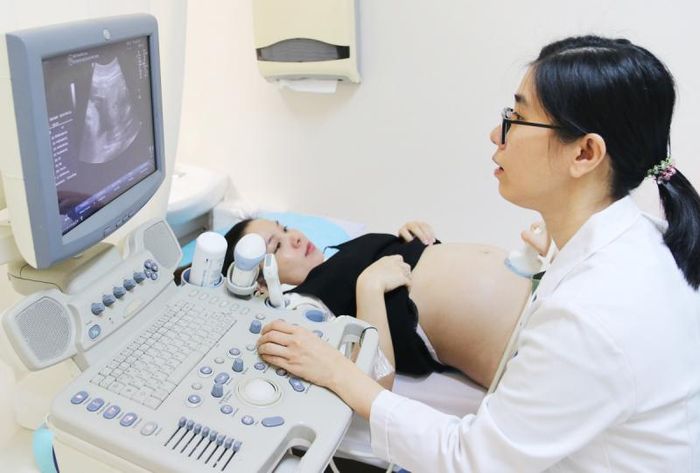
During pregnancy, mothers often worry if their baby will be normal like other babies. Most mothers fear birth defects. Fetal abnormalities are genetic or physical defects in the fetus that can affect pregnancy, childbirth, and have serious adverse effects on the baby when born. Ultrasound is an effective and simple way to detect fetal abnormalities. The current rate of fetal abnormalities in Vietnam is 3%, with the most common being defects in the nervous system, head, face, neck, chest, and abdomen.
Fetal abnormalities, if mild, can be easily corrected, but if severe, can lead to stillbirth or immediate death after birth. Some common fetal defects include Down syndrome, congenital heart defects, cleft lip, and cleft palate.
The causes of some fetal abnormalities may be difficult or impossible to determine. However, certain behaviors significantly increase the risk of fetal abnormalities, including smoking, using illegal drugs, and drinking alcohol during pregnancy. Exposure to toxic chemicals or viruses also increases the risk. Occasionally, one or both parents may pass on genetic abnormalities to their child. Genetic abnormalities occur when a gene becomes defective due to mutation or alteration. In some cases, a gene or part of a gene may be missing. These defects occur at conception and can often be prevented. A specific defect may be present in the family history of one or both parents.
To mitigate these risks, mothers should maintain a balanced diet, avoid stimulants and toxins, maintain good health, and consider genetic counseling and prenatal screening such as ultrasound, tests during sensitive periods are recommended. Ultrasound can help detect morphological abnormalities - what can be seen - but cannot diagnose functional disorders. Pre-birth tests can help determine whether the mother is infected or has other harmful conditions for the baby. Physical examinations and hearing tests can also help doctors diagnose congenital defects after the baby is born.

3. Missed Miscarriage
This is also a not uncommon occurrence during a woman's pregnancy. When the egg has been fertilized and transferred to the uterus but cannot develop into a mature fetus, it's called a missed miscarriage.
The causes leading to missed miscarriage are often due to maternal infection during pregnancy, abnormal uterus, inadequate nutrition, strenuous work, or chronic illnesses such as hypertension, liver and lung diseases, or anemia.
Pay attention to your body if you notice any abnormal vaginal discharge: You should not overlook any unusual vaginal discharge (discharge with odor and any color other than white), as it could be a sign of infection in the uterus. Infection can weaken the fetal membranes, cause intrauterine infection, or rupture your amniotic fluid.
Or signs of abnormalities such as mild to severe abdominal pain, dizziness, high fever, or the inability to detect a heartbeat. Or when ultrasound suddenly decreases fetal movements after 28 weeks or no movement at all. Typically, the fetal heartbeat begins around the fifth week of pregnancy, but it's only around the tenth week that detecting the fetal heartbeat becomes easier. Fetal heart rate monitoring can be performed using medical devices or by touching the mother's abdomen and counting the number of beats per minute.
Sometimes the task of detecting fetal heartbeats fails due to the baby changing positions or encountering problems with the umbilical cord. In such cases, your doctor may suggest checking the fetal heartbeat at the next prenatal visit. Alternatively, if fetal heartbeat detection remains unsuccessful, ultrasound testing may be conducted to find the cause. In some cases, no fetal heartbeat or weak heartbeat is a sign of fetal weakness or even missed miscarriage.

4. Fetal Macrosomia
Contrary to the condition of fetal growth restriction, fetal macrosomia is also encountered in quite a few cases. Most mothers assume that eating plenty of nutrients to help the baby grow quickly is beneficial, but in reality, this is not always true. Exceptional fetal development can be a warning sign of many health issues. A prime example is gestational diabetes in which increased insulin levels in the baby's blood lead to protein and fat accumulation in the baby's body, resulting in excessive growth.
Fetal macrosomia can complicate the mother's childbirth process. Moreover, after birth, the baby continues to produce insulin, leading to low blood sugar levels. If blood sugar levels drop too low, the childbirth process may be prolonged, leading to complications such as intellectual disabilities in the baby. Therefore, larger babies pose a greater risk rather than being a cause for celebration.


5. Fetal Intrauterine Growth Restriction
If an expectant mother ensures adequate nutrition and essential compounds daily but notices slow fetal development during ultrasound, failing to reach standard size, it's highly likely the fetus is encountering abnormal genetic issues, chromosomal abnormalities, or the mother is exposed to chemicals or suffers from a dangerous medical condition.
When mothers face this condition, complications such as shortness of breath, elevated blood sugar levels, and high body temperature may occur or even persist after delivery. Clearly, Intrauterine Growth Restriction (IUGR) is a prominent sign of fetal weakness. Hence, close monitoring of this condition is necessary.
Expectant mothers can proactively address fetal growth restriction by attending regular prenatal check-ups for medical advice, establishing a healthy, scientific, and effective maternity regimen.

6. Low HCG Levels
Within the mother's womb, the embryo is nourished through the placenta via the umbilical cord. The placenta acts as a metabolic exchange barrier between the mother's body and the fetus. Moreover, it serves an endocrine function by secreting regulatory hormones during pregnancy.
One of these hormones is HCG (Human Chorionic Gonadotropin). It's a peptide hormone secreted by the trophoblast cells, with the role of stimulating the embryonic stem cells to develop and mature. Additionally, HCG aids in stimulating the secretion of sex hormones, contributing to the fetal sexual differentiation.
HCG is an endocrine hormone produced by the placenta during pregnancy. Its concentration tends to fluctuate throughout the gestational period depending on the menstrual trimester. Typically, HCG levels peak between weeks 9 and 16 of gestation.
Normal levels vary from person to person, so low HCG levels are not necessarily a cause for alarm. However, miscarriage, blighted ovum, or ectopic pregnancy can result in low HCG levels, becoming a highly dangerous indicator of fetal distress.

7. Fetal Oxygen Deprivation
During pregnancy, the mother's blood volume must increase by half to nourish both herself and the baby. However, some expectant mothers encounter issues such as anemia. This is a common and often seen cause in pregnant women, which can lead to oxygen deprivation. Additionally, other factors such as high blood pressure, carbon monoxide poisoning, acute infections... can also cause the fetus to lack oxygen. Obstructions, short or twisted umbilical cords, or placental dysfunction can also lead to fetal oxygen deprivation...
Besides the mentioned factors, excessive tugging or pulling of the umbilical cord by the mother or being in an oxygen-deprived environment during pregnancy can also cause fetal oxygen deprivation. Depending on the degree of oxygen deprivation, it can affect the fetus to varying extents such as: low birth weight, premature birth, malnutrition... or more severely, delayed development.
To address this, expectant mothers should ensure a nutritious diet, take iron supplements as directed by their doctor, avoid smoking, and avoid exposure to coal smoke or kitchen fumes to ensure their health.
8. Abnormal Fetal Movement
Fetal movements within the mother's womb are indicative of life. Normally, a fetus will move about 3 times per hour, 10 times every 2 hours, and 30 times every 12 hours.
If within 12 hours you feel that the fetus moves less than 20 times, it indicates fetal oxygen deprivation; if less than 10 times, it signals a dangerous condition. Therefore, if the fetus is moving normally but suddenly reduces or stops moving altogether, it indicates fetal oxygen deprivation. This is a rather dangerous sign for your baby.
Because if you do not pay attention to your body and the interaction between you and your baby, it can be dangerous for your baby. Prolonged oxygen deprivation will affect the brain development of the fetus. Therefore, every day mothers should count the number of fetal movements in the morning, afternoon, and evening to monitor the fetal development.

9. Unchanged Uterine Height
During scheduled hospital check-ups, doctors will routinely examine the uterine height measurements. If the uterine height remains unchanged over an extended period, the mother must proceed to the next step to identify the cause.
In most cases, unchanged uterine height is due to fetal oxygen deprivation leading to slow development. Particularly after the 28th week of pregnancy, fetal growth rate accelerates significantly. If the mother's uterine height shows no change for 2 weeks, it signals a dangerous condition.


10. Contractions Occur in Stage 3
Contractions commonly occur in the late months of pregnancy and can be a sign of preterm labor. However, first-time mothers often confuse true contractions with false ones. False contractions are called Braxton-Hicks contractions. They are irregular, sudden, and do not increase in intensity. False contractions usually decrease within an hour. True contractions, on the other hand, typically recur every 10 minutes or less and gradually intensify.
Nevertheless, because the safety of both mother and baby is paramount, pregnant women should never dismiss contractions. In the final stage of pregnancy, whenever contractions appear or even feel like they are occurring, you must immediately call your doctor. If there are complications, doctors will promptly provide appropriate care for the pregnant woman.
In the last months of pregnancy, you should monitor more frequently if the doctor says your condition is prone to preterm labor. In reality, only the mother herself can truly sense her body. So, listen to your body.