1. Osteoporosis
Estrogen hormones play a crucial role in maintaining bone health. Osteoporosis is more commonly seen in women going through menopause. Studies show that women over 50 are most affected by joint inflammation and bone loss. During menopause, a woman's ovaries stop producing estrogen, which leads to a gradual reduction in bone mass. This results in a significant decrease in bone density, making bones weaker and more prone to fractures, even from minor injuries like twisting an ankle, falling, or bumping into something. The signs of osteoporosis often don't become noticeable until bone density decreases by over 30%. Symptoms may include:
Reduced bone density due to osteoporosis can lead to spinal compression fractures, which manifest as a hunchback posture, stooping, height loss, and acute back pain. Pain may also be felt along the long bones, especially in areas that bear the most weight, such as the hips, pelvis, and lower back. These pains tend to recur and worsen with movement, prolonged standing, sitting, or walking but may ease with rest. Pain in the lower spine or along the rib cage, affecting the intercostal nerves, sciatica, and thigh nerves, is common. Therefore, individuals with osteoporosis may find it difficult to perform movements like twisting their body or bending forward.


2. Increased Body Temperature
Perimenopause is the phase when the body begins the natural transition to menopause, marking the end of a woman's reproductive years. It is also referred to as the menopausal transition, during which the body stops ovulating, menstruation ceases, and fertility is lost. This stage typically occurs between the ages of 45 and 50 and may last anywhere from 2 to 5 years, depending on the individual. During menopause, a woman's body undergoes various changes, one of the most noticeable being a rapid rise in body temperature.
Sudden increases in body temperature are one of the most common symptoms of menopause. These temperature fluctuations can lead to dizziness, anxiety, palpitations, and sleep disturbances. Hot flashes may persist for an extended period, starting before menopause and continuing throughout the phase. A sudden feeling of heat, accompanied by sweating, is the most typical sign of perimenopause, and the intensity and duration of these hot flashes can vary throughout the day, even at night, often causing snoring and sleep difficulty. This sensation can last anywhere from 2 to 5 years. As estrogen levels decline, blood vessels may dilate quickly, causing skin temperature to rise. This can lead to a sensation of heat spreading from the chest to the shoulders, neck, and head. As sweat evaporates, it cools the body, causing chills, fatigue, and weakness. A hot flash can last anywhere from 30 seconds to 30 minutes.


3. Emotional Disturbances
Just like premenstrual syndrome (PMS) and pregnancy, hormonal changes during menopause can significantly affect a woman's mood. Estrogen and progesterone influence serotonin and other neurotransmitters that are linked to mood regulation. These drastic hormonal shifts can make menopausal women feel emotionally unstable. Research shows that around 20% of women experience feelings of depression during menopause. If a woman has previously struggled with depression, the likelihood of experiencing it again during this period increases.
Surprisingly, a desire to withdraw from social interactions is one of the common symptoms of menopause. If a woman is typically outgoing and enjoys socializing, she may suddenly feel the urge to spend time alone. Menopause is often viewed as a more introspective period, where women prefer solitude to navigate their emotional changes.


4. Hair Loss
Hair loss is a troublesome symptom for many women during menopause. It occurs due to hormonal imbalances, primarily the decrease in estrogen and progesterone levels. As these hormones decline, hair thins and grows more slowly. Meanwhile, an increase in male hormones called androgens, due to the reduction in female hormones, contributes to hair loss. Androgens shrink hair follicles, leading to more hair falling out.
Although hormonal imbalance is a key factor in hair loss during menopause, other factors also play a role, such as nutrient deficiencies, underlying health conditions like thyroid disease, and ongoing stress. To manage hair loss, it's important to reduce stress, maintain physical activity, follow a balanced diet, stay hydrated, and get enough rest.


5. Dry Skin
Most women enter menopause between the ages of 40 and 58. This marks the time when the ovaries stop releasing eggs, menstrual cycles end, and estrogen production begins to decline. Estrogen plays a crucial role in women's bodies, helping to regulate puberty, maintain strong bones, and promote collagen and natural oils in the skin. As menopause approaches, the reduction in estrogen leads to dry and itchy skin for many women.
The decrease in estrogen and hormonal imbalances slow down oil production in the skin and reduce the body's ability to retain moisture. The first areas where dry skin appears are typically the T-zone or elbows, but dryness or flaking can occur anywhere on the body—from the face, back, chest, and elbows to the legs, genital area, and even nails. These skin changes can start in the perimenopausal phase and may persist permanently. Understanding the root causes of dry skin during menopause can help you find effective solutions to alleviate these uncomfortable symptoms.


6. Increased Harmful Cholesterol
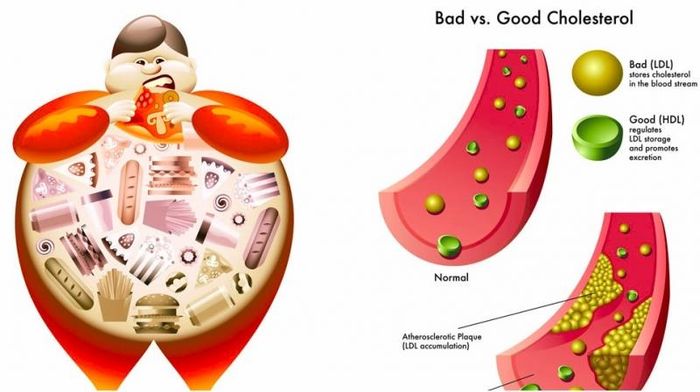
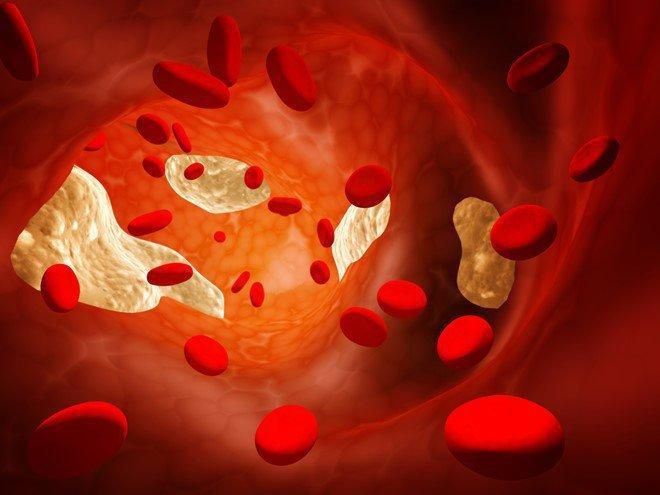
Estrogen not only regulates your menstrual cycle but also helps maintain proper levels of HDL and LDL cholesterol in the body. As estrogen levels decrease during menopause, LDL cholesterol starts to rise while HDL remains stable. This leads to an increase in harmful cholesterol levels, which can contribute to various heart-related conditions and obesity. Female hormones typically raise HDL-cholesterol, the 'good' cholesterol, which helps protect the cardiovascular system.
However, as estrogen production declines with menopause, lipid regulation becomes disrupted, increasing the risk of heart disease. Other factors, such as age and fat distribution in the body, also contribute to this change. Fat tends to accumulate in the abdominal area, particularly after menopause. Keep in mind that cholesterol levels tend to rise in women until around the age of 65, peaking between 48 and 56. Regular physical activity and a balanced diet can generally help control cholesterol levels.
7. Vaginal thinning, dryness, increased risk of urinary tract infections, and reduced libido
Menopause brings many uncomfortable changes to the vagina. In fact, the vagina is lined with a special type of skin tissue that consists of three layers, with the outermost layer being highly sensitive to estrogen. During the reproductive years, normal estrogen levels help keep the vaginal lining thick, well-lubricated, and elastic. However, as women enter menopause, estrogen levels decrease, causing the vaginal walls to become thinner, drier, and lose their elasticity and lubrication. This can lead to discomfort, itching, or even pain during sexual intercourse. Vaginal dryness can make intimacy difficult and painful, leading to a decrease in sexual desire or even a lack of interest in sexual activity. This can negatively affect marital relationships.
Additionally, women face an increased risk of other health issues, including gynecological infections, urinary tract infections, and discomfort in the genital area, which can lead to frequent urination, urgency, or incontinence. These changes can have a significant impact on a woman's mental health and daily life. Declining estrogen and testosterone levels after menopause can result in reduced sexual desire. During perimenopause and menopause, many women may find it harder to become aroused or responsive to sexual stimulation. Furthermore, low estrogen levels can impair blood flow to the vagina, exacerbating vaginal dryness.


8. Sleep disturbances
The first thing affected when you enter menopause is sleep. Due to hormonal changes and a decrease in estrogen and progesterone levels, sleep disturbances are common. Researchers suggest that there are three main factors that influence sleep during menopause. The first is mood swings leading to insomnia, the second is changes in breathing patterns, and the third is the development of muscle stiffness. The drop in estrogen during menopause contributes to both premenopausal and menopausal insomnia. This reduction causes symptoms such as hot flashes, sweating (vasomotor symptoms), anxiety, and mood changes, all of which negatively impact sleep quality.
Additionally, joint pain and bladder issues such as frequent nighttime urination are also common consequences of estrogen decline and can further disrupt sleep. The decrease in progesterone can also cause premenopausal insomnia, as progesterone has a sedative effect by influencing brain neurotransmitters. Melatonin, another important sleep hormone, also declines with age. The secretion of melatonin is partially influenced by the lack of estrogen and progesterone, which can worsen sleep disturbances during both perimenopause and menopause, leading to menopausal insomnia.


9. Memory loss
Previously, it was difficult to determine the extent of estrogen deficiency's impact on memory loss, particularly in those with mild cognitive impairment. The challenge was that most studies relied on women’s self-reports of mild memory symptoms, and memory loss can also be a natural part of aging. Therefore, it’s hard to pinpoint whether the memory issues are due to menopause or another cause.
However, recent research on estrogen’s effects on memory has provided evidence that the decline in estrogen during menopause contributes to memory loss. For example, a 2004 study on ovarian aging found that fluctuations in estrogen levels during perimenopause are a precursor to memory impairment. This was not simply due to the natural aging process. Another study lasting 4 years found that women in perimenopause had difficulty learning, but after menopause, their test results were similar to their performance before entering perimenopause.


10. Weight gain
Weight gain is a leading cause of increased risk for conditions like high blood pressure, heart disease, and diabetes. The accumulation of fat around the waist further compounds these risks. Unfortunately, women after menopause often experience a larger waistline. So, what happens during menopause that makes weight gain so easy? It could be a combination of menopause-related and aging factors. During perimenopause, progesterone levels decline gradually, while estrogen levels fluctuate dramatically from day to day or even within a single day.
In the early stages of perimenopause, the ovaries often produce an unusually high amount of estrogen. This is due to a weakened feedback loop between the ovaries, hypothalamus, and pituitary gland. Later, as perimenopause progresses and menstrual cycles become more irregular, the ovaries produce much less estrogen. Some studies suggest that higher estrogen levels can contribute to fat gain. This is evident from higher estrogen levels being linked to increased weight gain and higher body fat during reproductive years. From puberty to menopause, women tend to accumulate fat around the hips and thighs as subcutaneous fat. While it can be difficult to lose, this fat does not significantly increase the risk of other health issues.


