1. Early Signs of Kidney Failure
Common symptoms of kidney failure include:
- Oliguria or anuria: reduced urine output due to impaired kidney filtration. When the glomerular filtration rate (GFR) drops below 89 ml/min, urine output decreases. Below 15 ml/min, the patient experiences anuria.
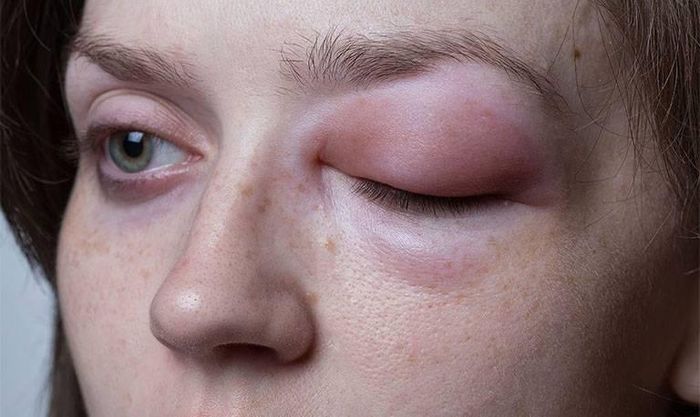
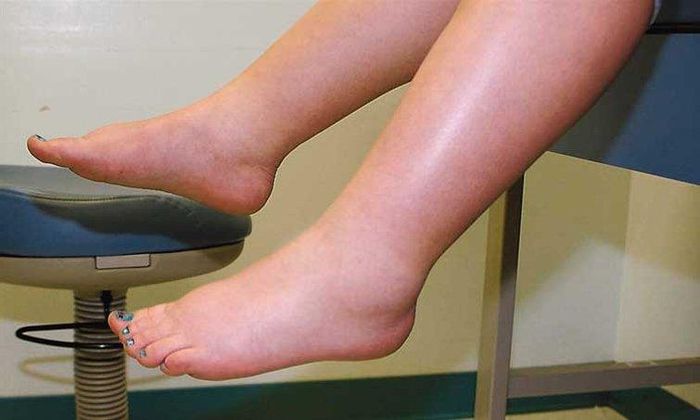
- Generalized edema: the degree of swelling varies by individual. Swelling primarily affects the lower limbs, with swelling on the feet and ankles extending up to the shins, knees, and groin area. The ankle bones and shins become less palpable, and pressing on the skin causes indentation, leaving a deep pit. Swelling can also be visible in the face and eyelids.
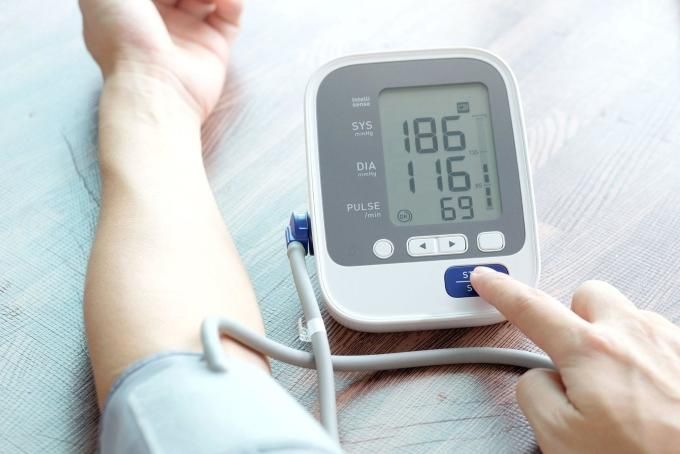
- High blood pressure: around 80% of kidney failure patients show signs of hypertension. Reduced blood flow to the kidneys stimulates the juxtaglomerular apparatus, activating the RAA system, leading to vasoconstriction and high blood pressure. Malignant hypertension can cause rapid kidney failure and death.
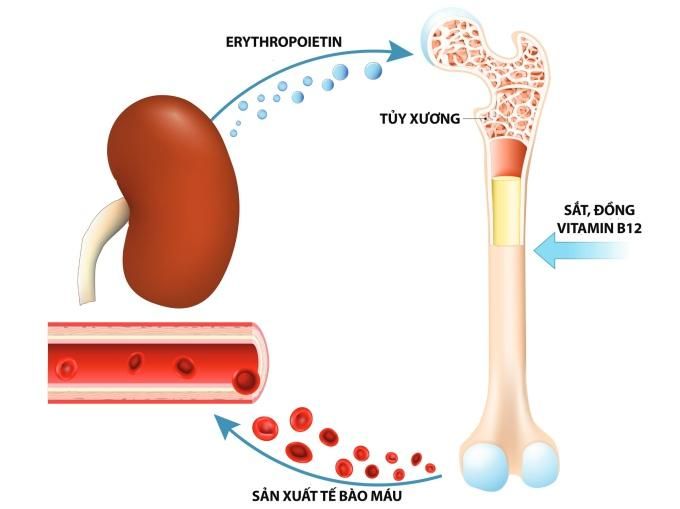
- Anemia: patients often feel fatigued, with pale skin and mucous membranes due to reduced erythropoietin production by the failing kidneys.
- Itching: a skin symptom of kidney failure due to calcium deposits in subcutaneous tissues.
- Loss of appetite, nausea, vomiting, and diarrhea.
- Bleeding: nosebleeds, gum bleeding, and gastrointestinal bleeding. Gastrointestinal bleeding can accelerate kidney failure.
- Cramps: caused by low calcium and sodium levels in the body.
- Tingling or burning sensations in the legs: a result of peripheral neuropathy caused by the disease.
- Osteodystrophy: vague bone pain, deep discomfort, pain episodes lasting weeks, and spontaneous fractures from minor trauma.
2. Complications of Kidney Failure
If left untreated or improperly managed, kidney failure can lead to several dangerous complications, including:
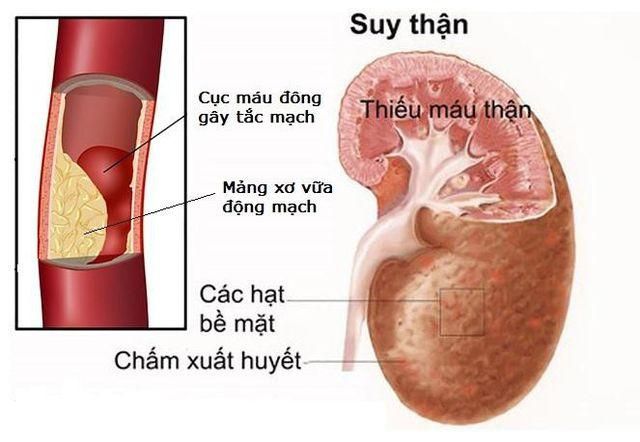
- Cerebrovascular accidents, brain hemorrhages, and myocardial infarction: High blood pressure from kidney failure puts excessive pressure on blood vessels, causing them to rupture or tear, which can form blood clots. These clots can travel through the bloodstream, blocking small vessels and causing strokes or heart attacks.
- Congestive heart failure, left ventricular hypertrophy: Kidney failure leads to metabolic imbalances in heart muscle cells, causing fluid buildup inside the cells. Over time, this makes it harder for the heart to contract. Kidney failure also leads to anemia, forcing the heart to work harder to supply oxygen to the tissues, eventually causing heart enlargement.
- Renal coma: The most severe complication. As kidney filtration decreases, waste products accumulate in the blood, leading to elevated ammonia levels. This can induce a coma and potentially result in death.
- Other complications may include: menstrual irregularities, decreased libido, glucose intolerance, and secondary hyperparathyroidism.

3. Diagnosing Kidney Failure
In medical facilities, doctors diagnose kidney failure not only by assessing clinical symptoms like fatigue, swelling, and decreased urination, but also by conducting diagnostic tests to ensure an accurate and clear diagnosis.
Key diagnostic tests and imaging methods for kidney failure include:
- Elevated serum creatinine levels sustained for over three months: Creatinine is a waste product normally excreted by the kidneys. When kidney function declines, creatinine accumulates in the bloodstream, and as kidney failure progresses, serum creatinine levels rise. Warning signs occur when creatinine levels exceed 1.2 mg/dL in women and 1.4 mg/dL in men.
- Glomerular filtration rate (GFR): This measures the amount of filtrate produced by the kidneys per minute. The average GFR is 90 ml/min or higher, but it tends to decrease with age. A GFR lower than 15 ml/min signals a high risk of kidney failure, requiring dialysis or a transplant.
- Increased blood urea nitrogen (BUN): Urea is a byproduct of ammonia metabolism in the kidneys. When kidney function is impaired, urea is not eliminated effectively, raising its levels in the blood. Normal BUN levels range from 2.5 to 7.5 mmol/L. Levels exceeding this threshold indicate impaired kidney function, and prolonged elevation may lead to kidney failure, potentially causing renal coma due to ammonia toxicity.
- Proteinuria: When the kidneys are damaged, the glomerular filtration membrane is compromised, allowing large protein molecules to leak into the urine. Proteinuria greater than g/24h is a red flag for kidney dysfunction and a potential sign of declining kidney function.
- Ultrasound: This imaging technique offers a detailed view of the kidneys to identify abnormalities in size, position, shape, or any unusual masses.
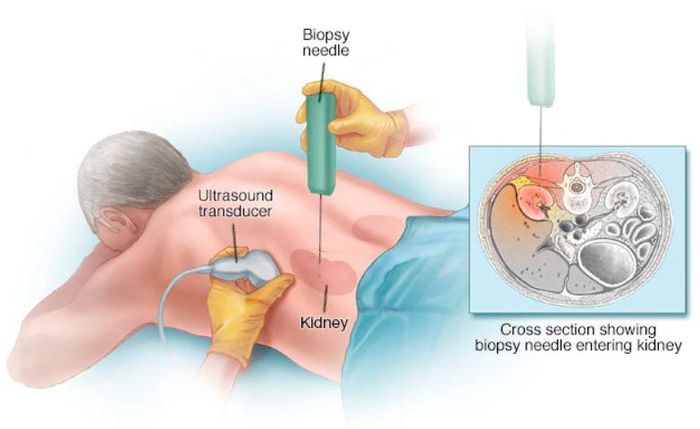
- Kidney biopsy: A biopsy helps determine the cause of kidney damage and assess its extent, providing crucial information for appropriate treatment strategies.

4. Treatment for Kidney Failure
Generally, the best treatment for kidney failure is conservative management with medications or replacement therapies such as dialysis or kidney transplantation. The treatment plan should be tailored based on the patient's condition and overall health.
For early-stage kidney failure, preventing further progression is crucial:
- Hypertension management: Kidney failure is often accompanied by high blood pressure. If untreated, this can worsen kidney damage and lead to other cardiovascular issues. Doctors may prescribe ACE inhibitors (Captopril, Enalapril) or AT1 receptor blockers (Losartan, Valsartan) to lower blood pressure while improving kidney function.
- Cholesterol control: A low-fat diet combined with statins can help reduce harmful cholesterol levels, preventing the buildup of plaque in blood vessels, which leads to atherosclerosis, blockages, and blood clots.
- Iron deficiency treatment: Patients will be prescribed iron supplements, essential amino acids, and micronutrients. In severe cases, intravenous EPO, iron, and renal protein may be required.
- Edema management: Diuretics help remove excess fluid through urine. Additionally, patients should reduce their salt intake and maintain proper hydration.
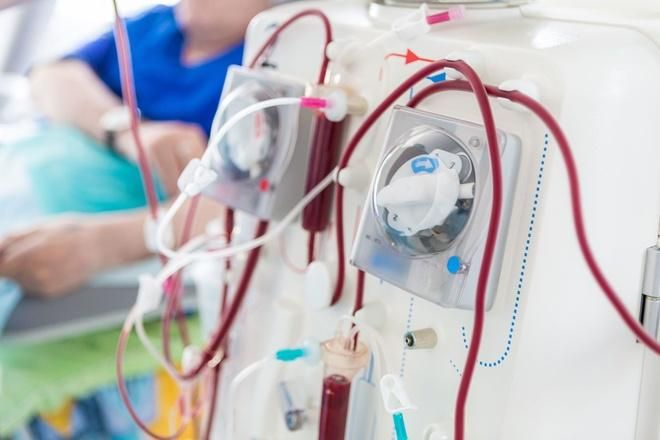
- Dialysis: When kidney function deteriorates, dialysis helps remove waste, water, and salts from the body, easing the burden on the kidneys and preventing complications.
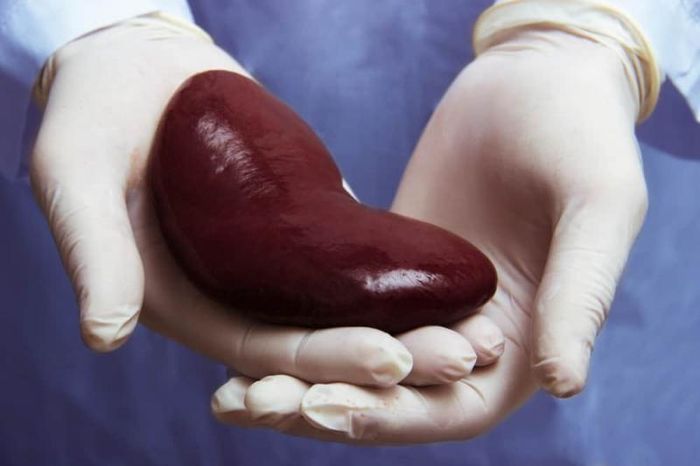
For patients with end-stage kidney failure, kidney transplantation is the only viable option to extend life. However, kidney transplants face significant challenges due to the scarcity of donors, and the success of the procedure depends on whether the patient's body accepts the new organ. Moreover, transplant costs are high, making it unaffordable for some patients.
5. Preventing Kidney Failure
Several preventive measures to reduce risk factors for kidney failure include:
- Managing blood sugar levels: High blood sugar can lead to atherosclerosis, causing blockages in the blood vessels supplying the kidneys, eventually leading to kidney failure. Regular exercise, a fiber-rich diet, and mindful carbohydrate intake are key preventive steps.
- Monitoring blood pressure regularly: For individuals with pre-existing hypertension or the elderly, maintaining stable blood pressure is crucial. A healthy lifestyle, adhering to prescribed antihypertensive medications, a diet rich in fruits and vegetables, avoiding alcohol, and quitting smoking are vital.
- Limiting salt intake: A salty diet increases fluid retention, raising blood pressure and putting excessive strain on the kidneys. The World Health Organization (WHO) recommends no more than 5g of salt per day, or 1.5g of sodium for those at risk of cardiovascular disease.
- Staying hydrated: Since nearly 70% of the body’s weight is water, hydration is essential for maintaining kidney function and overall bodily health. However, excessive water intake can dilute the blood and impair kidney function, so moderation is key. WHO suggests adults drink 35ml per kilogram of body weight daily.
- Avoiding smoking and excessive alcohol consumption: Long-term smoking and drinking can contribute to cardiovascular and liver diseases, which in turn affect kidney function. Reducing or eliminating alcohol and smoking helps prevent kidney damage.
- Maintaining a healthy lifestyle: Regular physical activity, sufficient sleep, and stress management, alongside a diet rich in fiber and adequate hydration, support overall health, including kidney health.
Additionally, any unusual health symptoms should prompt a visit to a healthcare facility for timely diagnosis. Most patients with acute kidney failure recover fully with proper treatment and rarely progress to chronic stages. Regular health check-ups are also recommended for early detection and timely intervention.

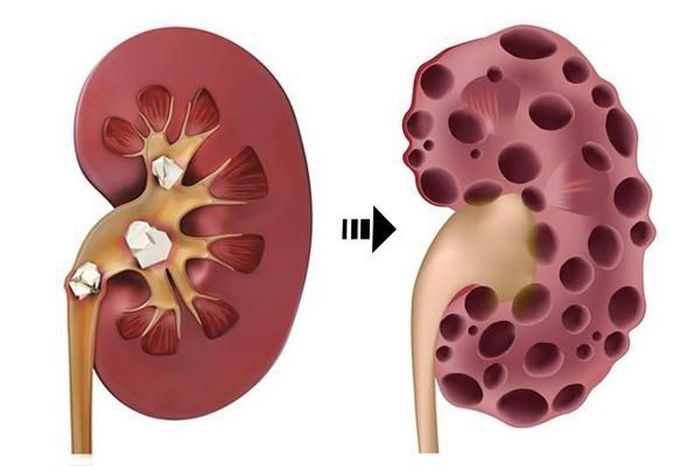
6. What is Kidney Failure?
Kidney failure, also known as renal insufficiency, is a condition in which kidney function deteriorates, leading to the loss of the kidneys' filtering ability. As a result, urine is not excreted, and waste products accumulate in the blood, causing systemic poisoning. This is the final stage of chronic kidney disease, and without dialysis or a kidney transplant, it is difficult for patients to survive.
There are two types of kidney failure:
- Acute: Kidney function rapidly declines over a few days or weeks, usually 1-3 weeks. This type can be fully reversible with prompt treatment, and rarely progresses to chronic failure. However, without timely intervention, patients can quickly lapse into a coma and die from systemic poisoning.
- Chronic: Kidney function gradually decreases over a long period, slowly worsening and becoming difficult to fully treat. The disease progresses in episodes, with increasing levels of toxins in the body. Prognosis is poor because the kidneys cannot recover.
7. Early Symptoms of Kidney Failure
Depending on whether the patient experiences acute or chronic kidney failure, the disease can progress through various stages. Symptoms and complications also develop at different stages. Specifically:
Acute kidney failure progresses through four stages:
- Stage 1: Within the first 24 hours, the patient may experience fatigue, nausea, vomiting, reduced or no urine output, chest pain, and difficulty breathing. With prompt and proper treatment, the patient can avoid progressing to stage 2.
- Stage 2: Symptoms worsen and become systemic, with possible fatal complications. Oliguria or anuria persists for 1-6 weeks. The urine becomes dark, and red blood cells may be present. The patient may experience widespread swelling, pulmonary edema, and congestive heart failure. Laboratory tests reveal elevated creatinine, urea, potassium levels, and metabolic acidosis.
- Stage 3: Urine production begins to resume after 5-7 days, with urine output gradually increasing from 200-300 ml/24h to 4-5 liters/24h. This excessive urine production can lead to dehydration, elevated urea, potassium levels, and electrolyte imbalances.
- Stage 4: The kidney function recovery phase, which can last from 2 to 6 weeks depending on the cause. The disease may fully recover without any lasting damage. Thanks to modern dialysis techniques, the recovery rate has significantly improved.
Chronic kidney failure progresses through five stages:
- Stage 1: The patient may not show noticeable symptoms or complications. The glomerular filtration rate (GFR) is slightly increased or stable (GFR > 90 ml/min). This stage is often unnoticed, discovered during routine health check-ups or testing for other conditions. Maintaining a healthy lifestyle and proper diet can help control and slow disease progression.
- Stage 2: Kidney function remains mildly impaired, but the GFR decreases (GFR: 60-89 ml/min), and protein may appear in the urine. There are clear signs of kidney damage. During this stage, the disease may flare up episodically. Symptoms include loss of appetite, mild anemia, nocturia, fatigue, and pain in the lower back.
- Stage 3: Kidney function deteriorates further (GFR: 30-53 ml/min), which is divided into stages 3A and 3B, with 3B indicating more severe damage. Symptoms such as swelling in the hands, feet, and eyelids, frequent urination at night, anemia, fatigue, and lower back pain become more noticeable. Dangerous complications may arise, including micro- or macroalbuminuria.
- Stage 4: The GFR drops to 15-29 ml/min, and symptoms become more pronounced, including anemia, pale skin, poor appetite, frequent urination, nausea, widespread swelling, and itching, often accompanied by headaches and joint pain. Without timely treatment, the patient may develop heart failure, diabetes, cerebral edema, and pulmonary edema. Early dialysis is essential.
- Stage 5: The most severe stage, with complete kidney failure (GFR < 15 ml/min). Urine production is severely impaired, leading to the accumulation of toxins in the bloodstream. The patient may experience acidosis, poisoning, especially affecting the cardiovascular, digestive, respiratory, nervous systems, and skin. Without dialysis or peritoneal dialysis, survival is unlikely. Kidney transplantation remains the most effective treatment, offering a chance of life for patients.
8. Causes of Kidney Failure
Kidney failure can be classified into two main types: acute kidney failure and chronic kidney failure, each with different underlying causes.
There are various ways to categorize the causes of kidney failure. Generally, acute kidney failure can be divided into:
- Pre-renal causes: Reduced blood flow to the kidneys, decreasing glomerular filtration pressure, leading to oliguria or anuria. These include severe blood loss, diarrhea, vomiting, severe burns, myocardial infarction, pericardial effusion compressing the heart, decompensated cirrhosis, and renal artery stenosis.
- Renal causes: Conditions such as rapidly progressive glomerulonephritis, proliferative glomerulonephritis, hemolysis, uremia, hemolytic uremic syndrome, preeclampsia, infections caused by bacteria and viruses (EBV, CMV, HIV), and adverse drug reactions (e.g., cyclosporine, amphotericin B, etc.)
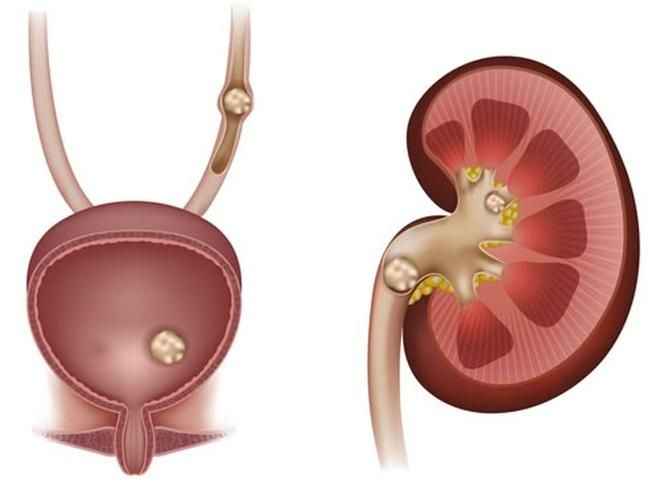
- Post-renal causes: Obstructions in the urinary tract, such as kidney stones in the ureters, bladder stones, bladder neck obstruction, urethral stricture, or tumors.
For chronic kidney failure, common causes include:
- Type 1 and Type 2 diabetes: Prolonged high blood sugar levels can damage the small blood vessels in the kidneys, impairing their filtration function.
- Atherosclerosis: Plaques of cholesterol buildup causing blood clots in the vessels, obstructing the blood supply to the kidneys, leading to ischemia and kidney dysfunction, which can eventually result in necrosis.
- Congenital urinary tract abnormalities: Blockages or congenital malformations in the kidneys.
- Urinary tract infections: Chronic infections can leave scarring, potentially causing kidney damage over time.
- Primary glomerulonephritis: Includes minimal change disease, membranous glomerulonephritis, and proliferative glomerulonephritis.
- Secondary glomerulonephritis: Conditions like IgA nephropathy, hepatitis B, systemic lupus erythematosus, vasculitis, diabetes, amyloidosis, multiple myeloma, and post-streptococcal glomerulonephritis.
- Excessive use of anti-inflammatory and analgesic medications (e.g., Ibuprofen, Naproxen, NSAIDs), or unregulated use of herbal remedies or traditional medicines.
- Progression from acute kidney failure to chronic kidney failure.