1. Symptoms of Cirrhosis
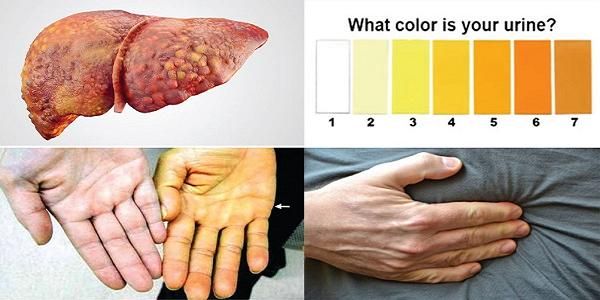
Individuals with cirrhosis may not always show symptoms, but when they do occur, they can be varied and not all happen simultaneously. Some common signs include:
- Loss of appetite
- Unexplained weight loss
- Fatigue
- Yellowing of the skin or eyes (jaundice)
- Itchy skin
- Signs of gastrointestinal bleeding (such as vomiting blood or passing black or blood-tinged stools)
- Abdominal swelling (due to ascites, where fluid accumulates in the abdominal cavity)
- Cognitive changes such as confusion, drowsiness, or even coma (caused by a condition known as hepatic encephalopathy)
- Severe muscle cramps
- Abnormal vaginal bleeding or prolonged menstrual cycles (in women)
- Impotence, infertility, or loss of sexual desire (in men)
- Development of enlarged breasts in men
- Varicose veins and spider veins on the chest and abdomen
2. Complications of Cirrhosis
Cirrhosis can lead to several severe complications, including:
- Portal Hypertension: The portal vein carries blood from organs like the stomach, intestines, pancreas, and spleen to the liver. Cirrhosis can increase pressure in this vein, potentially causing digestive bleeding and even death.
- Ascites and Edema: Increased portal pressure and low blood protein levels can cause fluid buildup in the abdomen (ascites) and legs (edema). Medication and a low-salt diet can help manage this condition.
- Infections: Cirrhosis patients often struggle to fight infections. Chronic ascites can lead to spontaneous bacterial peritonitis, a severe infection marked by fever, abdominal pain, diarrhea, and vomiting. Early medical attention is crucial when these symptoms arise.
- Hepatorenal Syndrome (HRS): In cirrhosis patients with ascites, kidney failure may occur, presenting as fatigue, nausea, vomiting, enlarged spleen, muscle wasting, muscle spasms, spider veins, and reduced urine output. Without timely intervention, this condition can be fatal.
- Hepatopulmonary Syndrome (HPS): This dangerous complication combines liver disease, dilated blood vessels in the lungs, and impaired gas exchange. Symptoms include shortness of breath and oxygen deficiency, which worsens when the patient stands. HPS significantly increases the risk of death.
- Bone and Joint Issues: Some cirrhosis patients experience weakened bones and have an elevated risk of fractures.
- Liver Cancer: Cirrhosis is a leading cause of liver cancer, which has the highest incidence and mortality rates in Vietnam, according to the 2020 Globocan statistics. Unfortunately, liver cancer often shows no symptoms in its early stages, and many patients are unaware until they undergo routine check-ups or abdominal ultrasounds.

3. Diagnosing Cirrhosis
Diagnosing cirrhosis involves considering several factors such as medical history, clinical examination, and laboratory tests. A liver biopsy remains the gold standard for diagnosis.
Medical and Family History: Key questions include whether the patient regularly consumes alcohol, has a previous liver condition, or uses medications frequently. Family history is also crucial, particularly for hereditary liver diseases or if there’s a history of chronic hepatitis B or C.
Clinical Symptoms: Symptoms may be categorized as compensated or decompensated cirrhosis.
Laboratory Tests:
- Complete Blood Count (CBC): Early stages may show normal results, but long-term alcohol users may have anemia. In decompensated cirrhosis, platelet counts are often low. In cases of infection, white blood cell counts will be elevated, particularly neutrophils.
- Coagulation Tests: In early stages, coagulation profiles may remain normal. Later stages typically show a reduced prothrombin ratio, prolonged APTT, and low fibrinogen.
- Biochemical Tests: As liver function declines, albumin levels drop, A/G ratio decreases, AST, ALT, GGT levels rise, and bilirubin increases, especially in severe bile duct obstruction. Elevated NH3 levels, glucose metabolism disorders, and electrolyte imbalances are common, with kidney dysfunction marked by rising urea and creatinine levels. Alpha-fetoprotein may increase, particularly in cases of liver cancer.
- Diagnostic Tests for Underlying Causes: Chronic hepatitis B and C markers are routinely tested. Chronic hepatitis B typically shows a positive HBsAg, high HBcAg, and elevated HBV DNA levels. Chronic hepatitis C often reveals a positive HCV Core Ag, HCV RNA, and HCV Ab. For parasitic liver diseases, tests for liver flukes may be positive. Wilson's disease shows elevated Cu2+ levels in blood and urine, while decreased ceruloplasmin is noted in the serum.
- Imaging and Functional Tests:
- Abdominal Ultrasound: It can reveal various liver abnormalities such as increased liver echogenicity, coarse liver texture, or even liver shrinkage in advanced stages. A liver tumor may appear as an irregular mass with a non-uniform texture.
- CT or MRI Scans: These imaging methods are more accurate than ultrasound in assessing liver damage, especially when MRI is used to evaluate bile duct abnormalities.
- Endoscopic Retrograde Cholangiopancreatography (ERCP): Indicated to assess bile duct diseases.
- Endoscopy: Helps detect and assess esophageal varices or gastrointestinal bleeding.
- Fibroscan: A non-invasive method to measure liver stiffness, indicating the extent of cirrhosis (F0 to F4). However, certain conditions like severe jaundice may affect the accuracy of the results.
- Liver Biopsy: This invasive procedure, though difficult to perform in all medical facilities, remains the definitive method for diagnosing cirrhosis or liver cancer.

4. Treatment for Cirrhosis
Treatment Principles: The treatment focuses on addressing the underlying cause of cirrhosis when possible, improving liver function, preventing complications, and managing any existing complications.
Treating the Cause: Cirrhosis caused by viral hepatitis (such as chronic hepatitis B or C) may benefit from antiviral medications (e.g., tenofovir, entecavir for hepatitis B, and sofosbuvir, ribavirin for hepatitis C). For alcohol-related cirrhosis, the key treatment is abstinence from alcohol.
Supporting Liver Function: In decompensated cirrhosis, patients should rest and follow a nutrition plan that ensures sufficient energy and protein intake. Fresh fruits, vitamins, and essential amino acids should be included. For ascites, salt intake should be minimized, and blood transfusions (e.g., fresh frozen plasma) may be required. Medications such as diuretics or liver cell protectants can be prescribed to improve liver function and fluid balance.
Preventing and Treating Complications:
- Ascites and Edema: Patients should reduce salt intake (low-sodium diet) and may be prescribed diuretics (e.g., furosemide, spironolactone). In more severe cases, paracentesis may be needed, or a transjugular intrahepatic portosystemic shunt (TIPS) may be considered to reduce portal pressure.
- Reducing Portal Pressure: Medications to lower portal hypertension and prevent esophageal varices bleeding may be used. Endoscopic banding or sclerotherapy may be recommended for variceal bleeding.
- Treating Infections: Cirrhosis patients are at higher risk of infections, including ascitic fluid infections, pneumonia, and sepsis. Empirical broad-spectrum antibiotics are often prescribed until cultures are available.
- Hepatic Encephalopathy: Treatment includes lactulose to reduce NH3 levels, along with medications to manage brain swelling, and in some cases, plasma exchange therapy.
- Liver Cancer Treatment: Options include transarterial chemoembolization (TACE), surgical resection, or chemotherapy.
Liver Transplantation: A liver transplant is the most effective treatment for end-stage cirrhosis. However, finding a suitable donor remains a major challenge.
5. Preventing Cirrhosis
Cirrhosis is difficult to cure completely, but it is highly preventable with simple lifestyle changes. To reduce the risk of liver fibrosis, consider adopting a healthy diet, good habits, and proactively avoiding potential causes of cirrhosis:
- Limit alcohol consumption: Control the amount and frequency of alcohol intake to avoid liver damage. For those with existing liver conditions, complete alcohol abstinence is necessary.
- Follow a balanced diet: Include plenty of vegetables, fruits, protein-rich foods, and whole grains while limiting fats and cutting down on salt. Always eat cooked food, avoid raw shellfish, which can carry harmful bacteria and parasites.
- Maintain a healthy weight.
- Exercise regularly.
- Have regular health check-ups.
- Quit smoking.
- Avoid high-risk behaviors that could lead to hepatitis B or C infections, such as drug injections or unprotected sex.
- Get vaccinated against hepatitis A and B, especially hepatitis B.
- Get the annual flu shot and consider vaccination against pneumonia.
- Follow your doctor’s instructions when taking medication. Overusing or incorrectly dosing drugs can negatively impact your liver.
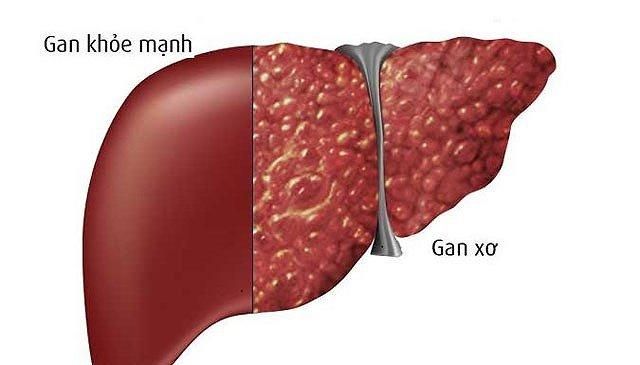
6. What is Cirrhosis?
Cirrhosis is the advanced stage of liver fibrosis (scarring), resulting from various factors like viral hepatitis and chronic alcohol abuse. The liver attempts to heal itself after each injury, but the healing process forms scar tissue. The longer the liver is damaged, the more scar tissue accumulates.
This scarring disrupts normal liver function. Scar tissue impedes blood flow through the liver, slowing down the liver's ability to process nutrients, hormones, medications, and toxins. It also reduces the liver’s production of proteins and other essential substances. In its final stages, cirrhosis can be life-threatening.
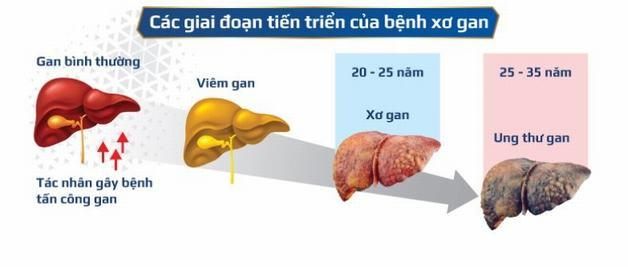
7. Stages of Cirrhosis
Stage 1
At this stage, there are no obvious signs of liver damage. However, inflammation of the liver has already begun. The liver attempts to reverse this process by forming scar tissue. Patients may feel tired and lack energy, but it can be difficult to pinpoint what’s happening to the liver. Although the liver is damaged, there are no significant symptoms, as fibrosis is still minimal. If treated properly, the liver can recover and return to normal.
Stage 2
At this point, portal hypertension (increased blood pressure in the liver) starts to develop, and more fibrous tissue appears. The cause of the damage must be addressed to improve the chances of recovery.
Stage 3
In stage 3, ascites (fluid accumulation in the abdomen) occurs. This signals severe cirrhosis. The liver can no longer return to normal, and a liver transplant is often recommended for a cure. Common symptoms at this stage include: loss of appetite, rapid weight loss, fatigue, confusion, yellowed skin and eyes, pale skin, rapid breathing, unhealing skin rashes, eczema, fluctuating blood sugar, swelling of the feet and ankles, and other signs of advanced cirrhosis.
Stage 4
By stage 4, cirrhosis is complete. Complications such as gastrointestinal bleeding, hepatic encephalopathy, and portal hypertension may occur. If these signs aren’t detected, the patient may not be eligible for a liver transplant. Life expectancy at this stage is typically around 12 months. Symptoms include: mental fatigue, excessive sleepiness, redness of the palms, personality changes, kidney failure leading to oliguria (low urine output), high fever, and peritonitis.
As there is no treatment for cirrhosis at stage 4, early intervention is the best approach.
8. Causes of Cirrhosis
Anything that damages the liver can lead to cirrhosis. The most common causes are viral hepatitis and prolonged alcohol abuse.
Viral Hepatitis
Chronic viral hepatitis is the leading cause of cirrhosis in Vietnam. Specifically, Hepatitis B and C can progress to cirrhosis and liver cancer. Currently, the prevalence of Hepatitis B and C in Vietnam is very high, with about 10 million cases of Hepatitis B and 1 million cases of Hepatitis C.
Alcohol-induced Cirrhosis
Alcohol abuse is one of the leading causes of cirrhosis. With the widespread alcohol consumption culture in Vietnam, alcohol has historically been the most common cause of cirrhosis. When consumed, alcohol gradually damages liver cells. Initially, alcohol can lead to fatty liver, followed by chronic hepatitis, and eventually cirrhosis.
Other Causes of Cirrhosis
- Non-alcoholic fatty liver disease: A condition linked to obesity, fatty liver, and type 2 diabetes.
- Autoimmune hepatitis: A condition where the body’s immune system attacks healthy liver tissue, causing damage.
- Drug abuse, including prescription and over-the-counter medications (acetaminophen, antibiotics, and certain antidepressants) can lead to cirrhosis.
- Cirrhosis caused by parasitic infections: Amoebas, malaria parasites, and liver flukes are common parasites that can cause liver damage and lead to cirrhosis.
- Certain genetic conditions: Wilson's disease, alpha-1 antitrypsin deficiency, hemochromatosis, Alagille syndrome, and glycogen storage diseases can cause cirrhosis.
- Cirrhosis caused by bile duct damage or obstruction: Conditions like cholangitis, bile duct obstruction, and bile duct cancer can lead to cirrhosis.
- Cirrhosis due to long-term blood congestion: Conditions like heart failure and hepatic vein thrombosis can result in cirrhosis.

