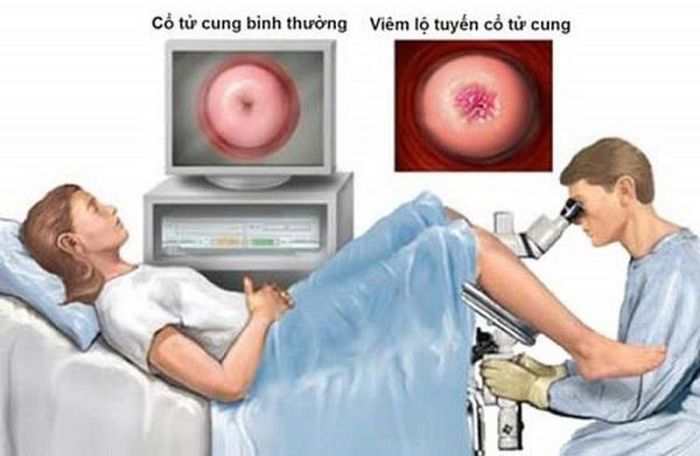
1. What is Cervical Gland Inflammation?
Cervical gland inflammation is a benign condition caused by glandular cells within the cervical canal expanding and invading the outer surface of the cervix, leading to cervical damage. These glands secrete mucus and are located beneath the cervical epithelium, which becomes exposed and infected by bacteria, fungi, viruses, or parasites.
Since the glands continue to secrete fluid outside the cervix as they do inside, patients often experience increased vaginal discharge, leading to infection (known as glandular inflammation). The disease is common in sexually active women, those of childbearing age, or postpartum women. However, some cases are congenital.
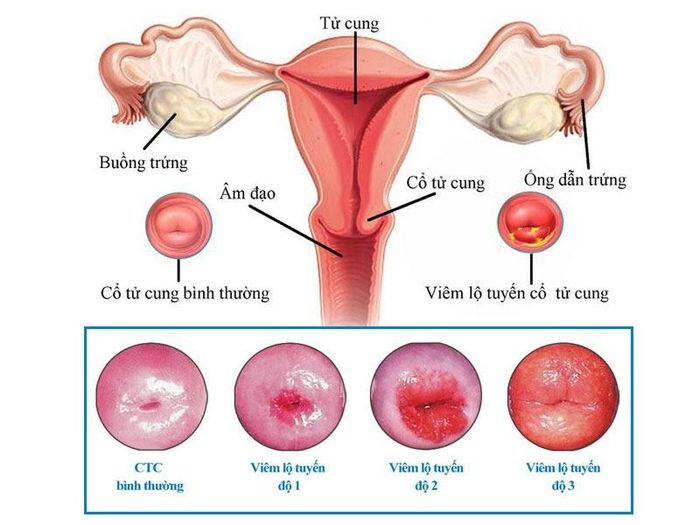
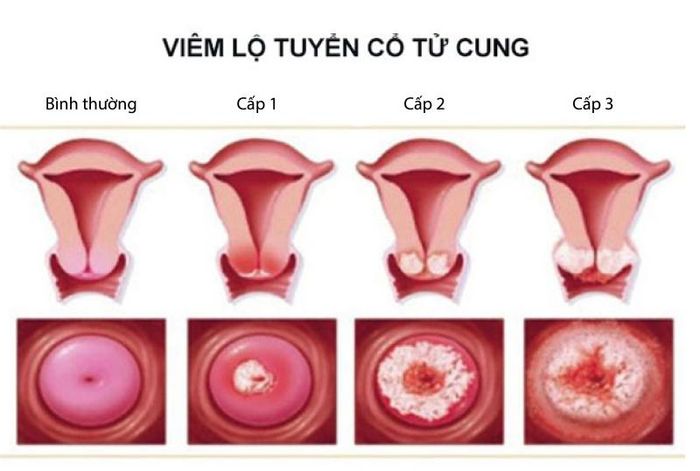
The disease is divided into 3 levels as follows:
- Level 1: Glandular cells in the cervix are just beginning to protrude outward, with a small area of damage, not exceeding 30%. Inflammation has not spread widely, and daily activities and sexual intercourse are not affected.
- Level 2: The damaged area of the cervix has spread to about 50-70%. Early examination and treatment are the only ways to prevent dangerous complications.
- Level 3: The area of cervical damage has spread to more than 70% of the area. Symptoms worsen, and the risk of dangerous complications increases, requiring immediate intervention.
2. Symptoms of Cervical Gland Inflammation
Cervical gland inflammation manifests differently depending on the progression of the disease.
Level 1 Cervical Gland Inflammation
In the initial stage, glandular inflammation may not be clearly evident, often leading to confusion with other gynecological conditions. Some typical signs include:
- Unusual vaginal discharge, initially cloudy white and later turning slightly yellow. It has an unpleasant fishy odor, with possible foamy discharge.
- Severe itching around the genital area, vulva, and vagina.
Level 2 Cervical Gland Inflammation
If glandular inflammation is not promptly controlled, it quickly progresses to a more severe stage (level 2). At this point, the area of glandular inflammation on the surface of the cervix has increased to 70%, resulting in several symptoms such as:
- More intense genital itching, with abnormal vaginal discharge.
- Foul-smelling vaginal discharge and increased genital odor.
- Increased watery vaginal discharge, leading to constant vaginal wetness.
- Vaginal pain during sexual intercourse.
- Deep vaginal and cervical pain during intercourse.
Level 3 Cervical Gland Inflammation
This is the most severe stage of cervical gland inflammation, which not only affects genital health but also impacts mental and overall physical health. It can cause more severe and dangerous symptoms such as:
- Increased vaginal discharge, turning greenish-yellow with a foul odor.
- Vaginal bleeding even outside of the menstrual cycle.
- Vaginal pain and bleeding during sexual intercourse.
- Lower abdominal cramping, which may be mistaken for menstrual cramps.
- Prolonged fatigue, weakness, and decreased libido.
3. Causes of Cervical Gland Inflammation
Some primary causes include:
Female Hormonal Imbalance: Fluctuations in female hormones greatly affect the body. Imbalance in estrogen hormone weakens genital health, causing the protective barrier to collapse and allowing bacteria, fungi, and parasites to thrive.
Vaginal pH Imbalance: Many women use vaginal cleansers containing strong detergents, deep vaginal douching, or have a high dose of antibiotics or long-term contraceptives. These factors can disrupt the vaginal pH balance, creating conditions for bacterial overgrowth.
Cervical Trauma: Using condoms during intercourse, using sex toys, or contraceptive devices can cause certain injuries to the cervix, leading to irritation and localized inflammation.
Unsafe, Repeated Abortions: Repeated surgical interventions in the genital area, especially repeated abortions or miscarriages, make the cervix less elastic, more prone to damage, and susceptible to bacterial attack.
Sexually Transmitted Infections (STIs): Dangerous sexually transmitted diseases such as syphilis, gonorrhea, genital herpes, etc., can cause complications and progress to glandular inflammation.
In addition to the main causes mentioned above, glandular inflammation can also occur in women who engage in sexual activity too early or with multiple partners. Women who have given birth multiple times are also at a higher risk of glandular inflammation.