When the inner lining of blood vessels is damaged, blood clots form as platelets stick together to create a blockage in the vessel wall. The body then releases chemicals that activate clotting factors. Normally, this is a healthy response to prevent excessive bleeding while the body repairs itself and restores normal circulatory function. The clots naturally dissolve once the injury heals. However, sometimes clots do not dissolve on their own or form unnecessarily. In such cases, they can partially or completely block blood flow, posing life-threatening risks.
Recognizing Blood Clot Symptoms
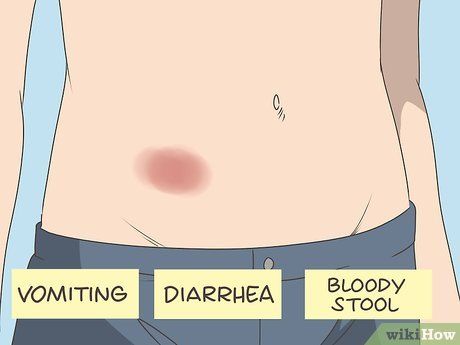
Be aware that blood clots in the abdominal area can cause severe pain and digestive issues. Symptoms vary depending on the clot's location in the body. If a clot forms in the artery responsible for blood supply to the intestines, symptoms may include intense abdominal pain. Additionally, you may notice the following symptoms:
- Vomiting. Abdominal clots irritate the stomach lining, prompting the body to vomit.
- Diarrhea. Reduced blood supply alters digestive function, often leading to diarrhea.
- Blood in stool. Any irritation to the digestive lining can cause bleeding, resulting in blood during bowel movements.
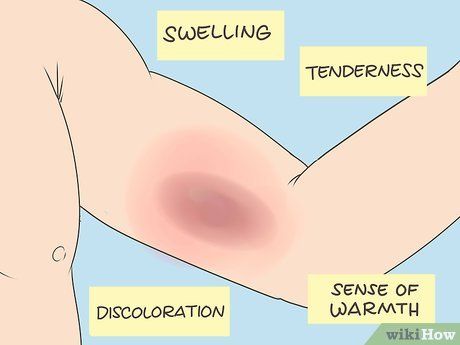
Understand that blood clots in the limbs can cause pain, swelling, and other noticeable symptoms. Clots in the arms or legs can block blood flow back to the heart, leading to conditions like phlebitis. Sudden, sharp pain may occur due to oxygen deprivation from reduced blood supply. Additionally, you might experience:
- Swelling. Blocked veins cause fluid retention and swelling in the affected area.
- Pain. Beyond sharp pain, you may feel discomfort or aching due to inflammation.
- Discoloration. Restricted blood flow can cause bruising or redness in the affected limb.
- Warmth. Inflammation increases blood flow to the area, bringing warmth from the body's core to the injury site.
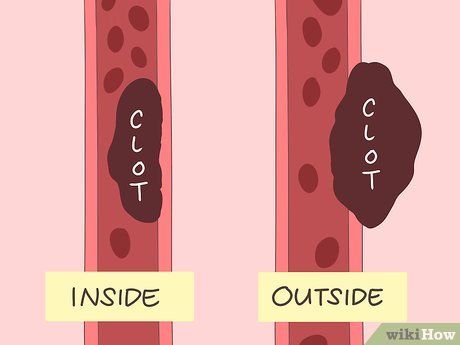
Recognize that blood clots can form inside or outside arteries or veins. When inside blood vessels, clots can partially or fully block blood flow or break loose, causing complications like strokes, pulmonary embolisms, or heart attacks. Clots outside blood vessels can still obstruct circulation by compressing nearby vessels.
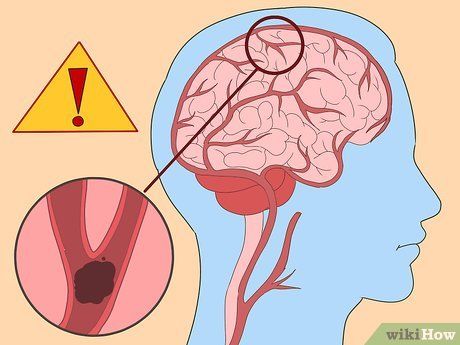
Note that blood clots in the brain can lead to severe symptoms. The brain controls bodily functions, and clots blocking blood flow can affect vision, speech, and nearly all other functions, potentially causing a
stroke. Symptoms may include:
- Vision problems
- Weakness
- Paralysis
- Seizures
- Loss of speech
- Disorientation

Understand that chest pain, shortness of breath, and sweating may indicate a blood clot in the heart. Clots in the heart can disrupt heart rhythm and block blood flow, causing chest pain (which may radiate to the arm, back, neck, or jaw), rapid breathing, and sweating.
- Such clots can lead to life-threatening conditions like heart attacks.
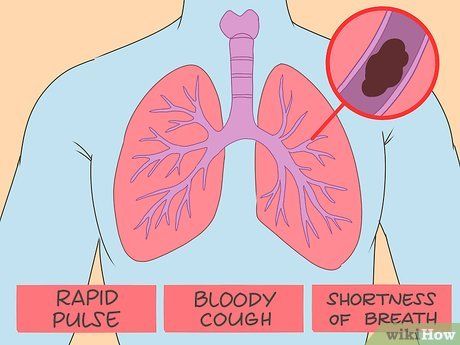
Know that blood clots in the lungs can cause chest pain and other symptoms. Similar to heart clots, lung clots often cause sharp, intense chest pain that may spread to the arm, back, neck, or jaw. Other symptoms include:
- Rapid pulse. The heart compensates by beating faster to supply enough blood.
- Coughing up blood. Clots can irritate the lungs, causing bleeding.
- Rapid breathing. Clots can block airflow, leading to difficulty breathing.
Understanding the Causes of Blood Clots
Be aware of the risks associated with prolonged immobility. Blood clots can sometimes form without a clear cause, but certain factors and situations increase the risk. Prolonged immobility is a primary factor. Remaining in bed or sitting with crossed legs for extended periods raises the likelihood of clot formation, especially in the arms and legs.
- Long-distance travel by plane or car can significantly restrict muscle movement, increasing the risk of clots forming in the veins.
Note the heightened risks during pregnancy and postpartum. In pregnant women, the expanding uterus slows blood circulation back to the heart, increasing the risk of clot formation, particularly in the legs and pelvic area. Women who have recently given birth also remain at high risk.

Understand that dehydration can contribute to blood clots. Proper hydration is essential for efficient blood circulation. Dehydration thickens the blood, making it easier for clots to form.
Recognize the risks of hormone therapy and contraceptives. Hormones like estrogen and progesterone can increase clotting factors, raising the risk of blood clots. Hormonal contraceptives (such as birth control pills) and hormone replacement therapy introduce these hormones into the body.
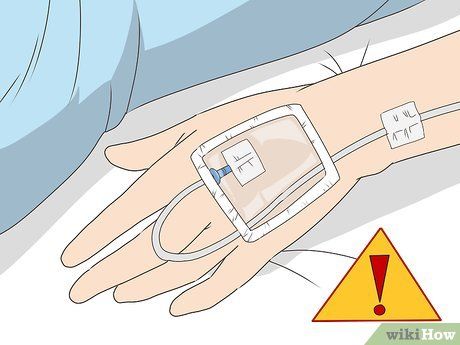
Understand that prolonged use of intravenous catheters can lead to blood clots. Intravenous catheters are foreign objects to the body. When inserted into veins, they can disrupt blood circulation, increasing the risk of clot formation.
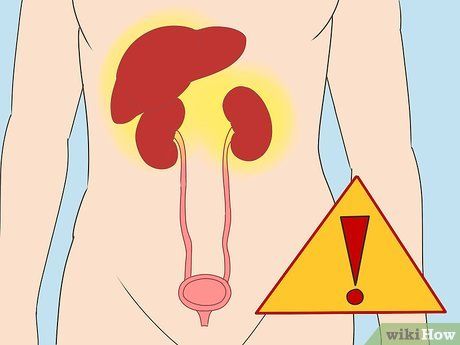
Remember that certain medical conditions can cause blood clots. Some diseases can irritate the bladder lining, leading to bleeding and clot formation, which may then be expelled through urine. These conditions include:
- Cancer
- Liver disease
- Kidney disease
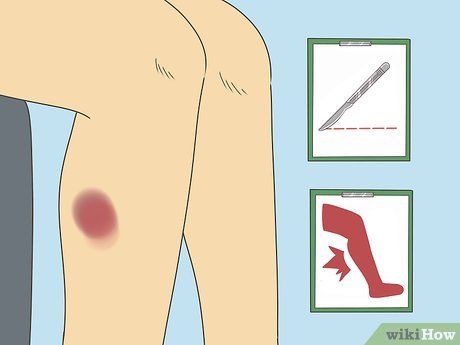
Consider the impact of recent surgeries or injuries. When the body is injured due to trauma or surgery, excessive bleeding (and clotting) can occur. Additionally, prolonged bed rest after surgery or injury increases the risk of clot formation.

Know that obesity increases the risk. Individuals who are significantly overweight or obese often accumulate cholesterol in their bodies, leading to narrowed arteries and an increased likelihood of clot formation.

Recognize the risks associated with smoking. Smoking can cause plaque buildup in blood vessels, narrowing them and contributing to the formation of blood clots.
Family history considerations. A personal or family history of blood clotting disorders significantly increases your risk of developing blood clots. These disorders can lead to narrowed blood vessels or reduced natural anticoagulant capabilities, both of which contribute to clot formation.
Diagnosing blood clots
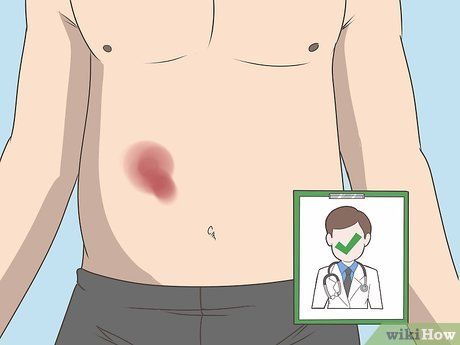
Seek immediate medical attention. If you experience symptoms of a blood clot, it is crucial to seek medical care promptly. Blood clots can lead to severe and life-threatening conditions.

Provide your doctor with a complete health history. Your doctor will inquire about your symptoms, lifestyle, personal medical history, and family medical history. Providing detailed information will aid in a quicker and more accurate diagnosis.
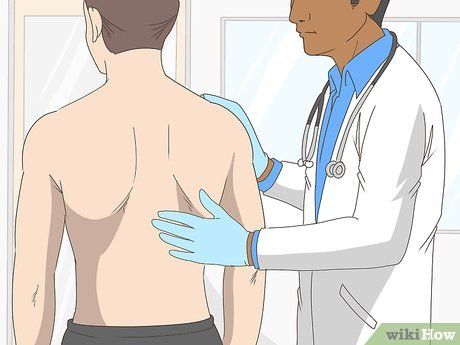
Physical examination. Your doctor will conduct a thorough physical exam to identify any signs or symptoms indicating the presence of a blood clot.
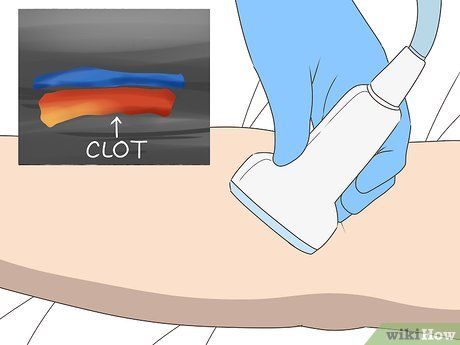
Follow the tests prescribed by your doctor. Based on your symptoms, your doctor will likely recommend a comprehensive blood test and other diagnostic procedures to detect blood clotting issues. Additionally, they may request:
- Ultrasound. Using ultrasound technology, doctors can identify blood clots within your vessels.
- Venography. During this procedure, a contrast dye is injected into a small vein in your hand or foot. Fluoroscopy allows the doctor to track the dye's movement and locate any clots.
- Arteriography. Here, the dye is injected directly into an artery. Similar to venography, this method helps doctors visualize the dye's path and confirm the presence of clots.
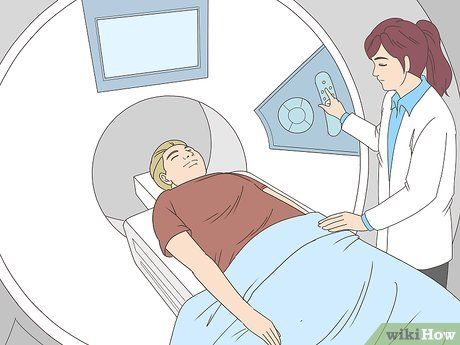
Imaging tests and/or lung blood flow and air tests. If a pulmonary embolism (a blood clot in the lungs) is suspected, your doctor may order imaging tests and/or lung blood flow and air tests. These tests can also detect clots in the brain or coronary arteries. They may include:
- Chest X-ray. While X-rays don't directly show clots, they can reveal conditions caused by clots, such as chest pain and shortness of breath.
- Electrocardiogram (EKG). This painless test records the heart's electrical activity and can indicate abnormalities related to pulmonary embolism.
- CT scan. A contrast dye is injected into a vein, and images of the brain and lungs are taken to detect signs of clots.
- Cerebral angiography. This test uses a catheter, X-ray imaging, and contrast dye to provide clear images of brain blood vessels.
- Carotid ultrasound. This non-invasive test uses sound waves to create images of the carotid arteries, identifying blockages or narrowing that increase stroke risk.
- Lung blood flow and air tests. A chemical is used to measure inhaled air flow, which is then compared to blood flow in the arteries to detect pulmonary embolism.

Receive a specific diagnosis. Once all necessary tests are completed, your doctor can diagnose the specific type of blood clot. Treatment will depend on the clot's location and type. The main types include:
- Thrombus. A clot that forms in a vein or artery.
- Embolus. A clot that travels through the bloodstream to another location.
- Deep Vein Thrombosis (DVT). A common and dangerous clot, often forming in the leg's deep veins (though it can also occur in the arms, pelvis, or elsewhere), blocking blood flow and causing pain and swelling.
Treating blood clots with medical methods

Begin treatment immediately. Blood clots can be life-threatening, so medical intervention should begin as soon as possible.
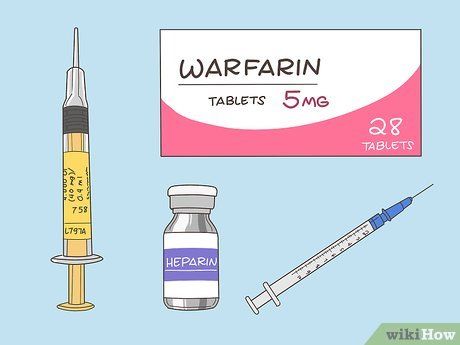
Take anticoagulant medication. Anticoagulants prevent the formation of blood clots. There are various types available, including:
- Enoxaparin (Lovenox). This injectable medication works immediately to thin the blood. The typical adult dose is 40 mg injected into fatty areas like the arm or abdomen.
- Warfarin (Coumadin). An oral anticoagulant, Warfarin thins the blood over time. Dosage varies by patient, and doctors may use a clotting test, known as INR, to determine the appropriate dose.
- Heparin. Administered intravenously, Heparin prevents clot growth. Dosage is determined through blood tests and tailored to individual needs.

Ask your doctor about thrombolytics. Thrombolytics, or clot-busting drugs, dissolve the fibrin strands that hold clots together. Dosage varies based on individual cases and treatment plans. Consult your doctor to determine the right dosage for you.

Consider surgical options. If medication alone cannot remove the clot, surgery may be necessary. Options include:
- Angioplasty. For heart clots, angioplasty uses a balloon to open the blockage, followed by a stent to keep the vessel open. The pressure from the balloon and stent breaks the clot into smaller pieces, restoring blood flow.
- Catheter-directed thrombolysis. This procedure involves inserting a catheter directly into the clot to deliver clot-dissolving medication.
- Thrombectomy. This surgery removes clots and is typically used when thrombolysis is ineffective or in emergency situations requiring immediate intervention.
Adjust your diet and lifestyle

Exercise for at least 30-45 minutes daily. Studies show that regular aerobic activity can prevent and reverse clot formation by improving blood circulation. Activities like walking, cycling, rowing, running, swimming, or jumping rope are excellent options. Consult your doctor to determine the safest exercises for you.

Drink plenty of water. Dehydration thickens the blood and can lead to complications. Ensure you stay hydrated, as maintaining proper fluid levels helps prevent the formation of blood clots.

Consume foods rich in nattokinase. Nattokinase is an enzyme that dissolves fibrin, helping to prevent clot formation and break down existing clots. It is found in natto (a Japanese fermented soybean dish), fermented black beans, fermented shrimp paste, and compressed soy sauce.
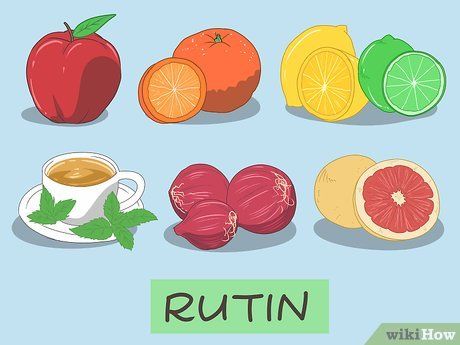
Incorporate rutin-rich foods into your diet. Rutin targets disulfide isomerase, an enzyme involved in blood clotting. It is present in apples, oranges, lemons, grapefruits (note that grapefruit interacts with some blood-thinning medications), buckwheat, onions, and tea. Include one of these foods in each meal, either as a dessert or as part of the main dish.

Increase your intake of bromelain. Bromelain interacts with fibrinogen to help dissolve the fibrin strands that bind clots. This enzyme is only found in pineapples. If you are at high risk for blood clots, consider adding pineapple as a dessert as often as possible.
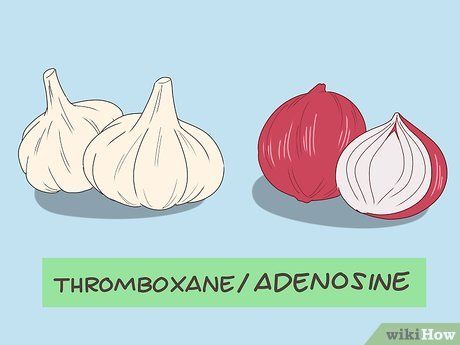
Add garlic to your diet. Garlic inhibits the production of thromboxane, a substance linked to blood clotting. It also contains ajoene and adenosine, which help prevent and dissolve clots.
- Onions also contain adenosine, so consider including them in your diet as well.

Opt for fish to meet your protein needs. Excessive protein intake, particularly from red meat and dairy products, appears to promote blood clot formation. Instead, aim to include more fish in your diet. Omega-3 fatty acids may help reduce cholesterol, thin the blood, and decrease clotting, although current evidence remains inconclusive.
- For the best results, focus on salmon, tuna, herring, mackerel, and sardines.
Warning- If you suspect you have a blood clot, do not delay seeking medical attention. Immediate treatment is crucial to avoid life-threatening complications.

































