Cysts are sealed sacs filled with fluid. These cysts can develop anywhere on the body and may result from infections, genetic factors, cellular defects, or blocked ducts. This article will help you recognize the symptoms of various types of cysts and how to treat them.
Steps
Identify the Type of Cyst
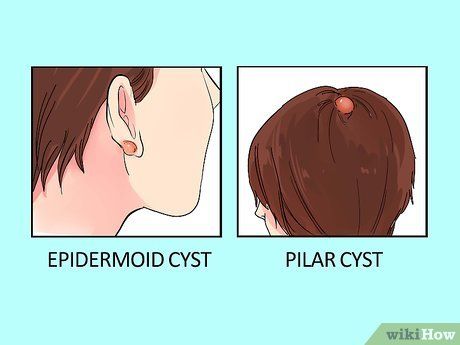
Distinguishing Between Sebaceous Cysts and Epidermoid Cysts. Epidermoid cysts are more common than sebaceous cysts. Each type has slightly different symptoms and treatment methods. Thus, correctly diagnosing the type of cyst is crucial for effective treatment.
- Both types of cysts have a skin-colored or white-yellow appearance and smooth surfaces.
- Epidermoid cysts are more common. This type of cyst grows slowly and generally does not cause pain. Epidermoid cysts do not require treatment unless they become painful or infected.
- Pilar cysts are primarily made of keratin (the protein found in hair and nails) and develop from the outer layer of hair follicles, typically on the scalp. Pilar cysts are often mistakenly referred to as sebaceous cysts, but they are distinct types of cysts.
- Sebaceous cysts typically form within hair follicles. They develop inside sebaceous glands, which produce the oily substance that covers hair. When this substance becomes trapped, it forms a small sac containing a cheesy-like material. Sebaceous cysts are commonly found near the neck, upper back, and scalp. They are often confused with pilar cysts or epidermoid cysts.

Distinguishing Between Breast Cysts and Tumors. Cysts can appear in one or both breasts. Without a mammogram or biopsy, it is nearly impossible to tell the difference between these two types of lumps in the breast. Symptoms of a breast cyst include:
- A soft, movable lump with distinct edges
- Pain at the lump site
- Increased size and discomfort right before menstruation begins
- Size and pain reduce after menstruation ends

Understanding Pustules. The term 'pimples' is a general description for various types of acne, including boils, blackheads, whiteheads, and pustules. Pustules are raised, red bumps typically 2-4 mm in size, resembling small lumps, and are the most severe form of acne. Infections of pustules are more serious than those of other types of acne like whiteheads. Pustules are painful.
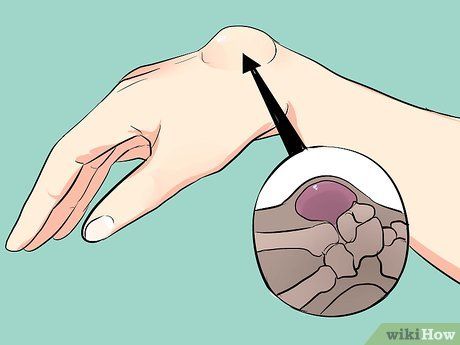
Identifying Ganglion Cysts. These are the most common type of lump found in the hands and wrists. Ganglion cysts are non-cancerous and generally harmless. This type of cyst is filled with fluid and may appear, disappear, or change size quickly. Ganglion cysts typically do not require treatment unless they interfere with joint function or cause cosmetic concerns.

Determining if the Pain is Due to a Pilonidal Cyst. This condition involves the formation of a cyst, abscess, or indentation in the crease between the buttocks, running from the lower end of the spine to the anus. Pilonidal cysts may be caused by wearing tight clothing, excessive body hair, prolonged sitting, or obesity. Symptoms may include: pus at the cyst site, pain, or warmth, redness, or swelling near the tailbone. Alternatively, there may be no symptoms other than a pit or dimple near the sacral spine.
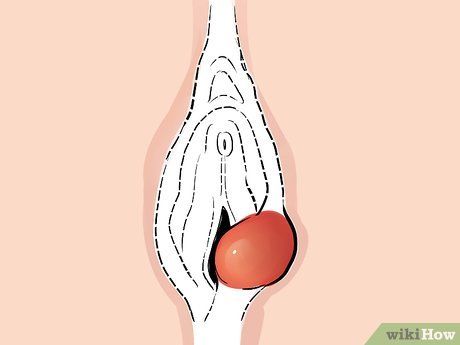
Distinguishing Bartholin's Gland Cysts. These glands are located on either side of the vaginal opening and are responsible for lubricating the vagina. When a Bartholin's gland becomes blocked, a relatively painless swelling forms, known as a Bartholin's cyst. It may not be noticeable unless the cyst becomes infected. Infection may develop after several days, causing pain, fever, discomfort when walking, pain during intercourse, and tenderness near the vaginal opening.
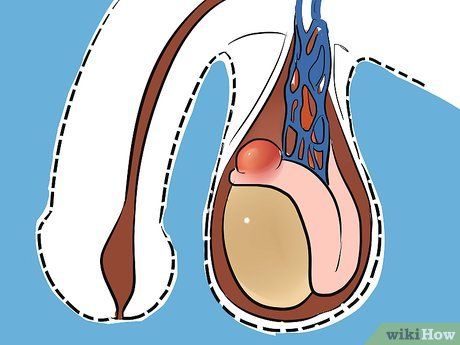
See a Doctor to Detect Swelling of the Testicles. Any case of testicular swelling should be diagnosed by a doctor to differentiate between cysts, cancer, hydrocele, or testicular infection. A testicular cyst, also known as an epididymal cyst, is a fluid-filled sac located above the testicle in the scrotum. It is typically painless and non-cancerous.

Consider Seeking a Second Opinion if Unsatisfied with a Diagnosis and Treatment Plan. Most cases of epidermoid cysts and pilar cysts don't require medical treatment. However, if you are not satisfied with the results after consulting a doctor, seeking additional advice may be worth considering. Epidermoid cysts and sebaceous cysts are usually easy to identify, but other conditions may present symptoms similar to these cysts.
- In a study by the Royal College of Surgeons in the UK, the authors discussed two cases where malignant melanoma and deep oral cavities were initially misdiagnosed as sebaceous cysts.
- Several infections can be mistaken for sebaceous cysts, including boils, carbuncles (furunculosis), and abscesses.
Preventing Cysts

Understanding Which Cysts Cannot Be Prevented. Pilar cysts develop after puberty and have a dominant genetic inheritance. This means that these cysts affect both sexes, and if one parent carries the gene for pilar cysts, the risk of the child inheriting it is higher. Around 70% of those with pilar cysts will experience multiple cysts throughout their lives.
- The cause of cyst development in breast tissue is still unclear.
- Doctors have yet to determine exact risk factors and prevention methods for pustules. However, pustules are believed to be associated with increased hormone levels during puberty, pregnancy, and deep follicular infections caused by sebum (skin oil) blockage.

Knowing Which Cysts Can Be Prevented. Most cysts are not preventable, except for a few types. For example, preventing a pilonidal cyst involves wearing loose clothing, maintaining a normal weight, and standing up after sitting for 30 minutes throughout the day.
- According to the American Academy of Dermatology, there is no effective method to prevent the formation of epidermoid cysts. However, certain groups are at higher risk of developing epidermoid cysts: men more than women, those with acne, and people who spend too much time in the sun.
- People with hand injuries are at higher risk of developing epidermoid cysts or ganglion cysts in the hand.
- Bartholin's cysts may develop following injury to the vaginal opening area.

Reducing the Risk of Cysts. While most cysts cannot be prevented, you can lower the risk of developing preventable types. Use oil-free skincare products and limit sun exposure.
- Shaving or waxing may also contribute to cyst formation. Avoid shaving or waxing too frequently in areas that have previously had cysts to prevent recurrence or the development of new cysts.
Home Treatment for Cysts
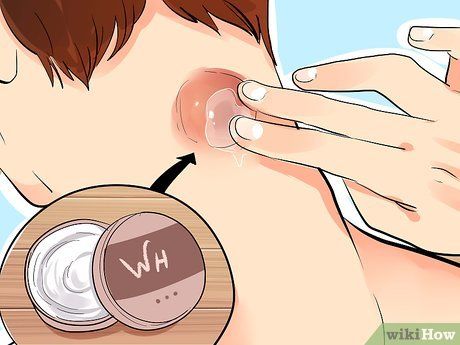
Home Treatment for Non-Infected Sebaceous and Epidermoid Cysts. Signs of infection include swelling, redness, warmth, or pain around the cyst. If home treatment methods are not effective or infection symptoms appear, seek medical attention from a doctor.
- Cysts that cause pain or discomfort while walking or during sexual activity should receive medical care and treatment.

Apply a Warm, Damp Towel to Epidermoid Cysts to Promote Drainage and Healing. The towel should be hot but not too hot to burn the skin. Apply the towel to the cyst 2-3 times a day.
- Pustules tend to respond better to cold compresses than to warm ones.
- Bartholin's cysts can be treated at home with a Sitz bath, which involves sitting in warm water to help drain the cyst.
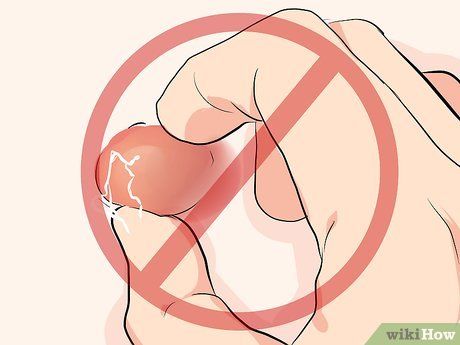
Do Not Pop, Squeeze, or Pierce Epidermoid or Sebaceous Cysts. These actions increase the risk of infection and can lead to scarring. Additionally, avoid popping pustules to prevent deeper infections and further scarring.

Allow Epidermoid Cysts to Drain Naturally. When a cyst begins to drain, cover it with a sterile dressing and change the dressing twice a day. Seek medical attention if a large amount of pus starts to drain, the surrounding skin becomes red, the cyst becomes warm and painful, or blood begins to ooze from the cyst.

Keep the Cyst Clean. To prevent infection, it is important to keep the cyst and surrounding skin clean. Wash the area with soap or antibacterial cream every day.
Seek Medical Attention

Know When to Seek Medical Help. Most cysts are harmless and will resolve on their own, but some may require medical attention. You should see a doctor if the cyst becomes swollen or painful, or if the skin around the cyst becomes warm, as these could be signs of infection.

Consult Your Doctor About Cyst Removal. If the cyst is affecting your daily life, do not attempt to pop it yourself. Instead, consult with your doctor to determine whether surgical removal of the cyst is safe and recommended.

Evaluating Surgical Options. There are various surgical procedures depending on the cyst's location, size, and the extent to which it obstructs bodily function. Three main methods are used to remove cysts. You and your doctor should discuss each procedure to determine the most suitable option for your situation and the type of cyst.
- Incision and drainage (I & D) is a simple procedure where the doctor makes a 2-3 mm incision in the cyst and gently presses to drain the fluid. This can be performed in an outpatient clinic for surface cysts such as epidermoid, sebaceous cysts, and pilonidal cysts, or for cysts that are not deeply infected (if necessary). Incision and drainage may also be used for breast, lymph node, testicular, or Bartholin's cysts in outpatient settings with local anesthesia. However, cysts have a high recurrence rate if the cyst wall is not removed. This procedure does not remove the cyst wall.
- The minimal excision technique helps remove the cyst wall and cheese-like oily material inside. The cyst is opened and drained before the cyst wall is pulled out. Depending on the size, suturing may or may not be necessary. This method may be used for breast, testicular, Bartholin's gland, or lymph node cysts. Excision is rarely used for acne cysts. The procedure is usually done under local anesthesia, allowing the patient to go home the same day; general anesthesia is typically used for children.
- Laser cyst removal is only suitable for large epidermoid cysts or those located in thicker skin. This procedure opens the cyst with a laser and gently presses out the internal fluid. After a month, a minimal excision procedure is performed to pull out the cyst wall. This method has high aesthetic value for non-inflammatory or non-infected cysts.

Assessing the Necessity of Cyst Removal on the Skin. Many at-home treatments can help promote drainage and healing of sebaceous or epidermoid cysts. However, you should seek medical attention if the cyst appears infected, grows rapidly, is in a constantly irritated area, or if you are concerned about cosmetic appearance.

Determining Whether Breast Cyst Removal is Necessary. Treatment for simple fluid-filled breast cysts is not always required. If you are premenopausal, your doctor may recommend monitoring the cyst monthly. A fine needle aspiration may be performed to drain the cyst.
- If the cyst does not resolve over 2-3 menstrual cycles or increases in size, your doctor may recommend an ultrasound.
- Oral contraceptives may be prescribed to regulate hormone levels during the menstrual cycle. This treatment is only recommended for women with severe symptoms.
- Surgical removal is only necessary if the cyst is troublesome, contains bloody or greenish fluid when aspirated, or if the doctor suspects it is a non-benign proliferative cyst. In such cases, the entire cyst will be surgically removed (after anesthesia), as incision and drainage will leave the cyst wall behind and increase the risk of recurrence.

Consulting a Dermatologist About Treating Cystic Acne. Initially, the doctor may prescribe medications to treat other forms of acne. If there is no improvement, the doctor may recommend using Isotretinoin or Accutane.
- Accutane is an effective medication for acne control. However, it may have side effects such as birth defects, increased risk of depression and suicide, effects on lipid levels, liver function, blood sugar, and white blood cell count. Blood tests should be conducted once a month to monitor reactions to the drug. Women must take two forms of birth control while using Accutane.
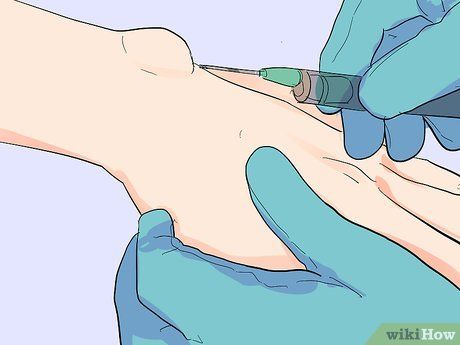
Seeking Treatment for Lymph Node Cysts. The treatment for these cysts typically involves observation, and surgery is generally not required. The affected area can be immobilized if movement exacerbates the size, pressure, or pain. If the cyst is painful or obstructs function, it may be aspirated. In this process, a small needle is used to withdraw the fluid at a sterile outpatient clinic.
- If symptoms do not improve with non-surgical methods (aspiration or immobilization), or if the cyst recurs after aspiration, the doctor may recommend surgical excision of the cyst, known as complete lymph node excision. During this procedure, part of the tendon or joint capsule may also be removed. There is still a small chance that the cyst may recur after complete removal. This surgery is performed under local anesthesia, and patients can typically be treated on an outpatient basis.
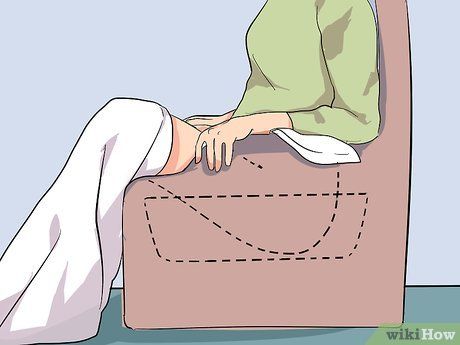
Treatment for Bartholin's Gland Cysts. The approach to treatment depends on the cyst's size, how inconvenient it is, and whether it is infected. Taking warm Sitz baths (sitting in a few centimeters of warm water) several times a day may encourage the Bartholin's gland to naturally drain.
- Incision and drainage are used if the Bartholin's gland becomes enlarged or infected, and Sitz baths are ineffective. Local anesthesia or sedation will be applied. A catheter may be left in place to keep the gland open for up to 6 weeks to allow complete drainage.
- Doctors may prescribe antibiotics to treat any infection.

Understanding Treatment for Testicular Cysts. The first step is for the doctor to confirm that the cyst is not cancerous. If the cyst is large enough to cause a heavy sensation or drag on the testicle, the doctor will discuss surgical removal options with you.
- The Children's Hospital of Philadelphia does not recommend surgery for adolescents. Instead, they encourage young people to learn how to self-examine and report any changes or growth (which could indicate a need for surgery). Testicular cysts in children often resolve on their own.
- Sclerotherapy, a technique where a sclerosing agent is injected, is an option to reduce the need for scrotal surgery and has shown good results in studies. When ultrasound is used to guide the injection of the sclerosing agent, symptoms resolved in 84% of men within 6 months. The sclerosing agent helps reduce the size and symptoms of the testicular cyst. This process significantly reduces health risks and the likelihood of cyst recurrence.
Advice
- Most types of cysts cannot be prevented and are non-cancerous. In most cases, doctors will wait and observe before recommending any medical intervention or surgery.
Warnings
- Avoid squeezing, pressing, or poking at cysts. These actions can increase the risk of infection and cause scarring in the tissue.
- Most skin cysts resolve on their own. If you'd like to speed up the process of cyst removal, you can visit a doctor to discuss treatment options based on the cyst's size, location, and type.
- Always wash your hands thoroughly before and after treating a cyst or any skin infection.
