"Giving birth at home" occurs when a woman decides to deliver her baby at home instead of going to the hospital. Many women prefer home births for a variety of reasons. For example, it allows the mother to have more freedom to move around, eat, and bathe. The mother also feels more comfortable giving birth in the presence of loved ones in a familiar environment. However, there can be challenges and risks associated with home births. Therefore, if you're uncertain about delivering at home, it’s important to understand what could happen beforehand. To start, check out Step 1 below:
Learn About Home Births

Understand the advantages and disadvantages of home births. Recently, there have been many cases of home births. However, data from 2009 shows that in the U.S., only about 0.72% of all births occurred at home. While most other developed countries also have similarly low numbers, some mothers still prefer giving birth at home rather than in a hospital. There are countless reasons why some mothers choose home birth over hospital birth. However, it’s important to note that "some scientific studies suggest that the risk of complications doubles or triples during home births." Although the rate of complications is still relatively low compared to acceptable levels (only a few cases of complications per 1000 births), mothers should be aware that home births may carry more risks than hospital births. Nevertheless, there are certain benefits to home births that hospital births can't offer, such as:
- The mother can move around freely, bathe, and eat as desired.
- The mother can adjust her birthing position.
- The mother feels more comfortable surrounded by familiar faces and a familiar space.
- If desired, the mother can give birth without medical assistance (such as pain relief medications).
- The mother can incorporate her religious or cultural practices during childbirth.
- In some cases, the mother may reduce the cost of childbirth.

Understanding when not to give birth at home. In certain situations, childbirth can increase the risk of complications for both the mother and baby, or both. In such cases, the health of both mother and child is more important than any minor benefits that home birth may offer. Therefore, it is recommended to give birth in a hospital where experienced doctors and medical equipment can support you. Here are some cases when expectant mothers should "definitely" give birth in a hospital:
- When the mother has any chronic health conditions (such as diabetes, epilepsy, etc.)
- When the mother has previously required a cesarean section
- If prenatal screenings detect any health issues with the fetus
- If the mother’s health status negatively impacts the pregnancy
- If the mother smokes, drinks alcohol, or uses any prohibited substances during pregnancy
- If the mother is carrying twins, triplets, or the fetus is not in the correct birth position
- If giving birth prematurely or past the due date. In other words, avoid home birth before 37 weeks or after 41 weeks of pregnancy.

Understanding the legality of home births. Generally, most countries do not prohibit home births. Home birth is legal in the United States, Australia, Canada, and governments may offer financial support depending on the situation. However, the legal aspects surrounding midwives in the U.S. can be complex.
- In the U.S., all 50 states allow hiring certified midwives. These midwives typically work in hospitals—although they rarely visit homes, it remains legal to hire them for home births. In 27 states, hiring freelance midwives or certified professional midwives is entirely legal. Freelance midwives are often self-taught, having learned through apprenticeship or informal training, and are not required to be registered nurses or doctors. Certified professional midwives, on the other hand, are accredited by the North American Registry of Midwives, and do not require insurance or verification.
Creating a Birth Plan

Consulting with a doctor or midwife. You should have a midwife or doctor accompanying you during a home birth. Plan for the midwife or doctor to arrive early at your home so that you can discuss your situation before labor begins, and make sure to keep their contact number on hand in case your birth doesn’t go as expected.
- The Mayo Clinic advises ensuring that your doctor or midwife can easily consult with nearby hospital doctors if necessary.
- You should also find or hire a doula who can offer emotional support and physical energy throughout your labor.

Planning your childbirth. Giving birth is a physically exhausting and emotionally intense experience. The last thing you want to do while in labor is to make last-minute decisions about how to deliver your baby. It's smarter to plan and review your birth plan carefully before labor begins. Try to map out the steps from the beginning to the end of labor. Even if you can’t follow the plan exactly, having a plan in place will give you peace of mind. In your plan, try to address questions such as:
- Who do you want present during labor, aside from the doctor/midwife?
- Where do you plan to give birth? Keep in mind that if labor lasts long, you may want to move around for comfort.
- What should you bring to your birth? Discuss this with your doctor, as you'll likely need towels, bed sheets, pillows, blankets, and waterproof bedding for the bed and floor mats.
- How will you manage pain? Will you use pain medication, the Lamaze method, or other pain control techniques?

Prepare transportation to the hospital. Many home births are successful and complication-free. However, each birth carries the potential for minor changes that could pose risks to the health of either the mother or the baby. Therefore, it’s crucial to be prepared to quickly transport the mother to the hospital in case of an emergency. Ensure your vehicle has a full tank of gas, and pack necessary items like clean towels and blankets. Know the quickest route to the nearest hospital—consider even driving there beforehand to familiarize yourself with the way.

Choose where you will give birth. While you may be able to adjust your position and move around during labor, it’s a good idea to designate a specific area in your home for childbirth. Choose a safe, comfortable spot—many people prefer giving birth in their own bed, but you could also choose a sofa or even the floor. Ensure the space is clean and equipped with towels, blankets, and pillows. You might also want to have a waterproof cover or plastic sheet to protect from blood stains.
- In an emergency, a clean, dry bath towel can serve as an effective waterproof barrier to prevent stains.
- Although your doctor or midwife will likely have these items, it's still a good idea to prepare sterile gauze and a cord clamp nearby for cutting the umbilical cord.

Wait for the signs of labor. Once you have everything prepared, all you need to do is wait for the labor to begin. On average, most pregnancies last around 38 weeks, although a healthy birth can happen 1 or 2 weeks earlier. If your pregnancy ends before 37 weeks or extends beyond 41 weeks, head to the hospital immediately. Otherwise, prepare for the following signs that labor may be starting:
- Water breaking
- Cervical contractions
- Spotting (light pink or brownish mucus)
- Contractions lasting 30 to 90 seconds
Giving Birth
Natural Birth

Listen to your doctor or midwife. The healthcare professionals you choose for your home birth have been trained to safely assist with the delivery of your baby and are certified to do so. Always listen to the advice of your doctor or midwife and follow their instructions as best as possible. Some of their recommendations may temporarily increase your discomfort, but their ultimate goal is to ensure the fastest and safest delivery for both you and your baby. So try to follow their instructions as closely as possible.
- Most of the advice is simple guidance – always follow the advice of your doctor or midwife.

Stay calm and focused. It's unavoidable that childbirth may be painful and stressful, but never let yourself become discouraged or frustrated. Stay relaxed and alert. This will help you follow the instructions from your doctor or midwife as best as you can, ensuring that your delivery is as quick and safe as possible. One of the easiest ways to relax is to let go of tension and take deep breaths.

Monitor signs of complications. As mentioned earlier, most home births proceed without major issues. However, complications can arise during delivery. If you notice any of the following signs, go to the hospital immediately, as they may indicate serious pregnancy complications that require medical equipment and healthcare professionals:
- Meconium-stained amniotic fluid when your water breaks.
- Prolapsed umbilical cord.
- Heavy vaginal bleeding without amniotic fluid, or if the amniotic fluid contains an unusual amount of blood (normal amniotic fluid is pink, brown, or lightly tinged with blood).
- Failure to expel the placenta after delivery or if the placenta is incomplete.
- The baby is not in a head-down position.
- Any form of injury to the baby during delivery.
- The labor isn't progressing to the stage of delivery.

Have a medical professional monitor your cervical dilation. In the early stages of labor, your cervix softens, thins, and opens to allow the baby to be born. Initially, it may not be very uncomfortable. As labor progresses, contractions become stronger and more frequent. You may feel an increase in pain or pressure in your lower back or abdomen as the cervix dilates. Your doctor will monitor this process closely. Once your cervix is fully dilated to about 10cm, you will be ready to move on to the second stage of labor.
- You will begin to feel the urge to push. Your doctor may advise you not to push until your cervix is fully dilated to 10 cm.
- At this point, it's typically not too late to use pain relief. If pain relief is available and suitable for you, discuss with your doctor or midwife to determine if it's the right option.

Follow medical staff instructions during pushing. In the second stage of labor, contractions will become stronger and more frequent. If your cervix is fully dilated, you may feel a strong urge to push, and it is perfectly fine to do so. Inform your doctor or midwife of any changes you experience, and they will guide you on when to push, how to breathe, and when to rest. Follow their guidance as best as you can. This stage may last up to two hours for first-time mothers, or sometimes much faster (sometimes as little as 15 minutes) for women who have given birth before.
- Don’t worry about different positions like lying on the floor, kneeling, or squatting. Your doctor or midwife will position you in the most comfortable way to help with effective pushing.
- When pushing, don’t worry if you accidentally urinate or have a bowel movement. This is completely normal, and your birthing team will wait for it to happen. Just focus on pushing the baby out.

Pushing the baby through the birth canal. The combination of pushing and contractions will guide your baby from the womb into the birth canal. At this point, the medical staff will be able to see the baby's head, referred to as the "crown." You may use a mirror to see it yourself. Don’t be alarmed, as the head will soon appear fully. This is a normal part of the process. Once the head is out, the baby will continue to move down the birth canal. You will need to push strongly to help the head emerge completely. Afterwards, the nurse will clean the baby's nose and mouth of amniotic fluid and assist you in delivering the rest of the baby’s body.

Caring for the baby after birth. Congratulations on successfully delivering at home! The doctor or midwife will clamp and cut the umbilical cord with sterile scissors. Then, the baby will be gently wiped with a clean cloth and wrapped in a warm, clean blanket. After delivery, the midwife may advise you to begin breastfeeding your baby. Don’t bathe the baby immediately, as you will notice a white covering on the skin, which is perfectly normal. This white layer is called "vernix," and it helps protect the baby from bacterial infections and keeps the skin moisturized.
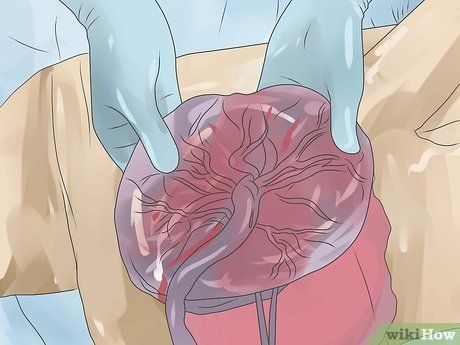
Expelling the placenta. After delivering your baby, although the hardest part is over, the task isn’t complete yet. In the third and final stage of labor, you must expel the placenta, the organ that nourished your baby while in the womb. Mild contractions (which many mothers may not even notice because they are so light) will help separate the placenta from the uterine wall. The placenta will then be expelled through the birth canal, typically within 5-20 minutes. Compared to delivering the baby, this is a relatively minor challenge. If the placenta is not expelled or remains inside, it’s critical to go to the hospital, as this could lead to serious consequences.
Taking the baby to the pediatrician. It’s a good idea to take your baby to see the pediatrician after birth if the baby is in good health. However, it’s important to schedule a check-up within a few days to ensure that there are no underlying health issues with your baby. Plan to visit the pediatrician within 1 or 2 days after birth. The doctor will conduct an examination and provide guidance on how to care for your baby’s health. You may also want to check your own health – childbirth is a strenuous process, and if something doesn’t feel right, it’s best to let the doctor check you over for any potential issues.
Water Birth

Giving birth underwater involves the act of delivering a baby submerged in water. This birthing method has gained popularity in recent years, with some hospitals even setting up pools for water births. However, some doctors consider this method less safe than traditional childbirth. While some mothers claim that water birth is more comfortable, relaxing, less painful, and more 'natural' than regular birth, it does carry certain risks, such as:
- Infections from contaminated water
- The baby might suffer complications from swallowing water
- Although rare, there is a risk of brain damage or death from oxygen deprivation while the baby is underwater.

Similar to giving birth at home, water birth is not advisable if either the mother or the baby faces certain health risks. If any of the complications mentioned in Part 1 arise during pregnancy, it's better to avoid water birth and opt for a hospital delivery instead. Additionally, water birth should be avoided if the mother has genital herpes or any other infectious condition that could potentially be passed to the baby through the water.

Preparing a pool for the water birth is an essential step. During the first 15 minutes of labor, ask your doctor, midwife, or a trusted friend to fill a pool with water approximately 30.48 centimeters deep. Specially designed birthing pools are available for sale or rent, and some health insurance policies may cover this cost. Once ready, undress down to your waist (or completely, if preferred) and step into the pool.
- Ensure that the water is clean and not warmer than about 37°C.

You might want your partner, such as your husband, to join you in the water during labor, for emotional support and closeness. Others prefer having the doctor or midwife in the pool with them instead. If you choose to have your husband join you, you can lean on him for support while pushing the baby out.

The birthing process will begin with the assistance of your doctor or midwife, who will guide you through breathing techniques, pushing, and resting as necessary. Once you feel the baby coming, ask the doctor, midwife, or your partner to position themselves between your legs to catch the baby as it emerges. During the delivery, you may want to grip someone's hand tightly.
- Similar to traditional birth, you can change positions for comfort. For instance, you may try pushing while lying or kneeling in the water.
- If either you or the baby shows signs of complications, you should exit the water immediately (see Part 3 for more information).

Immediately Remove the Baby from the Water. As soon as the baby is born, lift them out of the water so they can begin breathing. After holding your baby for a moment, carefully step out of the pool to cut the umbilical cord and ensure the baby stays warm, dry, and dressed in a blanket.
- In certain cases, the baby may pass stool while still in the womb. If this occurs, make sure the baby's head remains above the water and away from any contaminated water sources to avoid serious infection if the baby swallows or inhales their own feces. If you suspect this has happened, rush your baby to the hospital immediately.
Advice
- Consider asking knowledgeable friends or a registered nurse near your area for assistance.
- Never leave your baby unattended without a doctor or nurse nearby. Many situations can worsen quickly.
- If possible, clean the vaginal area before delivery to ensure it remains hygienic and sanitary.
Warnings
- In twin pregnancies, if one baby is head-down and the other is breech, this can create a challenging situation (one baby may begin to be delivered while the other remains in the womb, requiring a specially trained doctor, nurse, or midwife to handle the situation).
- Nurses, friends, and even doctors may be somewhat apprehensive about home births. This is not ideal in today's society. Try to understand if they act hesitantly or distractedly. You don’t need to be upset with them.
- If the umbilical cord is wrapped around the baby's neck or if the twins' cords are tangled or if parts of their bodies are attached, a cesarean section may be necessary. Therefore, always ensure that professional assistance is readily available or nearby during delivery.























