A fever can be caused by many factors such as viruses, bacterial infections, or even the common cold, which makes children feel unwell. Fever is the body’s natural response to fight infections or illnesses. A fever is identified by a temporary increase in body temperature that becomes concerning or uncomfortable when it reaches 39.4°C or higher. In infants, a fever could sometimes indicate a more serious underlying issue. Therefore, it is important to monitor your child closely. As a parent or caregiver, you can take the necessary steps outlined below to help ease your child’s discomfort.
Steps
Managing a Fever at Home
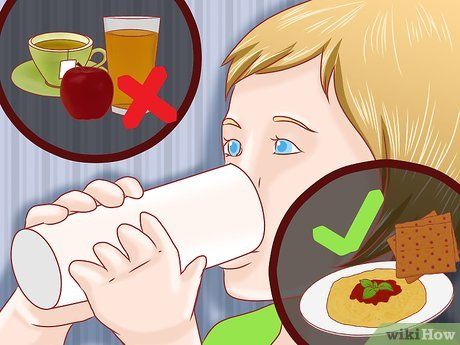
Keep the child hydrated. Ensure your child stays hydrated by offering plenty of fluids. Fever leads to excessive sweating, causing dehydration, which can be dangerous. Consult with a doctor about using electrolyte solutions, such as those found in formula milk.
- Avoid giving fruit juices or apple juice; instead, dilute them with 50% water.
- You can offer your child popsicles or gelatin.
- Steer clear of caffeinated drinks, as they stimulate urination, contributing to dehydration.
- Let your child eat as they normally would, but keep in mind that they may not feel like eating much while feverish. Offer bland foods like bread, crackers, pasta, or oatmeal.
- Breastfed infants should continue to nurse frequently to stay hydrated.
- Never force your child to eat if they don’t want to.
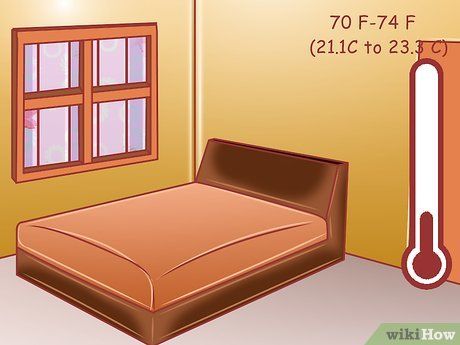
Let the child rest in a comfortable room. Ensure the child lies down in a room with a comfortable temperature ranging from 21.1°C to 23.3°C.
- Avoid running the heater continuously, as it may cause the child to become too hot.
- Similarly, turn off the air conditioner to prevent the child from getting too cold and to help raise their body temperature.
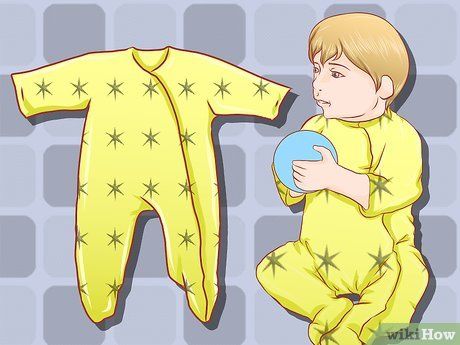
Dress the child in light clothing. Thick clothing may increase body temperature. Overdressing can trap heat and make the child more uncomfortable.
- Dress the child in loose, breathable clothes and use a light blanket if the room temperature is too cold or if the child is shivering. Adjust the room temperature if needed to keep the child comfortable.

Give the child a warm bath. Warm water, neither too hot nor too cold, can help reduce fever.
- If you plan to give your child a warm bath, administer medicine beforehand to prevent their body temperature from rising after the bath.
- Avoid cold water, ice baths, or using rubs as they may cause the child to feel chilled and worsen the situation.

Administer medication to the child. Be cautious when giving medications like Tylenol, Advil, or Motrin. Carefully read the instructions to ensure the correct dosage for the child’s age. Always consult a healthcare professional before giving fever-reducing medication.
- Acetaminophen (Tylenol) and ibuprofen (Advil, Motrin) are commonly recommended by doctors or pharmacists to reduce fever in children.
- If the child is under 3 months old, always call the doctor before giving any medication.
- Avoid exceeding the recommended dosage, as it may damage the liver or kidneys, or even be fatal.
- You may administer Acetaminophen every 4 to 6 hours and Ibuprofen every 6 to 8 hours if the child is over 6 months old.
- Track the type of medication, dosage, and timing to prevent overdose.
- For temperatures below 38.9°C, try to avoid using medication unless advised by a doctor or nurse.
- Never give aspirin to children, as it can cause a rare but dangerous condition called Reye's syndrome.
Seek Medical Help

Check if the temperature is rising. Even a slight fever could indicate a serious infection in a child. Depending on the child’s age, it is important to contact a pediatrician if the child’s temperature significantly increases.
- For infants up to 3 months old with a temperature of 38°C or higher, call the pediatrician for advice on how to handle the situation.
- If the child is older than 3 months and has a temperature of 38.9°C or higher for over a day, contact the pediatrician.
- Even if it's just a suspicion, it's always safer to contact the pediatrician to ensure the child’s safety.

Know when to contact a pediatrician. If the child has a fever but is still playing and eating normally, there is no immediate cause for concern. The American Academy of Pediatrics (AAP) advises contacting a pediatrician if the child is younger than 3 months old and has a temperature of 38°C or higher. For children over 3 months old, if the fever lasts more than 24 hours and is accompanied by other symptoms like coughing, ear pain, loss of appetite, vomiting, or diarrhea, call the pediatrician or take the child to an urgent care clinic.
- If the child becomes lethargic, uncomfortable after a fever breaks, unusually irritable, has a stiff neck, or doesn't cry tears, contact the pediatrician immediately.
- Consult the pediatrician if the child has pre-existing medical conditions like heart issues, immune disorders, or sickle cell disease when they have a fever.
- Contact the pediatrician if the fever lasts more than 48 hours, the child urinates less, has excessive diarrhea or vomiting, as these may indicate the need for a thorough check-up.
- Call the pediatrician if the child’s fever exceeds 40.5°C or lasts for more than 3 days.
- If the child is febrile and unresponsive, unable to walk, has trouble breathing, or displays a bluish tint in the lips, tongue, or nails, call emergency services at 115.

Prepare everything to take the child to the doctor. If your child requires medical attention, make sure to bring the necessary documents to ensure they receive prompt and appropriate care. Additionally, be prepared to provide information when at the clinic.
- Note down all relevant information regarding the child’s fever: when the fever started, how frequently the child’s temperature was checked, and inform the doctor of any other symptoms observed.
- List the medications, vitamins, and supplements the child is currently taking, along with any known allergies.
- Prepare questions for the doctor, such as the possible causes of the fever, what tests may be required, what treatments are recommended, and whether the child needs to take any medication.
- Be ready to answer questions from the doctor, such as when the symptoms began, if the child has taken any medications and when, and what steps you’ve taken to lower the fever.
- Mentally prepare for the possibility that the child may need to be hospitalized for monitoring or further testing, particularly if the child is very ill or under 3 months old.
Prevent Future Fevers

Wash your hands. In most cases, keeping your hands clean is essential, as they are the part of your body most likely to come into contact with germs that can spread to other areas.
- Wash your hands, especially before eating, after using the restroom, playing with pets, using public transport, or after visiting sick individuals.
- Ensure thorough handwashing, including the back of your hands, palms, between your fingers, and under your nails for at least 20 seconds using warm water and soap.
- Carry hand sanitizer when out and about or when soap and water are unavailable.
Avoid touching the T-zone on your face. The T-zone consists of the forehead, nose, and chin, forming a 'T' shape on the face. The nose, mouth, and eyes within this zone are key entry points for viruses and bacteria, leading to infections.
- Block all bodily fluids originating from the T-zone: cover your mouth when coughing, turn away from others when sneezing, and wipe your nose (then wash your hands!).
Avoid sharing personal items. Try not to share cups, water bottles, or other personal items with children, as this is an easy way to transfer germs, especially from parents to children, who may not yet have fully developed immune systems.
- Avoid using your mouth to clean a child's pacifier and then giving it to them. Germs from adults are very strong when transferred to a child’s mouth and can easily cause illness. The same applies to toothbrushes.

Keep your child at home when sick. Keep your child home from school if they are ill or have a fever to prevent the spread of illness to other children. If you know friends or family members are sick, try to keep your child away from them until they recover.

Ensure your child is up to date on vaccinations. Stay informed about your child’s vaccination schedule, including the annual flu vaccine, to reduce the risk of illness.
