Dehydration in young children occurs when their fluid intake is insufficient to compensate for the fluids lost through excretion. Common factors leading to dehydration include hot weather, feeding issues, fever, diarrhea, and vomiting. You can help prevent dehydration by identifying symptoms, reducing conditions that cause dehydration, and knowing when to seek medical help. Severe dehydration can lead to significant health problems in children and even be fatal.
Steps
Identifying Dehydration
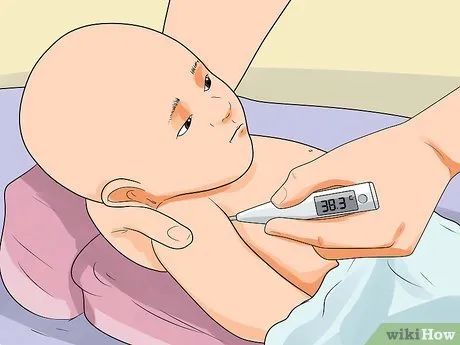
Understand the main causes of dehydration in young children. Fever, diarrhea, vomiting, hot weather, and reduced appetite are among the most common causes. Conditions such as cystic fibrosis or celiac disease can impair nutrient absorption and lead to dehydration. Signs of dehydration in children include:
- Sunken eyes.
- Reduced urination frequency.
- Dark-colored urine.
- A sunken soft spot on the top of a baby's head (known as the fontanelle).
- No tears when crying.
- Dry or sticky mucous membranes (the lining inside the mouth or tongue).
- Lethargy (slower than usual activity).
- Increased fussiness or inconsolable crying.
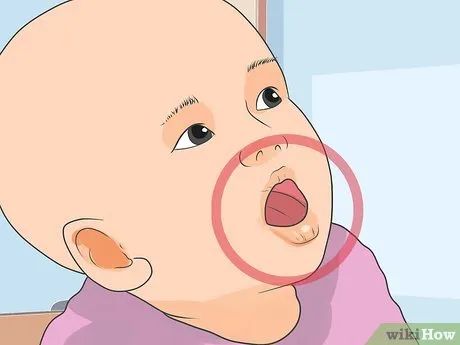
Identify mild to moderate dehydration symptoms in young children. Many cases of mild or moderate dehydration can be managed at home. If left untreated, dehydration can become severe. Pay attention to these symptoms before they worsen. The symptoms include:
- Reduced activity levels.
- Slower sucking reflex in infants.
- Lack of appetite.
- Fewer wet diapers than usual.
- Dry, cracked skin around the mouth.
- Dry mouth and lips.
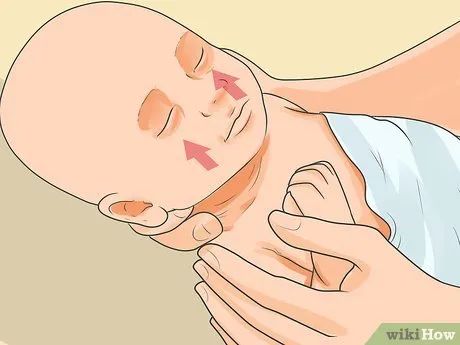
Recognize severe dehydration symptoms in young children. In such cases, medical attention is required. Contact a doctor immediately if the child shows signs of severe dehydration. Symptoms include:
- No tears or very few tears when crying.
- No wet diapers for 6 to 8 hours or fewer than three wet diapers in 24 hours, with dark yellow urine.
- Sunken fontanelle and eyes.
- Cold or discolored hands and feet.
- Very dry skin or mucous membranes in the mouth.
- Rapid breathing.
- Sluggish movements (very little activity) or extreme fussiness.
Managing Fluid Intake

Increase fluid intake for conditions that may lead to dehydration. Overheating or even higher-than-normal ambient temperatures can quickly cause dehydration. Fever, diarrhea, and vomiting also contribute to fluid loss. In such cases, ensure the child drinks additional fluids.
- Offer fluids every half hour instead of every few hours.
- Encourage more frequent breastfeeding if applicable.
- Provide smaller, more frequent bottle feeds.

Offer fluids other than water if the child is over 4 months old. If the child has not started solid foods, do not give more than 120 ml of additional fluids. You can provide extra water if the child has begun eating solids. Dilute fruit juice if offering it. You may also give oral rehydration solutions like Pedialyte, Rehydralyte, or Enfalyte.

Consult a doctor or lactation expert if the child is not latching properly. Improper breastfeeding increases the risk of dehydration. The child's mouth should cover the areola, not just the nipple. If you hear loud noises during feeding, the child may not be getting enough milk. A specialist can help diagnose and resolve breastfeeding issues.

Discuss your concerns with a doctor if the child refuses to eat. Keep track of daily diaper changes and the child's food intake or feeding frequency. The doctor can use this information to assess whether the child is adequately hydrated.
Avoid Overheating
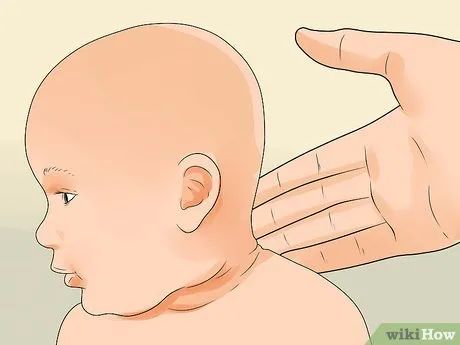
Check if the child is overheating by gently touching the back of their neck. Touching is often the best way to gauge a child's body temperature. If the skin feels hot and sweaty, the child may be overdressed. Overheating can lead to dehydration in young children.

Minimize the child's exposure to hot temperatures. Creating a cool environment around the child can significantly reduce the risk of dehydration. Higher ambient temperatures also increase the risk of Sudden Infant Death Syndrome (SIDS). Studies show that children exposed to an average temperature of 28.9 °C have twice the risk of SIDS compared to those in an average temperature of 20 °C.
- Use a thermometer to monitor the room temperature.
- Use air conditioning during summer.
- Avoid overheating the room with heaters in winter.

Use blankets or clothing appropriate for the weather and indoor temperature. Avoid wrapping the child in thick blankets if the indoor temperature is already warm, even if it's cold outside. Overheating due to excessive layers is considered a risk factor for Sudden Infant Death Syndrome (SIDS).
- Avoid over-bundling the child during sleep.
- Dress the child in weather-appropriate clothing.
- Steer clear of thick fabrics, heavy coats, hoods, or long clothing in summer unless they are made of breathable materials.

Keep the child in the shade when outdoors. This also helps protect their skin. Use a stroller with a movable canopy. Carry a sun umbrella if you're in sunny areas like the beach. Install sunshades on car windows to shield the child from sunlight while driving.
Preventing Dehydration During Illness
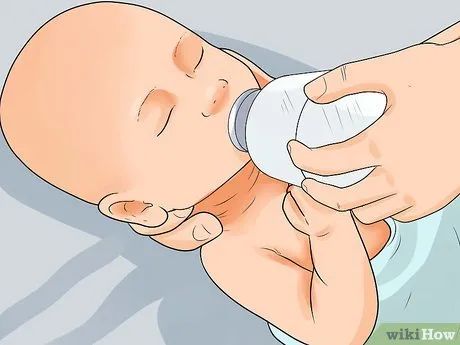
Pay extra attention to fluid intake when the child is sick. Children with fever, diarrhea, or vomiting are more prone to dehydration. Increase the frequency of breastfeeding or formula feeding. Offer smaller portions if the child is vomiting.
- For a vomiting child, consider giving 5-10ml of water using a medical syringe or spoon every 5 minutes. A doctor can guide you on the appropriate amount and frequency.
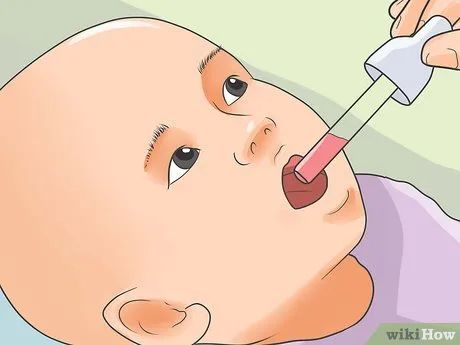
Observe whether the child is swallowing. A stuffy nose or sore throat due to illness can make swallowing difficult. Address these symptoms promptly.
- Consult a doctor about using pain relievers if the child refuses to swallow due to a sore throat.
- Use saline drops for infants to clear nasal congestion and a syringe to remove mucus. Ask a doctor for proper usage and consider alternative treatments if the condition persists or worsens.

Use oral rehydration solutions (ORS). Some are specifically designed for children to replenish lost fluids, sugars, and salts. Administer ORS as directed by a doctor if the child cannot swallow and continues to experience diarrhea or vomiting. Alternate between breastfeeding and ORS if you are nursing. If using formula, stop giving it and other beverages while using ORS.
- Common ORS brands include Pedialyte, Rehydralyte, and Enfalyte.

Seek emergency medical care if the child is severely ill and dehydrated. Dehydration in young children can be life-threatening. If the child's fever, diarrhea, or vomiting persists or worsens, or if severe dehydration symptoms appear, contact a doctor or take the child to the hospital immediately.
Warnings
- Avoid giving fruit juice to a child with diarrhea, as it may worsen the condition.
