Asthma is a treatable condition that often arises from allergic reactions: environmental triggers lead to inflammation in the respiratory pathways. Asthma causes difficulty breathing until the inflammation is treated and healing takes place. Approximately 334 million people worldwide suffer from asthma, with 25 million cases in the United States. If you suspect asthma, you can recognize it through symptoms, risk factors, and diagnostic tests.
Steps
Identify Risk Factors for Asthma

Consider the combination of gender and age factors. In the United States, boys under 18 are 54% more likely to develop asthma compared to girls. However, by age 20, women tend to have a higher incidence of asthma than men. At age 35, this gap changes to 10.1% in women and 5.6% in men. After menopause, the rate decreases in women, and the gap narrows, though it does not disappear entirely. Experts have various explanations for why gender and age influence the risk of asthma:
- Allergic tendencies (genetic sensitivity) in adolescent boys.
- Smaller airways in adolescent boys compared to girls.
- Hormonal fluctuations in pre-menstrual, menstrual, and menopausal stages in women.
- Studies have shown that hormonal changes in post-menopausal women diagnosed with asthma increase.
Consider family history of asthma. Experts have identified 100 genes associated with asthma and allergies. Research conducted on families, especially twins, has shown that asthma can be inherited. A 2009 study found that family history plays a major role in determining whether a person develops asthma. Comparing an average family with a family at high genetic risk for asthma, those at average risk are 2.4 times more likely to develop asthma, and those at high risk are 4.8 times more likely.
- Ask your parents and relatives about any family history of asthma.
- If you were adopted, your biological parents may provide family history information to your adoptive parents.
Record any allergic reactions. Studies have linked a specific immune protein called "IgE" to the development of asthma. If you have high IgE levels, you may be genetically predisposed to allergies. The presence of IgE in the blood can trigger allergic reactions such as airway inflammation, rashes, itching, watery eyes, wheezing, and more.
- Pay attention to allergic reactions triggered by common allergens, such as food, cockroaches, pets, mold, pollen, and dust.
- If you suffer from allergies, you may also be at a higher risk of asthma.
- If you experience severe allergic reactions with no identifiable cause, it's recommended to consult a doctor for testing. Your doctor may conduct a skin test with various allergens to identify allergic sensitivities.
Avoid exposure to cigarette smoke. Inhaled particles from smoke trigger coughing as the body responds, and these particles can also cause inflammation, exacerbating asthma symptoms. The more you're exposed to cigarette smoke, the higher your risk of developing asthma. If you smoke, talk to your doctor about methods and medications to quit. Some options include nicotine gum, gradual reduction, or medications such as Chantix or Wellbutrin. Even if you're struggling to quit, avoid smoking around others, as secondhand smoke can trigger asthma in them.
- Smoking during pregnancy can cause the baby to wheeze, increase the risk of food allergies, and elevate inflammatory proteins in the blood. The effects can worsen if the child continues to inhale secondhand smoke after birth. Consult with an obstetrician before using smoking cessation medications.

Reduce stress. Numerous studies have shown that high stress hormone levels can trigger asthma symptoms, increase sensitivity to allergens, and cause lung constriction. Identify the primary stressors in your life and seek ways to manage or eliminate them.
- Try relaxation techniques such as deep breathing, meditation, and yoga.
- Exercise regularly to boost endorphins, which help reduce pain and stress.
- Improve sleep habits: Go to sleep when you're tired, avoid watching TV in bed, refrain from eating before bedtime, steer clear of caffeine in the evening, and try to maintain a consistent sleep schedule.
Avoid environmental air pollution. Much of the asthma in young children is due to exposure to air pollution from factories, construction sites, vehicles, and industrial plants. Just like tobacco smoke, air pollution irritates the lungs, causing inflammation that damages and constricts the airways. If reducing exposure to air pollution isn't feasible, limit your contact with polluted environments.
- Avoid breathing air near busy streets or highways when possible.
- Encourage children to play in areas away from highways or construction zones.
- If you're considering relocating to the U.S., you can check areas with the best air quality by reviewing the EPA's air quality index guide.

Consider the medications you are taking. If you are on medication, pay attention to any asthma symptoms that appear after starting the medication. If they occur, consult your doctor before stopping, reducing the dosage, or changing the medication.
- Studies have shown that aspirin and ibuprofen can trigger bronchoconstriction and respiratory issues in asthma patients allergic to these substances.
- ACE inhibitors used to treat high blood pressure do not cause asthma but may lead to a dry cough that can be confusing. However, severe coughing caused by ACE inhibitors can irritate the lungs and worsen asthma. Common ACE inhibitors include ramipril and perindopril.
- Beta-blockers used to treat cardiovascular issues, high blood pressure, and migraines can lead to bronchoconstriction and airway narrowing. Some doctors may prescribe beta-blockers even for asthma patients, requiring close monitoring. Common beta-blockers include metoprolol and propranolol.

Maintain a healthy weight. Research has identified a link between weight gain and an increased risk of asthma. Excess weight makes it harder to breathe and reduces blood circulation throughout the body. Additionally, it increases the production of inflammatory proteins (cytokines), making you more susceptible to inflammation and airway constriction.
Recognizing mild to moderate signs and symptoms

See a doctor even if symptoms are mild. Newly appearing symptoms might not yet interfere significantly with your daily life or activities. However, as the condition progresses, you may notice increasing difficulty in performing normal tasks. Many patients experience early symptoms that worsen over time.
- If left undiagnosed or untreated, mild asthma symptoms can worsen. This is particularly true if you haven't identified triggers and taken steps to avoid them.

Be aware of frequent coughing. If you have asthma, your airways become obstructed due to constriction or inflammation caused by the disease. Your body responds by trying to clear the airways through coughing. Coughs due to infection are typically wet with mucus, while asthma-related coughing is dry with little to no mucus.
- If the coughing starts or worsens at night, it could be a sign of asthma. A common asthma symptom is nighttime coughing or a worsening cough immediately after waking up.
- In extreme cases, coughing can last throughout the day.

Listen for sounds during exhalation. Asthma patients often hear a wheezing or whistling sound when exhaling. This occurs because the airways become constricted. Pay attention when you hear such sounds. If the noise is heard toward the end of your breath, it might be an early warning sign of mild asthma. However, if the condition worsens, you will wheeze or whistle even during complete exhalation.

Watch for unusual shortness of breath. "Exercise-induced bronchoconstriction" is a type of asthma that occurs after physical activity, such as exercise. The constriction of the airways makes you feel more fatigued and breathless than usual, and you may need to stop sooner than expected. Compare your usual exercise time before feeling tired and short of breath.

Be aware of rapid breathing. The body increases the rate of respiration to deliver oxygen to constricted lungs. Place your palm on your chest and count the breaths per minute. Use a clock to measure the rate accurately. Normal breathing rate is between 12 and 20 breaths per minute.
- In moderate asthma, the breathing rate may range from 20 to 30 breaths per minute.

Do not ignore cold or flu symptoms. Although asthma-related coughing may differ from that of a cold or flu, bacteria and viruses can trigger asthma symptoms. Pay attention to signs of infection that may lead to asthma symptoms: sneezing, runny nose, sore throat, and congestion. If the cough produces black, green, or white mucus, you may have a bacterial infection. If the mucus is clear or white, it may be caused by a virus.
- If you notice these infection symptoms alongside wheezing and shortness of breath, you might be experiencing asthma triggered by infection.
- Consult a doctor to determine the exact cause.
Recognizing severe symptoms

Seek medical attention if you are unable to breathe, even during times of rest. Typically, shortness of breath in asthma patients due to heavy activity improves with adequate rest. However, if symptoms worsen or if you experience breathing difficulties during rest, it could be due to inflammation caused by triggers. If inflammation intensifies, you may struggle to breathe deeply or experience sudden breathlessness.
- You may feel unable to fully exhale. Your body will shorten the exhalation phase in order to inhale more oxygen more quickly.
- You may not be able to complete a sentence and will need to take short breaths in between words.

Check your breathing rate. Even mild to moderate asthma can cause rapid breathing, but severe cases can be dangerous. When the airways constrict, it becomes harder to inhale fresh air, leading to oxygen deficiency. Rapid breathing is the body's attempt to intake more oxygen in an effort to manage the situation before any damage occurs.
- Place your palm on your chest and note your breathing rate for one minute. Use a clock to measure the rate accurately.
- In severe asthma, the respiratory rate can exceed 30 breaths per minute.

Measure your pulse. Oxygenated blood circulates throughout the body to deliver oxygen to tissues and organs. In severe asthma, insufficient oxygen intake forces the heart to pump faster to distribute more oxygen. You may notice an increased heart rate during asthma attacks.
- Extend your hand, palm facing up.
- Place the index and middle fingers of your other hand on the outer side of your wrist, just below the thumb.
- You will feel the pulse from the radial artery.
- Count the beats for one minute. A normal heart rate is under 100 beats per minute, but during severe asthma, it can rise up to 120 beats per minute.
- Most smartphones now have built-in heart rate monitors. You can use this feature if available.

Be aware of pale blue coloring. Blood is bright red when oxygenated, and dark red when deoxygenated. Oxygen exposure turns blood red, so this often goes unnoticed. However, during severe asthma, you may experience "cyanosis"—a condition where deoxygenated blood flows through arteries, causing the skin to appear pale blue or gray, particularly around the lips, fingertips, nails, gums, or thin skin around the eyes.
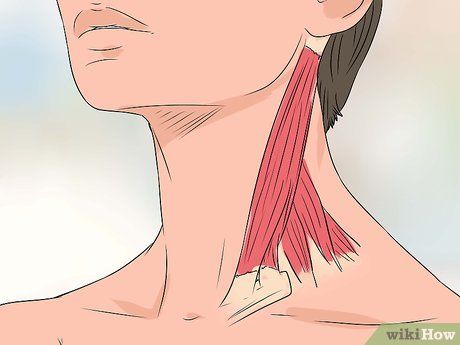
Observe for neck and chest muscle tightness. During deep breathing or respiratory distress, accessory muscles (not normally used for breathing) are engaged. These muscles are located in the neck, including the sternocleidomastoid and scalene muscles. Look for defined indentations in the neck muscles when struggling to breathe. Additionally, the intercostal muscles between the ribs may contract. These muscles help lift the rib cage during inhalation, and you may notice these contractions between the ribs during severe asthma symptoms.
- Use a mirror to observe for deep indentations in the neck muscles and contractions between the ribs.

Be aware of chest pain. When struggling to breathe, the muscles involved in respiration can become overworked. This leads to muscle fatigue in the chest, causing a feeling of tightness or pain. The pain can be dull, sharp, or stabbing, often located at or near the sternum. This condition requires immediate medical attention to rule out cardiovascular issues.
Notice any unusual sounds while breathing. With mild to moderate asthma, you may hear a wheezing or whistling sound while exhaling. However, in severe cases, you may hear sounds during both inhalation and exhalation. The whistling sound during inhalation is known as "inspiratory wheezing" and is caused by narrowing in the upper airways. Wheezing during exhalation is typically due to constriction in the lower airways.
- A wheezing sound while inhaling may indicate asthma or a severe allergic reaction. It is important to differentiate between the two causes to pinpoint the right diagnosis.
- Look out for hives or a red rash on the chest, which could signal an allergic reaction rather than asthma. Swelling of the lips or tongue also suggests an allergic response.

Address asthma symptoms promptly. If severe asthma leads to breathing difficulties, you should seek emergency medical care or head to the hospital immediately. Without a diagnosis, you may not have a preventative inhaler, but if you do, use it right away.
- Albuterol inhalers should typically be used no more than 4 times per day, but during an asthma attack, you may use it every 20 minutes for up to 2 hours.
- Breathe slowly and deeply, counting to 3 as you inhale and exhale. This helps reduce anxiety and regulate your breathing rhythm.
- Avoid triggers if you can identify them.
- Your asthma symptoms will improve with prescribed steroids. These medications can be administered through an inhaler or in pill form. Take the medication with water and wait a few hours for it to take effect, although symptoms can still be managed in the meantime.
Call for emergency help in severe asthma cases. These symptoms indicate an acute asthma attack, where your body is desperately trying to inhale as much air as possible to maintain function. This is considered an emergency that could be life-threatening if not treated promptly.
Proceed with diagnosis
Provide your medical history to the doctor. The information must be accurate to help the doctor identify the factors affecting you. Prepare this information beforehand so that you don't waste time thinking when you visit the clinic:
- Any signs or symptoms of asthma (coughing, shortness of breath, wheezing, etc.)
- Personal medical history (previous allergies, etc.)
- Family history (lung conditions or allergies in parents or siblings, etc.)
- Social history (smoking, diet, exercise, environment)
- Current medications (such as aspirin) and supplements or vitamins you are taking

Undergo a health check-up. The doctor may examine part or all of the following areas: ears, eyes, nose, throat, skin, chest, and lungs. Using a stethoscope, the doctor will listen to your lungs, noting any sounds or absence of sounds in the chest.
- As asthma is often linked to allergies, the doctor will check for symptoms like a runny nose, red eyes, watery eyes, and skin rashes.
- Finally, the doctor will examine your throat for signs of swelling and breathing capacity, as well as any abnormal sounds indicating airway constriction.
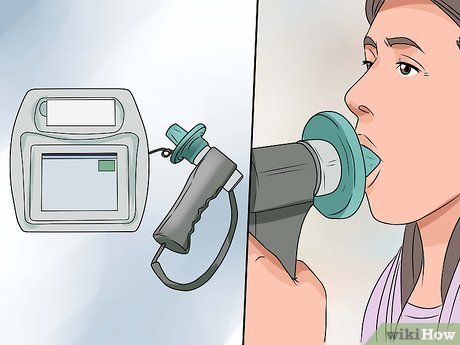
Ask the doctor to confirm the diagnosis with a spirometry test. During this test, you will breathe into a device called a spirometer to measure air flow and the amount of air you inhale and exhale. Inhale deeply and exhale forcefully for as long as possible while the device measures your airflow. A positive result confirms asthma, but a negative result does not rule out this condition.

Undergo a peak flow test. This method is similar to spirometry and measures the amount of air you can exhale. The doctor may recommend this test to help make an accurate diagnosis. To perform the test, place your mouth on the device, ensuring it is calibrated to zero. Stand up straight, take a deep breath, and then exhale forcefully and quickly in one breath. Repeat several times to obtain consistent results. The highest value is your peak flow. When you feel an asthma attack approaching, repeat the test and compare the peak flow value with your maximum reading.
- If the peak flow is over 80%, you're in the safe range.
- If the peak flow is between 50% and 80%, your asthma is not well-controlled, and the doctor may prescribe medication. You are at moderate risk of an asthma attack in this range.
- If the peak flow is below 50%, you're experiencing severe respiratory distress and need medication for treatment.
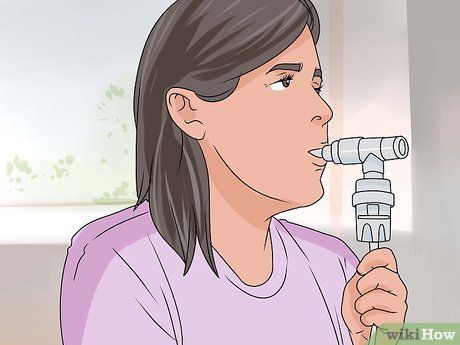
Ask the doctor to perform a methacholine allergy test. If you do not have symptoms during your clinic visit, it may be difficult for the doctor to make a precise diagnosis. In this case, the doctor may recommend a methacholine allergy test using a methacholine inhaler. Methacholine causes airway constriction if you have asthma, and it triggers symptoms that can be measured using spirometry and the peak flow test.

Test for asthma medication response. Sometimes, doctors may skip certain tests and simply prescribe asthma medication to assess the condition. If symptoms gradually improve, it is possible that you have asthma. The doctor will prescribe medication based on the severity of symptoms, medical history, and health check-up results.
- A commonly prescribed medication is the albuterol/salbutamol inhaler, which is used by pursing your lips around the mouthpiece and inhaling the medication into your lungs.
- Bronchodilators work by relaxing the constricted airways, thereby opening them up.
Advice
- Visit an allergy specialist to identify the underlying causes of your allergies. Identifying allergens can help you avoid asthma attacks triggered by those substances.
Warnings
- If any symptoms appear, seek medical attention promptly.
