Stroke is the third leading cause of death in the United States and can cause lifelong complications and disabilities. It is considered a medical emergency that requires immediate treatment. Learning to recognize stroke signs is essential because timely assistance can ensure proper treatment and reduce the likelihood of disability for the patient.
Steps
Pay attention to the signs of a stroke

Recognize stroke symptoms. There are several warning signs that someone may be about to experience a stroke, including the sudden onset of the following:
- numbness or weakness in the face, arm, or leg, especially on one side of the body. One side of the face may droop when the person tries to smile
- confusion, trouble speaking, or difficulty understanding others, slurred speech
- vision problems in one or both eyes, sudden darkness or double vision
- severe headache, usually unexplained, possibly accompanied by nausea or vomiting
- difficulty walking, loss of balance or coordination, along with dizziness

Pay attention to the specific symptoms in women. In addition to common stroke symptoms, women may exhibit unique signs. These symptoms include:
- Weakness
- Shortness of breath
- Sudden behavioral changes or agitation
- Nausea and vomiting
- Hiccups
- Hallucinations

Check for stroke signs using the ‘FAST’ method. FAST is an acronym that helps remember how to check for stroke symptoms.
- F- FACE: Ask the person to smile. Does one side of their face droop?
- A- ARMS: Ask the person to raise both arms. Does one arm fall?
- S- SPEECH: Ask the person to repeat simple phrases. Is their speech slurred or unusual?
- T- TIME: If you notice any of these signs, immediately call emergency services at 115.

Seek immediate medical help. If you suspect a stroke, call emergency services at 115 right away. Every minute without treatment counts. For each minute delayed, the victim may lose 1.9 million brain cells, decreasing the chances of recovery and increasing the risk of complications or death.
- Furthermore, there is a small ‘treatment window’ (the golden period) for ischemic strokes, making it critical to reach a hospital as soon as possible.
- Some hospitals have specialized units for stroke treatment. If you're at risk of a stroke, it's helpful to know the locations of these centers.
Know the risk factors

Evaluate health status. Stroke can happen to anyone; however, certain individuals are at higher risk. Discuss with your doctor about high-risk factors for stroke due to conditions such as:
- Diabetes
- Heart diseases like atrial fibrillation (a-fib) or stenosis
- Previous strokes or transient ischemic attacks (TIA)

Consider your lifestyle habits. If your lifestyle does not prioritize exercise and healthy eating, you are at a higher risk of having a stroke. Some habits that may increase your stroke risk include:
- Being overweight or obese
- Physical inactivity
- Excessive alcohol consumption or substance abuse
- Smoking
- High blood pressure
- High cholesterol

Learn about genetic factors. Some risks are unavoidable and may be related to your genetic background. These factors include:
- Age: Stroke risk doubles every 10 years after the age of 55
- Race or ethnicity: African Americans, Latinos, and Asians are at a higher risk of stroke
- Women are at a slightly higher risk
- Family history of stroke
Identify other risk factors if you're a woman. There are additional factors that may affect the stroke risk in women. These include:
- Birth control: Oral contraceptives can increase stroke risk, especially when combined with other risk factors like smoking or high blood pressure
- Pregnancy: Pregnancy raises blood pressure and puts more strain on the heart
- Hormone replacement therapy (HRT): Women who use hormone therapy to alleviate menopause symptoms may face higher stroke risks
- Migraines with aura: Women are more likely to experience migraines, which are associated with a higher risk of stroke.
Understand strokes
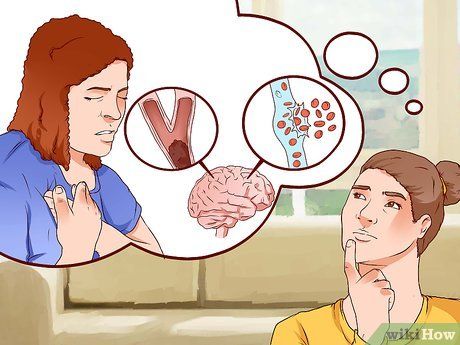
Know how a stroke occurs. A stroke happens when the blood flow that delivers oxygen and nutrients to the brain is blocked or reduced. This can cause brain cells to begin dying almost immediately. Prolonged lack of blood supply can lead to brain death, resulting in long-term disability.
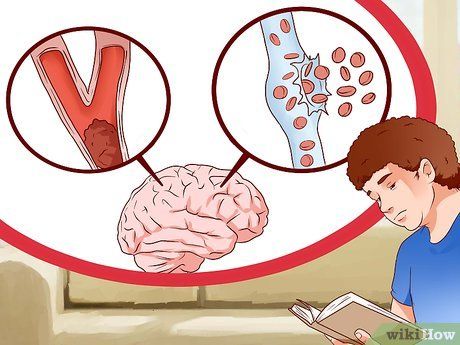
Understanding the Two Types of Strokes. Most stroke cases are categorized into two types: ischemic and hemorrhagic. Ischemic stroke occurs when blood clots block the flow of blood. Around 80% of stroke cases are ischemic. Hemorrhagic stroke happens when a weak blood vessel in the brain bursts, causing bleeding inside the brain.
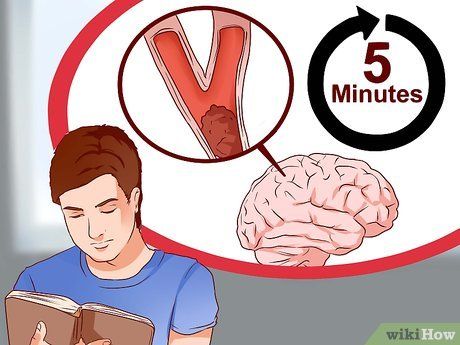
Learn About Transient Ischemic Attacks. Also known as TIAs, these are mild strokes. It occurs when blood flow to the brain is temporarily blocked. For instance, a small moving blood clot might briefly obstruct a blood vessel. Although the symptoms resemble those of a more severe stroke, ischemic strokes in this case last for a shorter duration, typically under 5 minutes. The symptoms appear and disappear within 24 hours.
- However, you cannot determine if you're experiencing a TIA or a full stroke just by the duration or symptoms.
- Regardless of the situation, it's essential to call emergency services, as TIAs are a warning sign for a potential future stroke.

Awareness of Disabilities Caused by Stroke. Stroke-related disabilities can include movement problems (paralysis), cognitive difficulties, speech issues, memory loss, and more. The severity of these impairments can vary, depending on the stroke's seriousness (such as the size of the blood clot, extent of brain damage) and how quickly the patient receives treatment.
Warning
- Make sure to note the time when symptoms first appear. This information is crucial for doctors when treating the patient.
- Keep a phone nearby or within reach. When any of the stroke symptoms are present, you must immediately call emergency services.
- The patient might only display one symptom of a stroke. Nonetheless, seeking urgent medical attention remains extremely important.
