If you suspect you have diabetes, it’s essential to consult a healthcare professional immediately. Type 1 diabetes occurs when the pancreas' cells fail to produce insulin; this autoimmune condition impairs the pancreas’ function. Type 2 diabetes is often associated with lifestyle factors (such as lack of physical activity and excessive sugar consumption). Recognizing the symptoms and understanding how diabetes is diagnosed are crucial for early treatment.
Steps
Identifying the Signs and Symptoms of Diabetes
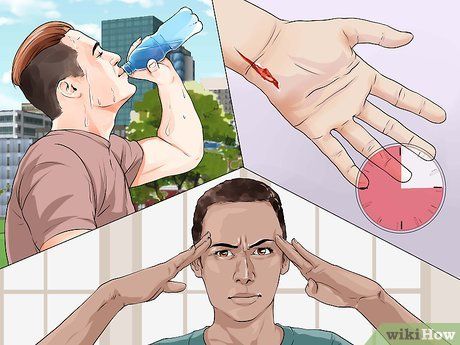
Be cautious of the following signs and symptoms. If you experience more than two of the symptoms listed below, it’s advisable to seek medical attention for further evaluation. Common signs and symptoms of both Type 1 and Type 2 diabetes include:
- Excessive thirst
- Severe hunger
- Blurred vision
- Frequent urination (waking up more than three times a night to urinate)
- Fatigue (especially after meals)
- Irritability
- Wounds that don’t heal or take a long time to heal
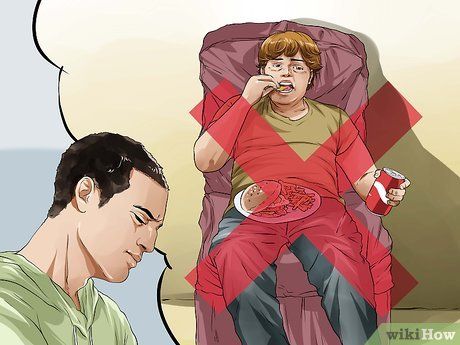
Be mindful of lifestyle choices. People who lead a sedentary lifestyle (little or no physical activity) are at higher risk for Type 2 diabetes. Overweight or obese individuals, as well as those who consume large amounts of sugary foods and refined carbohydrates, have a significantly higher risk of developing Type 2 diabetes.
- Note that Type 2 diabetes is usually caused by unhealthy lifestyle choices, in contrast to Type 1 diabetes – a congenital condition that has existed since childhood due to the pancreas' inability to use insulin because of a lack of beta cells.

Get a medical checkup. The only way to definitively determine whether you have diabetes is to undergo medical testing (blood tests). The blood test results classify your condition as "normal", "prediabetes" (meaning there’s a high risk of developing diabetes if lifestyle changes are not made), or "diabetes".
- It’s best to find out whether you have diabetes as soon as possible, as early treatment is crucial.
- Uncontrolled blood sugar levels can have long-term health effects. If blood sugar is managed through treatment, many of the long-term consequences of diabetes can be prevented or at least delayed. Hence, timely diagnosis and treatment are of utmost importance.
Diabetes Diagnosis Tests

Take the test with your doctor. Your doctor may perform two different tests to check your blood glucose levels. Typically, a fasting blood glucose test is used to diagnose diabetes, but your doctor may also conduct a urine test.
- Normal blood glucose levels range from 70 to 100.
- If in the "prediabetes" stage, blood glucose levels will range from 100 to 125.
- Blood glucose levels above 126 are considered diabetic. Fasting blood glucose or random blood glucose levels of 200 or higher may also be indicative of diabetes.
- Note that HbA1c tests are not perfect diagnostic tools. Conditions like iron deficiency anemia and chronic anemia can cause inaccurate results.

Measure HbA1c levels (hemoglobin A1c). This is a newer test used by doctors to diagnose diabetes. It measures the amount of sugar attached to hemoglobin (a type of protein) in red blood cells. The higher the level, the more sugar is attached, indicating a higher risk for diabetes. After all, diabetes is characterized by an increase in blood sugar levels.
- The typical correlation between HbA1c levels and average blood glucose levels is as follows: An HbA1c of 6 corresponds to a blood glucose level of 135; HbA1c of 7 = 170; HbA1c of 8 = 205; HbA1c of 9 = 240; HbA1c of 10 = 275; HbA1c of 11 = 301; HbA1c of 12 = 345.
- In most laboratories, the normal range for HbA1c is 4.0% - 5.9%. In poorly controlled diabetes, the range is 8.0% or higher, while well-controlled diabetes is under 7.0%.
- Measuring HbA1c provides a more accurate reflection of your condition, as it reflects the average blood sugar levels over the past 3 months, unlike the glucose test, which measures blood sugar levels at a single point in time.

Diabetes Treatment. To manage diabetes, you need to take insulin injections or medication daily, along with controlling your diet and exercising.
- In some mild cases of Type 2 diabetes, adjusting your diet and exercise routine may be enough. Adopting the right lifestyle changes can significantly help in managing diabetes and normalizing blood sugar levels. This is the motivation you need to make lifestyle changes for diabetes treatment.
- Your doctor will recommend reducing sugar and carbohydrate intake, along with 30 minutes of exercise daily. If followed correctly, you will notice a significant reduction in blood sugar levels.
- On the other hand, individuals with Type 1 diabetes always need insulin injections, as this autoimmune disease prevents the body from producing insulin.
- Proper treatment of diabetes is crucial. If left untreated, high blood sugar levels can lead to more severe health issues such as nerve damage, kidney damage or failure, blindness, and serious circulation problems that may lead to infections hard to treat (which could progress into necrosis requiring amputation, especially in the lower limbs).

Regular Check-ups. You should get a blood test every 3 months if you fall into the "prediabetes" or "diabetes" category. Regular testing helps track whether your condition is improving (for those who have made positive lifestyle changes) or worsening.
- Blood tests also help your doctor adjust insulin doses and oral medication. The goal is to keep your blood sugar within a specific range, so the numerical data from regular blood tests is very important.
- Routine blood tests also serve as motivation to stay active and maintain a healthy diet, which will lead to visible results in your next blood test.
- If you are in the prediabetes range or managing your diabetes well, you may only need testing every 6 months. However, if your diabetes is not well controlled, your doctor may recommend testing every 3 to 4 months.
