Tetanus may be a common term, but do you know when it’s necessary to get the tetanus vaccine? In countries like the U.S. and other developed nations, tetanus is rare due to high vaccination rates. Vaccination plays a crucial role because, to this day, tetanus has no cure. The disease is caused by toxins from bacteria found in dirt, dust, and animal waste. These harmful bacteria exist in spore form, making them difficult to destroy as they can survive high temperatures and resist many medicines and chemicals. Tetanus bacteria attack the nervous system and cause intense pain through muscle spasms, especially in the jaw and neck. It can also cause suffocation and lead to death. For these reasons, knowing when to get a tetanus shot is of utmost importance.
Steps
Knowing the Right Time for Tetanus Vaccination
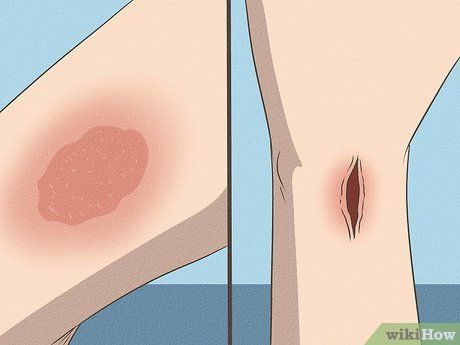
Get a booster shot if you suffer from certain types of injuries. Typically, the bacteria’s toxins enter the body through cuts caused by objects contaminated with tetanus spores. If you experience an injury or wound that makes tetanus infection more likely, you should receive a booster shot. These injuries include:
- Any wound contaminated by dirt, dust, or horse manure.
- Puncture wounds. Objects that can cause these include wood splinters, nails, needles, glass, or bites from people or animals.
- Burns. Second-degree burns (localized or blistering burns) and third-degree burns (full-thickness burns) have a higher risk of infection compared to first-degree burns (surface-level burns).
- Crush injuries that lead to tissue damage from being trapped between heavy objects. These can also happen when a body part is struck by a falling heavy object.
- Wounds involving necrotic tissue. Without blood circulation, necrotic tissue is more prone to infection, especially in cases of severe injury. For example, areas with dead tissue (necrosis) carry a higher infection risk.
- Injuries with foreign objects. Wounds containing debris like glass shards, gravel, or other materials are at a higher risk of infection.
How to determine if it's time for a tetanus shot. If you've never received the full tetanus vaccination series (the primary series) or are unsure when your last dose was, it's time to get a tetanus shot. After an injury, you may wonder if a booster shot is necessary. You should get one if:
- Your wound was caused by a "clean" object, but your last tetanus shot was over 10 years ago.
- Your wound was caused by a "dirty" object, and your last tetanus shot was over 5 years ago.
- You aren't sure if the object that caused the injury was "clean" or "dirty," and your last tetanus shot was more than 5 years ago.

Tetanus vaccination during pregnancy. To transfer tetanus antibodies to your unborn child, it is recommended to get vaccinated during pregnancy between 27 to 36 weeks.
- Your doctor may suggest the Tdap vaccine (tetanus, diphtheria, and pertussis) during the third trimester of your pregnancy.
- If you haven't received the Tdap vaccine before and didn't get it during pregnancy, you should get it right after giving birth.
- If you have a cut or dirty wound during pregnancy, you should get a tetanus booster shot.
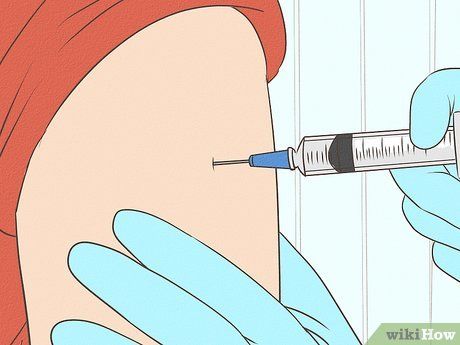
Becoming immune. The best way to "treat" tetanus is to prevent it in the first place. Although mild reactions to the vaccine are common, serious side effects are extremely rare. Typical reactions include swelling, pain, and redness at the injection site, but these usually resolve within 1-2 days. Don't worry about getting an additional booster shot. Generally, there’s no issue if you don't wait a full 10 years for your next dose. Some tetanus vaccines include:
- DTaP. The diphtheria, tetanus, and pertussis vaccine (for prolonged cough) is typically given to children at 2, 4, and 6 months of age, with a booster shot at 15 to 18 months. DTaP is particularly effective for young children, who often need a booster shot between 4 to 6 years old.
- Tdap. Over time, immunity to tetanus decreases, so older children need a booster shot. The booster contains a full dose of tetanus vaccine and reduced doses of diphtheria and pertussis. Anyone aged 11 to 18 is recommended to receive the booster, with the ideal age being 11 or 12 years old.
- Td. For adults, a Td booster (tetanus and diphtheria) is recommended every 10 years to maintain immunity. As antibody levels decrease after 5 years, it’s advised to get a booster shot if you have a deep wound, infection, or haven't been vaccinated in more than 5 years.
Recognizing and Identifying Tetanus

Learn about those most at risk for tetanus and how it spreads. Almost all cases of tetanus occur in people who have never been vaccinated or in adults who don't follow the recommended 10-year booster schedule. However, unlike other vaccine-preventable diseases, tetanus is not contagious. Instead, it spreads through bacterial spores that usually enter the body through open wounds. These spores produce a potent neurotoxin that causes muscle spasms and stiffness.
- Complications from tetanus are most common in unvaccinated individuals or adults without adequate immunity, especially in industrialized countries.
- You may also be at risk for tetanus after natural disasters, particularly in developing countries.
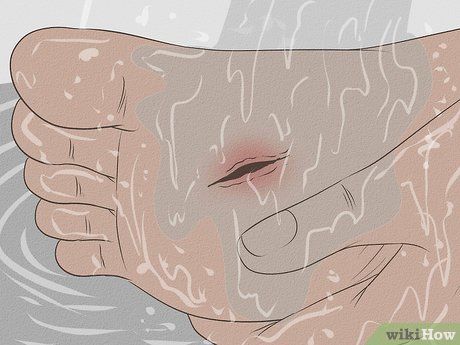
Reduce the Risk of Tetanus. When you sustain an injury or trauma, it’s important to clean and disinfect the wound promptly. Delaying this process beyond 4 hours increases the risk of developing tetanus. This becomes even more critical when the injury is caused by an object that punctures the skin, introducing bacteria and debris deep into the wound, creating an ideal environment for tetanus bacteria to thrive.
- Consider the cleanliness of the object that caused the injury to assess the need for a booster shot. Dirty or contaminated objects can carry dirt, saliva, or fecal matter, while clean objects are less likely to be contaminated. Remember, it's not always possible to know for sure whether the object harbors bacteria.
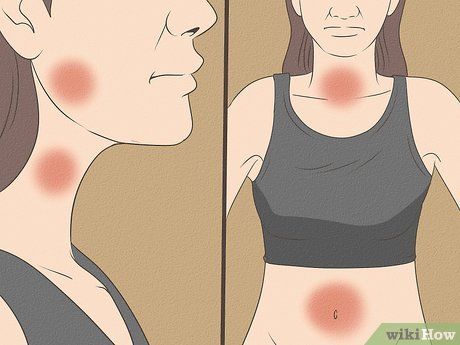
Pay Attention to Symptoms. The incubation period for tetanus can vary, ranging from 3 to 21 days, with an average of 8 days. The severity of tetanus is classified on a scale from I to IV, and longer incubation periods often correlate with milder forms of the disease. Common tetanus symptoms (in the order of appearance) include:
- Jaw muscle spasms (often referred to as 'lockjaw')
- Stiff neck
- Difficult swallowing (dysphagia)
- Rigid abdominal muscles

Recognize Other Tetanus Symptoms. Symptoms are the sole basis for diagnosing tetanus, as no blood test can confirm the condition. Therefore, it is crucial to recognize every symptom. You may also experience fever, sweating, high blood pressure, or a rapid heartbeat (tachycardia). Possible complications include:
- Laryngeal spasms or vocal cord tightening leading to breathing difficulties
- Bone fractures
- Seizures
- Irregular heart rhythm
- Secondary infections like pneumonia due to prolonged illness
- Pulmonary embolism or blood clots in the lungs
- Death (accounting for 10% of recorded cases)
Tetanus Treatment
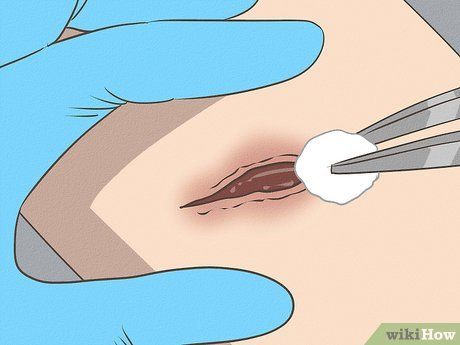
Medical Care. If you suspect or even think you might have tetanus, seek medical care immediately. This is an emergency situation, and hospitalization is required since tetanus has a high mortality rate (10%). In the hospital, you will receive tetanus immune globulin, which helps neutralize any toxins that haven’t yet attacked your nerve cells. The wound will be thoroughly cleaned, and you will receive a tetanus vaccination to prevent future infections.
- Having tetanus does not make you immune to it in the future. In fact, to avoid reinfection, you will need a tetanus vaccination.

Let the doctor determine your treatment plan. No blood test can diagnose tetanus, so laboratory tests are not helpful for evaluating this condition. As a result, most doctors opt for immediate treatment when there is a suspicion of infection, rather than waiting and monitoring.
- Doctors mainly base their diagnosis on the current symptoms and clinical signs. The more severe the symptoms, the more urgent the treatment.

Treating Tetanus Symptoms. As there is no cure for tetanus, treatment focuses on addressing the symptoms and complications associated with it. You will be administered antibiotics and muscle spasm control medications either orally, via injection, or intravenously.
- Some muscle relaxants include pain medications from the benzodiazepine class (such as diazepam (Valium), lorazepam (Ativan), alprazolam (Xanax), and midazolam (Versed)).
- Antibiotics are generally ineffective for treating tetanus, but they may be prescribed to inhibit the growth of Clostridium tetani bacteria, thus slowing toxin production.
Advice
- There is a vaccine that protects against both diphtheria and pertussis (Tdap), as well as one that only protects against diphtheria (Td). Both types are effective for 10 years.
- The date of your last booster shot is recorded in your vaccination records at your doctor's office. You can request this information from your doctor on your personal immunization card.
- If you are at risk for infection, ensure you are familiar with the signs and complications of tetanus. Muscle spasms can become severe enough to impair normal breathing. Seizures may be severe enough to cause spinal or long bone fractures.
- Better safe than sorry—if you’re particularly concerned about a potential tetanus infection, consider getting vaccinated.
- A few rare conditions may exhibit similar symptoms to tetanus. Malignant hyperthermia is a genetic disorder that causes rapid fever and severe muscle spasms during anesthesia. Stiff-Person Syndrome is an extremely rare neurological condition that causes periodic muscle contractions. Symptoms of this condition usually begin around the age of 45.
Warning
- Seek emergency care immediately for any severe injury or wound. If you suspect tetanus infection, do not wait for symptoms to appear before receiving appropriate treatment. Tetanus is incurable, and currently, we can only manage the symptoms until the condition resolves itself.
