Preparing baby cereal with formula milk or breast milk is an important transition step that parents of young children often take to introduce solid food. Typically, babies begin eating cereal mixed with formula around 4 to 6 months of age. This timing may vary depending on a doctor’s advice and the child’s developmental milestones.
Steps
Ensure the baby is ready for solid foods.

Wait until the baby is 4 to 6 months old. A baby’s digestive system isn’t ready to handle cereal until around 6 months of age. Introducing solids too early can increase the risk of choking or inhaling food into the lungs. Early exposure to cereals may also raise the risk of food allergies.
- Most babies are ready for cereal around 4 months old. Your doctor can help you determine what’s best for your baby.
- If your baby has reflux, you might start solid foods earlier, but always consult your pediatrician first.
- Your baby should be able to eat from a spoon before you introduce solid foods.
- Introducing solids too early can lead to excessive weight gain in babies.

Ensure your baby has reached the necessary developmental milestones. In addition to being the right age, your baby must also meet certain developmental milestones before being introduced to cereal. Your baby should be able to sit up with support, control their head and neck, lift their body while lying down, bring their hands or toys to their mouth, lean forward and open their mouth when hungry or craving food. If your baby is 6 months old but hasn’t met these milestones yet, you might want to wait before introducing solids.
- It's crucial for the baby to achieve these milestones as it ensures they can swallow cereal safely.
- Infants naturally have a reflex that pushes things out of their mouth. This reflex occurs when the tongue lifts and pushes any object placed between their lips. This reflex usually disappears between 4 and 6 months. You will find it very challenging to feed a baby with a spoon while this reflex is still present.

Consult with your pediatrician or general practitioner. It's important to discuss with a healthcare provider before introducing solid foods to your baby. The doctor will assess if your baby is ready to tolerate solids. This is also a good time to ask any remaining questions you have about introducing solids.
- In some cases, your baby’s digestive system may not be fully developed, or they may not recognize when they are full, leading to overeating.
- Don’t introduce solids to your baby before the doctor confirms that it’s appropriate.
Mixing baby cereal into a bottle.

Seek advice from your pediatrician. Avoid mixing baby cereal into a bottle unless your pediatrician advises you to do so. This method is generally recommended only for babies with gastroesophageal reflux. If you feed your baby cereal from a bottle, they may struggle to learn how to eat from a spoon, and it could increase the risk of overeating, leading to excess weight gain.
- To reduce reflux, keep your baby upright (such as holding them against your shoulder) for 20 to 30 minutes after feeding.
- Try using pre-mixed formula specifically designed for "reflux control". These formulas typically contain rice starch.
- Consider giving your baby a formula that is less likely to cause allergies, such as one without cow’s milk or soy milk, and see if it helps with the reflux. Use this formula for one or two weeks.
- The American Academy of Pediatrics does not recommend adding cereal to a bottle, but your pediatrician is the best source of advice on whether this is suitable for your child.

Mixing baby cereal into a bottle. Start by adding one teaspoon of cereal for every 6 teaspoons of formula. Mix the cereal just before you plan to feed your baby. The mixture will continue to thicken if left to sit.
- Your pediatrician may recommend a different ratio of cereal to formula.
- You can add up to one tablespoon of baby cereal to the bottle.

Give your baby cereal milk at night. It's recommended to offer your baby cereal milk during the late evening. This helps the baby sleep longer, as the baby feels fuller for a longer period. You may need to slightly enlarge the hole in the nipple of the bottle, as the mixture will be thicker than regular milk.
- Don't feed your baby cereal at every meal. Baby cereal is primarily composed of carbohydrates, which don't provide as many nutrients as formula or breast milk. Offering cereal at all meals may reduce the overall nutritional value your baby receives.
- You can either cut an "X" or "Y" shape on the bottle nipple or purchase a larger nipple that suits the consistency of the cereal formula.
Monitor your baby’s reaction. Observe how your baby swallows the cereal. If the mixture seems too thick, your baby may have difficulty swallowing it and may tire out during feeding. Also, watch for signs of constipation or excessive weight gain, which can be side effects of the cereal diet.
- Adjust the amount of cereal based on your observations of your baby’s response.
- If your baby gets constipated from rice cereal, you can try switching to oatmeal cereal.
- If you're treating reflux, you may see improvement within 2 or 3 days. If there is no change after this period, cereal may not be the right solution for your baby.
Feeding your baby cereal with a spoon.

Mix baby cereal with formula milk. Check the instructions on the packaging to prepare the cereal. Typically, you will mix 1 tablespoon (15 ml) of cereal for every 4 tablespoons (60 ml) of formula or breast milk. For example, if your baby is currently consuming 8 tablespoons of formula, you would mix in 2 tablespoons of baby cereal.
- Stir the mixture well until it reaches a consistency similar to diluted milk or soup.
- If you are using pre-mixed cereal with formula, follow the packaging instructions. Many brands only require adding water.

Feed your baby the cereal mixture with a spoon. Even though the mixture may seem as thin as milk, you should still feed your baby with a small spoon. Feeding with a spoon helps avoid overfeeding and excessive calorie intake.
- Your baby is used to drinking from a bottle, and instinctively they will know how much to consume based on the amount in the bottle. However, when introducing cereal, your baby may have trouble understanding when to stop eating.
- Alternatively, you can add a little formula into the cereal mixture to keep it at its original consistency. This is a good way to help your baby transition to eating solid food.

Start with small portions when introducing solids to your baby. The first solid food meal should be diluted, and you can gradually make it thicker over time. Begin by giving your baby 1 teaspoon (5 ml) of the mixture after a breastfeeding or bottle-feeding session, then slowly increase the amount to 1-4 tablespoons (15-60 ml) twice a day. This gradual process helps your infant develop their swallowing skills.
- Place the spoon near your baby's lips so they can smell and taste the cereal. Initially, they may not want to eat it.
- If your baby refuses or dislikes the solid food mixture, try again the following day. You can also try making it more diluted.
- Your baby may spit out the food initially, as it is a natural reflex.
- Try breastfeeding or bottle-feeding, followed by spoon-feeding, then continue with breastfeeding or bottle-feeding.
- You can gradually thicken the mixture once your baby has tolerated the solid food for 3-5 days.
- Your baby may vomit after the first few attempts, but don't worry—just try feeding them again the next day.
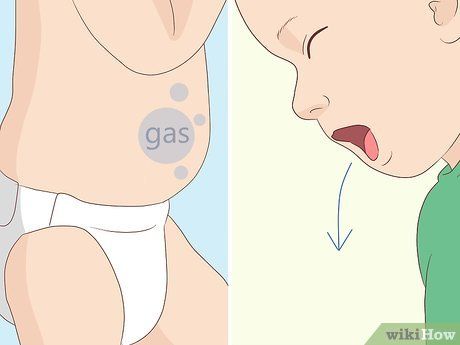
Watch for signs of allergies. Infants who are allergic to solid food may experience bloating, vomiting, or diarrhea. If any of these symptoms occur, stop feeding the mixture and consult a doctor. If your baby develops a rash or has trouble breathing after eating, take them to the doctor immediately.
- Babies are at higher risk of allergies if there is a family history of allergies, eczema, or asthma.
- Inform your doctor about your family's food allergy history when discussing your baby's introduction to solid foods.
Consider using alternative baby food options.

Avoid arsenic in rice. Most rice-based baby foods are made from processed white rice, which contains higher levels of arsenic compared to other grains. Arsenic is a carcinogen and can cause health problems later on. If you're concerned about arsenic exposure, you can opt for baby food made from other grains, such as oats, quinoa, wheat, and barley.
- Whole grains not only reduce the risk of arsenic exposure but also provide more fiber and nutrition than white rice-based baby food.
- The American Academy of Pediatrics recommends replacing rice-based baby food with oat-based options.

Introduce different foods to your baby. While cereals are the most common first food for babies, you can also introduce other foods. Finely minced meat and pureed vegetables can be great first solid foods. Mashed avocado and cooked pears are also excellent options for a first meal.
- Cereal is the traditional choice for first solid foods, but you are free to choose other options.
- Whatever food you choose, ensure it does not contain added sugar or salt.
- Wait two or three days before introducing a new food to your baby.
Advice
- If you are unsure or have any questions, consult a pediatrician for guidance.
Warning
- Do not mix baby food with formula milk in a bottle unless instructed by a pediatrician. Feeding baby food in a bottle can pose risks such as choking and overeating.
What You Need
- Pre-prepared formula milk or breast milk
- Baby cereal powder
- Baby spoon
- Small bowl
