Blood clots, whether they form in the arteries or the lungs, fall into the category of "venous thrombosis" (VT). The symptoms and effects of blood clots vary depending on where they occur in the body. However, all blood clots pose a risk of fatality if left untreated, including conditions like heart disease and stroke. It is crucial to educate yourself on how to prevent blood clots from forming in the first place.
Steps
Understand the Risk Factors

Be extra vigilant as you age. The initial risk of a blood clot is 100 per 100,000 people. However, this risk increases exponentially with age: at 80 years old, the rate of venous thrombosis rises to 500 per 100,000. Therefore, it is important to get regular check-ups to monitor your overall health.
- Surgical procedures or hip and leg fractures can also elevate the risk of blood clot formation.

Consider your activity level. Individuals with a sedentary or inactive lifestyle are at a higher risk of pulmonary embolism, or blood clots in the lungs. Those who sit for over 6 hours a day are twice as likely to experience pulmonary embolism compared to those who sit for less than 2 hours. Sitting, lying, or standing for extended periods can cause blood to pool, leading to the formation of clots. This is why venous thrombosis is commonly seen in hospitalized patients, especially post-surgery, and in long-distance travelers.

Calculate your Body Mass Index (BMI). Individuals in the obese category have a higher risk of venous thrombosis compared to those with a healthy weight. Although the exact correlation isn't fully understood, experts believe that part of this is due to estrogen produced by fat cells. Estrogen is an independent risk factor for blood clots. Fat cells also produce the cytokine protein, which plays a key role in the formation of venous thrombosis. Although not always the case, obesity may also lead to a sedentary lifestyle compared to those with a healthy weight.
- You can calculate BMI using an online tool. Just enter your age, height, weight, and gender to get the result.
- Obese individuals will have a BMI of 30 or higher. The overweight category ranges from 25 to 29.9, and normal weight is between 18.5 and 24.9. A BMI below 18.5 is considered underweight.
Pay attention to hormone levels. Hormonal changes, particularly estrogen, can increase the risk of venous thrombosis. This is commonly seen in premenopausal women who take estrogen as part of hormone replacement therapy. Women using hormonal birth control or pregnant women are also at higher risk.
- Before starting any hormone therapy, consult your doctor about the potential risks and available options.
Recognize hypercoagulability. Blood clotting is a normal process, as blood needs to clot to stop bleeding in case of injury. On the other hand, hypercoagulability occurs when the blood clots too much, even when it's still in the body. This condition can result from prolonged sitting or lying down, cancer, dehydration, smoking, and hormone therapy. You are at risk for hypercoagulability if:
- You have a family history of abnormal blood clotting.
- You have had blood clots at a young age.
- You develop blood clots while pregnant.
- You’ve had multiple miscarriages with no identified cause.
- You have a genetic disorder, such as Factor V Leiden or Lupus Anticoagulant.

Recognize other health issues that may increase the risk of blood clots. Atrial fibrillation (irregular heartbeat) and the buildup of cholesterol plaque in the arteries can both lead to blood clots.
- In atrial fibrillation, blood flow is disrupted, leading to pooling and clotting.
- People with atrial fibrillation often have an irregular heartbeat without any other symptoms; this condition is usually discovered during a routine health check. It can be managed with blood thinners or other medications, lifestyle changes, and sometimes a pacemaker or surgery.
- Cholesterol plaque can build up in the arteries (sometimes as part of arteriosclerosis), and when the plaque ruptures, it can trigger the clotting process. Most heart attacks and strokes are caused by ruptured arteries in the heart or brain.
Preventing Blood Clots

Exercise regularly. Studies show that engaging in moderate to intense exercise for 150 minutes a week can reduce the risk of many health problems. On average, you should aim for 20-30 minutes of moderate exercise (walking, cycling, aerobics, etc.) each day. Choose activities you enjoy to ensure consistency. Exercise boosts circulation, enhances overall health, and helps prevent venous thrombosis.

Occasionally elevate your legs. You can raise your legs while resting or sleeping. Lift your legs from the calves to the feet, without raising your knees; avoid placing a pillow under your knees to prop them up. Instead, elevate your legs about 15 cm above the level of your heart. Avoid crossing your legs.

Break the habit of sitting for long periods. While exercise is crucial, it won’t be effective if you sit for extended periods before working out. If you’re sitting or lying down for long periods, such as during travel, working on a computer, or lying in bed, make sure to take breaks for light exercise. Every 2 hours, get up and move around. You can take a walk or perform simple foot exercises like rotating your heels and toes.
- Any activity that causes you to sit with your knees bent increases the risk of blood clots.

Stay well-hydrated. Severe dehydration can "thicken" the blood, stimulating clot formation. Everyone, especially the elderly and those at higher risk, should drink plenty of water. The American Institute of Medicine recommends that men drink 13 cups (3 liters) of water daily, while women should drink 9 cups (2.2 liters) per day.
- Do not wait until you're thirsty. Thirst is the first and most obvious sign that your body is dehydrated.
- Other signs of dehydration include dry mouth or severely dry skin.
- Drinking water immediately can help hydrate your body. If you experience diarrhea, vomiting, or heavy sweating, you may need to drink an electrolyte solution like Gatorade to rehydrate.

Regular health checkups during pregnancy are essential. Elevated estrogen levels can increase the risk of venous thromboembolism. During pregnancy, estrogen levels cannot be controlled by the body. The only solution is to avoid other risk factors, such as smoking or prolonged sitting, and schedule regular checkups for monitoring.
- If a venous clot forms in the arms or legs, doctors may prescribe safe medications during pregnancy to prevent the clot from traveling to the lungs or brain, which could be fatal.
- Blood thinners during pregnancy can pose risks as they interfere with placenta attachment.
- However, if there are many venous clots, Lovenox might be helpful. After childbirth, mothers may switch to Coumadin, which is safe during breastfeeding.
- In the US and Western Europe, venous thromboembolism is the leading cause of death in pregnant women.

Discuss with your doctor about alternatives to hormone replacement therapy (HRT). HRT, used to manage menopausal symptoms, increases the risk of blood clots. Non-hormonal alternatives like Estroven, which contains soy isoflavones, can help reduce hot flashes without increasing clotting risks. You can also include isoflavones in your diet from foods like soybeans, soy milk, or tofu. Keep in mind that there are no current guidelines on supplemental dosages.
- Alternatively, you might choose to live with menopausal symptoms without treatment. Though uncomfortable, this option poses no health risks.
Only take hormonal contraceptives if advised by your doctor. The combination of estrogen and progestin in most birth control pills can increase the risk of blood clots by 3-4 times. However, for healthy women with no additional risk factors, the risk is very low, about 1 in 3000 cases of venous thrombosis.
- Women with heavy menstrual bleeding or uterine abnormalities should consider non-hormonal treatments when possible. Options may include estrogen-free contraceptives (containing only progesterone) or non-hormonal alternatives like an IUD.
- Even if you have a history of or are at risk of blood clots, you can still use hormonal contraceptives while taking blood thinners. Doctors may prescribe low-estrogen (or estrogen-free) birth control pills to reduce clotting risks.
Maintaining a healthy weight is crucial. Excess fat cells, which are linked to an increased risk of venous thromboembolism, make weight management important, especially if you're obese (BMI of 30 or higher). The healthiest way to lose weight is through a combination of regular exercise and a balanced diet. While calorie intake should be restricted, it should not fall below 1200 calories per day. If exercising, additional calories may be required. It's advisable to consult with your doctor for personalized guidance.
- Wear a heart rate monitor while exercising to track your pulse.
- To determine your target heart rate, subtract your age from 220.
- Multiply the result by 0.6 to calculate your ideal heart rate. Maintain this target for at least 20 minutes, at least 4 times a week.
- For example, a 50-year-old woman should aim for a heart rate of (220-50) x 0.6 = 102.
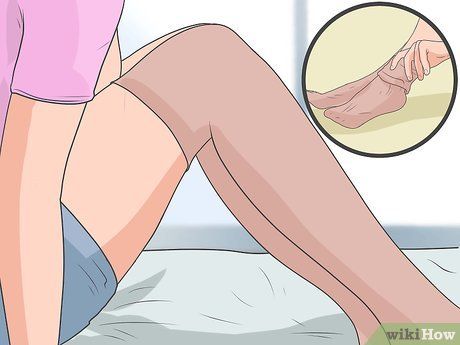
Wear compression stockings. Compression stockings, also known as anti-thromboembolism stockings, are commonly worn by people who need to sit or stand for long periods, such as servers, nurses, and doctors, to improve circulation. These stockings are also used if you have a blood clot to reduce pain and swelling in the legs. They may also be recommended for bedridden patients.
- Compression stockings are available in most pharmacies. The length should reach the knee to effectively promote circulation.

Consult with your doctor about blood thinners. If you're at high risk for venous thrombosis, your doctor may prescribe medication to prevent it. Depending on your specific condition, they may recommend prescription drugs (like Coumadin or Lovenox) or over-the-counter options such as Aspirin.
- Coumadin is a prescription drug typically taken at a dose of 5mg per day. However, its effect may vary based on your body's response to vitamin K, which is essential for normal blood clotting. Therefore, dosages may differ.
- Lovenox is an injectable prescription medication that can be administered at home. You'll receive pre-filled syringes to inject twice a day, with the dosage depending on your weight.
- Aspirin is an over-the-counter option suitable for those at low risk. It has been shown to help prevent blood-related conditions, from clots to stroke and heart attacks.

Ask your doctor about medications if you have cancer. One in five patients with malignant cancer develops venous thrombosis. Various factors, such as inflammation related to cancer, lack of movement, or medication side effects, contribute to this. Cancer patients with venous thrombosis are often prescribed Lovenox or Coumadin and may also be given an Inferior Vena Cava (IVC) filter. The IVC filter acts as a barrier, preventing clots that have broken off from the deep veins of the legs from reaching the lungs or heart, thus reducing the risk of fatality.

Consider natural remedies. While natural therapies to prevent blood clots are often passed down through word of mouth, they lack scientific proof. It is believed that plant-based nutrients can help prevent venous thrombosis in cancer patients, but no mechanism has yet been established to show how natural diets can suppress inflammation and reduce cytokine production. Recommended foods in a diet designed to prevent blood clots include:
- Fruits: Apricots, oranges, black raspberries, tomatoes, pineapples, plums, blueberries.
- Spices: Curry, Cayenne pepper, Paprika, Oregano, Turmeric, Ginger, Licorice, Ginkgo biloba.
- Vitamins: Vitamin E (almonds, walnuts, lentils, oats, and wheat) and omega-3 fatty acids (fatty fish like salmon).
- Plant-based sources: Sunflower seeds, canola oil, castor oil.
- Supplements: Garlic, Ginkgo biloba, Vitamin C, Nattokinase supplements.
- Alcohol: Wine and honey.
Warning
- If one leg is swollen, tight, painful, with red or slightly bluish skin, and feels warm, it may be a sign of deep vein thrombosis. In such cases, you should see a doctor as soon as possible.
- If you experience shortness of breath, severe chest pain, dizziness or fainting, rapid heartbeat, or coughing up blood without a clear cause, it could indicate a pulmonary embolism. Call emergency services (115) immediately. This may result from a clot traveling to the lungs and requires urgent medical attention.
