Male incontinence is a symptom associated with various syndromes and medical conditions that require thorough investigation. It could stem from issues with the nervous system, urinary-reproductive organs, or other disorders. The key to preventing recurrence is identifying the underlying cause of the condition. Reflect on any changes in your life, such as starting a new medication that may have an impact, or gaining weight which could put additional pressure on the bladder. There are preventive measures that apply to everyone in good health, but if you're experiencing incontinence, visiting a doctor to discuss your symptoms is the first and most important step.
Steps
Follow the steps to prevent incontinence
Identify the types of incontinence that can be prevented. There are various underlying causes of incontinence, some of which unfortunately cannot be controlled. Conditions such as prostate enlargement, neurological disorders, strokes, prostate/bladder cancer, etc., are beyond prevention. However, you can take steps to minimize the risk of developing some of these potential health issues.

Quit Smoking. A great way to reduce the risk of developing incontinence is by quitting smoking. The National Institutes of Health report that up to 50% of bladder cancer cases are caused by smoking. Tumors create pressure on the bladder, leading to urinary incontinence. If you need help, make an appointment with your doctor, who can assist you in quitting smoking. Your doctor may prescribe medication and recommend a local support group.
Lose weight to prevent incontinence. When you are overweight, the bladder endures additional pressure. This pressure can lead to incontinence. Although weight loss is a challenging task, the effort will ultimately be worth it. Start exercising more and try to eat healthy foods. Other weight loss methods include:
- Ensure daily intake of appropriate amounts of protein, fruits, vegetables, low-fat dairy, and healthy starches. The food groups you consume daily depend on your weight, age, and health. If you need 2,000 calories a day, you should eat 6-8 servings of grains, 4-5 servings of vegetables, 4-5 servings of fruits, 85-170 grams of protein, 2-3 servings of low-fat dairy, and 2-3 servings of fats and oils.
- Schedule regular workouts and stick to it. Your exercise routine should include cardiovascular exercises (like running or swimming), weight-bearing exercises (like push-ups or weightlifting), and flexibility exercises (like yoga or stretching).
- Limit portion sizes for each meal.
- Choose low-calorie snacks like fruits and vegetables.

Increase zinc intake in your diet. Studies show that in prostate cancer patients, zinc levels in cancerous prostate cells decrease by 62-75%, and zinc plays a role in the progression of prostate cells to malignancy. Zinc supplementation is recommended, though the exact amount required is not yet clear. You should consult your doctor about the appropriate dosage based on your current zinc intake in your diet.

Increase lycopene intake. Lycopene is a plant nutrient and an effective antioxidant that has been proven to help fight cancer. The five foods with the highest lycopene content per cup include:
- Guava: 8587 uq
- Watermelon: 6889 uq
- Tomatoes: 7298 uq
- Papaya: 2651 uq
- Grapefruit: 2611 uq

Eat more soybeans. Isoflavones in soybeans may help prevent prostate cancer. You can increase your soy intake with Japanese soybeans, soy milk, or tofu.

Include omega-3 fatty acids in your diet. Omega-3 fatty acids are found in various fish and seafood, including salmon, mackerel, sardines, and bass. Studies have shown that omega-3 helps combat breast cancer, colon cancer, and prostate cancer.

Stay hydrated. Drink at least 8 glasses of water daily to prevent conditions like urinary tract infections, constipation, and kidney stones, which can lead to incontinence. You should also consider drinking most of your fluids during the day and limit intake in the evening before bed.

Practice timed voiding. If you're concerned about developing incontinence, you can train your bladder to some extent. Set regular times to urinate throughout the day. This technique helps condition your bladder and can prevent incontinence.

Avoid foods and drinks that trigger incontinence. Certain substances can cause incontinence, including alcohol, caffeine, acidic foods, spicy foods, sugar, and artificial sweeteners.
- Alcohol is a diuretic, which causes the body to lose fluids. It also irritates the bladder, leading to incontinence. Try to limit your alcohol consumption to about one drink per night if possible.
- Caffeine is another diuretic. It is best to consume caffeinated beverages earlier in the day if needed.

Try Kegel exercises. Kegel exercises are an excellent method to prevent incontinence by strengthening the pelvic floor muscles. Learning how to perform them correctly can be a bit tricky, as you need to isolate the pelvic muscles. These are the muscles you use when attempting to stop the flow of urine. You should feel or see your testicles lift when you tighten these muscles.
- Once you've isolated the pelvic muscles, tighten them and hold for a count of 5, then relax for 5 seconds. Aim to repeat this 10 times, 3 times a day.

Avoid diuretics. Diuretics are medications that help eliminate excess fluid from the body. They are often prescribed to people with heart conditions. Unfortunately, they tend to cause incontinence. There are several types of diuretics: thiazide, loop, potassium-sparing, and quinazoline. Common diuretics include:
- Thiazide diuretics: Clorpres, Tenoretic, Thalitone, Capozide, Dyazide, Hyzaar, Lopressor HCT, Maxzide, and Prinzide.
- Loop diuretics: Lasix and Demadex.
- Potassium-sparing diuretics: Aldactazide, Aldactone, Dyazide, and Maxzide.
- Quinazoline diuretics: Zaroxolyn
- Always consult your doctor before discontinuing any prescribed medications.

Consider avoiding muscle relaxants. Muscle relaxants are prescribed to treat certain types of muscle injuries. While they help relax the body, they can also cause incontinence. Common muscle relaxants include:
- Valium, Soma, Flexeril, Skelaxin, and Robaxin.
- Sedative medications may also contribute to incontinence.

Identify antihypertensive medications that may cause incontinence. Antihypertensive medications are used to lower blood pressure and may include combinations of different diuretics. If you are taking antihypertensive medication, ask your doctor about options that do not have side effects that lead to incontinence. Common diuretics used for high blood pressure include:
- Moduretic, Minizide, Monopril HCT, and Accuretic.
Treatment for Overflow Incontinence

Watch for symptoms of overflow incontinence. Overflow incontinence occurs due to an obstruction in the bladder outlet, leading to 'overflow' and causing urinary leakage. Benign prostatic hyperplasia (BPH) is the leading cause as an enlarged prostate compresses the urethra. However, other conditions can also lead to these symptoms, including:
- Frequent urination
- Intermittent urination (difficulty urinating despite the urge)
- Nocturia (frequent nighttime urination)
- Weak urine stream
- Recurrent urinary tract infections (UTIs)
- Incontinence
- Occasional urinary retention (inability to urinate)
Consult a doctor. While prostate enlargement is one of the most common causes of overflow incontinence, it's not the only cause. You should visit a doctor and describe your symptoms to help them accurately diagnose your condition.
- A tumor in the bladder or prostate can also lead to overflow incontinence, so your doctor will conduct screenings to rule out these possibilities. Tests may include a prostate-specific antigen (PSA) blood test, a digital rectal exam (DRE) to check for prostate abnormalities, and/or cystoscopy (a tube inserted into the bladder via the urethra to check for tumors). If a tumor is found, the doctor will recommend a biopsy to determine whether the tumor is benign or malignant.

Identify medications that may lead to overflow incontinence. During your examination, your doctor will ask about the medications you are taking, as some medications can cause side effects that lead to overflow incontinence. Diuretics used for cardiovascular conditions, sedatives, and muscle relaxants are common culprits. Some antidepressants, sleep aids, and blood pressure medications are also linked to overflow incontinence.
- Since these medications are prescribed for much more serious conditions than incontinence, you should never stop taking them without your doctor's guidance.
- While not medications, excessive consumption of coffee, tea, alcohol, and vitamins B or C can also cause overflow incontinence. Your doctor may order blood tests to determine if your diet is too high in these vitamins.

Ask about medications for overflow incontinence. For mild to moderate benign prostatic hyperplasia (BPH), several medications are prescribed to manage symptoms:
- Alpha-blockers like Hytrin, which may not shrink the prostate but can alleviate symptoms within weeks.
- 5-alpha-reductase inhibitors like Avodart, which shrink the prostate but may take up to six months to show improvement.
- Cialis, primarily used for erectile dysfunction (ED), also helps alleviate BPH symptoms.
- Your doctor may prescribe a combination of Avodart and Hytrin for combined effects. This is a common, safe, and effective treatment for managing overflow incontinence.

Consider surgery for severe cases. Transurethral resection of the prostate (TURP) is an effective procedure for clearing the urinary tract obstruction caused by prostate enlargement. This technique uses an endoscope inserted through the urethra to scrape or remove excess prostate tissue that invades the urethra.
- This procedure can be performed using various methods, including laser or microwave energy, transurethral needles, or selective vaporization. It is a minimally invasive procedure commonly used for treatment in many cases.
- A second surgery may be required after about ten years due to regrowth of tissue.
Treating stress incontinence.
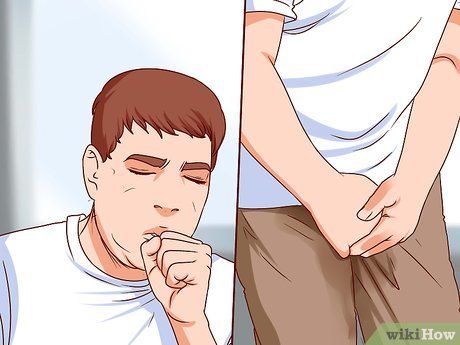
Identify symptoms of stress incontinence. Stress incontinence (also known as urinary leakage due to increased abdominal pressure) is often more related to small amounts of urine leakage rather than the numerous symptoms of overflow incontinence. You may notice urine leaking when you laugh, cough, sneeze, jog, or lift heavy objects.
Identify causes of stress incontinence. Increased pressure on the bladder due to obesity or pregnancy is the most common cause. Stress incontinence can also occur due to a lack of bladder contraction pressure resulting from complications after surgery. Surgeries commonly linked to this complication include prostate surgery and transurethral resection of the prostate (TURP).
- 10-20% of TURP surgeries result in stress incontinence, with even higher rates in prostate cancer surgeries.

See a doctor. Your doctor will examine your symptoms and run tests to determine the best treatment plan for you. If you're obese, metabolic disorder tests may be necessary, as conditions like thyroid issues could contribute to weight gain.

Lose weight. If your doctor concludes that your weight is putting unnecessary pressure on your bladder, they may suggest weight loss as a primary treatment for this condition.
- This process will include transitioning to a balanced, healthy diet along with regular exercise. You can find more information in the article "How to Lose Weight" and "How to Eat Healthy".
- You may need to consult with a nutritionist and personal trainer to create the best, healthiest weight loss plan for you.

Practice Kegel exercises. While primarily known for helping women strengthen pelvic muscles after childbirth, Kegel exercises can also assist men with stress incontinence. Perform the exercise by tightening the muscles that control urination. Initially, you can practice by stopping urination midstream to understand the feeling of tightening these muscles when not urinating.
- Squeeze the muscles slowly while counting to 5, then slowly relax while counting to 5. Repeat this exercise 10 times, 3 times a day.

Consider weight loss surgery options. For individuals with morbid obesity, a doctor may recommend gastric banding or other weight loss surgery options. A study revealed that 71% of patients who lost more than 18 BMI points through gastric banding surgery regained their ability to control urination within a year after the procedure.
Treating neurogenic bladder incontinence.

Identify the causes of neurogenic bladder incontinence. Urination occurs when nerves transmit signals to the brain and from the brain, instructing the bladder muscles and surrounding areas to contract and relax. If you have a neuro-muscular disorder, such as multiple sclerosis (MS), these signals may be disrupted, leading to neurogenic bladder syndrome. People who have had a stroke may also develop neurogenic bladder syndrome if the muscles in the bladder responsible for contraction and relaxation are affected.

See a doctor. Most patients with neurogenic bladder syndrome are familiar with the underlying causes. However, it is still important to see a doctor for a specific diagnosis. The doctor will provide an overview of treatment options and help you determine which method is best for your specific case.
Try physical-psychological therapy. Also known as scheduled voiding, physical-psychological therapy combines willpower and exercise to help manage incontinence. This therapy involves Kegel exercises (as described in the treatment of stress incontinence) and keeping a voiding diary to help you avoid incontinence episodes before they occur.
- A voiding diary is a daily record of fluid intake, frequency of urination, urine output, and instances of leakage. You can use this record to determine when to stay near a restroom and when to force yourself to urinate to minimize incontinence episodes.

Talk to your doctor about available medication options. While there is no current medication specifically for bladder sphincter muscles to treat neurogenic bladder, some medications can help either decrease or increase muscle contractions. Your doctor will determine the best group of medications tailored for your specific case.
Discuss surgical options with your doctor. There are several surgical methods to consider, depending on the underlying cause of your neurogenic bladder syndrome. The doctor might discuss:
- Electrical stimulation therapy, which involves electrodes and a small implanted device to help restore disrupted signals caused by nerve damage.
- Artificial sphincter, a ring placed around the bladder neck that works in conjunction with an implanted pump and adjustable balloon to control urine retention.
Treatment for overactive bladder syndrome (OAB)

Identify the symptoms of overactive bladder. Overactive bladder (OAB) is a condition that leads to a sudden, uncontrollable urge to urinate. Common symptoms include:
- Urinary urgency (the primary symptom)
- Uncontrollable urinary urgency (unable to reach the bathroom in time)
- Frequent urination and nocturia (waking up to urinate during the night)

Visit your doctor. Your doctor will help confirm the diagnosis of overactive bladder syndrome as a potential underlying cause. Only 2% of men with overactive bladder experience incontinence, so the doctor will need to consider other possible underlying causes.
- The doctor will perform a physical exam and may recommend a urinalysis, and in more complicated cases, a cystoscopy may be required.
- The results may show increased muscle activity in the bladder wall.
Follow a Timed Voiding Schedule. Treatment involves behavioral therapy with a timed voiding regimen. This regimen consists of urinating at regular intervals, for example, every four hours, even if you do not feel the urge to urinate.
- This is a bladder training method, a form of cognitive-behavioral therapy. You will aim to train your bladder to empty at scheduled times to prevent incontinence.
- A recent report showed that behavioral biofeedback therapy (timed voiding) is more effective than pharmacological therapy with oxybutynin or placebo in patients treating unstable sphincter conditions.
- Biofeedback is a therapy where patients are attached to electrodes to measure their involuntary physiological responses. This method allows patients to observe their biological responses (such as the sensation of needing to urinate) and distinguish them from 'false alarms.' Seeing actual data rather than just making judgments helps them better interpret their body’s signals.

Consult Your Doctor About Medications You Can Use. There are various pharmacological interventions, particularly Ditropan, with a dosage of 5 mg twice a day. Combined therapies involving behavior modification, medication, and biofeedback are commonly used.
Advice
- Encouraging a healthier lifestyle is always a good idea – a tobacco-free lifestyle combined with physical activity and a balanced diet – can also prevent urinary incontinence.
