Lymphedema is a condition where fluid accumulates in the soft tissues of the body due to a blockage or removal of lymph nodes. This condition is most commonly caused by lymph node removal following cancer treatment, but it can also result from environmental or genetic factors. Lymphedema usually develops within three years after surgery. It can also be caused by abnormal lymphatic system development from birth, with symptoms potentially appearing later in life. Early detection and treatment are the best ways to prevent lymphedema.
Steps
Lymphedema Prevention
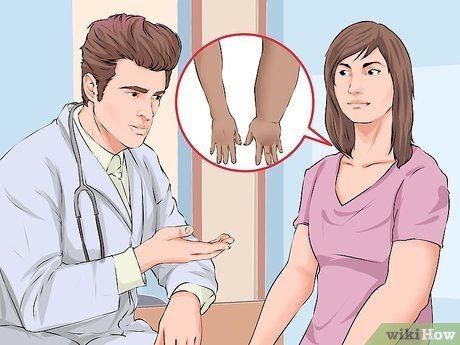
Consult your doctor as soon as you notice signs of lymphedema. Symptoms of lymphedema include swelling in the arms, legs, hands, fingers, neck, or chest. If you notice swelling or other symptoms (listed below), you should seek medical advice immediately.
- Identifying the early signs is the best way to prevent the condition from worsening.
- There is no cure for lymphedema, but early treatment can help alleviate symptoms and prevent further issues.
- Lymphedema may develop days, weeks, months, or even years after cancer treatment.
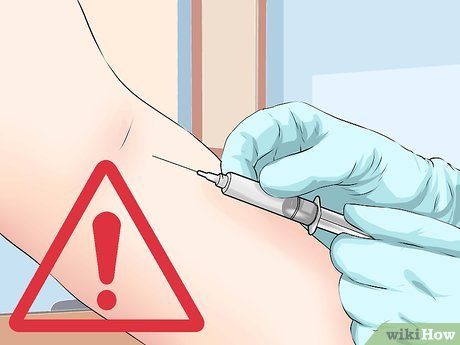
Avoid drawing blood from the arm at risk of lymphedema. Lymphedema typically develops in the area of the body that underwent surgery. You should refrain from having injections or intravenous treatments in the arm that is at risk of developing lymphedema.
- When measuring blood pressure, opt for the arm with the lower risk of lymphedema.
- Consider purchasing a medical alert bracelet to inform others not to draw blood, administer IVs, or inject into the arm at risk of lymphedema.

Avoid prolonged exposure to hot water. Do not expose the arm or leg at risk of lymphedema to hot water, steam, or areas with high temperatures. If you wish to take a hot bath, avoid submerging your arm.
- Do not use hot packs or other heat treatments.
- Avoid massaging the area at risk of lymphedema too vigorously.
- High temperatures and massage can push bodily fluids into sensitive areas, triggering lymphedema.
- Limit sun exposure on the affected arm if possible.

Avoid lifting heavy objects or carrying a heavy bag on your shoulder. To aid recovery after surgery or cancer treatment, avoid using the affected body part to carry heavy loads. Be cautious not to place excessive pressure on the arm at risk of lymphedema.
- When lifting, try to raise your arm above your waist.
- As you recover, you can gradually begin lifting heavier objects.
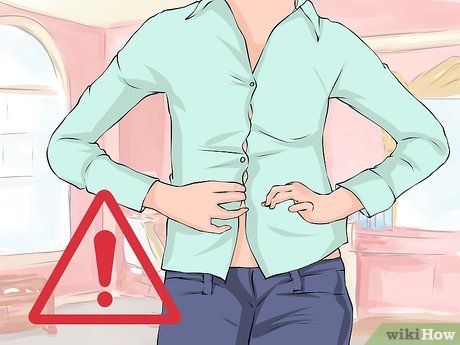
Avoid tight clothing or jewelry. If a watch, ring, bracelet, or other jewelry is too tight, loosen it or stop wearing it. Additionally, wear loose clothing that does not restrict movement.
- Avoid wearing tight-necked shirts if there is a risk of lymphedema in the head or neck area.
- Tight wraps or tight jewelry around the neck, arms, legs, wrists, and other parts of the body can cause fluid buildup in those areas.
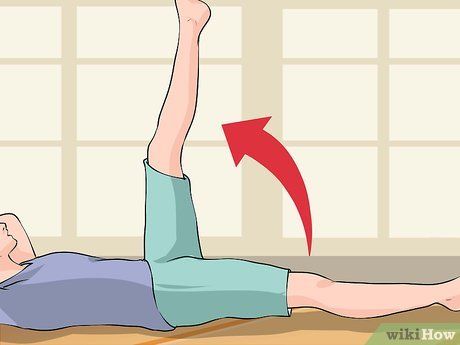
Elevate your arm/leg. If you are at risk of lymphedema, try to elevate the affected arm or leg whenever possible. This helps prevent fluid buildup and reduces swelling.
- This preventive measure is most effective in preventing lymphedema from developing in the arm, hand, or fingers.
- If sleeping on your back, elevate your legs above your heart. For example, place a pillow under your knees or feet.

Change your posture. Avoid sitting or standing in one position for extended periods. Instead, try to shift your position regularly. Do not cross your legs while sitting, and aim to sit with your back supported when on the bed.
- Sitting upright with your back supported in bed helps improve lymphatic fluid flow in the body.
- You can set reminders on your phone or use a clock to remind yourself to move frequently. Additionally, use natural cues to prompt movement, such as changing positions during TV commercials.

Wear protective clothing. Cuts, sunburns, burns, insect bites, and scratches can push fluid into the affected area, increasing the risk of lymphedema. Wearing loose, long clothing can protect your skin from these injuries.
- Opt for loose-fitting clothing, rather than tight options.
- Avoid wearing compression sleeves (typically worn by athletes), as they can squeeze the arm.
Protect your arms and legs from injury. Any cuts, open wounds, scratches, or burns on the affected arm or leg can lead to infections. Infections prevent lymphatic fluid from filtering bacteria and viruses. Signs of infection include swelling, pain, redness, warmth, and fever. If these symptoms occur, seek medical attention immediately.
- Avoid sharp objects from puncturing your skin.
- Use a thimble when sewing, wear thick gloves for gardening, and apply insect repellent when outdoors.
- Moisturize your skin with a gentle lotion to prevent dryness and cracking.
- Be cautious when shaving with a razor.
- If you get manicures, ensure the technician is aware of your health condition. Avoid places with poor hygiene or those where clients have experienced fungal, bacterial, or viral infections.
- Wear gloves when doing household tasks or gardening to protect your hands, fingers, and nails.
- Wear comfortable, closed-toe shoes to minimize foot and toe injuries.

Adopt a balanced, low-salt diet. Every meal should contain 2-3 servings of fruit and 3-5 servings of vegetables. Eat fiber-rich foods like whole grain bread, cereals, pasta, rice, and fresh fruits and vegetables. It’s best to avoid alcohol (limit to one serving per day).
- Avoid consuming fast food or calorie-dense snacks that offer little nutritional value. These foods are not only high in calories and low in nutrients, but they also contain excessive amounts of salt.
- Limit your intake of red meat and processed meats such as sausages or smoked meats.
Maintain a healthy weight. Being overweight or obese contributes to an increased risk of lymphedema. Excess weight adds pressure to the swollen area, affecting lymphatic fluid drainage.
- A balanced diet, regular exercise, and proper lifestyle choices are key to maintaining an ideal weight.
- If you need assistance, consult your doctor. They can offer advice tailored to your health condition.

Maintain a healthy lifestyle. Achieving and maintaining a healthy weight helps prevent lymphedema from developing. You should follow a balanced diet and exercise regularly to promote overall health.
- Getting enough sleep supports a strong immune system and reduces the risk of lymphedema.
- Consult with your doctor to design a suitable exercise program. Intense exercises are not recommended, but you should aim for daily physical activity.

Avoid smoking. Smoking constricts capillaries and small blood vessels, hindering the free circulation of fluids in the body. It also depletes oxygen and other essential nutrients needed for fluid circulation. Smoking damages the skin's elasticity.
- If you need assistance to quit smoking, consult your doctor about available methods to stop smoking. Numerous support resources are available to help you quit.
- Quitting smoking also reduces the risk of cancer and other health issues.
Recognize the symptoms of the condition

Pay attention to swelling in the arm, leg, breast, or hand. Swelling in the soft tissues of the arm or leg is one of the most common signs of lymphedema. In the early stages, the skin remains soft, and the swollen area will indent when pressed.
- Your doctor may use a tape measure to monitor the swollen area and track its progress.
- In later stages of lymphedema, the swollen area will become firmer and harder. Pressing the swollen area will not cause it to indent.

Notice any heaviness in the arm or leg. Along with or before noticing swelling, you may feel a sense of heaviness or difficulty moving the affected arm or leg due to fluid buildup. If you are at risk for lymphedema, this could be an early sign of the condition.
- If you’ve had surgery, radiation therapy, or lymph node removal, use a mirror to check for any swelling (if present).
- Compare both sides of your body to spot any differences.
Be mindful if you experience joint mobility issues. Stiffness in fingers, toes, knees, elbows, or other joints may indicate an increase in fluid buildup due to lymphedema. Although joint stiffness can have multiple causes, the pressure in joints from fluid accumulation might be a sign of lymphedema.
- Lymphedema symptoms may develop gradually or appear all at once.
- Be aware of your body to recognize unusual signs.

Pay attention if your toes or feet feel itchy or burn. This could be a sign of cellulitis—a bacterial skin infection that is not contagious. Since lymphedema affects the immune system, it’s important to see a doctor immediately if you notice symptoms of cellulitis.
- Cellulitis can be caused by insect bites or scrapes.
- Your doctor will treat the infection with antibiotics. Do not ignore signs of infection as it can quickly become life-threatening.

Check for signs of thickened skin (hyperkeratosis). Fluid buildup can lead to thickening of the skin. If you notice thicker skin on your arms, hands, legs, feet, or other changes such as blisters or warts, it may be a sign of lymphedema.
- Keeping the skin clean is crucial for those with hyperkeratosis.
- Use therapeutic moisturizing creams daily and avoid lotions containing lanolin or fragrances.

Be cautious when clothing or jewelry feels tight. People with lymphedema often feel uncomfortable wearing a bra, even without weight gain. Similarly, tight rings, uncomfortable watches, or bracelets may be signs of lymphedema.
- You may find it difficult to fit one arm into a sleeve.
- Since lymphedema symptoms can develop gradually, you might not notice swelling in the shoulder or arm until you have trouble dressing. If you feel tightness on one side or struggle to fit into snug clothing like t-shirts or jackets, be alert for signs of lymphedema.

Observe for signs of taut, shiny, warm, or red skin. The skin may appear "shiny" or "stretched tight." This could be a sign of cellulitis. If you notice any change in the color or texture of your skin, consult a doctor immediately.
- The affected area of skin can spread quickly.
- Other less common symptoms include fatigue, fever, pain, or cold-like symptoms.
Recognize signs on the head/neck

Be aware of swelling around the eyes, face, lips, neck, or under the chin. Head and neck lymphedema symptoms typically appear 2-6 months after cancer treatment in the head area. Sometimes, lymphedema develops in the larynx and throat (mouth and pharynx). It may also extend outside the neck and face, depending on which lymphatic channels are blocked.
- Consult a doctor if you notice any signs of head or neck lymphedema.
- If left unchecked, swelling may lead to inflammation and quickly become uncontrollable.

Feel for any tightness or swelling in the affected area. Since head and neck swelling can be hard to spot, the first symptoms of lymphedema in this area are often felt through physical sensations. Pay attention if you notice any tightness around the head or neck.
- You might find it difficult to move your head, neck, or face. The skin may feel stiff or uncomfortable, even if the swelling is not clearly visible.
- Your doctor may perform further tests to check for lymphedema, such as radioactive nuclear imaging of the lymphatic system or another imaging technique using contrast dye to highlight any irregularities in lymphatic circulation.

Be cautious if swelling in the eyes affects your vision. Blurry vision, excessive tearing, uncontrolled tearing, red eyes, or pain around the eyes could indicate the presence of the lymphatic-multiplied eyelash syndrome. This is a genetic condition present at birth, but symptoms might only emerge during adolescence.
- The growth of additional eyelashes along the inner eyelid lining is also a sign of lymphatic-multiplied eyelash syndrome.
- Other vision-related issues from this condition include abnormal corneal curvature and corneal scarring.

Monitor for difficulty swallowing, speaking, or breathing. In more severe cases of lymphedema, swelling in the neck and throat can affect normal functions. You may experience drooling or have difficulty keeping food in your mouth.
- Swelling may lead to nasal congestion or ear pain. It can also affect the sinus glands and nasal cavities.
- To confirm head and neck lymphedema, your doctor may perform an ultrasound or MRI scan. These tests help identify the location of lymph fluid in the head.
Advice
- Even if you are at risk of lymphedema, it's important to see a doctor to rule out other causes of symptoms similar to lymphedema.
Warning
- Seek medical attention immediately if you notice signs of infection such as a fever above 38°C, persistent sweating, chills, a rash, or other skin abnormalities like pain, redness, or swelling.
