Skin rashes are inflamed, red patches of skin that can be accompanied by various symptoms such as pain, itching, and swelling. They can result from allergic reactions, infections, inflammations, exposure to irritants or heat, or other health issues. While some rashes may heal on their own, others may require medical treatment. However, there are several steps you can take to prevent many types of skin rashes.
Steps
Preventing Heat Rash

Avoid situations that cause sweating. Heat rashes occur when sweat glands in the skin become blocked. Instead of evaporating, sweat gets trapped under the skin, leading to a rash.
- Heat rashes typically appear in hot, humid conditions.
- Keep your body dry by staying indoors during the hottest part of the day.
- Use air conditioning to cool down.
- Take a cool shower or apply a damp, cool cloth to the overheated areas of your body.

Avoid high-intensity exercise in hot and humid conditions. The temperature your body emits combined with warm weather can cause rashes in areas of the body with the most sweat glands, such as under the arms.
- Instead of exercising outdoors in the heat, consider going to an air-conditioned gym.
- Take a cool shower after exercising.

Wear light, loose clothing. Tight-fitting clothes can cause skin irritation and rashes due to the heat trapped by your body.
- Allow your skin to breathe by wearing light and loose clothes. This applies to children as well. Don’t overdress your child in hot weather.
- However, during exercise, this is an exception. Wearing properly fitted clothes designed to wick sweat and excess moisture can help prevent heat rashes, especially during high-intensity exercises like cycling and running.

Stay hydrated. Your body needs water to function properly, and the fluids lost through sweating need to be replenished.
- Drink water throughout the day to avoid dehydration.
- Drink at least 2-4 cups (480-960 ml) of cool water every hour.
Prevent diaper rash

Keep skin folds dry and clean. Diaper rash occurs due to friction between skin areas, causing irritation and rashes. It mainly appears in moist and warm areas, especially where skin rubs against other skin, such as in the groin, under the breasts, between the thighs, under the arms, or between the toes. Diaper rash can also lead to fungal or bacterial infections. Unlike heat rashes, diaper rash can occur in any environmental condition.
- Keep skin clean and dry, especially in areas where skin rubs together. Use antiperspirant products for the underarm areas. Moisturizing balms can create a protective layer for areas like inner thighs. Applying baby powder or medicated powder can help absorb excess moisture.
- Wear open-toed shoes or sandals. This can help reduce moisture between the toes.

Apply moisturizing cream. Medicated moisturizers are available in most pharmacies. Ointments designed for treating diaper rashes, such as Desitin, can be helpful for areas that are frequently damp and prone to friction, like the groin area. Zinc oxide ointments are also effective.
- If you suffer from skin friction rashes frequently, consult your doctor about Tetrix moisturizer containing dimethicone. This cream is more effective than over-the-counter options.

Wear clean, loose-fitting clothing. Clothes that rub against the skin can cause rashes. It’s recommended to wear clothing made from natural fabrics like cotton, silk, or bamboo because synthetic fabrics can irritate the skin and block air circulation.

Lose weight. Skin rashes often occur in overweight or obese individuals because friction can occur in many areas of the body. You may want to consult your doctor to see if weight loss could help with rash treatment.
- Do not attempt to lose weight without consulting a doctor first.
Prevent eczema flare-ups
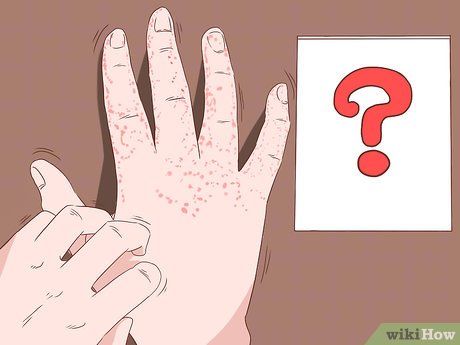
Identify and avoid eczema triggers. Eczema, or atopic dermatitis, is a chronic skin condition characterized by red, flaky, itchy rashes that may be sensitive to touch and swollen. People with eczema often lack certain proteins in the skin, and some health issues can exacerbate the condition. Learning to recognize and avoid eczema triggers is essential, such as:
- Skin infections
- Allergens like pollen, mold, dust mites, pets, and certain foods
- Cold, dry winter air, extreme temperatures, or sudden temperature changes
- Harsh chemicals or rough materials like wool
- Psychological stress
- Fragrances or dyes in skincare products or soap

Hỏi bác sĩ về thuốc hoặc các phương pháp điều trị dị ứng. Bạn có thể không thể tránh khỏi việc tiếp xúc với tác nhân kích thích, đặc biệt là nếu dị ứng với những thứ như phấn hoa. Trong trường hợp đó, nên trao đổi với bác sĩ về các phương pháp điều trị dị ứng để giảm triệu chứng.

Tắm nhanh. Tắm quá nhiều và quá lâu có thể lấy đi lớp dầu tự nhiên trên da, khiến da khô thêm.
- Thời gian tắm chỉ nên kéo dài tối đa 10-15 phút.
- Khi tắm, bạn nên tắm nước ấm thay vì nước nóng.
- Sau khi tắm, dùng khăn mềm thấm khô nước trên da.
- Chỉ dùng sữa tắm hoặc xà phòng dịu nhẹ. Sữa tắm, xà phòng tắm không gây dị ứng thường dịu nhẹ cho da và không lấy đi lớp dầu tự nhiên bảo vệ da.
- Tránh dùng sữa tắm kháng khuẩn hoặc sữa tắm chứa cồn vì sẽ dễ khiến da bị khô.
- Chọn sữa tắm có tác dụng dưỡng ẩm.

Dưỡng ẩm da ít nhất 2 lần mỗi ngày. Sản phẩm dưỡng ẩm giúp giữ lại độ ẩm tự nhiên của da, từ đó bảo vệ và giữ nước cho da.
- Da được dưỡng ẩm sẽ khó bị kích ứng hơn, ví dụ như khó bị kích thích do vải chà xát lên da, từ đó phòng ngừa được viêm da cơ địa.
- Ngoài ra, nên thoa sản phẩm dưỡng ẩm sau khi tắm và lau khô người.
Phòng ngừa viêm da tiếp xúc
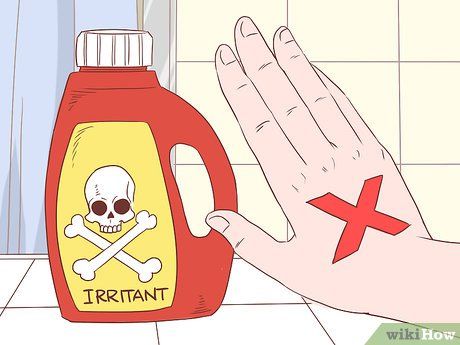
Tránh tác nhân kích ứng da và dị nguyên. Viêm da tiếp xúc là do các tác nhân kích ứng tiếp xúc với da. Viêm da tiếp xúc có thể là phản ứng dị ứng hoặc do một tác nhân kích ứng phổ biến (không gây dị ứng). Tránh tiếp xúc với tác nhân kích ứng có thể giúp phòng ngừa viêm da tiếp xúc.
- Tránh để da tiếp xúc với các tác nhân kích ứng phổ biến như mạt bụi, phấn hoa, hóa chất, mỹ phẩm, dầu thực vật (cây thường xuân độc) và các chất khác kích thích phản ứng viêm da tiếp xúc. Viêm da tiếp xúc do tác nhân kích ứng thường khiến da phát ban bong vảy, khô nhưng không ngứa. Tuy nhiên, một số loại viêm da tiếp xúc có thể gây ngứa và mụn nước.
- Một số người có thể phản ứng với tác nhân kích ứng ngay cả sau chỉ một lần tiếp xúc, trong khi một số khác sẽ xuất hiện triệu chứng sau khi tiếp xúc nhiều lần. Một số trường hợp có thể dần kháng lại tác nhân kích ứng.

Undergo allergy testing. If you are unsure whether you have an allergy, a doctor may conduct an allergy test to identify the triggers of contact dermatitis.
- Common allergens include nickel, medicinal products (such as topical antibiotics and antihistamines), formaldehyde, tattoos, and Henna products.
- Another common allergen is Peru balsam, which is used in cosmetics, perfumes, mouthwash, and flavoring agents. Discontinue use if a new product causes an allergic reaction.
- Carefully read product labels to avoid purchasing items containing allergens.

Wash the skin immediately after contact. If you come into contact with an allergen or irritant, it is essential to wash the skin immediately to prevent or reduce the reaction.
- Use warm water and a mild soap or take a shower if the area of contact is widespread.
- Wash clothes and items that have come into contact with the allergen or irritant.

Wear protective clothing or gloves when handling irritants. If you need to handle these substances, take protective measures to prevent direct skin contact with the allergen or irritant by wearing full-body protective clothing, safety glasses, and gloves.
- Always follow proper procedures and guidelines when handling harmful substances.

Apply moisturizing products to protect the skin. Moisturizers create a protective layer on the skin and help restore the outer skin layer.
- Apply moisturizing products before potential exposure to irritants and reapply frequently to keep the skin healthy.

Consult a doctor if you develop a rash after taking medication. Many medications can cause "drug rashes" as a side effect or allergic reaction. These rashes typically begin within a week of taking a new medication and appear as red spots spreading over a large area of the body. Some medications that may cause rashes include:
- Antibiotics
- Anticonvulsants
- Diuretics
Preventing psoriasis flare-ups

Take prescribed medication. Following your doctor's recommendation for psoriasis medication can help prevent flare-ups. This is especially true for medications that target the immune system, such as biologic drugs.
- Do not stop taking medication without consulting your doctor. Discontinuing psoriasis medication without professional advice can worsen the condition and cause a more severe form of psoriasis to develop.

Avoid stress. Psoriasis is an autoimmune disorder of the skin, characterized by rashes, flaky skin, and itching. The exact cause of psoriasis is often unknown, but certain triggers can worsen or cause flare-ups, including stress.
- Take steps to reduce stress in your life. Try relaxation techniques like Yoga and meditation.
- Exercise regularly. Physical activity boosts endorphin levels and helps alleviate stress.
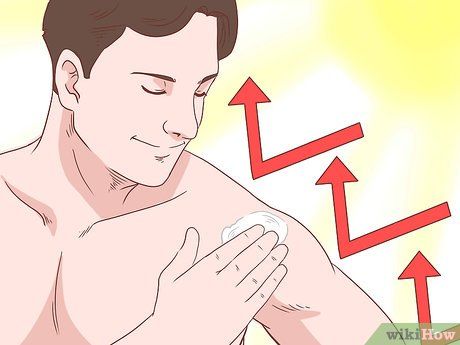
Avoid skin injuries. Skin injuries, such as from vaccinations, bites, scratches, or sunburn, can trigger the formation of new psoriasis lesions, known as the Koebner phenomenon.
- Wear protective clothing and immediately treat any cuts or injuries with proper hygiene techniques.
- Prevent sunburn by applying sunscreen, wearing protective clothing (such as hats and long, loose-fitting clothes), and staying in the shade. Also, limit direct sun exposure.

Avoid medications that can trigger psoriasis. Certain medications, such as antimalarials, Lithium, Inderal, Indomethacin, and Quinidine, can exacerbate psoriasis.
- If you suspect a medication is triggering your psoriasis, consult your doctor for alternative treatments.
- Do not abruptly stop taking prescription medications without consulting your doctor.
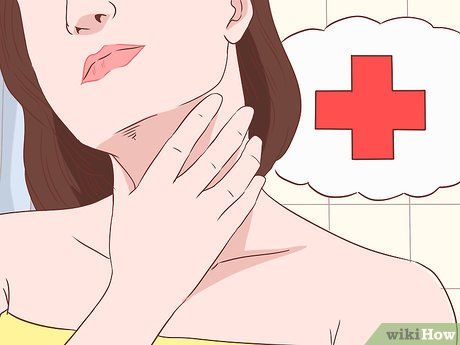
Avoid and treat infections. Anything that affects the immune system can trigger a psoriasis flare-up, including streptococcal throat infections (bacterial throat infection), oral thrush (caused by Candida albicans), and respiratory infections.
- Seek medical attention immediately if an infection is suspected.

Avoid high-calorie beer. A clinical study found that regular beer consumption (except light beer, wine, and other alcoholic beverages) is linked to an increased risk of psoriasis flare-ups.
- Women who drink beer more than five times a week have a 2.3 times higher risk of developing psoriasis compared to women who don’t drink beer.

Quit smoking. Smoking worsens psoriasis. It also negatively impacts overall health. Consider discussing with your doctor or pharmacist about ways to quit smoking.
- Women who smoke are at higher risk of exacerbating their psoriasis.

Avoid dry, cold weather. Cold and dry weather strips away the skin's natural moisture layer, potentially triggering a psoriasis flare-up.
- Keep warm and consider using a humidifier indoors.
Tips
- Avoid triggers and allergens that could provoke a skin rash.
- Visit a doctor if the rash persists.
- If you suspect an allergic reaction and have an Epipen, you may administer the injection while waiting for emergency help.
- Consider using medications like Cortisone to relieve itching and stop the rash.
Warning
- If you're unsure whether a medication might be causing the rash, consult your doctor. Do not stop taking prescribed medication without medical advice.
- Some allergic reactions can lead to life-threatening anaphylaxis. Seek medical help or call emergency services immediately if you experience severe symptoms. Warning signs of a severe allergic reaction include swelling of the lips or tongue, widespread rash, coughing, wheezing, or difficulty breathing.
- Some skin rashes can be severe, so it's crucial to get medical attention if you're uncertain about the severity of the rash.
