The liver is a large organ situated in the upper-right part of the abdomen and plays a critical role in the body's overall function. It helps detoxify the blood, eliminating toxins that enter the bloodstream. Additionally, the liver produces bile to aid in the digestion of fats and stores glucose to provide the body with necessary energy. Hepatomegaly, or an enlarged liver, is not a disease in itself but rather a symptom of an underlying condition, such as alcohol addiction, viral infections (hepatitis), metabolic disorders, cancer, gallstones, and some heart diseases. To determine if you have an enlarged liver, it is essential to recognize the signs and symptoms, undergo a specialist diagnosis, and pay attention to potential risk factors.
Steps
Identify the signs and symptoms

Pay attention to jaundice symptoms. Jaundice is characterized by a yellowish pigment appearing in the skin, mucous membranes, and the whites of the eyes due to elevated levels of bilirubin in the blood. Bilirubin is an orange-yellow pigment found in bile. A healthy liver typically eliminates excess bilirubin, so its presence indicates liver problems.
- In addition to the yellowish tint in the skin and eyes, jaundice symptoms may include fatigue, abdominal pain, weight loss, vomiting, fever, pale stools, and dark urine.
- Jaundice symptoms often occur when the liver is severely compromised. It is best to seek medical attention immediately if you notice any signs of jaundice.
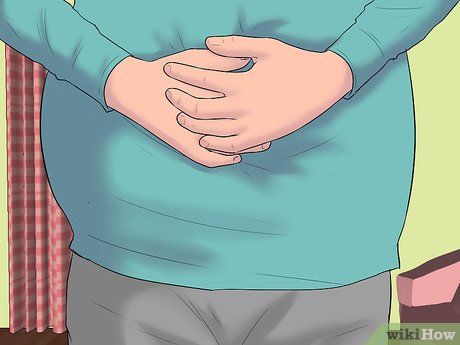
Pay attention to symptoms of bloating (abdominal distension) or abdominal pain. A swollen abdomen (if not caused by pregnancy) often indicates the accumulation of fat, fluids, stool, or the presence of a tumor, cyst, fibroid, or organ enlargement (such as the liver or spleen). In more severe cases, bloating can signal an underlying condition that requires medical evaluation.
- Ascites, which refers to fluid accumulation, is a common symptom of liver enlargement.
- Bloating can cause loss of appetite due to a feeling of fullness, a symptom known as 'early satiety.' It can also lead to a decreased desire to eat.
- Swelling can also occur in the legs.
- Abdominal pain, especially on the upper right side, can be a sign of liver enlargement, especially when accompanied by other symptoms.

Recognize common symptoms that may indicate liver enlargement. Symptoms like fever, loss of appetite, nausea, vomiting, upper right abdominal pain, and unexplained weight loss not only suggest liver enlargement but may also be signs of liver disease if they become severe, prolonged, or occur suddenly.
- A loss of appetite or disinterest in food may accompany bloating as mentioned earlier. This could also be a symptom of gallbladder disease, where eating triggers pain. It may also occur in cancer patients or those with hepatitis.
- Doctors often define significant weight loss as losing more than 10% of body weight. It's important to consult a doctor if you experience unexplained weight loss.
- Fever indicates inflammation or infection in the body. Liver enlargement can result from infections such as hepatitis, so it's crucial to manage fever appropriately.
- Unusual pale or light-colored stool, even gray or white, can be a sign of liver problems.

Be aware of extreme fatigue. You may feel unusually tired, even after slight exertion. This happens when the liver's nutritional reserves are compromised, causing the body to use muscle tissue for energy.
- Fatigue may be a sign that the liver is malfunctioning, and swelling could be a related symptom. Conditions like hepatitis and cancer can cause fatigue.

Notice an increase in itching. When the liver weakens, you might experience itching. This itching can be localized or affect the entire body. It occurs when bile ducts in the liver become blocked, releasing bile salts into the bloodstream, which then accumulate in the skin and cause itching.
- You may feel desperate to treat the itching, but if you suspect liver issues, it's essential to consult a doctor first.

Identify spider angiomas (vascular stars). These are dilated blood vessels that radiate out from a central red dot, resembling a spider's web. They typically appear on the face, neck, hands, and upper chest and are a common sign of liver disease or hepatitis.
- A single spider angioma is usually not concerning. However, if it's accompanied by other symptoms like lethargy, fatigue, bloating, or jaundice, you should see a doctor as these could indicate liver dysfunction.
- Spider angiomas can grow up to 5 mm in diameter.
- If you press gently on the angioma, the red color will fade in a few seconds and turn white due to blood flow being restricted.
Receiving a Specialist Diagnosis

Schedule an appointment with your primary care physician. When you visit your doctor, they will first ask about your medical history. It is important to be open and honest with your physician.
- Be aware that the doctor may ask private questions related to substance use, alcohol consumption, sexual activity, and partners. Your answers are crucial for an accurate diagnosis, so be truthful and specific in your responses.
- Tell your doctor about any medications or supplements you are taking, including vitamins and herbs.

Clinical Examination. A clinical examination is the first step in diagnosing liver enlargement. The doctor will examine your skin for jaundice and look for signs of spider angiomas if you haven't mentioned these symptoms. They will then palpate the abdomen to examine the liver.
- An enlarged liver may feel abnormal, either soft or hard, with or without lumps, depending on the underlying cause. This examination can help determine the size and consistency of the liver. The doctor will use two methods: percussion and palpation.
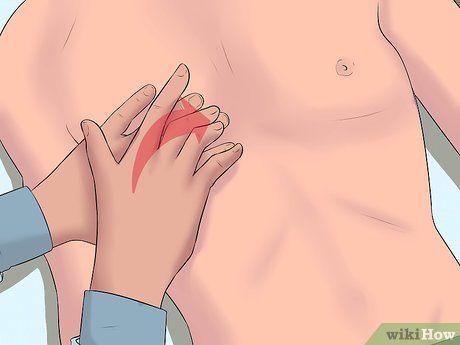
Understanding Percussion Technique for Liver Diagnosis. Percussion is a diagnostic technique used to assess the liver's size and confirm that it has not extended beyond the rib cage, which serves as the liver's protective barrier. This technique involves tapping on the body to listen for sounds. The doctor will tap on your body and listen to the sound. If the dull sound spreads more than 2.5 cm below the rib cage, your liver may be enlarged. Note that this technique might not provide accurate results if you are bloated, and you may need an ultrasound instead.
- If the doctor is right-handed, they will place their left hand on your chest, press the middle finger gently against the rib cage, and then use the middle finger of their right hand to tap on the left hand's finger. The tapping motion comes from the wrist (similar to playing the piano).
- Starting below the rib cage, the tapping sound will be resonant, as this area contains air-filled lungs.
- The doctor will slowly move along the line above the liver, listening until the resonant sound shifts to a dull 'thud,' indicating they've reached the top of the liver. They will continue tapping until they reach the bottom of the rib cage, where the sound changes to a combination of intestinal noises (gurgling and air sounds).
- The doctor will measure how far the liver extends beyond the rib cage, if at all. This is often a sign of a problem, as the rib cage's role is to protect vital organs like the liver and spleen. (If your lungs are excessively inflated, the doctor might feel the liver's edge.)
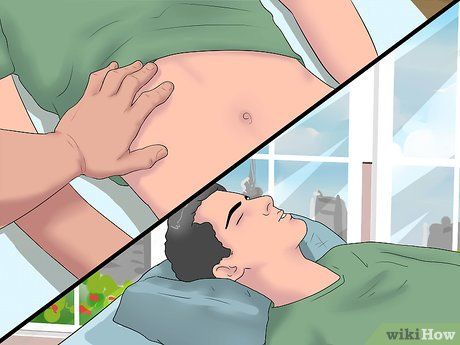
Understanding Palpation Technique to Assess the Shape and Consistency of the Liver. The doctor will also palpate to check if your liver is enlarged. Similar to percussion, palpation involves using the hands to feel and press on the body.
- If the doctor is right-handed, they will place their left hand under your right ribcage. You will be asked to take a deep breath and exhale slowly as the doctor attempts to 'grip' your liver between their hands. They will use the tips of their fingers to feel the liver's edge between the ribcage and the lower chest, checking for details such as shape, uniformity, texture, softness, and the clarity of the liver's border.
- The doctor will also assess the liver's surface texture to determine if it is lumpy, irregular, or if there are any small nodules. They will also check if the liver feels hard or firm. Additionally, they will ask if you feel any pain when they press on the area.

Blood Tests. Typically, your doctor will want to take a blood sample to assess liver function and health. Blood tests are commonly used to detect viral infections, such as hepatitis.
- The blood sample will provide liver enzyme levels, offering key insights into the health and functionality of the liver. Other tests may include: a complete blood count, viral hepatitis screening, and coagulation tests.
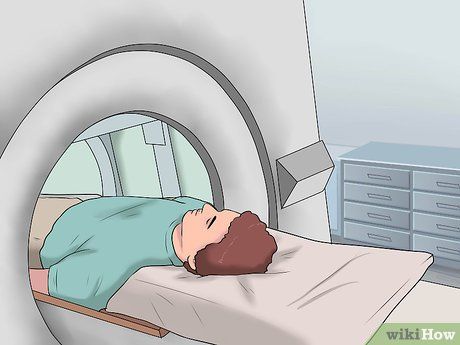
Imaging Tests. Imaging tests such as ultrasound, CT scans, and MRIs are commonly recommended to confirm diagnoses and evaluate the anatomical structure of the liver and surrounding tissues. These tests provide detailed information to help doctors make reliable assessments of the liver's condition.
- Abdominal Ultrasound — In this test, you will lie down while the doctor moves a probe across your abdomen. The probe emits high-frequency sound waves that bounce off organs, which are then recorded by a computer. These sound waves are converted into images showing the organs inside the abdominal cavity. Your doctor will guide you on how to prepare for this test, but typically, you should refrain from eating or drinking beforehand.
- Abdominal CT Scan — During a CT scan, cross-sectional images of the abdominal region are created using X-rays. You will lie on a narrow table that slides into the CT scanner and stay still as X-ray beams rotate around you. These beams are then converted into images on a computer. Your doctor will advise you on how to prepare for a CT scan. Sometimes, a special contrast dye is required, which may be administered through an intravenous line or orally. You might be asked to avoid eating or drinking before the scan.
- Abdominal MRI — This test uses magnetic fields and radio waves to create images of the inside of your abdomen instead of X-rays. You will lie still on a narrow table that slides into a large cylindrical MRI machine. For clearer images, contrast dye may be required, and your doctor will discuss this with you beforehand. Like other tests, you may need to refrain from eating or drinking before the MRI.
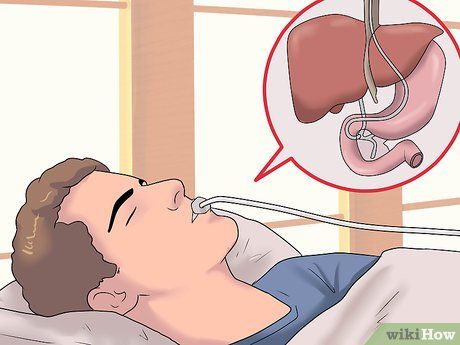
Endoscopic Retrograde Cholangiopancreatography (ERCP). This technique is used to detect issues in the bile ducts, which carry bile from the liver to the gallbladder and small intestine.
- During this procedure, you will be given sedative medication through an intravenous line in your arm. The doctor will then insert an endoscope through your mouth, down your esophagus and stomach, until it reaches the small intestine (near the stomach). A catheter will be passed through the endoscope and into the bile ducts connected to the pancreas and gallbladder. A contrast dye will then be injected into the bile ducts to make abnormalities easier to identify, followed by X-ray imaging.
- This test is usually performed after imaging tests such as ultrasound, CT, or MRI.
- As with many other tests, the doctor will explain the procedure and potential outcomes. You will need to sign a consent form for the ERCP procedure and refrain from eating or drinking for 4 hours before the test.
- ERCP can also be used therapeutically. For example, if there are gallstones or obstructions in the gallbladder, the doctor can use the procedure to remove them.
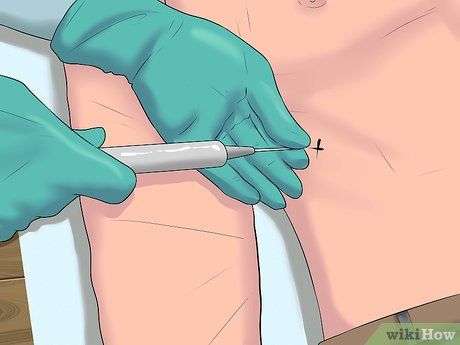
Biopsy. Liver enlargement and liver diseases are typically diagnosed through medical history review, clinical examination, blood tests, and imaging tests. However, a biopsy may be required in certain cases, especially if the diagnosis is unclear or there are concerns about cancer.
- In this procedure, a thin, long needle is inserted into the liver to collect a tissue sample, usually performed by a liver specialist (or a gastroenterologist or liver research expert). This is an invasive test, so you will be given anesthesia or a local anesthetic. The biopsy sample will then be sent to a laboratory for further analysis, especially to check for the presence of cancer cells.
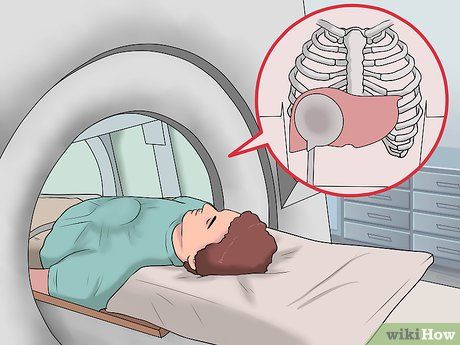
Magnetic Resonance Elastography (MRE). MRE, a relatively new imaging technique, combines MRI imaging with sound waves to produce images (elastographs) that assess tissue stiffness, in this case, the liver. Liver stiffness is a symptom of chronic liver disease that MRE can detect. This non-invasive test can serve as an alternative to liver biopsy.
- Magnetic Resonance Elastography is an emerging technique that is growing rapidly. Currently, MRE is available at only a few medical centers, but the number is increasing. You should consult with your doctor to determine whether this option is suitable for you.
Note on Risk Factors
Identifying the Risk from Hepatitis. Hepatitis A, B, and C cause liver inflammation and can lead to liver enlargement, along with a smooth, soft liver edge. You are at high risk of developing liver enlargement if you have any form of hepatitis.
- Liver damage occurs as blood cells and immune cells rush to the liver to combat the infection.

Consider If You Have Right-Sided Heart Failure. Right-sided heart failure can lead to liver enlargement, with a soft and smooth liver edge.
- This happens because blood accumulates in the liver due to the heart's inability to pump effectively. As the heart fails to perform its function, blood backs up into the liver.
Recognizing the Risk of Cirrhosis. Cirrhosis is a chronic disease that results in increased liver density due to fibrosis (excessive scar tissue production). Cirrhosis often results from a lifestyle that damages the liver. Notably, alcohol abuse can directly lead to cirrhosis.
- Cirrhosis can cause the liver to enlarge or shrink, but it is typically associated with liver enlargement.

Consider Genetic Diseases or Metabolic Disorders. Individuals with genetic diseases or metabolic disorders, such as Wilson's disease and Gaucher's disease, may also face a higher risk of liver enlargement.

Understanding the Risks of Cancer. Cancer patients may experience liver enlargement due to the spread of cancer cells (metastasis) into the liver. It is quite possible that your liver will enlarge if diagnosed with cancer, especially if the cancer originates in organs located near the liver.

Be Cautious of Alcohol Abuse. Consuming alcohol for years or exceeding a few drinks per week can cause liver damage and impair the liver's ability to regenerate. Both habits may lead to permanent damage to the structure and function of the liver.
- If alcohol consumption leads to liver dysfunction, the liver may enlarge and become swollen due to reduced drainage capacity. Fat can also accumulate in the liver if alcohol intake is excessive.
- The National Institute on Alcohol Abuse and Alcoholism defines "moderate drinking" as no more than 1 drink per day for women and 2 drinks per day for men.

Consider Medication Usage. Many over-the-counter medications can harm the liver if used over extended periods or in doses exceeding the recommended amount. The most toxic drugs for the liver include birth control pills, anabolic steroids, diclofenac, amiodarone, statins, and several others.
- If taking long-term medication, it is essential to undergo regular checkups and follow your doctor's advice.
- Acetaminophen (Tylenol), especially when overdosed, is a common cause of liver failure and may lead to liver enlargement. The risk is higher if acetaminophen is taken with alcohol.
- Note that certain herbal supplements like black cohosh, ephedra, and mistletoe may also increase the risk of liver damage.

Monitor Fatty Food Consumption. Frequently eating fatty foods, such as French fries, hamburgers, or any unhealthy foods, can result in fat accumulation in the liver, a condition known as fatty liver disease. The buildup of fat in the liver may gradually damage liver cells.
- Liver damage weakens the organ, causing it to swell due to decreased ability to process blood, toxins, and fat accumulation.
- It's important to note that being overweight or obese increases the risk of liver disease. A person is considered overweight or obese based on their body mass index (BMI), a measure of body fat. BMI is calculated by dividing a person's weight in kilograms (kg) by their height in meters (m) squared. A BMI between 25 and 29.9 is considered overweight, and a BMI over 30 is considered obese.
