Asthma is the most prevalent chronic illness among school-aged children, impacting around 7 million kids in the United States. This inflammatory condition narrows the airways, causing breathing difficulties, and sufferers often experience periodic "asthma attacks" with worsening symptoms. Without proper treatment, these attacks can escalate, leading to severe injury or even death. Therefore, it is crucial to quickly and accurately identify asthma attacks in children.
Steps
Listen to the child

Pay attention if the child mentions difficulty breathing. An older child who has previously experienced asthma attacks may sense when one is about to occur. If the child says, "I can't breathe" or is struggling to breathe, take their words seriously! In the early stages of an asthma attack, the child may wheeze, although this symptom may not be present during severe episodes.

Take chest pain complaints seriously. Children with asthma may also complain of chest pain or a tight feeling in their chest. Chest pain is quite common during an asthma attack because air gets trapped in the narrowed airways, leading to increased pressure in the chest. Due to the narrowed airways, breathing sounds may also become quieter.

Understand the limitations of children. Young children or those who have never experienced an asthma attack before may not be able to describe or mention difficulty breathing or chest pain. Instead, they may feel scared and describe their symptoms vaguely, such as saying, "I feel weird" or "I’m sick." Carefully observe children with asthma for signs of an attack, such as shallow breathing or wheezing. Do not assume a child is not having an asthma attack simply because they do not complain of breathing difficulties or chest pain.

Assess breathing rate. Infants and very young children (newborns to 6 years old) have a high metabolic rate, which means their breathing rate is also faster. Children in this age group cannot accurately describe their symptoms, so you must closely monitor their breathing patterns. If you have even the slightest concern about their breathing, check for other symptoms. The average breathing rate for this age group varies widely, but general reference ranges are as follows:
- Infants (under 1 year): 30-60 breaths per minute
- Toddlers (1-3 years): 24-40 breaths
- Preschoolers (3-6 years): 22-34 breaths
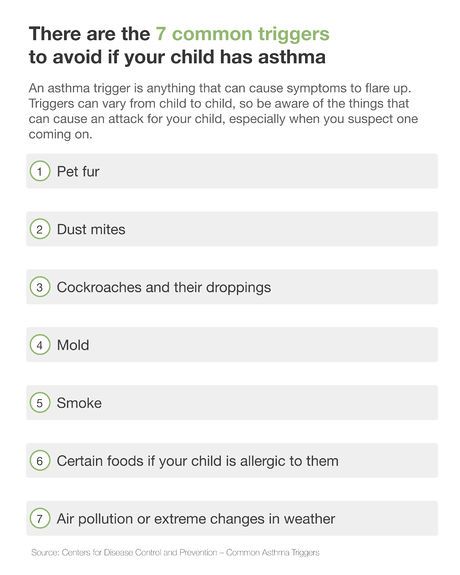
Watch for environmental triggers. Most children with asthma begin showing signs by the age of 5, when they start reacting negatively to asthma triggers. A trigger is anything that causes symptoms to flare up. Triggers vary for each child, so you must pay attention to what might cause an attack, especially if you suspect one is imminent. Some triggers (like dust mites and pet dander) can be eliminated, while others (like air pollution) require careful monitoring. Common triggers include:
- Pet dander: vacuum or clean frequently to remove dander.
- Dust mites: use mattress and pillow covers, wash bedding regularly, avoid stuffed animals in the child’s room, and avoid down-filled pillows or comforters.
- Cockroaches: cockroaches and their droppings are common asthma triggers. Keep food and water sources sealed, clean up spills, and consider pest control measures.
- Mold: caused by moisture, so use a humidity monitor and a dehumidifier to prevent mold growth.
- Smoke: whether from cigarettes or wood fires, smoke can trigger asthma. Even smoking outside leaves residue on clothes and hair that can harm the child.
- Certain foods: eggs, milk, peanuts, soy products, wheat, fish, shellfish, salads, and fresh fruits can trigger asthma if the child is allergic.
- Air pollution and extreme weather changes.

Observe the child’s behavior. Keeping the environment clean and free of asthma triggers may not be enough. Strong emotions like sadness, excitement, or fear can increase the risk of an asthma attack. Similarly, excessive physical activity can leave the child breathless, causing rapid, deep breathing that may lead to an asthma attack.

Properly treat respiratory infections. Viral or bacterial infections in the upper or lower respiratory tract can trigger asthma attacks. Take your child to a pediatrician if they show signs of a respiratory infection. They may need medication to control the infection or speed up recovery.
- Remember that antibiotics only treat bacterial infections. Viral respiratory infections should be managed rather than treated directly.
Assess the child's breathing

Watch for signs of rapid breathing. Typically, an adult's breathing rate does not exceed 20 breaths per minute. Depending on their age, children may have a faster resting respiratory rate. Be alert for any signs of abnormally rapid breathing.
- Children aged 6-12 usually breathe 18-30 times per minute.
- Children aged 12-18 typically breathe 12-20 times per minute.

Observe if the child is struggling to breathe. Normally, young children primarily use their diaphragm to breathe. However, children with asthma often rely on other muscles to help draw in more air. Look for signs that their neck, chest, or abdominal muscles are working harder than usual.
- A child struggling to breathe may lean forward with their hands on their knees or a table. If you notice this posture, it could indicate an asthma attack.

Listen for wheezing sounds. Children with asthma often produce a faint, vibrating whistling sound when breathing, especially during exhalation, as air is forced through narrowed airways.
- Wheezing can be heard during both inhalation and exhalation, but in mild asthma attacks or the early stages of a severe attack, wheezing may only be noticeable during exhalation.

Pay attention to coughing sounds. Asthma is the most common cause of chronic coughing in children. Coughing increases pressure in the airways, forcing them to expand and temporarily improving airflow. While coughing may make breathing easier for the child, it is a symptom of a larger issue. Children often cough when their bodies are trying to expel environmental triggers, which can cause asthma attacks.
- However, coughing can also indicate a respiratory infection, which may trigger an asthma attack.
- Persistent nighttime coughing is a common symptom of mild to moderate asthma in children, but prolonged coughing may signal an ongoing asthma attack.
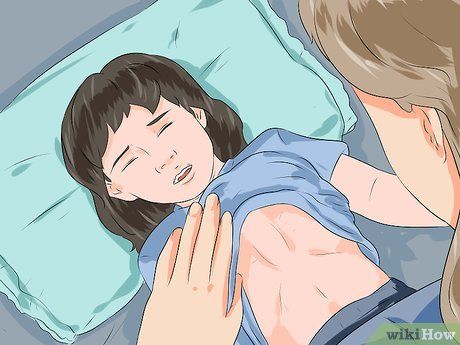
Look for retractions. Retractions are visible "pulling in" of the skin between or below the ribs or around the collarbone when a child breathes. This occurs when muscles work harder to draw in air, but the airways are too constricted to allow proper airflow.
- If mild retractions are observed, seek medical attention as soon as possible. Moderate to severe retractions require immediate emergency care.

Watch for flaring nostrils. When a child is struggling to breathe, you may notice their nostrils flaring. This is a helpful indicator of an asthma attack in infants and very young children, who cannot verbalize symptoms or assume the same postures as older children.

Look for signs of a "silent chest." If the child appears distressed but you do not hear wheezing, a "silent chest" may be occurring. This is a sign of severe asthma, where the airways are so constricted that there is not enough air to produce wheezing sounds. Seek emergency care immediately. The child may become exhausted from trying to breathe and fail to expel carbon dioxide, leading to insufficient oxygen intake.
- Another sign of insufficient oxygen is the child’s inability to speak in full sentences, which also requires urgent medical attention.
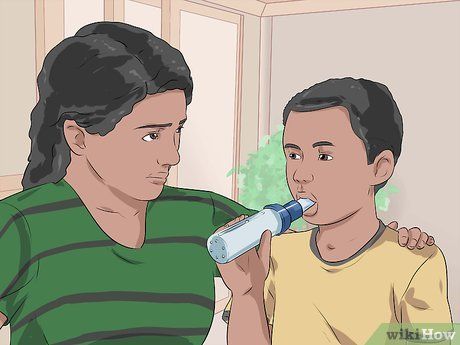
Use a peak flow meter to assess asthma severity. A peak flow meter is a simple device used to measure "peak expiratory flow rate" (PEFR). Daily measurements can help establish your child’s normal PEFR range. Abnormal readings serve as early warning signs of an impending asthma attack. Normal PEFR ranges depend on the child’s age and height; consult a doctor to understand the values for each "zone" and the appropriate actions for red or yellow zones. Generally:
- A PEFR reading of 80-100% of the personal best indicates the "green zone" (low risk).
- A PEFR reading of 50-80% of the personal best indicates the "yellow zone" (moderate risk; continue monitoring and follow the doctor’s care plan).
- A PEFR reading below 50% of the personal best indicates a high risk of an asthma attack. Administer immediate medication and seek hospital care.
Assess the child's appearance

Evaluate the overall appearance. Children experiencing an asthma attack often struggle to breathe, which can be evident from their outward appearance. If you notice the child exerting effort to breathe or sense that something is wrong, trust your instincts. Administer their inhaler or other prescribed emergency medication and seek immediate medical attention if necessary.

Look for pale, cold, and clammy skin. During an asthma attack, the child’s body works harder just to breathe, often causing the skin to sweat or become damp. Instead of a flushed or rosy complexion from physical exertion, the skin may appear pale or white. Blood appears red when oxygenated, so a lack of oxygen can prevent the usual pinkish hue from showing.

Watch for a bluish tint on the skin. If you notice a bluish tint on the skin, lips, or fingernails, the child is experiencing a severe asthma attack. This indicates a critical lack of oxygen and requires immediate emergency care.
Caring for a child during an asthma attack

Administer asthma medication. If your child has a history of asthma, you likely have prescribed medication at home, often in the form of an inhaler. In the event of an asthma attack, administer the inhaler immediately. While using an inhaler is straightforward, improper use can reduce its effectiveness. Follow these steps for correct usage:
- Remove the cap and shake the inhaler vigorously.
- Spray a small amount into the air if necessary. For a new inhaler or one that hasn’t been used in a while, prime it by spraying a test dose.
- Ask the child to exhale fully, then inhale as you release a puff of medication.
- Encourage the child to take slow, deep breaths for 10 seconds.
- Always use a spacer to ensure the medication reaches the lungs instead of the throat. Consult your doctor for guidance on using an inhaler with a spacer.

Check the inhaler label before administering a second dose to determine if a waiting period is required. If the medication is a β2-agonist like albuterol, wait at least one minute before giving another dose. For other types of medication, a waiting period may not be necessary.

Monitor the medication’s effectiveness. Typically, the medication takes effect within minutes. If there’s no improvement, administer another dose as recommended on the label or by your doctor. In some cases, your doctor may advise giving an additional dose immediately. If symptoms persist, seek emergency medical care.

Contact your doctor if symptoms are mild but prolonged. Mild symptoms may include coughing, wheezing, or slight difficulty breathing. Reach out to your pediatrician if asthma symptoms remain mild but do not improve after using medication. In some cases, the doctor may need to treat the child directly or provide further instructions.

Seek emergency care for severe and prolonged symptoms. Signs like a "silent chest" or bluish lips and nails indicate a severe lack of oxygen. Immediate treatment is crucial to prevent brain damage or death.
- If asthma medication is available, administer it on the way to the emergency room, but do not delay seeking care.
- Delayed treatment during a severe asthma attack can lead to permanent brain damage or even death.
- Call emergency services if your child’s bluish tint does not improve after medication or spreads beyond the lips and nails.
- Call for emergency help if your child becomes unconscious or is difficult to wake.

Call emergency services for asthma attacks triggered by allergic reactions. If the asthma attack is caused by food allergies, insect stings, or medication, seek emergency care immediately. These types of allergies can escalate quickly and lead to airway obstruction.

What to expect in the emergency room. First, the doctor will confirm the signs and symptoms of asthma. Upon arrival, medical staff may provide oxygen if necessary and administer additional medication. In severe cases, intravenous corticosteroids may be required. Most patients recover under professional care, and your child may be discharged early. However, if there’s no improvement after several hours, an overnight hospital stay may be necessary.
- The doctor may order a chest X-ray, pulse oximetry, or blood tests.
Tips
- Identify situations that may trigger or worsen asthma attacks, such as exposure to allergens, prolonged physical activity, secondhand smoke, respiratory infections, and strong emotions.
Warnings
- Asthma is a serious and potentially life-threatening condition. Always seek immediate treatment for children exhibiting severe symptoms, including difficulty breathing, bluish skin, rapid pulse, excessive sweating, sudden restlessness, or drowsiness.
