Experts state that the most common symptoms of knee arthritis include pain, swelling, and stiffness in the knee joint. Studies show that the most prevalent types of arthritis are osteoarthritis and rheumatoid arthritis. In osteoarthritis, the cartilage in the knee gradually wears away over time, while rheumatoid arthritis is a chronic autoimmune disorder affecting the joint lining. If you suspect you have knee arthritis, you'll want to address the symptoms quickly. Although you should consult a doctor, there are some signs you can identify on your own.
Steps
Recognizing Symptoms of Knee Arthritis

- Genetics. Genetic factors may predispose you to certain types of arthritis (e.g., rheumatoid arthritis or systemic lupus erythematosus). A family history of arthritis increases your risk.
- Gender. Men are more prone to gout—a type of arthritis caused by high uric acid levels—while women are more likely to develop rheumatoid arthritis.
- Age. The risk of arthritis increases with age.
- Obesity. Excess weight adds pressure to the knee joints and can elevate the risk of arthritis.
- History of joint injury. Knee injuries can contribute to joint degeneration.
- Infections. Bacteria can cause joint infections and exacerbate various types of arthritis.
- Occupation. Jobs requiring frequent knee bending or squatting can increase the risk of knee osteoarthritis.
- If you have one or more risk factors, consult a doctor about preventive measures (or see the prevention section below).

- Pain worsens during activity.
- Reduced or limited range of motion.
- Knee stiffness.
- Swelling and knee joint pain.
- A feeling of joint weakness.
- Fatigue and discomfort (often occurring during rheumatoid arthritis flare-ups).
- Mild fever and chills (common during rheumatoid arthritis flare-ups).
- Joint deformity (knees bending inward or bow-leggedness) is often a more severe symptom of untreated arthritis.

- Activities that put pressure on the knee joint, such as long walks, climbing stairs, or standing for extended periods, can exacerbate arthritis pain.
- In severe cases of knee arthritis, pain may even occur while sitting or lying down.
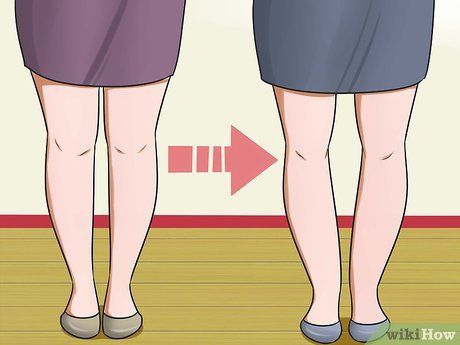
- When cartilage on one side of the knee wears down, you might notice the knee bending inward or becoming bow-legged.
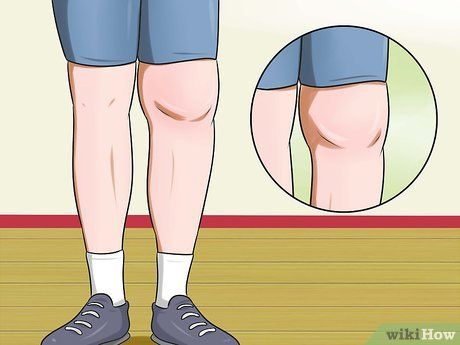
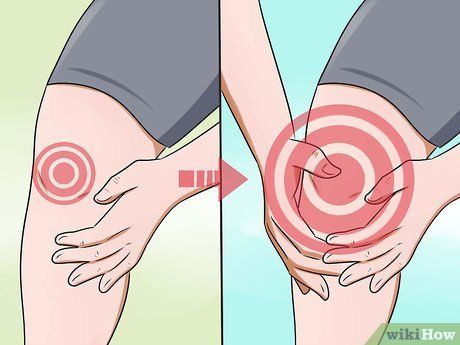
- Those with rheumatoid arthritis often experience periods of worsening symptoms called 'flare-ups.' During these phases, symptoms intensify, peak, and then gradually subside.

- The doctor will check for swelling, redness, and warmth in the knee, as well as assess your range of motion. If arthritis is suspected, they may recommend one or more of the following tests to confirm the diagnosis:
- Tests to analyze markers of arthritis in blood, urine, and/or joint fluid. Joint fluid is extracted by inserting a needle into the joint space and drawing it out.
- Ultrasound imaging to visualize soft tissues, cartilage, and fluid-filled structures in the knee. Ultrasound can also guide needle placement during joint fluid extraction.
- X-rays to detect cartilage loss, bone damage, and/or bone spurs.
- Computed tomography (CT) scans to visualize the bones in the knee. CT images are taken from multiple angles and combined to create cross-sectional views of internal structures.
- Magnetic resonance imaging (MRI) can provide detailed cross-sectional images of soft tissues around the joint, such as cartilage, tendons, and ligaments.
Preventing Knee Arthritis

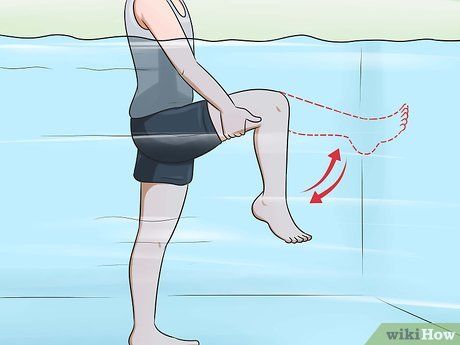
- Water exercises are an excellent option for individuals with joint issues.
- Using a cane or crutch on the side opposite the affected knee can help reduce pressure on the joint.

- While they may help manage pain, joint supplements do not regenerate cartilage. Reliable studies show they are no more effective than placebos but carry minimal risks (though they are more expensive). Therefore, most orthopedic specialists recommend trying them.
- Some doctors suggest taking joint supplements for three months to assess their effectiveness.
- Over-the-counter joint supplements are not regulated by the FDA, so consult your doctor before use.
Treating Knee Arthritis

- Always consult a doctor before using over-the-counter medications for arthritis, especially if you are already taking other arthritis treatments.
- Never exceed the recommended dosage, including for over-the-counter anti-inflammatory drugs. Overdosing on NSAIDs can be life-threatening.
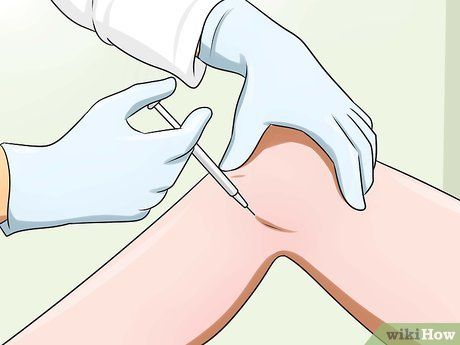
- Your doctor may recommend hyaluronic acid injections (also known as artificial joint fluid or joint lubricant injections) into the knee joint.
- While not always effective, these injections can help alleviate symptoms for 3-6 months.
- Disease-modifying antirheumatic drugs (DMARDs), such as Methotrexate or Hydroxychloroquine, slow or prevent the immune system from attacking the joints.
- Biologics, like Etanercept and Infliximab, target specific protein molecules involved in the immune response that leads to arthritis.
- Corticosteroids, such as Prednisone and Cortisone, reduce inflammation and suppress the immune system. They can be taken orally or injected directly into the affected joint.

- In joint fusion surgery, the doctor removes the ends of the two bones in the joint, then locks them together until they heal into a single, solid bone.
- In joint replacement surgery, the doctor removes the damaged joint and replaces it with an artificial one.
Advice
- If you suspect you are experiencing early signs of arthritis, you should see a doctor immediately. Early treatment can alter the progression of certain types of arthritis.
- The treatment process for knee arthritis should start with the most basic steps and then progress to more complex ones, which may include surgery.
- Not all treatment methods are suitable for every patient, so you need to discuss with your doctor to determine the most appropriate treatment.
