According to the National Stroke Association, approximately 800,000 people experience a stroke each year. Every four minutes, one person dies from a stroke, but 80% of strokes are preventable. Stroke is the fifth leading cause of death and a major cause of disability among adults in the United States. There are three types of stroke with similar symptoms but different treatment methods. A stroke occurs when blood flow to a part of the brain is suddenly blocked, preventing cells from receiving oxygen. If blood flow is not quickly restored, brain cells die, leading to physical or mental disabilities. Recognizing symptoms and risk factors is crucial for timely medical intervention in the case of a stroke.
Steps
Identify the Signs and Symptoms

Facial or Limb Weakness. The person may struggle to hold objects or suddenly lose balance while standing. Look for signs that one side of their face or part of their body has become weak. A section of their mouth may droop when they smile, or they may be unable to raise both arms above their head.

Confusion or difficulty with speaking or understanding speech. When a specific part of the brain is affected, the person may struggle with pronouncing words and understanding what others are saying. They may seem confused when listening to you, reacting in ways that suggest they don't comprehend, speaking unclearly, or using words that don't relate to the conversation. This can be a serious sign. Call emergency services immediately, and try to keep the person calm.

Ask if the person is experiencing vision problems in one or both eyes. A stroke can suddenly impact vision significantly. One eye or both may experience partial or complete blindness, or the person may see double (if they cannot speak, ask them to nod or shake their head if possible). You might notice the person turning to the left to look at what is happening in their left eye's field of vision with their right eye.

Watch for signs of loss of coordination or balance. When a person's legs or arms become weak, you may observe difficulty in maintaining balance or coordination. The person might have trouble picking up a pen or walking due to one leg not functioning properly. You may also notice them becoming weak, suddenly slipping, or falling.

Sudden severe headache. A stroke, often referred to as a 'brain attack,' can cause an abrupt, severe headache, often considered the worst headache a person has ever experienced. It may be accompanied by nausea and vomiting due to increased pressure in the brain.
Pay attention to symptoms of a Transient Ischemic Attack (TIA). TIA occurs similarly to a stroke (commonly known as a 'mini-stroke'), but it lasts less than five minutes and does not cause permanent damage. However, it remains a medical emergency that requires evaluation and treatment to reduce the risk of it progressing into a full stroke. The risk of a stroke is high within hours or days after TIA symptoms appear. Doctors believe these symptoms are caused by a temporary blockage of a brain artery.
- About 20% of TIA patients will experience a stroke within 90 days, and about 2% of these strokes occur within the next 2 days.
- Over time, TIA can lead to Multi-Infarct Dementia (MID) or memory loss.

Remember the acronym FAST. FAST stands for Face, Arm, Speech, and Time, and it reminds you of the signs to check for if you suspect someone may be at risk of a stroke, as well as the critical importance of time. If you notice these signs, you should immediately call your local emergency services. The treatment and effectiveness of treatment will depend on every minute.
- Face: Ask the person to smile and see if one side of their face droops.
- Arm: Ask the person to raise both arms. Can they do it? Does one arm drop?
- Speech: Is the person slurring their speech? Can they talk? Are they confused when asked to repeat a short sentence?
- Time: Call emergency services immediately if these symptoms are present. Don’t hesitate.
Stroke Treatment

Take appropriate action. If you or someone nearby experiences any of the above symptoms, seek emergency medical treatment immediately. These signs are clear indicators of stroke risk.
- You should still call your local medical center even if the symptoms disappear quickly or are painless.
- Make sure to note the time you first noticed the symptoms to help healthcare professionals determine the right treatment approach.

Provide full medical history and test results to the doctor. Even in an emergency, doctors will carefully review the patient's medical history and test results before conducting further tests and treatment. Here are some medical tests that may be used:
- CT Scan: A type of X-ray imaging that provides detailed images of the brain after a stroke.
- MRI: Helps identify areas of brain damage and can be used in place of or alongside CT scans.
- Carotid Ultrasound: A non-invasive test used to check for narrowing of the carotid arteries. This test is useful after a TIA (transient ischemic attack) when no lasting brain damage has occurred. If a 70% blockage is detected, surgery may be required to prevent a stroke.
- Carotid Angiography: Uses a catheter inserted into the vein and injected dye to create images of the carotid arteries.
- EKG (Electrocardiogram): Assesses heart health and identifies risk factors for stroke.
- Blood Tests: Used to check for low blood sugar levels (a sign of stroke) and clotting issues, which indicate a high risk of hemorrhagic stroke.
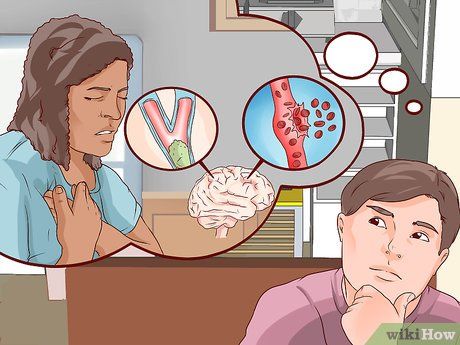
Identify the types of stroke. While the symptoms and impacts of a stroke are similar, there are different types of strokes, each with distinct causes and treatments. Doctors will determine the type of stroke based on test results.
- Hemorrhagic Stroke: Occurs when blood vessels in the brain rupture or leak. Blood leaks into or around the brain, causing pressure and potentially damaging brain tissue. The most common type is intracerebral hemorrhage, where a blood vessel inside the brain bursts. Subarachnoid hemorrhage occurs when blood leaks around the brain into the space between the brain and its protective coverings, known as the subarachnoid space.
- Ischemic Stroke: The most common type, accounting for about 83% of stroke cases. It occurs when a blood clot (also known as a thrombus) blocks a brain artery or when atherosclerosis prevents proper blood and oxygen flow to the brain, leading to a lack of oxygen in the brain (cerebral ischemia).
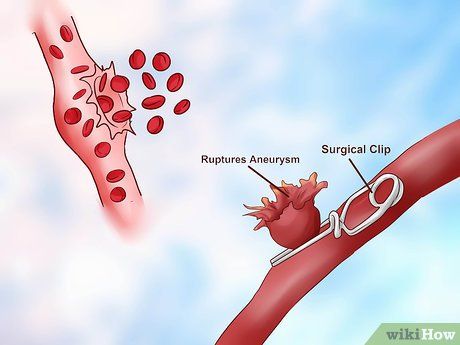
Emergency treatment for hemorrhagic stroke. In the case of a hemorrhagic stroke, doctors will quickly control the bleeding. Some treatment methods include:
- Surgical clipping of an aneurysm or endovascular embolization to stop the bleeding if the aneurysm is the cause of the stroke.
- Surgery to drain blood that hasn’t been reabsorbed into the brain tissue and to relieve pressure within the brain (usually for severe cases).
- Surgery to remove an arteriovenous malformation (AVM) if it's accessible. Stereotactic radiosurgery, a minimally invasive technique, is used to remove the AVM.
- Bypass surgery in the brain to increase blood flow in certain specific cases.
- Immediately stop the use of blood-thinning medications as they make it harder to control the bleeding in the brain.
- Supportive medical care as blood re-circulates throughout the body, similar to post-hematoma recovery.

Medications and treatments for ischemic stroke. Medication and medical treatments may be used to prevent further stroke or brain damage. Some of these include:
- TPA (tissue plasminogen activator) to dissolve the blood clot in the brain artery. This medication is administered via injection into the arm of the person having a clot-induced stroke and must be given within four hours of the onset of symptoms. The sooner it’s given, the better the outcome.
- Antiplatelet drugs to prevent blood clotting and brain damage. These must be given within 48 hours and may be more dangerous for hemorrhagic stroke patients, so a precise diagnosis is essential before use.
- Carotid endarterectomy or angioplasty if the patient has heart disease. In this procedure, surgeons remove plaque or clear the carotid artery if it’s blocked by a membrane or becomes thickened and stiff. This procedure helps open the carotid artery and provides more oxygenated blood to the brain if there’s at least a 70% blockage.
- Thrombectomy therapy where a catheter is inserted into the throat and advanced to the brain to deliver medication directly to the clot that needs to be removed.
Identifying risk factors

Consider the factor of age. Age is one of the most significant risk factors when identifying stroke risk. The risk of stroke nearly doubles every ten years after the age of 55.

Take into account prior strokes or TIAs. One of the largest risk factors for stroke is if someone has had a prior stroke or a TIA (transient ischemic attack, or 'mini-stroke'). Work with your doctor to minimize any other risk factors if you have experienced either of these conditions before.

Note that women are generally at a higher risk of stroke-related death. While men have a higher incidence of strokes, women are more likely to die from one. The use of birth control pills also increases the stroke risk for women.

Be aware of atrial fibrillation (AF). Atrial fibrillation is a condition where the heart beats rapidly and irregularly in the left atrium. Doctors can diagnose AF through an electrocardiogram (ECG).
- Symptoms of AF include a fluttering sensation in the chest, chest pain, dizziness, shortness of breath, and fatigue.
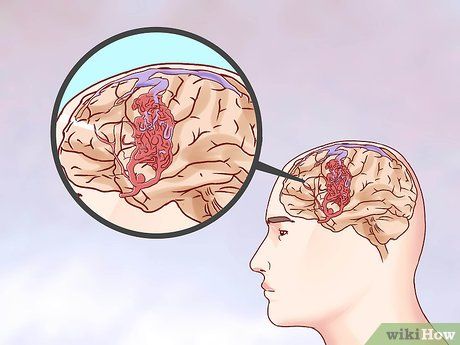
Be mindful of arteriovenous malformations (AVM). These malformations cause blood vessels in or around the brain to bypass normal tissue, increasing the risk of stroke. Most AVMs are genetic (but not always hereditary), and they affect less than 1% of the population. However, AVMs are more commonly found in men than in women.

Testing for peripheral artery disease. Peripheral artery disease is a condition where arteries narrow, leading to blood clots and reduced blood flow throughout the body.
- The legs are typically the most affected area.
- Peripheral artery disease is a significant risk factor for stroke.
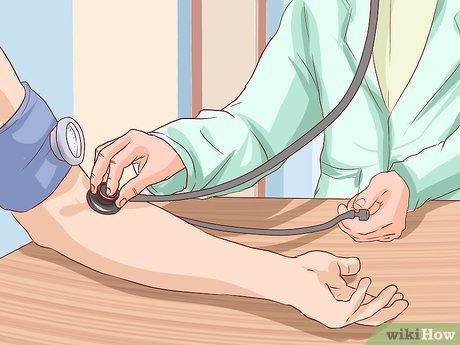
Be cautious with blood pressure. High blood pressure places excessive strain on arteries and other blood vessels. This can create weak points that may rupture easily (hemorrhagic stroke) or form bulging areas filled with blood, known as aneurysms.
- Damage to the arteries can lead to blood clots and poor circulation, resulting in ischemic stroke.

Understand the risks of diabetes. If you have diabetes, your risk of stroke is elevated due to the health complications associated with the condition. Diabetes can lead to other health issues such as high cholesterol, high blood pressure, and heart disease, all of which increase your likelihood of experiencing a stroke.
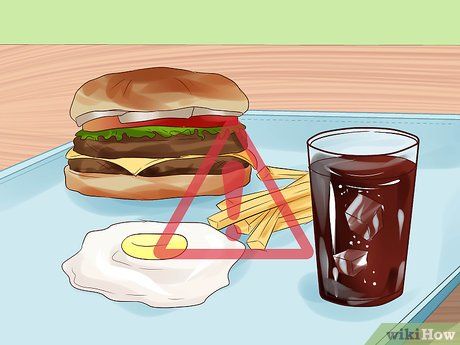
Lower your cholesterol levels. High cholesterol is a significant risk factor for stroke. It can cause plaque buildup in the arteries, which can impede blood flow and result in a stroke. Maintain a diet low in trans fats to help keep your cholesterol levels within a healthy range.

Avoid smoking. Smoking negatively impacts both the heart and blood vessels. Additionally, nicotine increases blood pressure. These factors together elevate your stroke risk.
- Even exposure to secondhand smoke can increase the stroke risk for non-smokers.

Limit alcohol consumption. Excessive alcohol intake can lead to several health issues, such as high blood pressure and diabetes, both of which raise your risk of stroke.
- Alcohol can cause blood platelets to clump together, increasing the risk of stroke or heart attack. Overconsumption can also lead to chronic heart disease and irregular heartbeats like atrial fibrillation, which can form blood clots and cause a stroke.
- The U.S. Centers for Disease Control and Prevention recommend that women limit alcohol to one drink per day, while men should not exceed two drinks daily.

Maintain a healthy weight to avoid obesity. Obesity can lead to several health conditions such as diabetes and high blood pressure, both of which increase your risk of stroke.

Exercise to maintain good health. Regular physical activity can help prevent some of the issues mentioned earlier, such as high blood pressure, high cholesterol, and diabetes. Aim to engage in cardiovascular exercises for at least 30 minutes a day to keep your heart healthy.

Consider family history. Certain ethnic groups have a higher risk of stroke compared to others due to a combination of physical and genetic factors. African Americans, Hispanics, Native Americans, and Alaska Natives are at greater risk due to their genetic background.
- Both African Americans and Hispanics also have a higher risk of sickle cell disease, where the red blood cells become abnormally shaped, potentially blocking blood flow and increasing the risk of ischemic stroke.
Advice
- Remember FAST to quickly assess the situation and seek medical assistance immediately in the event of a stroke.
- Those suffering from ischemic strokes tend to have better outcomes if treated within the first hour of symptom onset. Treatment may involve medication and/or medical interventions.
Warning
- Although a TIA (Transient Ischemic Attack) doesn’t cause permanent damage, it serves as a warning that a stroke or heart failure could be imminent. If you or a loved one experience stroke-like symptoms that disappear within a few minutes, it’s crucial to seek medical attention immediately to reduce the risk of a severe stroke.
- While this article provides some medical insights on strokes, it should not be considered as medical advice. Always seek professional care right away if you suspect that you or someone close to you might be at risk for a stroke.
