Chikungunya fever is a viral disease transmitted to humans by mosquitoes infected with the virus. These mosquitoes can also carry other diseases such as dengue and yellow fever. Chikungunya is found worldwide, especially in the Caribbean, tropical regions of Asia, Africa, South America, and North America. There is currently no cure or vaccine available for this disease, and treatment primarily focuses on alleviating the symptoms. It is crucial to recognize the signs and symptoms of the disease, manage the symptoms, and prevent complications.
Steps
Identifying Signs and Symptoms
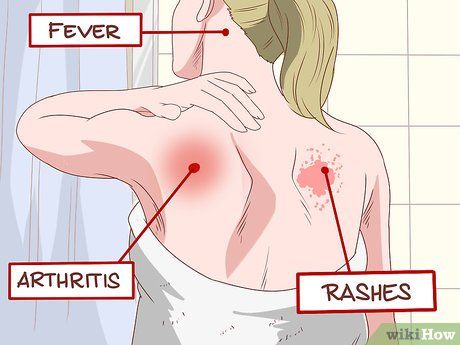
- Fever: Typically ranging from 39 to 40.5 °C, lasting from three days to a week. Patients may experience a biphasic fever (fever disappearing for a few days, followed by a mild fever returning (38–39 °C)). During this time, the virus multiplies in the patient’s blood and spreads to other parts of the body.
- Arthritis (Joint Pain): Patients often feel pain in the small joints of the hands, wrists, ankles, and larger joints like the knees and shoulders, but not in the hips. Around 70% of patients experience pain migrating from one joint to another (as pain in one joint subsides, it moves to another). Pain is usually worst in the morning but tends to improve with light exercise. Joints may also swell or feel tender, and patients may develop tenosynovitis. Joint pain typically resolves in 1 to 3 weeks, and the intense pain usually eases after the first week. However, in some cases, joint pain may persist for up to a year.
- Rash: About 40% to 50% of patients develop a rash. The most common type is a maculopapular rash, which consists of red spots with swollen patches on top, appearing 3-5 days after fever and lasting 3 to 4 days. The rash usually starts on the arms, then spreads to the face and torso. To check, remove your shirt and look in a mirror for areas of swelling and redness, and don’t forget to inspect the back, neck, and underarms by raising your arms.

- Raynaud's phenomenon is a condition where blood flow to the hands and feet is reduced in response to cold temperatures or physical stress. Check the fingertips for any signs of coldness or bruising.

- If you have underlying joint conditions like rheumatoid arthritis, you may be more prone to entering the chronic phase after chikungunya infection.
- Though rare, there have been reports of rheumatoid arthritis developing after chikungunya infection. The average onset time is around 10 months.

- Muscle pain (pain in muscles/back)
- Headache
- Sore throat
- Abdominal pain
- Constipation
- Swollen lymph nodes in the neck
- Leptospirosis: Pay attention to calf pain (the inner calf muscle just below the knee) when walking. You should also check for redness in the whites of your eyes (subconjunctival hemorrhage). This phenomenon is caused by small blood vessels bursting. Recall if you’ve been near livestock or near water sources contaminated by livestock, as these animals can transmit the disease through water and soil.
- Dengue Fever: Take note if you’ve been exposed to mosquitoes or bitten in tropical climates like Africa, South America, Central America, the Caribbean, India, and Southern North America. Dengue fever is more common in these areas. Check the mirror for any bruising on your skin, bleeding, or redness in the whites of your eyes, bleeding gums, or frequent nosebleeds. Hemorrhaging is the key difference between dengue fever and chikungunya fever.
- Malaria: Pay attention if you’ve been exposed to mosquitoes in malaria-endemic regions like South America, Africa, India, the Middle East, and Southeast Asia. Watch for cold chills followed by fever and sweating, lasting 6 to 10 hours. These stages can recur.
- Meningitis: Watch for an outbreak in densely populated areas. If you live in an area with an outbreak, you could be at risk. Check your temperature and watch for a stiff or painful neck or difficulty moving it. Severe headaches and fatigue/confusion may accompany it. You might also notice a rash with small red, brown, or purple spots that may enlarge into blisters. The rash usually appears on the trunk, legs, palms, and soles of your feet.
- Rheumatic Fever: Rheumatic fever typically occurs after streptococcal infections, such as strep throat. It is not transmitted by mosquito bites and is more common in children aged 5-15 years. Check if a child experiences pain in multiple joints with migrating pain (relief in one joint while another becomes painful), along with a fever similar to chikungunya. However, the main distinction is the presence of involuntary movements (chorea), small, painless lumps under the skin, and a characteristic rash. The rash may be flat or slightly raised, with jagged edges (erythema marginatum), forming rings with a bright pink outer edge and a lighter inner area.
Treating the Symptoms of Chikungunya Fever

- Fever lasting longer than five days or above 39°C
- Dizziness (possibly due to neurological issues or dehydration)
- Cold fingers or toes (Raynaud's phenomenon)
- Oral bleeding or bruising under the skin (this could indicate dengue fever)
- Rash
- Pain, redness, stiffness, or swelling in joints
- Low urine output (could be due to dehydration leading to kidney damage)

- Virus culture tests to detect viral growth. This is typically done within the first three days of the illness, when the virus is replicating rapidly.
- RT-PCR (Reverse Transcription Polymerase Chain Reaction) methods use genetic codes for the virus-specific proteins to amplify the chikungunya-specific genes. If it is chikungunya, the test will show elevated chikungunya gene levels on a computerized graph.
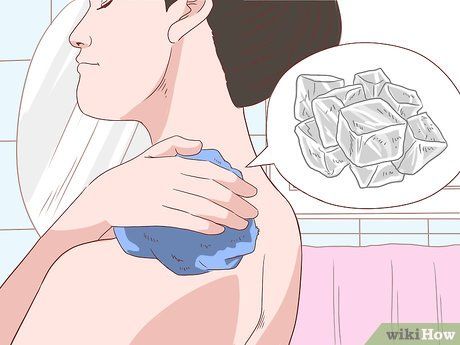
- Apply cold compresses to reduce pain and swelling. You can use frozen vegetables or meat packs, or ice bags. Wrap a towel around the cold packs and place them on the affected area. Avoid applying cold packs or ice directly to the skin as it may cause tissue damage.

- If you have a history of liver or kidney problems, consult a doctor before taking paracetamol/acetaminophen. Ask a pediatrician or pharmacist for appropriate dosages for children.
- Avoid taking aspirin or non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or naproxen. Since chikungunya shares symptoms with other mosquito-borne diseases like dengue fever, which can cause bleeding, NSAIDs and aspirin may increase the risk of bleeding. The doctor needs to rule out dengue before recommending NSAIDs for joint pain relief.
- If your joint pain is severe or doesn’t improve with NSAIDs, the doctor may prescribe hydroxychloroquine 200mg once daily or chloroquine phosphate 300mg daily, for up to 4 weeks.

- Sitting in a chair. Stretch one leg parallel to the floor for 10 seconds, then lower it, keeping the foot flat on the floor. Repeat with the other leg. Perform this exercise multiple times a day, 2 or 3 times, with 10 repetitions for each leg.
- Try standing on your tiptoes, with feet close together, and moving your heels up and down.
- Lie on your side. Raise one leg high for about 1 second, then lower it and place it on the other leg. Do this 10 times. Then, turn to the other side and repeat the motion. Perform 10 repetitions for each leg, several times a day.
- You may also try your own light exercises. Just avoid heavy movements or weights.

- Be cautious with antihistamines, as they may cause drowsiness. Avoid driving or operating machinery after taking the medication.
- Soaking in a warm bath with colloidal oatmeal may help soothe the skin.
- Persistent dark spots on the skin can be treated with hydroquinone products. These products help lighten dark spots.
- There are many solutions and creams available for treating irritated skin, so it’s best to consult a doctor to determine the best option for your condition.

- Eupatorium perfoliatum 200C: This homeopathic remedy is a top choice for treating chikungunya fever, derived from a plant extract that you should use when symptoms appear. It can reduce symptoms and joint pain. Take 6 drops every month when symptoms are present.
- Wild Chrysanthemum: This flower extract is used to treat chikungunya symptoms by enhancing the immune system’s effectiveness. Take 40 drops daily, divided into three doses.
Be aware of complications and prevent chikungunya fever

- The chikungunya virus can enter the heart muscle and cause myocarditis, which leads to abnormal heart rhythms.

- If you notice neurological damage starting from your feet or hands, you may have Guillain-Barré syndrome. Watch for reduced sensation, reflexes, and movement in both sides of the body. Also, be alert to sensations of sharp pain, burning, tingling, or pinpricks on both sides of the body. This condition can progress to the upper body and cause difficulty breathing due to nerve damage affecting the respiratory muscles.
- If you experience difficulty breathing or any of the symptoms mentioned above, call emergency services immediately.

- If you're having trouble seeing objects straight ahead (central vision) or if the colors of objects appear duller than usual, it could be optic neuritis.

- If left untreated, hepatitis can progress to liver failure.

- Your doctor may perform further tests to assess kidney function and could administer intravenous fluids if dehydration is severe.
- Stay indoors or only venture out when it's dark. Although mosquitoes can bite at any time, they are most active during the day, especially when transmitting chikungunya.
- Wear long pants and long-sleeved shirts to protect your skin from mosquito bites. Opt for light-colored clothing to make it easier to spot mosquitoes and other insects on your clothes.
- Sleep under a mosquito net to avoid bites.
- Use insect repellent with at least 20% DEET. You can also use other active ingredients such as eucalyptus oil, picaridin, or IR3535. The higher the concentration of active ingredients, the longer the repellent works.
Advice
- Hydroxychloroquine and Chloroquine phosphate are medications commonly used for treating rheumatoid arthritis, but they may also be effective for alleviating severe joint pain associated with chikungunya fever. X-ray scans can help identify any damage or changes in joint cartilage.
Warning
- Avoid taking aspirin as it can lead to stomach or intestinal bleeding, as well as Reye's syndrome in children under 18. Reye's syndrome is a serious condition that affects children between 4 and 12 years old, causing severe liver and brain symptoms and potentially leading to death.
