Sclerosing dermatitis is a skin condition often categorized as a form of acute eczema. While it can be quite painful, it is generally easy to prevent and treat. If diagnosed with sclerosing dermatitis, home remedies and medical interventions can help manage the condition effectively when necessary.
Steps
Receive a Diagnosis and Identify Symptoms

Consult a doctor for diagnosis. If you experience symptoms of sclerosing dermatitis, it is important to visit a doctor for a proper diagnosis. The doctor will outline the treatment process, which may include prevention methods, home remedies, or medication if required.

Identifying the Symptoms of Lichen Simplex Chronicus. The symptoms of this condition can vary from person to person, but there are some common signs to look for. Typical symptoms of Lichen Simplex Chronicus include:
- Itching, particularly at night.
- Red or dark brown patches on the skin.
- Small bumps that contain fluid and form scabs when scratched.
- Thick, cracked, dry, and peeling skin.
- Rough, sensitive, and swollen skin due to itching.
- The most common areas affected by Lichen Simplex Chronicus are the chest, abdomen, and buttocks. The rash may spread to other areas of the body.
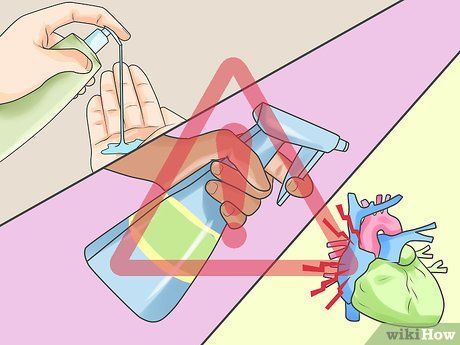
Beware of Irritants and Risk Factors. Certain irritants and risk factors can make you more susceptible to Lichen Simplex Chronicus. Being mindful of these factors can help you prevent the condition properly.
- Working in environments where you are exposed to metals like nickel, solvents, or cleaning agents can increase your risk of developing Lichen Simplex Chronicus.
- Conditions like congestive heart failure, Parkinson's disease, and HIV/AIDS also increase your vulnerability to this condition.
- Lichen Simplex Chronicus may flare up if your skin is sensitive and/or if you use harsh soaps that cause allergic reactions on the skin.
Utilizing Home Therapy

Identifying the Causes of Lichen Simplex Chronicus. This condition often flares up due to specific triggers. Identifying these triggers can help you prevent and manage the condition.
- Common triggers include allergens, food allergies, cosmetics, environmental factors, insect bites, or harsh soaps and detergents.
- If in doubt, you should minimize exposure to suspected irritants to see if symptoms improve.
- External factors that can worsen Lichen Simplex Chronicus include hot showers, stress, sweating, wearing wool clothing, exposure to smoke, and pollution.
- Some foods, including eggs, milk, peanuts, soy, fish, and wheat, may also aggravate the condition.
- Use gentle or “hypoallergenic” soaps and laundry detergents. These products contain fewer harmful chemicals that irritate the skin. Always rinse clothes with clean water after washing to ensure detergent is completely washed out.
- Products labeled “hypoallergenic” are typically tested for sensitive skin and are less likely to cause skin irritation.
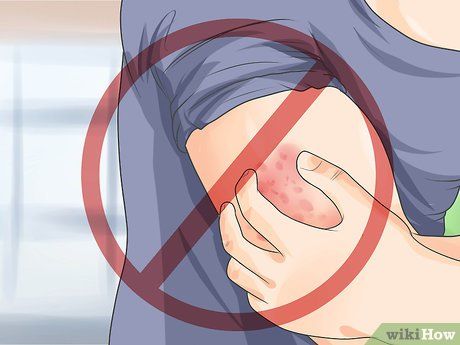
Don't Scratch. Regardless of the treatment method you choose for Lichen Simplex Chronicus, scratching is strictly prohibited. Scratching can open up pores and lead to other issues, including infections.
- If scratching is unavoidable, occasionally apply a bandage to the most affected areas. This helps reduce exposure to irritants and prevents further scratching. Do not apply bandages frequently to avoid additional irritation.

Moisturize your skin to reduce irritation. Maintaining the skin's natural moisture helps prevent dryness and reduce further irritation. You can keep your skin moisturized in various ways, such as using moisturizing lotion, avoiding excessively high temperatures, and using a humidifier.
- Use mild products designed for sensitive skin while showering. Products from Dove, Aveeno, and Cetaphil can be great options. Avoid hot water to prevent drying out and irritating your skin.
- Apply a moisturizer at least twice a day. The best time to apply it is right after a shower when your skin is still damp. In the evening, you can use oils to help lock in moisture.
- Opt for fragrance-free, color-free moisturizers to avoid irritation. If you're unsure whether a product is suitable for your skin, ask your doctor or pharmacist. Ointments tend to be thicker and more effective than lotions, and they often cause less irritation.
- Soak in warm water with added baking soda, uncooked oatmeal, or oatmeal powder for 10-15 minutes to help moisturize your skin. Afterward, apply a cream or oil to lock in moisture.
- Place a humidifier in your home to keep the air moist, preventing your skin from drying out.
- Avoid extreme heat, as it can dry out your skin.

Drink plenty of water. Staying hydrated is essential to keep your skin moisturized. Aim for at least 8 glasses of water a day to help maintain your skin's natural moisture balance and prevent dehydration.

Apply cold compresses to reduce itching and inflammation. Itching and inflammation caused by eczema result from histamine in the blood. A cold compress can help alleviate itching and inflammation by restricting blood flow and cooling the skin.
- Histamine is produced when allergens enter the body, triggering allergic reactions such as itching and inflammation.
- You can apply a cold compress to the affected area for 10-15 minutes every 2 hours, or as needed.

Protect your skin. You can prevent and alleviate symptoms of eczema by protecting your skin. Wearing clothing, bandages, and using insect repellent can all help safeguard your skin.
- Wear cool, loose-fitting clothes made from soft materials like cotton or silk to avoid scratching and excessive sweating. Avoid wool clothing as it can irritate the skin.
- Opt for long sleeves and pants to prevent scratching and protect sensitive areas from outside irritants.
- When outdoors, especially in areas where insect bites are a concern, apply insect repellent to unaffected skin areas. This step will help keep insects away and reduce the risk of allergic reactions.
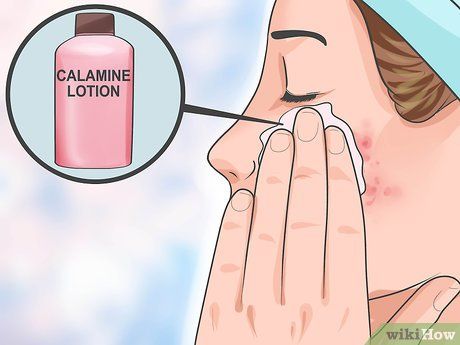
Use Calamine lotion or anti-itch cream. Over-the-counter Calamine lotion or anti-itch creams can be helpful for soothing eczema symptoms. You can find these products at stores or online pharmacies.
- Over-the-counter anti-itch creams, such as hydrocortisone, can provide relief from itching. Be sure to choose a cream containing at least 1% hydrocortisone.
- Apply the cream to affected areas before moisturizing your skin.
- Follow the product instructions for how often to apply the cream.

Take over-the-counter antihistamines to reduce inflammation and itching. These medications block histamine (the cause of allergic reactions) and help alleviate itching and skin inflammation. Various antihistamines are available without a prescription at pharmacies and online stores. Before using any medication, it’s a good idea to consult with a doctor, as it could interact with other medications or health conditions.
- Chlorpheniramine comes in 2 mg and 4 mg tablets. Adults can take 4 mg every 4-6 hours. Do not exceed 24 mg per day.
- Diphenhydramine (Benadryl) is available in 25 mg and 50 mg tablets. Adults can take 25 mg every 6 hours. Do not exceed 300 mg per day.
- Cetirizine (Zyrtec) comes in 5 mg and 10 mg tablets. Adults can take up to 10 mg every 24 hours.
- These medications have sedative effects, so avoid driving, drinking alcohol, or operating machinery while using them.
- Consult a doctor or pharmacist for the appropriate dosage if you plan to use these treatments for children.

Use over-the-counter corticosteroid creams to reduce itching and inflammation. Corticosteroid creams can help reduce inflammation, which in turn reduces itching and the urge to scratch. Apply the cream to the affected areas once daily.
- Experts recommend applying the cream in the morning after showering, so it absorbs into the skin throughout the day.
- An example of a corticosteroid cream is hydrocortisone 1%.
Seek Medical Assistance
See a doctor if the condition worsens. You should visit a doctor if blisters and rashes persist for more than a week or if the discomfort becomes unbearable. A doctor may prescribe oral medications, steroid creams, or light therapy to treat eczema.
- See a doctor immediately if: you’re unable to sleep due to discomfort, the condition interferes with your daily activities, your skin is in severe pain, home remedies aren’t effective, or you suspect an infection.

Consider light therapy. A doctor may recommend light therapy to help heal eczema. This effective treatment could involve limited exposure to natural sunlight or artificial light. However, it comes with some risks.
- Light therapy involves controlled exposure to natural sunlight or artificial UVA (ultraviolet A) and narrowband UVB rays. It may be done alone or in combination with medication.
- Sun exposure can increase the risk of premature aging and skin cancer.

Use prescription corticosteroids. If itching or rashes do not improve with over-the-counter corticosteroid creams, your doctor may prescribe stronger topical or oral corticosteroids like Prednisone.
- Oral steroids and stronger topical steroids can cause serious side effects if used long-term. Follow your doctor's instructions and avoid using the medication for longer than prescribed.
- Continue moisturizing your skin while using oral corticosteroids or topical steroids. This will help keep the skin hydrated and prevent flare-ups after stopping steroid use.

Take prescribed antibiotics to combat infection. If blisters or rashes become infected, you may need antibiotics to keep your body healthy. Always consult with your doctor if you notice signs of infection such as swelling, redness, warmth, or pus.
- Prescribed antibiotics can vary. Common antibiotics include Erythromycin, Penicillin, Dicloxacillin, Clindamycin, or Doxycycline.

Use Calcineurin inhibitors to help restore skin. You may use Calcineurin inhibitors when other treatments are ineffective. These medications, including Tacrolimus and Pimecrolimus, help maintain normal skin, control itching, and reduce flare-ups of eczema.
- Calcineurin inhibitors affect the immune system and may cause side effects like kidney issues, high blood pressure, and headaches. Rare but serious side effects include an increased risk of certain cancers.
- These medications are prescribed for patients over 2 years old and only when other treatments have failed.
