Gestational diabetes affects about 9% of pregnant women, typically developing around the 24th week of pregnancy. While most cases don't present significant symptoms, doctors may recommend screening for gestational diabetes as part of regular prenatal checkups. Glucose is a form of sugar, and the cells of women with gestational diabetes have difficulty absorbing it, causing blood sugar levels to remain high. Elevated glucose in the blood can lead to various health issues for both the mother and the baby.
Steps
Follow a diet that controls both weight and blood sugar levels

Consume the recommended daily caloric intake. Women with a normal pre-pregnancy weight should aim for around 30 calories per kg of body weight each day, based on their weight during pregnancy. Women who were obese before pregnancy may reduce their caloric intake by 33%, which would be around 25 calories per kg per day, based on their weight during pregnancy. Keep in mind that this is a general guideline. You should consult with your doctor to receive the most accurate caloric recommendations.
- Buy a food scale to weigh your food. This helps you understand portion sizes. By reading food labels, you can estimate the calorie and nutrient content in each portion.
- Track your calorie intake by keeping a food diary. You can use a small notebook to log your meals and look up the calorie content online or in guides. There are also smartphone apps, such as www.myfitnesspal.com, that make it easier to track your calories.
- Combine food journaling with regular weight checks to monitor whether you are gaining or losing weight.
- If you haven't gained enough weight, you should increase your caloric intake by 200-500 calories daily. Continue monitoring to ensure your weight gain is on track.

Monitor your carbohydrate intake. Carbohydrates are one of the three essential macronutrients, alongside protein and fat. There are three main types of carbohydrates: sugars, starches, and fibers. Sugars are the simplest form of carbohydrates and include fructose, glucose, sucrose, and others. Starches, also known as complex carbohydrates, are made up of sugar molecules linked together in chains. Fiber is a type of carbohydrate that the human body cannot break down. When you eat sugar or starch, they are broken down and converted into glucose. Glucose (a type of sugar) is converted faster than complex carbohydrates. Fiber does not convert into glucose because it is indigestible.
- There is no specific number for the required carbohydrate intake during pregnancy. Therefore, you should discuss this with your doctor. Track your carbohydrate intake along with your blood glucose levels. If your blood glucose remains high, you should reduce your intake of sugars, complex carbohydrates, and increase fiber consumption.
- There is no need to limit fiber intake. The recommended amount is 20-30g of fiber per day.
- Keep a food diary to track your carbohydrate intake. Smartphone apps can make it easier to track your carbohydrate and sugar consumption.
- Reduce your sugar consumption.

Consume starch in moderation. Even when consuming low-glycemic starches like barley, oats, and quinoa, you should still eat them in moderation. Starches are converted into glucose within cells. The general rule is to consume about one cup of starch per meal.
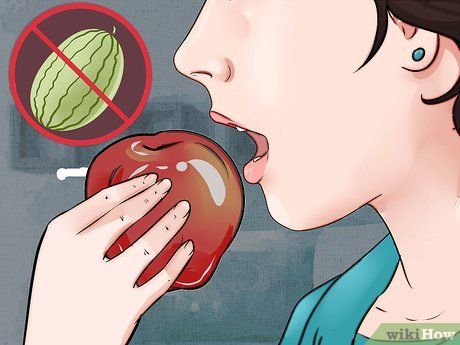
Eat fruit in moderation. Even if consuming low-glycemic fruits, you should limit yourself to 1-3 servings of fruit per day. Additionally, only consume one serving of fruit at a time.
- Avoid fruits with a high glycemic index, such as watermelon.
- Avoid canned fruit preserved in sugary syrup.
- Avoid fruit juices with added sugars.
- Pair fruits with other foods that contain healthy fats, like nuts, peanut butter, or cheese, to reduce their impact on blood sugar.

Balance your meals throughout the day. Eating too much at once can spike your blood sugar levels. It’s best to divide your intake into 3 main meals and 2-3 snacks throughout the day.
- Carry snacks such as nuts or cut vegetables for a quick bite.
- Eat a variety of nutrient-dense foods that include healthy fats and proteins, such as avocados, coconut oil, lean meats, and nuts.
Exercise to manage weight

Regular exercise. Exercising not only helps reduce blood glucose levels but also alters how cells respond to insulin. Cells become more sensitive to insulin, meaning the body doesn't need to produce excessive insulin to help cells absorb glucose. By absorbing glucose from the blood, the levels decrease. Experts recommend that pregnant women engage in 30 minutes of exercise each day.
- Consult your doctor about the most suitable type of exercise for you.
- If you haven’t exercised regularly in a while, it's important to start slowly. Begin with 10 minutes of exercise a few days a week, gradually increasing to 30 minutes daily.
- Swimming. Swimming is an excellent form of exercise for pregnant women. Moving through water reduces stress on the joints and lower back.

Increase your physical activity. You don't have to work out at the gym. Simple actions like parking further away from the supermarket or market, taking the stairs, or walking your dog regularly can be highly beneficial.

Avoid activities that pose potential risks to pregnant women. While most exercise forms are suitable for pregnant women, there are certain exercises to avoid, such as sit-ups or leg lifts that require lying on your back. It's advisable to avoid these exercises during the first trimester. Additionally, avoid or limit sports that involve high contact risks that could harm the mother or baby, such as martial arts, soccer, and basketball. It's also important to steer clear of activities that pose a high risk of falling.
Monitor your blood sugar levels

Track your blood glucose levels as recommended by your doctor. Experts suggest using a blood glucose meter to measure your blood sugar levels daily to prevent hypoglycemia. This method helps identify the ideal insulin needs. Learning how to use a glucose meter is crucial. When choosing a device, opt for one with easy-to-access test strips. Initially, you may need to check your blood sugar 3-4 times a day or even in the evening.

Understand the benefits of Insulin therapy. Managing insulin levels helps improve carbohydrate metabolism and lower blood sugar. Insulin therapy is tailored to each individual based on factors like weight, lifestyle, age, family support, and occupation. It's important to follow your doctor's instructions when administering insulin injections.

Recognize when to start Insulin therapy. If medication is needed, your doctor may recommend starting blood sugar control medications like Metformin or Glyburide. If medication alone isn’t effective, you may be advised to follow the traditional treatment of injecting intermediate-acting insulin (like NPH) in the morning and evening, and short-acting insulin during one or more meals. The injection dosage depends on your weight, how far along you are in your pregnancy, and how high your blood sugar levels are.
Empower yourself with knowledge
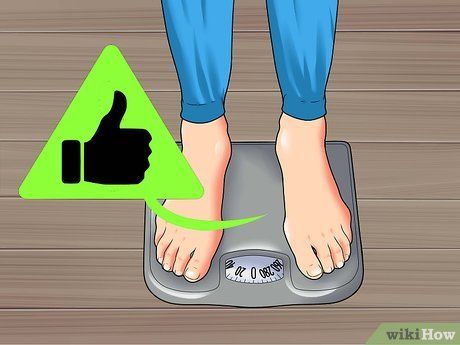
Know how much weight to gain. The National Institute of Child Health and Human Development (USA) has guidelines for the amount of weight women should gain during pregnancy, both overall and weekly, based on pre-pregnancy height and weight, and number of fetuses.
- Generally, if you are underweight, you can safely gain 16-18 kg.
- If you have a normal weight, you can safely gain 13-16 kg.
- If you are overweight, you can safely gain 10-12 kg.
- If you are obese, you can safely gain 7-9 kg.
- Women carrying multiples can safely gain 16-20 kg.

Understand the target blood sugar levels. The American Diabetes Association provides guidelines for the blood sugar levels that pregnant women with diabetes should aim for. Keep in mind that each individual’s target levels will vary, so it’s important to consult with your doctor to set personalized goals.
- Before meals, blood sugar should be at or below 95 mg/dL.
- One hour after meals, blood sugar should be at or below 140 mg/dL.
- Two hours after meals, blood sugar should be at or below 120 mg/dL.
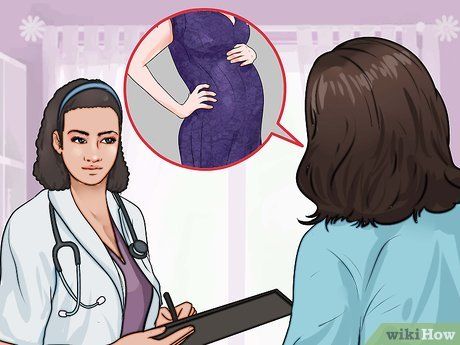
Consult with your doctor when planning pregnancy. If you are planning to become pregnant, it’s important to have a comprehensive health check, including discussing the potential risk of gestational diabetes with your doctor. Preventive measures that can reduce the risk of developing gestational diabetes include maintaining a healthy diet, staying active, and ensuring a healthy weight before pregnancy. Your doctor can assist in developing a health plan to improve your well-being as you prepare for pregnancy.

Recognize the symptoms of high blood sugar. Gestational diabetes often doesn’t cause symptoms in most pregnant women, but high blood sugar will manifest with certain signs. If your blood sugar level reaches 130 mg/dL or higher, you may experience the following symptoms:
- Increased thirst
- Headache
- Blurred vision
- Fatigue
- Frequent urination
- Seek medical attention immediately if you experience any of these symptoms or if your blood sugar reading is high.

Recognize the symptoms of low blood sugar. If you have gestational diabetes and are using insulin, and experience any of the following symptoms, you should check your blood sugar levels. If the reading is low, eat a piece of candy or drink a small amount of fruit juice. Recheck your blood sugar levels after 15 minutes.
- Excessive sweating
- Feeling weak
- Dizziness
- Trembling
- Confusion
- Pale skin
Advice
- Ensure you stay properly hydrated by drinking at least 8 glasses of water each day.
Warning
- Consult your doctor if you experience significant weight changes or insufficient weight gain.
- If gestational diabetes is left untreated, it can increase the risk of the baby growing too large, the need for a cesarean delivery, issues with the baby’s blood sugar levels, and the risk of preeclampsia.
