Animal bites are common occurrences everywhere. Children are more often bitten than adults, with dogs being the primary culprits (85–90%). The most common complication from animal bites is skin infection, though severe injuries or permanent disabilities are rare. The main concern with animal bites is rabies. Knowing how to disinfect and properly care for a dog bite wound, as well as when to seek medical help, can greatly reduce the risk of complications.
Steps
Treating Minor Bites
Inspect the bite. Dog bite wounds are usually minor and can be treated at home. If the bite results in just a scratch or a small puncture wound, home care should suffice.
- This differs from deep tissue injuries, open wounds, or crushed bones/joints. These types of injuries require medical attention, as explained in Step Two.
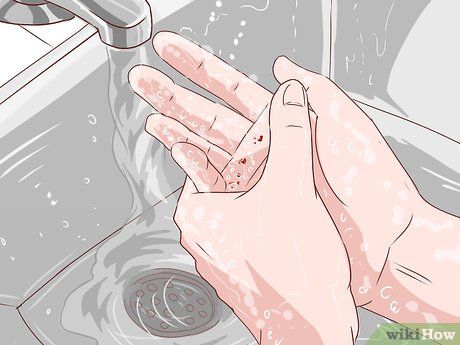
Clean the wound with soap and water. Take a few minutes to wash the bite thoroughly with soap and water at a comfortable temperature. This will help remove bacteria from the wound and the surrounding area.
- You can use any soap, but antibacterial soap is the best choice.
- Although soap and water may sting, it’s important to clean the wound thoroughly.

Apply pressure if the wound is bleeding. Use a clean cloth or gauze to apply firm pressure to the wound if it continues to bleed after cleaning. This should slow or stop the bleeding enough to bandage the wound within a few minutes.
- If the bleeding persists for over 15 minutes and you cannot bandage the wound, seek medical attention immediately.

Apply antibiotic ointment. Ointments like Neosporin or Bacitracin can help prevent infection while the wound heals. Follow the instructions on the packaging when applying the ointment to the wound.

Cover the wound with a bandage. Once you’ve applied the antibiotic ointment, properly cover the wound with a bandage. Be careful not to wrap it too tightly as it could affect blood circulation or cause discomfort.

Change the bandage when necessary. You should change the bandage whenever it gets dirty, for example, after showering. Gently clean the wound, apply the antibiotic ointment, and use a fresh bandage.

Update your tetanus vaccination status. If you’ve been bitten by a dog and the skin is broken, you may be at risk for tetanus. Medical experts recommend getting a tetanus shot if your last vaccination was more than 5 years ago.
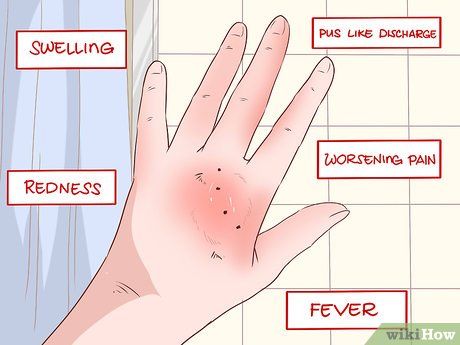
Keep an eye on the bite. Watch for signs of infection as the wound heals. If you suspect the wound is infected, see a doctor immediately. Here are some signs to watch for:
- Increased pain
- Swelling
- Redness or warmth around the wound
- Fever
- Discharge or pus
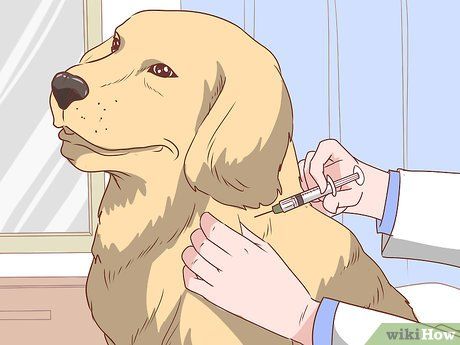
Check the dog's rabies vaccination status, if possible. A bite, even a small one, can transmit rabies. It’s important for those bitten by a dog to identify whether the dog has been vaccinated for rabies to avoid concerns later.
- If you can't determine whether the dog has been vaccinated — such as in the case of a stray dog — observe the dog for 15 days (if possible) for signs of rabies. If you can’t confirm the dog’s vaccination status, seek medical attention.

You may need medical care for other health complications. Even with a minor bite, there could be other health risks that require medical attention. Some health complications to be aware of include:
- Diabetes
- Kidney disease
- Cancer
- HIV
- Medications that weaken the immune system, such as those used for immune disorders.
Treating Severe Bites
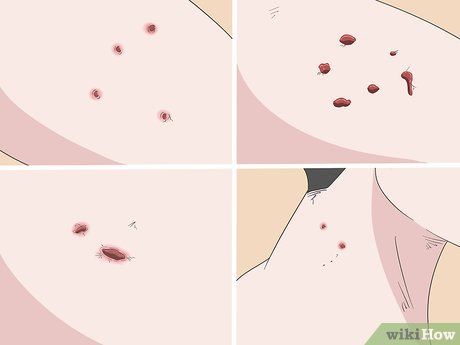
Examine the bite. A serious bite is one with deep tooth marks that can tear tissue. Depending on the force of the dog's bite, the wound may damage bones, ligaments, or joints, causing pain when moving or making it impossible to move the area around the wound. If you notice any of the following signs, seek medical help rather than treating the wound at home:
- The wound is deep, exposing fat, muscle, and bone.
- The bite has jagged teeth marks or wide gaps between them.
- The wound is bleeding heavily and won’t stop after 15 minutes.
- The wound is larger than 1-2 cm.
- The wound is on the head or neck.

Apply pressure to the wound. Before heading to the doctor, use a clean cloth to apply pressure to the wound to help stop the bleeding, if possible. Keep applying pressure until you reach the doctor.

See a doctor. A healthcare professional will determine the best course of treatment, including stopping the bleeding and suturing the wound. The doctor will clean the wound with an antiseptic like iodine and may perform a minor surgery if needed to remove dead tissue, damage, or infection that could hinder healing.
- The doctor will check your vaccination records to see if you need a tetanus shot.
- If the doctor suspects bone damage, an X-ray may be required to plan proper treatment.
- Inform the doctor whether the dog has been vaccinated for rabies. If the doctor believes you’re at risk for rabies, they will administer the vaccine.
Take prescribed antibiotics. If there’s a risk of infection, your doctor will prescribe antibiotics.
- The most common antibiotic is amoxicillin-clavulanate (Augmentin). It’s typically taken for 3-5 days in pill form. The most common side effect is digestive upset.

Change the dressings as instructed. The doctor will specify when to change the bandages after treating the wound. Typically, you will need to replace the bandage once or twice a day.
Advice
- It’s important to train your dog properly to reduce the risk of bites.
- You can find articles online on how to prevent dog bites.
Warning
- If the wound begins to itch and the surrounding skin swells, consult a doctor.
- This article only provides information on treating dog bite wounds and should not be considered medical advice. See a doctor if you are unsure about the severity of the wound.
- If the wound worsens, it’s best to consult a skilled doctor.
- If you can’t determine whether the dog has been vaccinated for rabies (whether it’s your dog or someone else’s), visit a medical center. Rabies can be treated if you go to a medical center immediately after being bitten. You cannot wait for symptoms to appear before seeking help.
- Wounds on the hands, feet, or head require more specialized medical care because the skin in these areas is thin and may affect many joints.
