Nasal congestion occurs when the tissues and blood vessels in the nose become swollen, releasing fluid (mucus). The most common symptom of congestion is a runny nose. There are several causes of nasal congestion, including bacterial or viral infections (such as a cold), dry air, allergies, medications, or asthma. It's important to visit a doctor to determine the underlying cause of the congestion. However, if the symptoms aren't severe, you can try a few simple methods to relieve the congestion.
Steps
Thin the mucus in the nose

Apply a warm towel to your nose and face several times a day. The heat helps dilate blood vessels and promotes the movement of mucus. Soak the towel in warm water, but avoid making it too hot as it could burn your skin. Wring out the excess water and place it on your face and nose. Relax for 5 to 10 minutes before removing the towel.
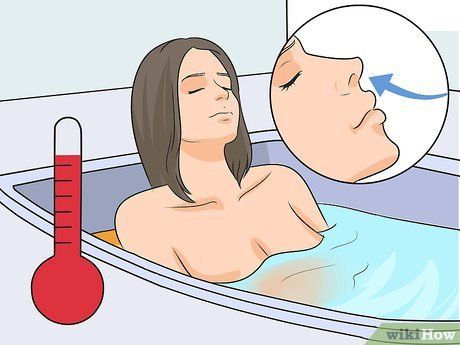
Inhale steam while taking a hot shower. This method helps to thin the mucus. You can do this by soaking in a hot bath or taking a hot shower, inhaling the steam rising from the water. Alternatively, you can sit in the bathroom while hot water runs into the tub or shower for 10 to 15 minutes. The steam will fill the room and help loosen the mucus in your nose.

Use a humidifier or vaporizer. Dry air in your bedroom or home can lead to nasal congestion. A humidifier or vaporizer works by releasing water vapor into the air, which helps alleviate dryness. You can use a humidifier at night to increase moisture levels and help thin the mucus.

Drink plenty of fluids. Drinking a lot of water helps thin the mucus and prevent sinus congestion. It’s recommended to drink eight cups of water per day to stay hydrated. You can also enjoy other beverages like fruit juices, caffeine-free coffee, and herbal teas without caffeine throughout the day.
Clear your nasal passages

Gently blow your nose. Blowing your nose too forcefully can expel germs and mucus from your nose, but the high pressure may cause them to return to your sinuses. Instead, gently blow your nose to remove the mucus. Press one nostril closed with your finger and use a tissue to gently blow the other nostril.

Sit up. Although you may feel like resting by lying down when you're unwell, this can make it harder for your sinuses to clear. Sitting up helps open your nasal passages. Additionally, this position helps drain mucus from your nose, making it easier to clear. You can prop your head up with pillows while resting or sleeping at night.

Rinse your nose with a neti pot. Pouring warm water into your nose can help clear accumulated mucus. Use a neti pot to pour a saline solution into your nostrils.
- Fill the neti pot with warm saline solution. This solution restores the body's natural fluids and tissues. Mix a small spoonful of salt into 0.5 liters of water to create the solution.
- To use the neti pot, tilt your head to one side over the sink and place the spout in the upper nostril. Breathe through your mouth and gently pour the solution into the upper nostril so the liquid flows through the lower nostril. Repeat with the other nostril.
- Clean the neti pot spout after use with boiling water to sterilize it.
Use decongestant medications

Be aware that decongestant medications and nasal sprays can have serious side effects. If you are on any medication or have a medical condition, consult a doctor before using over-the-counter nasal sprays and medications. For example, if you have an enlarged prostate, glaucoma, heart disease, high blood pressure, or thyroid conditions, consult your doctor or pharmacist before use, as these medications, including nasal sprays, could worsen these conditions. Your doctor will guide you on which medications are suitable for you. Be aware of potential side effects of decongestants, including:
- Nasal irritation, which may include nosebleeds
- Skin itching
- Headaches
- Dry mouth
- Agitation or anxiety
- Shaking or tremors
- Sleep disturbances (insomnia)
- Rapid or irregular heartbeat
- Palpitations
- High blood pressure

Consider using over-the-counter decongestants. These medications often contain phenylephrine or pseudoephedrine as the active ingredients. They work by narrowing blood vessels in the nasal passages, reducing blood flow to swollen tissues, which allows air to flow more easily.
- Phenylephrine is available in tablet, liquid (spray), or dissolvable tablet form. It is also a common ingredient in many cold and flu medications. Follow the instructions on the package.
- Pseudoephedrine is available in regular tablets, 12-hour extended-release tablets, 24-hour extended-release tablets, and oral liquid form. Follow the instructions on the packaging.

Use nasal sprays. Nasal sprays help relieve nasal congestion by shrinking blood vessels in the nose and reducing swelling. You can visit your doctor to get a prescription or purchase an over-the-counter nasal spray from the pharmacy. To use a nasal spray:
- Gently blow your nose to clear any mucus before applying the spray.
- Shake the spray bottle before use.
- Lift your head up and exhale gently. (Tilting your head back may cause the medication to be absorbed more, leading to potential side effects.)
- Use your other finger to close the opposite nostril.
- Place the nozzle of the spray in your nostril and press down while breathing in gently through your nose. Repeat on the other nostril.
- Avoid sneezing or blowing your nose right after using the spray.

Limit the use of nasal sprays. Do not use nasal sprays for more than three consecutive days. Using them longer can cause your nasal congestion to return.
- If congestion persists for more than three days, you should use the nasal spray for the first three days, and then switch to oral decongestants. Do not use both treatments simultaneously, as this could increase the risk of side effects.
Seek medical assistance
Provide your doctor with a full list of symptoms. Your doctor needs to know your current symptoms and any previous medical conditions, along with other related symptoms such as fever, headaches, coughing, shortness of breath, etc.
- During the examination, the doctor will use a penlight to check the inside of your nose and ears for any accumulated fluids, palpate your cheekbones and/or forehead to check for weakened sinus pressure, and feel the swollen lymph nodes around your neck.
- The doctor may recommend a blood test to check your white blood cell (WBC) count. If elevated, it could indicate an infection or inflammation, such as an allergy.
- If necessary, the doctor may refer you to an ENT (Ear, Nose, and Throat) specialist for further tests or examination.

Consult your doctor about prescription medications. Most nasal decongestants are available over-the-counter without a prescription. Depending on the cause of your congestion, you might need a different type of medication. For instance, sinus infections require antibiotics to fight bacteria, while conditions like asthma or other serious disorders may require steroids.

Call a doctor if you experience severe symptoms. In some cases, nasal congestion can become severe or be accompanied by other dangerous symptoms. Contact your doctor immediately if you notice any of the following signs:
- Nasal congestion lasting longer than ten days.
- High fever and/or fever lasting more than three days.
- Greenish nasal discharge along with sinus pain (pain around the cheekbones or forehead) or fever. This could indicate a bacterial infection.
- If you have asthma, emphysema, or are using medications that suppress the immune system, such as steroids. These conditions may increase the risk of infection.
- Blood or clear fluid continuously draining from your nose after a head injury. Clear fluid or blood could be a sign of a head injury involving the brain.
Advice
- Ensure you get plenty of rest and take good care of yourself when you're sick.
- See a doctor if your condition does not improve, or if it improves but then worsens. You may need medication to fully recover.
