Scalds from boiling water are among the most common household accidents. Hot beverages, bathwater, or boiling water on the stove can easily splash onto the skin and cause burns. Anyone can experience a boiling water scald at any time. Knowing how to assess the situation and determine the severity of the burn will help you treat it promptly.
Steps
Assess the Situation

Look for signs of a first-degree burn. After being splashed with boiling water, you need to identify the type of burn. Burns are categorized by degrees, with higher degrees indicating more severe burns. A first-degree burn affects the outer layer of the skin. Symptoms include:
- Damage to the top layer of skin
- Dry, red, and painful skin
- Skin that turns pale or white when pressed
- First-degree burns typically heal within 3-6 days and do not leave scars

Identify second-degree burns. If the water is hotter or the skin is exposed to hot water for a longer duration, you may suffer from second-degree burns. These are considered partial-thickness burns, with symptoms including:
- Damage to two layers of skin but only a slight burn in the second layer
- Red and oozing burns
- Blisters
- White or pale skin at the burn site when pressed
- Pain upon light touch and changes in skin temperature
- Second-degree burns typically heal within 1-3 weeks and may leave scars or cause skin discoloration (lighter or darker than the surrounding skin)
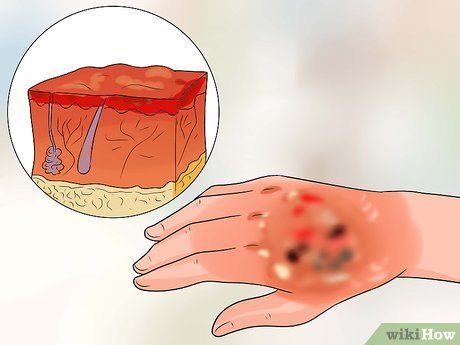
Recognize third-degree burns. Third-degree burns occur when the water is extremely hot or the skin is exposed to hot water for an excessively long time. These are considered full-thickness burns, with symptoms such as:
- Damage to two layers of skin and deeper, but not completely through the second layer
- Pain at the burn site when pressed firmly (may not hurt immediately due to nerve death or damage)
- Skin does not turn white when pressed
- Blisters form at the burn site
- Black, charred scabs or peeling skin
- Third-degree burns require hospitalization and surgical or medical treatment for recovery, especially if they cover more than 5% of the body.

Observe signs of fourth-degree burns. Fourth-degree burns are the most severe cases. These are critical injuries requiring immediate medical attention. Symptoms include:
- Complete damage through both layers of skin, often affecting fat and underlying muscles. In third and fourth-degree burns, bones may also be affected.
- No pain
- Discolored skin at the burn site—white, gray, or black
- Dryness at the burn site
- Surgery and hospitalization are required for treatment and recovery

Observe large (extensive) burns. Regardless of the degree, burns can be considered large if they occur around joints or cover a significant portion of the body. If complications accompany burn symptoms or normal activities are hindered due to the burn, it may be classified as a large burn.
- Burns on one arm/leg equate to 10% of an adult's body; 20% equates to the torso. Extensive burns cover more than 20% of the total body surface.
- Burns covering 5% of the body (e.g., elbow, half a leg) with deep burns (e.g., third or fourth-degree) are considered large burns.
- Treatment for large burns is similar to third or fourth-degree burns, requiring immediate emergency care.
Treat Minor Burns

Identify situations requiring medical attention. Even minor burns (first or second-degree) need medical care if they meet certain criteria. Burns encircling the entire tissue around one or more fingers require immediate medical attention. Such burns can impede blood circulation to the fingers and, in severe cases, may lead to amputation if untreated.
- Additionally, seek medical care for minor burns on the face or neck, extensive burns on the hands, groin, legs, feet, buttocks, or over joints.

Clean the burn. Minor burns can be treated at home. The first step is to clean the burn by removing clothing covering it and soaking the affected area in cool water. Avoid using cold running water, as it can damage the skin and increase the risk of scarring or complications. Do not use hot water to avoid irritating the burn.
- Gently wash the burn with mild soap.
- Avoid using harsh products like hydrogen peroxide, as they can hinder the healing process.
- If clothing sticks to the skin, do not attempt to remove it. The burn may be more severe than it appears, and emergency care is needed. Cut away the clothing (except the part stuck to the burn) and apply a cold compress or ice pack for about 2 minutes.

Cool the burn. After cleaning, soak the burn in cool water for 15-20 minutes. Avoid using ice or running water directly on the burn to prevent further skin damage. Next, dip a clean cloth in cool water and gently place it over the burn (do not rub or scrub). Simply lay the cloth on the burn.
- You can soak the cloth in tap water and refrigerate it to make it cooler.
- Do not apply butter to the burn. Butter does not cool the burn and can cause infection.

Prevent infection. To prevent infection, care for the burn after cooling it. Use clean hands or a cotton ball to apply antibiotic ointment like Neosporin or Bacitracin. If the burn is an open wound, use non-stick gauze instead of cotton balls, as fibers can stick to the burn. Then, cover the burn with a non-stick bandage (e.g., Telfa). Change the bandage every 1-2 days and reapply the ointment.
- Do not pop blisters that form on the burn.
- Avoid scratching as new skin forms to prevent infection. Burned skin is highly susceptible to infection.
- You can apply soothing ointments like aloe vera, cocoa butter, or mineral oil to relieve itching.

Manage pain. Any minor burn can cause discomfort. After covering the burn, elevate the affected area above the heart to reduce swelling and pain. For persistent pain, take over-the-counter pain relievers like Acetaminophen (Tylenol) or Ibuprofen (Advil and Motrin). Take the medication multiple times a day as needed, following the instructions on the packaging.
- The recommended dose for Acetaminophen is 650 mg every 4-6 hours, up to 3250 mg per day.
- The recommended dose for Ibuprofen is 400-800 mg every 6 hours, up to 3200 mg per day.
- Always read the recommended dosage on the packaging, as it may vary depending on the type and brand of medication.
Treating Severe Burns

Call for emergency help. If you suspect a severe burn (third or fourth-degree), seek immediate assistance. Severe burns should not be treated at home and require professional care. Call emergency services if:
- The burn is deep and severe
- The burn is above first-degree and the person has not had a tetanus shot in over 5 years
- The burn is larger than 7.5 cm or encircles any part of the body
- There are signs of infection, such as redness, intense pain, oozing, or fever
- The burn occurs in someone under 5 or over 70 years old
- The burn affects someone with a weakened immune system (e.g., HIV patients, those on immunosuppressants, diabetics, or individuals with liver disease)

Care for the victim. After calling for help, monitor the burn victim's condition. If the victim is unresponsive or in shock, inform emergency responders so they can prepare accordingly.
- If the victim is not breathing, perform chest compressions while waiting for emergency services.

Remove tight clothing. While waiting for help, remove tight clothing and jewelry near the burn. However, leave any clothing or jewelry stuck to the burn intact, as removing it could tear the skin and cause further damage.
- Apply cold compresses around metal jewelry like rings or hard-to-remove items like bracelets, as metal can conduct heat to the burn.
- You can cut and loosen clothing stuck around the burn.
- Keep the victim warm, as severe burns can lead to shock.
- Unlike minor burns, do not soak large burns in water to avoid hypothermia. If the burn is on a movable area, elevate it above the heart to reduce swelling.
- Avoid giving painkillers, popping blisters, scrubbing dead skin, or applying ointments, as these actions can interfere with professional treatment.

Cover the burn. After removing or cutting away clothing near the burn, use a clean, non-stick bandage to cover the burn and prevent infection. Avoid using materials that could stick to the burn. Opt for non-stick gauze or wet bandages.
- If you suspect the bandage might stick due to the severity of the burn, do nothing and wait for emergency services.
Warnings
- A burn that appears severe but is painless may be worse than you think. Cool the burn immediately and seek emergency care if you suspect a serious burn. Many people mistakenly believe third-degree burns are not dangerous initially due to the pain-blocking mechanism. Failing to cool the burn or delaying treatment can lead to deeper damage, complications in recovery, and a higher risk of scarring.
