Candida infection is caused by the Candida albicans fungus and can affect areas such as the mouth, vagina, skin, stomach, and urinary tract. Most women will experience a vaginal yeast infection at least once in their lifetime, and nearly all individuals with HIV/AIDS will suffer from Candida infections. Oral yeast infections (thrush) are commonly seen in newborns, elderly individuals, and those with weakened immune systems.
Steps
Traditional Medication
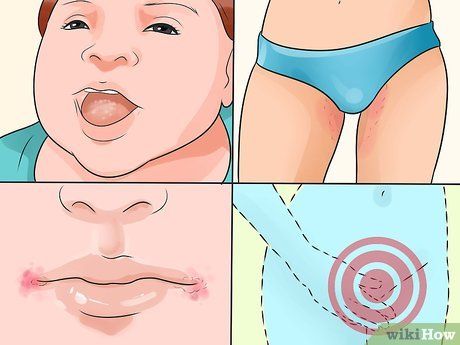
Identify the symptoms. The risk of yeast infections increases if you are taking antibiotics, pregnant, overweight, diabetic, or have a weakened immune system. Common symptoms of a yeast infection include:
- Itching, irritation, pain, and a burning sensation in the vaginal area
- White, chunky discharge with an odor
- Rashes, patches, and blisters in the groin area
Consult a doctor. It is advisable to see a doctor if you suspect a yeast infection, experience first-time symptoms of yeast infection, or notice any other unusual symptoms. The doctor may take samples for testing, such as a vaginal swab, CT scan, or stool examination if the infection is widespread. If you have recurrent yeast infections, the doctor may test for immune deficiencies or other underlying conditions. You may be dealing with a more complex yeast infection if:
- There are severe symptoms like redness, swelling, intense itching, leading to tears, cracks, or ulcers on the skin.
- Yeast infections recur more than four times a year.
- The infection is caused by a yeast other than Candida albicans.
- You are pregnant.
- You have diabetes.
- You are taking certain medications, such as those for HIV.
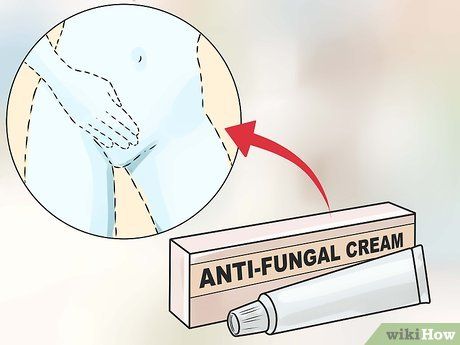
Use antifungal cream. A doctor may prescribe an antifungal medication to treat the infection or recommend over-the-counter options. Since yeast infections are caused by fungi, over-the-counter antifungal creams are a common treatment method.
- Consult your doctor if symptoms do not improve after 3-4 days of using the medication.
- Do not use over-the-counter medications for pregnant women or in cases of recurrent yeast infections. In these cases, a visit to the doctor is necessary for proper treatment.
- Ensure that you are using a cream specifically designed for treating yeast infections, as other antifungal creams may not be suitable for vaginal use.
- Over-the-counter creams are typically applied for 1-7 days. Follow the instructions on the packaging regarding the frequency of use.
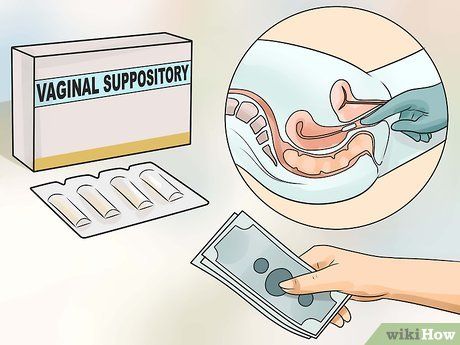
Use vaginal suppositories. Like antifungal creams, over-the-counter vaginal suppositories treat yeast infections by directly targeting the causative fungi. The active ingredients may vary but typically include antifungal agents such as Clotrimazole, Butoconazole, Miconazole, or Tioconazole.
- Vaginal suppositories can also be used for 1-7 days. Be sure to read the instructions carefully for usage frequency and proper insertion techniques.
- These suppositories typically come in cone, stick, or wedge shapes and are inserted directly into the vagina.

Take over-the-counter oral medications. Oral antifungal tablets can also be used, though they are less common than topical treatments and less effective for severe yeast infections. It is advisable to consult a doctor before taking new medications, as some drugs may interact with other medications, herbs, or supplements, causing side effects.
- Carefully read the label for the correct dosage and frequency of intake. Oral treatment usually lasts 1-7 days.
- These tablets contain antifungal ingredients that are safe for oral consumption.
- Avoid overusing antibiotics as they can destroy beneficial bacteria that help control Candida yeast.
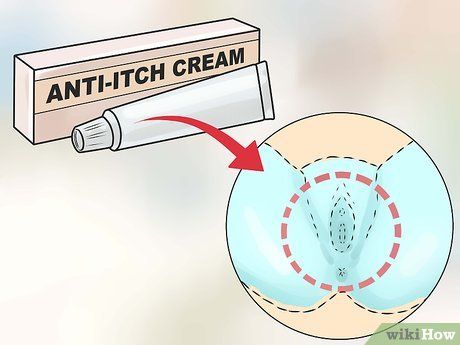
Apply anti-itch cream. Anti-itch creams should only be applied around the vaginal area, not inside. Vaginal creams may be combined with mild corticosteroids to relieve inflammation and itching, and they are often sold with an applicator to measure the correct amount of cream.
- Consult a doctor before using over-the-counter anti-itch creams.
- These creams are thicker than lotions but may still run, so consider using a sanitary pad or panty liner. Avoid using tampons as they may absorb the cream and reduce its effectiveness.
- Anti-itch creams do not cure yeast infections but can provide relief from itching, irritation, and general discomfort caused by the infection. They should be used alongside antifungal treatments, vaginal suppositories, or oral medications.
- Only use anti-itch creams that are specifically designed for vaginal use. Other anti-itch creams may disrupt the vaginal pH balance, potentially worsening the yeast infection.
Change your diet

Avoid certain foods and beverages. A restrictive diet can help reduce the presence of yeast-causing bacteria. Experts recommend avoiding alcoholic drinks, sweets, beverages containing artificial sweeteners, refined carbohydrates, and foods rich in yeast.
- Some dairy products, including cheese and butter, may contribute to yeast infections, though more research is needed.
- If blood sugar levels are low or you're unsure which foods to avoid, consult with your doctor or a nutritionist to create an appropriate diet plan.

Take Vitamin C supplements. Vitamin C, or ascorbic acid, is a powerful antioxidant that plays a crucial role in supporting immune function. It is recommended to take 500-1000 mg per day, divided into 2-3 doses. Alternatively, you can increase your intake of vitamin C-rich foods. However, always check with your doctor before taking vitamin C supplements, especially if you're on immune-suppressing medications or have a weakened immune system. On the other hand, natural sources of vitamin C are safe and include:
- Red or green bell peppers
- Citrus fruits like oranges, grapefruits, lemons, or non-concentrated citrus juice
- Spinach, broccoli, and Brussels sprouts
- Strawberries and raspberries
- Tomatoes
- Mangoes, papayas, and cantaloupes

Boost your Vitamin E intake. Vitamin E is an antioxidant that strengthens the immune system and is particularly effective against yeast infections caused by a weakened immune system. The recommended daily dose for adults is 15 mg. Foods rich in vitamin E include:
- Vegetable oils
- Almonds
- Peanuts
- Hazelnuts
- Sunflower seeds
- Spinach
- Broccoli

Eat foods rich in omega-3 fatty acids. Essential fatty acids help reduce inflammation and the burning sensation associated with yeast infections. Experts recommend a combination of omega-6 (found in evening primrose oil) and omega-3 (found in fish oil or flaxseed oil). The recommended dosage is 2 teaspoons of oil daily or 1000-15000 mg, divided into two doses. Foods rich in omega-3 include:
- Eggs
- Pinto beans, soybeans, and black-eyed peas
- Tofu
- Wild-caught salmon and sardines
- Walnuts, almonds, chia seeds, and flaxseeds
- Canola oil, fish oil, and flaxseed oil

Supplementing with probiotics can promote better health. Probiotics are beneficial bacteria commonly found in the gut and stomach lining that help control Candida yeast while boosting the immune system. Some studies suggest that yogurt with live probiotics can prevent yeast infections. To enhance probiotic intake, you can:
- Try probiotic supplements with a concentration of 1-10 billion Bifidobacterium, up to twice a day.
- Consult a doctor before taking probiotics if you're on immunosuppressive drugs or antibiotics.
- Consume 250 ml of unsweetened plain yogurt daily to help prevent yeast infections.
- Consider vaginal probiotic suppositories to restore bacterial balance in the vagina.
Using natural ingredients at home can help manage your health. Many people turn to everyday home remedies to enhance wellness and prevent infections. Natural substances often provide effective solutions for various issues, including yeast infections.

Garlic is well-known for its antibacterial and antifungal properties due to the natural compound allicin. It's recommended to consume 1 raw garlic clove daily or add 2-3 crushed cloves to your meals. For supplements, you can take the equivalent of 1 garlic clove daily or 4000-5000 mg of allicin.
- Garlic can interact with certain medications, including HIV treatments. It may also increase bleeding risk for those with weakened immune systems or those on blood-thinning drugs. Always consult your doctor before using garlic or garlic supplements.

Echinacea extract is a herb known for its antiviral and antioxidant properties that boost immune function, reduce inflammation, and balance hormones. It's especially effective when used alongside Econazole, an antifungal medication for yeast infections. Studies suggest that 2-9 ml of Echinacea extract or one cup of Echinacea tea daily can help manage yeast infections caused by Candida.
- To make tea, steep 1-2 g of dried Echinacea root or extract in warm water for about 5 minutes. Strain and drink.
- As Echinacea can interact with various medications, consult your doctor before use.
- Possible side effects include stomach pain, nausea, dizziness, and dry eyes. Do not take Echinacea on an empty stomach.
- Avoid Echinacea if you have conditions like multiple sclerosis, tuberculosis, connective tissue disorders, leukemia, diabetes, HIV/AIDS, autoimmune diseases, or liver disorders.

Try using tea tree oil for a soothing bath. Tea tree oil is well-known for its antiviral and antifungal properties. Research suggests that tea tree oil can be effective in treating vaginal yeast infections. However, avoid applying the essential oil directly to the vagina. Instead, try a relaxing tea tree oil bath.
- Add 10-15 drops of tea tree oil to a warm bath and soak for about 15 minutes. Repeat this process 2-3 times a week to help manage and prevent recurrent vaginal yeast infections.
Preventing yeast infections is key to maintaining vaginal health. By keeping the area clean and dry, you can avoid recurrent infections. Some hygiene tips include: avoid using soap on the vaginal area and simply rinse with warm water; always wipe from front to back after using the restroom; steer clear of feminine products like sprays, powders, or perfumes for the vaginal area; change pads, tampons, or menstrual cups every 2-4 hours.
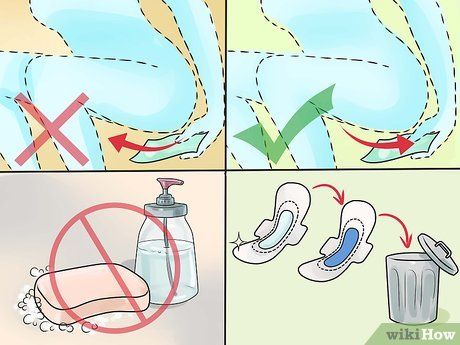
Personal hygiene plays an important role in preventing yeast infections. To avoid recurrence and future infections, keep the vaginal area dry and clean. Here are some helpful hygiene practices: do not use soap in the vaginal area—just rinse with warm water; always wipe from front to back after using the bathroom; avoid products like feminine sprays, deodorants, and powders; and change sanitary pads, menstrual cups, and tampons every 2-4 hours.

Wear comfortable clothing to help prevent yeast infections. Avoid tight clothing, such as leggings, skinny jeans, or pantyhose, which can irritate the skin and worsen infection symptoms. Also, refrain from wearing damp or sweaty workout clothes for long periods. Wash sweat-soaked clothes after each use. Additionally, choose cotton underwear or pantyhose instead of silk or nylon, as these materials can increase moisture and irritation in the vaginal area.

Avoid douching, as it may worsen yeast infections. While some people believe douching helps clean the vagina, it actually disrupts the natural pH balance, irritates the skin and mucous membranes, and increases the risk of vaginal infections, pelvic inflammatory disease, and complications during pregnancy. Whether using herbal or medicinal products, douching is not recommended.
