Numerous everyday microbes occasionally grab headlines in local and national news. These often include organisms responsible for illnesses like food poisoning, fever, and pneumonia. Yet, these common pathogens, typically living harmlessly on our bodies, can suddenly turn hostile, consuming our flesh! This can range from destroying surrounding tissues to literally devouring flesh and brain matter.
10. Streptococcus Pyogenes
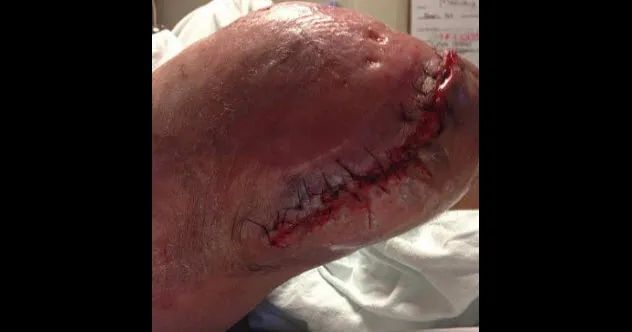
Streptococcus pyogenes, commonly referred to as group A streptococcus (GAS), is a natural inhabitant of the human body. Typically, it lives harmlessly on our skin and other body parts. However, being naturally pathogenic, it can occasionally lead to illnesses like strep throat and scarlet fever.
In more serious instances, this bacterium can consume flesh, a condition known as necrotizing fasciitis. In 1999, the CDC documented 600 cases of necrotizing fasciitis caused by S. pyogenes. The bacterium produces toxins and enzymes that directly destroy nearby body cells.
Without treatment, it can devour significant portions of the body and result in death. Alarmingly, a new strain of S. pyogenes, known as emm89, is emerging as a powerful cause of necrotizing fasciitis.
It’s crucial to understand that flesh-eating disease primarily affects individuals with weakened immune systems, such as diabetics.
9. Apophysomyces
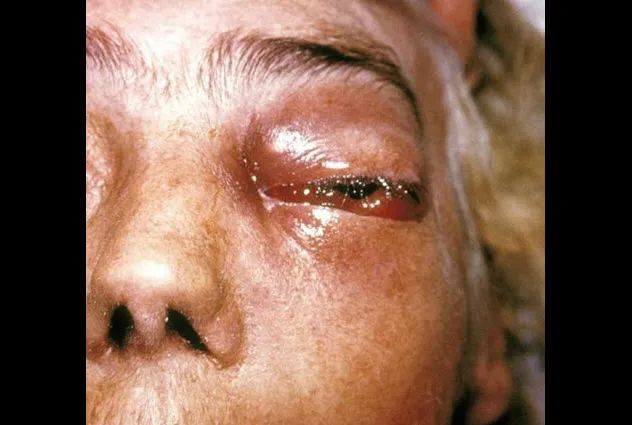
Soil is home to countless microorganisms, including a fungus known as Apophysomyces. While infections from this fungus are rare, it can lead to a flesh-eating condition called mucormycosis.
Mucormycosis isn’t exclusive to Apophysomyces. Other fungi in the Mucorales order, such as Mucor and Rhizopus, can also trigger it. For the infection to occur, the fungus must penetrate deep into the tissue.
A tragic example of this disease occurred after a tornado struck Joplin, Missouri, in 2011. Thirteen survivors of the disaster were later infected by the fungus. As it grew, the fungus invaded surrounding tissues with its mycelia, damaging blood vessels and cutting off blood supply.
Deprived of blood and essential nutrients, the tissue started to necrotize. Researchers found that the tornado’s force had driven the fungus from the soil deep into the victims’ wounds, marking an exceptionally rare and unfortunate event.
8. Leishmania
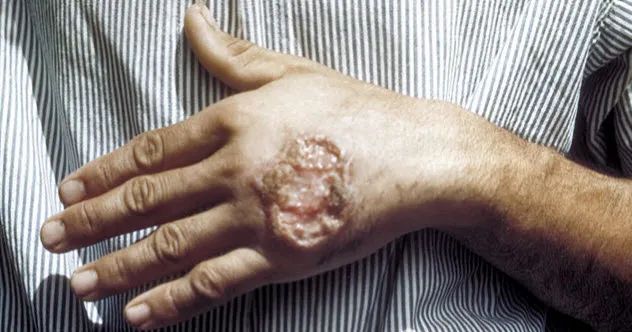
Even a typical fly bite can escalate into a flesh-eating condition under specific conditions. Leishmania, a parasite prevalent in tropical and subtropical regions, including parts of southern Europe, requires both a human and a sand fly host to complete its life cycle.
Once Leishmania has developed inside a sand fly, it is transmitted to humans through a bite. The parasite continues to mature within the human body, infiltrating nearby cells. These infected cells eventually burst and perish after housing the parasite.
Flesh destruction typically occurs around the bite site and can expand considerably without treatment. In rare cases, the parasite can spread systemically, moving to other body parts and causing damage there as well.
Leishmaniasis comes in two forms: cutaneous and visceral. The cutaneous type results in raw, ulcerated skin, while the visceral type targets internal organs. Currently, war-ravaged Syria is facing an outbreak of leishmaniasis. Travelers to regions like the Amazon and Africa are also at risk of contracting this infection.
7. Aeromonas Hydrophila
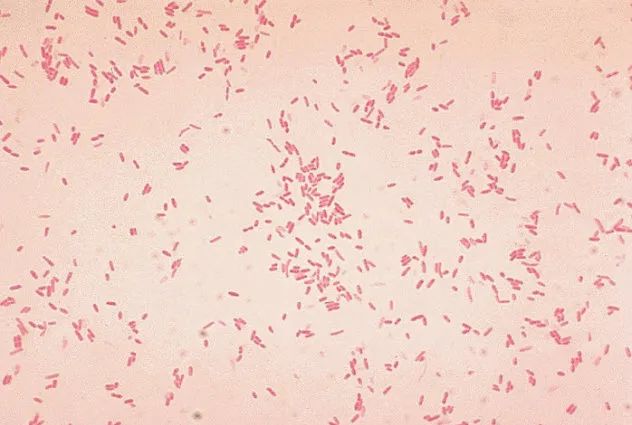
Aeromonas hydrophila is frequently found in freshwater and brackish environments like estuaries. It can also pollute drinking water if purification systems fail or are inadequate. Travelers often contract this bacterium, leading to symptoms like diarrhea, commonly known as traveler’s diarrhea.
The bacterium can also taint food products if the water used for cleaning facilities or produce is contaminated. Since Aeromonas hydrophila thrives in cold temperatures, refrigerating contaminated foods may not remove the bacteria, potentially harming those who consume them later.
Although rare, this bacterium can cause flesh-eating disease when open wounds come into contact with contaminated water, as seen in a 2012 case involving a Georgia woman. The bacteria entered her body through a wound sustained during a zip line accident.
Common treatments to halt the disease’s progression include amputation and the removal of affected internal organs. Therefore, avoid exposing open wounds to water.
6. Bacteroides Fragilis
Bacteroides fragilis flourishes in the oxygen-poor environment of the human gut, particularly in the colon. As a natural inhabitant, it plays a role in digestion and helps protect against harmful microbes by outcompeting them for space and nutrients. Its adaptation to the gut environment gives it an advantage over invading pathogens.
Ironically, when this typically beneficial bacterium escapes the gut, often due to surgery or trauma, it can trigger severe necrotizing (flesh-eating) infections. These infections are marked by excessive pus and swelling in the affected tissues.
Treating a B. fragilis infection can be somewhat challenging. The bacterium produces enzymes that degrade penicillins and related antibiotics, rendering them ineffective. Often, stronger antibiotics like carbapenems are required. However, overuse of these advanced antibiotics can contribute to rising antibiotic resistance.
5. Clostridium Perfringes
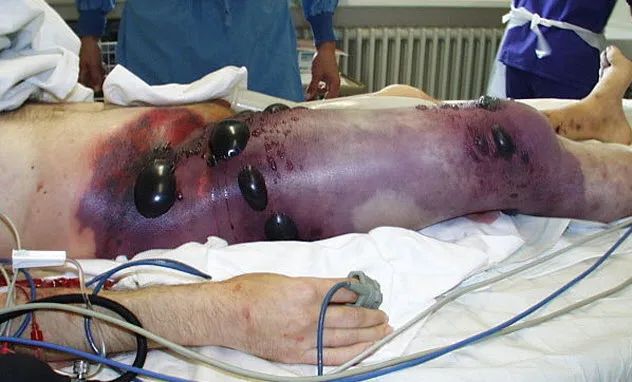
Clostridium perfringes, related to the Clostridium botulinum bacterium responsible for botulism, is another prevalent pathogenic species within the Clostridium genus. It is frequently found in soil, the human gut, and raw meat and poultry products.
Consuming these products raw can lead to food poisoning caused by the bacterium. In severe cases, C. perfringes can trigger necrotizing fasciitis, similar to pathogens like Streptococcus pyogenes, Aeromonas hydrophila, and Bacteroides fragilis.
Clostridium perfringes can devour skin surfaces or deeper muscle tissues, often necessitating amputation. Additionally, it can cause gas gangrene, a severe condition.
Gas gangrene is a critical infection that affects muscles rather than just the skin. It is marked by gas formation in dying muscle tissues. Infections typically occur when wounds are exposed to contaminated soil.
This is particularly common in battlefield settings, where open wounds are exposed to dirt. Treatment often involves skin grafting or amputation.
4. Klebsiella Pneumoniae
Klebsiella pneumoniae is a natural inhabitant of the human body, typically found in the gut and nasopharynx regions. Known for its high antibiotic resistance, this bacterium is linked to various illnesses, including pneumonia, bloodstream infections, and meningitis. Infections often occur in hospitals, where the bacterium thrives in catheters and respiratory equipment.
In rare instances, Klebsiella pneumoniae can cause flesh-eating disease. The first North American case was reported in the Western Journal of Emerging Diseases, involving an elderly Filipino woman in California who suffered from muscle necrosis due to K. pneumoniae. Such cases are more common in southern Asia, where the bacterium is widespread.
Treating Klebsiella pneumoniae infections is particularly challenging due to its resistance to a broad range of antibiotics. Notably, it is resistant to all penicillins and shows growing resistance to newer generations of drugs as well.
3. Naegleria Fowleri

Before diving into freshwater environments, consider covering your nose as a precaution. Found in lakes, rivers, and similar settings, Naegleria fowleri is an amoeba that consumes brain tissue.
Once it enters the nose, the amoeba travels along the olfactory nerves to the brain, where it begins feeding. While it typically consumes bacteria, the lack of such food in the brain forces Naegleria fowleri to feed on brain matter instead.
Although natural freshwater sources are common habitats for this amoeba, contaminated pools or tap water can also contain it. Importantly, infection occurs only when contaminated water enters the nose, not through ingestion or other body openings.
Infections from Naegleria fowleri are rare but almost always fatal. No standard drug treatment exists, and surgery is often a last resort. To prevent infection, avoid untreated or warm freshwater sources. Properly chlorinated pools and tap water are generally safe.
2. Staphylococcus Aureus

Staphylococcus aureus, commonly known as Staph, is a frequent pathogen that can temporarily reside on human skin and other body parts. The CDC estimates that 30% of the global population carries this bacterium in their nasal area, though it often remains nonpathogenic.
Staph is linked to bloodstream infections and heart valve infections (endocarditis) when it enters the bloodstream through open wounds or surgeries. If ingested, it can cause food poisoning by releasing toxins. While cooking kills the bacterium, the toxins remain active.
In severe cases, Staphylococcus aureus can lead to necrotizing fasciitis, particularly in patients with conditions like diabetes and hypertension. With weakened immune systems, the bacterium can invade and destroy body tissues. Treatment is challenging, especially when infections are caused by methicillin-resistant Staphylococcus aureus (MRSA), which resists many antibiotics.
1. Vibrio Vulnificus

Vibrio species typically thrive in marine environments, as they need salty water to grow. This genus includes Vibrio cholerae, known for causing cholera, and Vibrio vulnificus.
Vibrio vulnificus is often contracted through seafood like crabs, leading to diarrhea and vomiting when ingested. In rare cases, susceptible individuals may develop liver disease. Exposure of open wounds to seawater contaminated with V. vulnificus can result in necrotizing infections.
Necrotizing infections from V. vulnificus are prevalent in coastal areas, such as US states along the Gulf of Mexico. In 2015, multiple cases of flesh-eating disease caused by this bacterium were reported. Florida alone records up to nine deaths annually due to V. vulnificus.
Infections peak between May and October. To avoid necrotizing fasciitis from Vibrio vulnificus, it’s crucial to protect open wounds from saltwater exposure, particularly during warmer months when the bacterium thrives.
