We have just left the Season of Giving, a globally recognized time of goodwill. While many of us search haphazardly for the perfect gift for friends or loved ones, thousands of people worldwide are praying for their loved ones to receive the 'Gift of Life.' Thanks to advancements in modern science and medical technology, what once were considered deadly conditions can now be cured through the generous donation of organs and tissues. With a donor's selfless contribution, an individual's quality of life can be enhanced, and those suffering can recover. This list presents 10 important aspects of donation, shared in no particular order.
10. Blood Donations
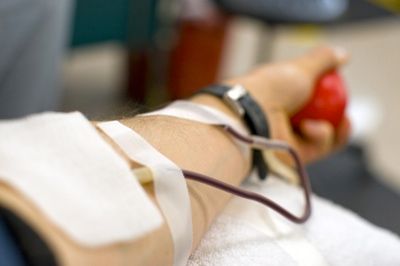
As of now, no suitable, long-term synthetic replacement exists for whole human blood, which makes donating whole blood or platelets (apheresis) absolutely vital. When administered in the right environment, the procedure is quick, usually taking only about 10 minutes. However, because pre-screening of each donor is required, the entire process typically lasts about an hour. In the United States, blood products are given daily, averaging 38,000 units, with the demand projected to rise by around 6% annually. The need for blood becomes even greater in times of war or disaster. Blood has a limited shelf life, with different components (whole blood, red blood cells, platelets, and plasma) lasting anywhere from 5 days to over a year, depending on the type.
Interesting note: Blood collected in the U.S. from paid donors cannot legally be used for transfusions. If you've been compensated for donating blood, it was likely utilized by the pharmaceutical industry for the creation of medications.
9. Consent vs. Dissent

No one can benefit from the Gift of Life unless proper permissions and legal releases are provided. These legal requirements vary from country to country. In the U.S., it is common for an individual to confirm their consent to organ donation, often through a 'DONOR' sticker on the back of their driver's license or by creating a 'living will.' In essence, people must actively state their wish to donate. On the other hand, the practice in many countries, including Spain, follows a 'dissent' model, which means individuals are assumed to be organ donors unless they have explicitly declined during their lifetime. This model is thought to contribute to Spain’s high donation rate—34 donors per million population. The U.S. sits at the median with 26 donors per million, while Austria has a significantly lower rate at 10 donors per million.
8. The Big Six
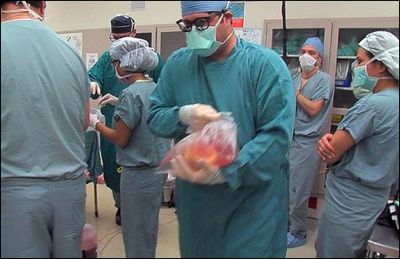
The kidneys, heart, liver, pancreas, lungs, and intestines are the main organs most people consider when talking about organ donation. These are the organs with the highest demand on waiting lists globally. These organs must be transplanted within hours as there’s no way to store them for later use. However, tissue donation works differently. According to OrganDonor.gov, 'Corneas, the middle ear, skin, heart valves, bone, veins, cartilage, tendons, and ligaments can be preserved in tissue banks and used to restore sight, heal burns, repair heart valves, replace veins, and repair damaged connective tissue and cartilage in recipients.' With proper planning, one person’s death can help more than 50 others regain their health.
7. Stem Cells

Stem cells are two simple words, yet together they spark significant controversy. Much of the current medical research is focused on these fundamental building blocks of life and their vast potential in medical treatments. Researchers anticipate stem cells will play a crucial role in the future treatment of conditions such as stroke, diabetes, spinal cord injuries, blindness, deafness, Parkinson’s disease, Alzheimer’s disease, arthritis, and cancer. Contrary to common belief, stem cells are not primarily harvested from fetal tissue but from alternative sources like blood from umbilical cords. Stem cells can also be harvested from whole blood, with the cells being extracted from bone marrow through daily injections of a drug called Filgrastim.
Bone marrow transplants are essentially a form of stem cell transplant. Interestingly, many who oppose stem cell research still support this type of therapy for treating leukemia and other conditions. Healthy adults between the ages of 18 and 60 can donate blood stem cells, and numerous organizations across the globe focus on screening and matching these donations.
6. Live Donations
Not all life-saving donations come from deceased individuals. The most well-known forms of live donations include blood, bone marrow, and blood stem cells. It is common knowledge that humans have two kidneys and can live with just one. Fewer people know that it's possible to donate one or two lobes of the liver, and this remarkable organ will regenerate itself to near full size in both the donor and recipient in a short time. A person can also donate a whole lung or part of a lung, part of the pancreas, or part of the intestines. Though these organs won't regenerate in either recipient or donor, they continue to function fully. Additionally, many parents are grateful to those who choose to donate sperm or ova, one of the few live donation types where monetary compensation is generally accepted and not considered immoral.
Interesting sidenote: According to OrganDonor.gov, “Surprisingly, it is also possible for a living person to donate a heart, but only if he or she is receiving a replacement heart. This occurs when it is determined that someone with severe lung disease and a normally functioning heart would have a better chance of survival by receiving a combined heart and lung transplant. As a result, the heart-lung recipient’s own heart, if it’s in good condition, is donated to another person who needs a heart transplant.” Currently, there are 82 heart/lung recipients on the U.S. waiting list.
5. Ethnicity

In today’s world, we are all increasingly acknowledging that 'all men are created equal.' However, when it comes to organ donation, this ideal is not always reflected. Unfortunately, ethnicity plays a significant role in disease and organ failure statistics. The U.S. Department of Health and Human Services reports that 'Native Americans are four times more likely than Whites to suffer from diabetes. African Americans, Asian and Pacific Islanders, and Hispanics are three times more likely than Whites to develop kidney disease. Many African Americans also suffer from high blood pressure (hypertension), which can lead to kidney failure.'
As a result of these disparities, ethnicity becomes an important factor when matching potential organ donors to recipients. An ethnic match can often be critical in ensuring a successful transplant and minimizing rejection issues. Unfortunately, cultural beliefs and religious restrictions sometimes make it challenging for individuals from minority groups to consider becoming donors, ultimately impacting those who desperately need life-saving organ transplants.
4. Suicides

While society generally views suicide as a tragic and misguided response to one's struggles, there are rare instances where this act inadvertently leads to a life-saving outcome. In approximately 3.8% of suicide cases resulting in brain death, the individuals may become viable organ donors. Families are more likely to approve organ donation in these cases than in other causes of death, though the reasons for this trend are not fully understood. Most of these cases involve young men, averaging 26 years old, who typically have healthy organs.
In contrast, lawmakers are revising regulations in an effort to prevent individuals from seeking to give the ultimate gift of life through suicide. A prominent example of suicide-related organ donation was depicted in the 2008 movie *Seven Pounds*, starring Will Smith. This film, in fact, prompted my research, which led to the creation of this list.
3. Organ Tourism

We often find ourselves shocked and disturbed by movies like *Turistas* and TV shows that increasingly feature plots around the dark world of black market organ trade. These terrifying portrayals are actually reflecting a disturbing reality that is growing due to the escalating demand for transplantable organs. This phenomenon, often called “organ tourism,” “transplant tourism,” or “organlegging” (similar to bootlegging, but for organs), is widespread in underdeveloped countries. In many overcrowded, economically struggling regions, selling a spare organ may be one of the few ways to earn a living. Unfortunately, these illegal surgeries typically take place in unsanitary conditions, using unsterile equipment, and the focus afterward is on delivering the harvested organ to its buyer, not on the donor’s recovery. In cases where the donor survives the procedure, they are frequently left with far less than the promised payment, which can range from $500 to $5000.
Debates about the right to sell one’s organs are ongoing, with discussions about creating laws to regulate this practice country by country. Proponents of legalized payment argue that compensating organ donors would encourage more people to donate. However, opponents are concerned that allowing such transactions would make transplants available only to the wealthiest, exacerbating inequalities. Regardless, the trade in organs continues, and regulating the safety of all parties involved will remain challenging until these legal and ethical issues are resolved.
2. Rejection
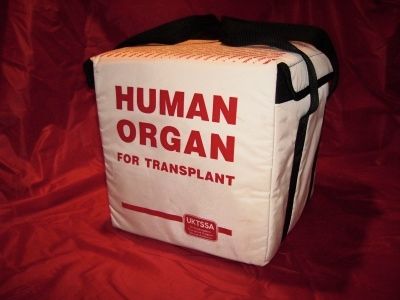
The breakthrough that allowed these life-saving gifts to even exist in the first place came when scientists unlocked the mysteries of organ rejection. The discovery of blood groups by Professor Karl Landsteiner in 1900 paved the way for significant advancements in immunology. Transplant rejection occurs when the body’s immune system identifies the transplanted organ as foreign tissue, much like it would attack a virus or bacteria. However, since an organ isn’t a harmful invader, doctors work diligently to ensure compatibility between donor and recipient to prevent this reaction.
Before an organ donation takes place, each potential donor undergoes thorough screening to assess any risks of infection, disease, or complications, ensuring that the organs are in optimal condition for transplant. Hyperacute rejection, which typically occurs within minutes of the surgery due to a blood type mismatch, can only be addressed by removing the organ. Acute rejection can occur within one week to three months after surgery and is often treated with a short course of powerful corticosteroids that suppress the immune system. In some cases, a bone marrow transplant from the same donor as the organ can help reduce rejection. Chronic rejection, however, is a long-term failure of the organ that cannot be reversed or treated effectively.
1. Waiting Lists
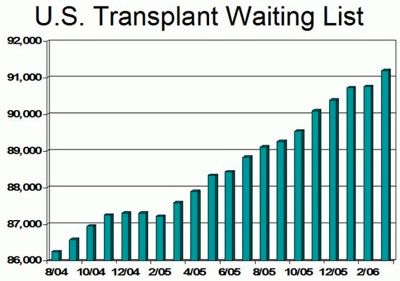
Everyone has experienced the frustration of waiting in a line, but no wait is more tense or life-threatening than the wait for an organ transplant. The United Network for Organ Sharing (UNOS) updates its list of transplant candidates daily, with a staggering 104,945 individuals currently on the list. Of those, 80% are waiting for kidneys. Because the need for organs far exceeds the supply, waiting times can be lengthy. For instance, the average wait for a heart transplant is three weeks, while a kidney transplant can take as long as 476 days. Lung transplants can have the longest waiting times, often up to 1,068 days for a single lung, nearly three years. While the U.S. performs about 74 transplants daily, 17 people die each day while still waiting for a match.
