Henrietta Lacks' life story is as remarkable as it is groundbreaking. A poor African American tobacco farmer from southern Virginia, she was diagnosed with a particularly aggressive form of cervical cancer.
For years, scientists struggled to grow human cells in the lab, but all attempts failed. However, after a biopsy of Henrietta’s tumor, a breakthrough occurred. The consequences were so profound that they forever altered the course of medical research.
10. Henrietta’s Tumor Gave Birth to the First Ever Immortal Human Cells Cultivated in a Lab

In January of 1951, Henrietta visited the Johns Hopkins Gynecology Clinic due to severe bleeding. There, she was diagnosed with cervical cancer, had a tissue sample taken from her tumor, and received radiation and surgical treatments. Tragically, her cancer advanced too quickly, and she passed away in October of that year.
Henrietta’s tissue sample was sent to Dr. George Otto Gey, the director of tissue culture research at Johns Hopkins. For years, Gey had been working tirelessly to create a cell line that could survive indefinitely in a laboratory setting.
After many attempts, he finally succeeded using his unique cultivation method. This process involved immersing the cells in a mixture of chicken plasma, beef embryo extract, and human placental cord serum. Upon examination, Gey found that Henrietta’s cells were multiplying rapidly and continuously.
Within just two years, Henrietta’s tissue samples were carefully packaged and sent across the globe. The cells were named “HeLa,” derived from the first two letters of Henrietta’s first and last names.
It’s worth noting that the total number of HeLa cells grown so far could stretch over 105 kilometers (65 miles)—enough to encircle the Earth’s equator more than three times.
Despite being cancerous, HeLa cells behaved like typical cells in the human body. This unique characteristic allowed scientists to observe how they reacted in different environments. What was once considered unethical or out of reach for research became possible as scientists began to understand cell division and the effects of viruses on cells.
The tragic end of one woman’s life marked the beginning of an extraordinary journey in science and medicine.
9. Her Cells Were Taken Without Her Knowledge or Consent

In the 1950s, it was not considered unethical to include individuals in scientific research without their consent or to administer unauthorized medical treatments. At that time, there were no legal protections for people like Henrietta, whose privacy was violated by researchers.
Dr. Gey initially concealed Henrietta’s identity by attributing the breakthrough to a fictional woman named “Helen Lane.” The truth about her identity didn’t emerge until years later.
While Henrietta did not receive the recognition she deserved during her lifetime, Dr. Gey appeared to have good intentions. It is said that he dedicated his life to cell culture research, even using his own family and himself in his experiments.
Dr. Gey’s sole hope for Henrietta’s cells was that they would make the kind of scientific impact they ultimately did. Despite facing financial difficulties, Gey never sold any of Henrietta’s tissue samples. However, many companies and industries would go on to profit from the HeLa cells he cultivated.
8. The Case of the Immortal Cells Remained a Medical Mystery
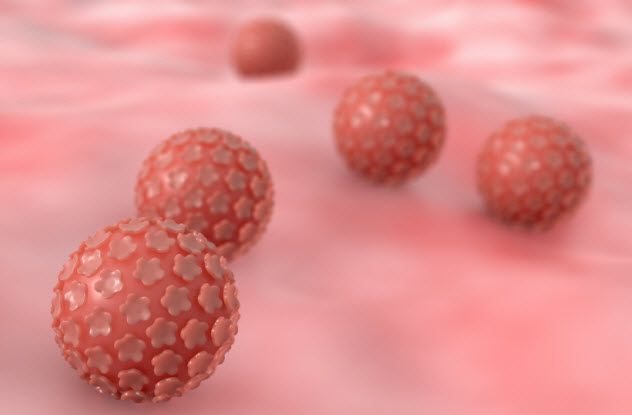
For years, scientists were puzzled by why Henrietta’s cancer cells continued to multiply at such an aggressive pace without dying. Some speculated that the combination of human papillomavirus (HPV) and Henrietta’s genetic makeup might have been the catalyst for the cells' unusual behavior.
Additionally, it was discovered that Henrietta had syphilis, which may have contributed to the rapid growth of her cancer cells due to a compromised immune system. However, it wasn’t until 2013 that a highly plausible explanation for the phenomenon emerged.
A study conducted by researchers from the University of Washington revealed that the mutated HPV genome, which carries its own cancer-causing genes, inserted itself near an oncogene in Henrietta’s DNA. This triggered the oncogene and led to the rapid replication of HeLa cells within her body.
“In a way, this was a perfect storm of cellular malfunction,” explained Andrew Adey, one of the study’s authors. “The HPV virus integrated into her genome in possibly the worst way imaginable.”
7. The Lacks Family Was Left in the Dark About the HeLa Cells

Although Henrietta’s cells contributed to saving millions of lives, neither she nor her family saw any benefit. Initially, her family was completely unaware that her cells were being used in such groundbreaking research. It wasn’t until years later, when Bobette Lacks, Henrietta’s daughter-in-law, met a cancer researcher by chance, that she learned that Henrietta’s cells had been growing since her death in 1951.
Tragically, the treatments derived from HeLa cells were beyond the Lacks family’s reach. Like many others without insurance, they couldn’t afford them. Henrietta’s husband suffered from prostate cancer, their eldest daughter had developmental challenges, and another daughter dealt with various medical issues—all of which went untreated. The family that should have been compensated never received a penny.
In an unexpected turn of events, the Lacks family finally received some compensation in 2013 for their matriarch’s contribution. A team from the European Molecular Biology Laboratory had sequenced and published Henrietta’s genome without her family’s consent.
When Henrietta’s grandchildren learned about the publication, they felt that this research further infringed upon their family’s private medical history. They took a firm stand and demanded that the scientists retract their study.
After some time, the family agreed to allow the release of much of the information regarding Henrietta’s genome.
6. HeLa Cells Played a Crucial Role in Early Cancer Research
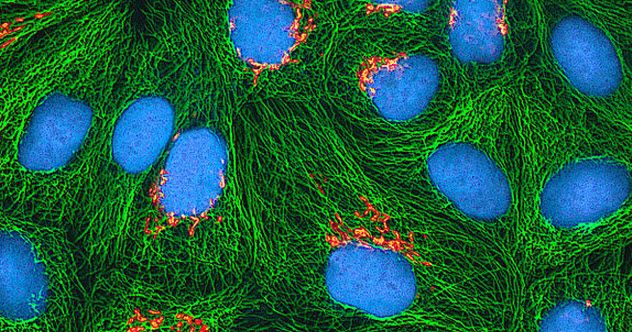
Through research conducted with HeLa cells, scientists have gained significant insights into how cancer cells function. One key discovery was that Henrietta’s cancer cells triggered the activation of an enzyme called telomerase, which the cells used to repair damaged DNA. This enabled HeLa cells to multiply and survive, unlike regular cells which die after a short period.
Scientists also found that telomerase played a role in extending the length of chromosomes. In normal human cell division, telomeres (the protective ends of chromosomes) shorten with each division, and eventually, the cells are destroyed once the telomeres can no longer shorten.
In contrast, HeLa cells behave differently. Due to the hyperactivity of telomerase in these cells, the telomeres never run out. This continuous cell division has made HeLa cells an indispensable tool for cancer research, even to this day.
These breakthroughs have paved the way for further research, leading to significant advancements in cancer treatment.
5. HeLa Cells Contributed to the Advancement of Genetic Research
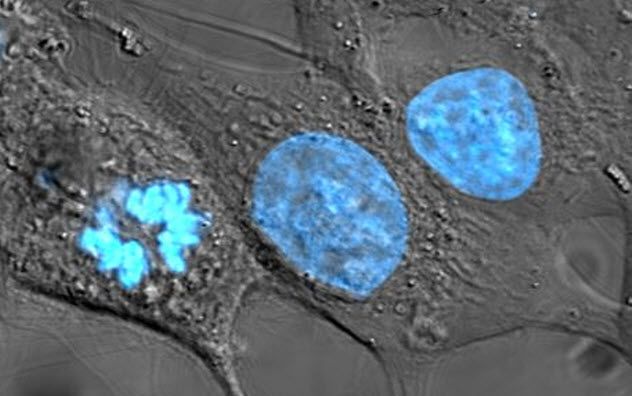
In 1953, a Texas-based geneticist was working with HeLa cells when a chemical accidentally spilled on them. What initially seemed like a potential disaster turned out to be an unexpected blessing. Upon further examination, the scientist observed that the chromosomes within the cells grew larger and untangled, making them significantly more visible.
Two years later, Joe Hin Tjio and Albert Levan refined the technique, leading to the groundbreaking discovery that human cells have precisely 46 chromosomes. Prior to this breakthrough, it had been extremely difficult to accurately count chromosomes due to the small size and dense structure of DNA.
Additionally, it was once widely believed that humans had 48 chromosomes, just like chimpanzees and gorillas. However, Tjio and Levan's work disproved this theory. This discovery was a game-changer, as it enabled the identification of genetic disorders when cells showed more or fewer than 46 chromosomes.
4. Research with HeLa Cells Led to the Development of the Cervical Cancer Vaccine

In 2008, German virologist Harald zur Hausen was awarded the Nobel Prize for his groundbreaking discovery that two specific strains of HPV were directly linked to cervical cancer. In the 1970s, it was widely believed that herpes simplex was the cause of cervical cancer.
However, working with the HeLa cell line, zur Hausen found that certain strains of HPV, including HPV16 and HPV18, inserted their genetic material into cervical cells, triggering abnormal cell replication and the development of cancer.
Years before zur Hausen’s breakthrough, scientists were already working on an HPV vaccine to prevent the virus and lower the risk of cervical cancer in women. In the 1990s, researchers from the National Cancer Institute discovered specific proteins on the virus's surface that resembled the virus itself. This discovery was crucial because these proteins were found to trigger the production of antibodies.
All of this research ultimately led to the creation of Gardasil and Cervarix, two widely available HPV vaccines.
3. Some Scientists Propose That HeLa Cells Could Represent a New Species
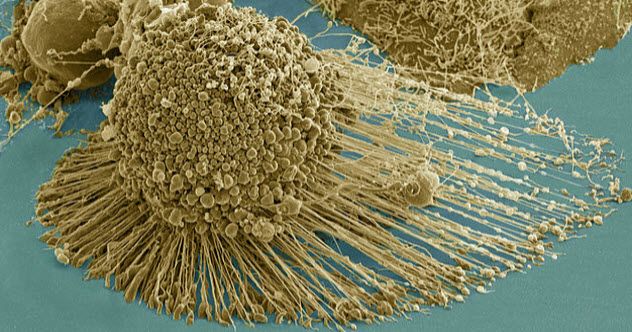
Evolutionary biologist Leigh Van Valen from the University of Chicago suggests that HeLa cells are not connected to humans. He and other scientists argue that these cells are microbial in nature, vastly different from human cells, and should be considered an entirely new species.
HeLa cells are believed to have evolved genetically over time, adapting to the environment of the petri dish through natural selection. Reports indicate that new strains of HeLa cells have emerged in recent years.
One study proposes that the generation of cancer cells could be the foundation for the creation of a new species. It also suggests that tumors could be regarded as 'parasitic organisms.'
Researchers have even suggested a new scientific name for HeLa cells—Helacyton gartleri—honoring Stanley Gartler, who recognized the remarkable success of these cells.
2. HeLa Cells Played a Pivotal Role in the Development of the Polio Vaccine

Jonas Salk, a researcher at the University of Pittsburgh, devoted years of relentless effort to eradicating the polio epidemic that ravaged the US in the 1950s. However, before he could finalize his polio vaccine, he required vast quantities of tissue samples for his research.
Fortunately, the National Foundation for Infantile Paralysis funded a specialized facility at Tuskegee Institute dedicated to the production of HeLa cells. With these cells in hand, Salk was able to conduct large-scale testing.
On April 26, 1954, testing began on nearly two million children from the US, Finland, and Canada. The results were overwhelmingly positive—the vaccine proved both safe and effective. Since then, it has become a fundamental part of child healthcare worldwide.
1. HeLa Cells Had Contaminated Other Cell Cultures Globally

In 1966, geneticist Stanley Gartler was examining tissue samples when he made an unusual discovery. Every sample contained an enzyme known as glucose-6-phosphate dehydrogenase-A (G6PD-A).
Gartler was baffled because he knew these tissue samples came from Caucasians and even animals. G6PD-A is a rare enzyme typically found only in humans, and almost exclusively in African Americans. This raised concerns as it indicated the contamination of Gartler’s samples, and likely many others.
Gartler speculated that the HeLa cell line was to blame. Though initially met with skepticism from other scientists worried about the financial implications, Gartler’s suspicions were ultimately confirmed. Samples had been contaminated during transfers between labs, resulting in a significant loss of research investments.
It was later discovered that HeLa cells could travel through the air. At the time, laboratories lacked the proper containment systems to prevent such contamination. Fortunately, advances in cell culture techniques have since addressed these concerns.
