 This image highlights that the Centers for Disease Control and Prevention operates beyond its Georgia headquarters. The sign is displayed in the sample processing zone of the CDC Ebola laboratory in Bo, Sierra Leone.
© David Snyder/ZUMA Press/Corbis
This image highlights that the Centers for Disease Control and Prevention operates beyond its Georgia headquarters. The sign is displayed in the sample processing zone of the CDC Ebola laboratory in Bo, Sierra Leone.
© David Snyder/ZUMA Press/CorbisFrom the West African Ebola crisis to the measles outbreak at Disneyland, it's clear why infectious diseases dominate 21st-century concerns (though we hope not literally). Fears of bioterrorism, fueled by the post-9/11 anthrax attacks and lingering worries about potentially unsecured Soviet smallpox reserves, further amplify a sense of vulnerability. This makes us wonder: what are the most dangerous pathogens stored at the Centers for Disease Control and Prevention in Georgia?
In its mission to save lives, combat infectious diseases and bioterrorism, and address major health challenges in the U.S. and globally, the CDC must navigate a delicate balance. Without the ability to study diseases, its scientists cannot effectively control or prevent them. This is their core responsibility, as reflected in their name, and they carry it out in one of the world's most secure and advanced facilities. Imagine it as a high-security prison for the most dangerous pathogens, and consider this a curated list of 10 major public health threats.
10: Rabies
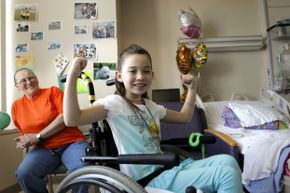 Precious Reynolds, an eight-year-old girl shown here at UC Davis Hospital in Sacramento, California, made history as the sixth person to overcome rabies without vaccination.
© Michael Macor/San Francisco Chronicle/San Francisco Chronicle/Corbis
Precious Reynolds, an eight-year-old girl shown here at UC Davis Hospital in Sacramento, California, made history as the sixth person to overcome rabies without vaccination.
© Michael Macor/San Francisco Chronicle/San Francisco Chronicle/CorbisAs children, we dreaded dog bites not just for the immediate pain but for the terrifying prospect of rabies shots—dozens of large needles injected into the stomach. While the thought was horrifying, we didn’t realize how much worse the disease itself could be.
After an incubation period of three to 12 weeks, rabies often begins with numbness or tingling at the bite site, worsening over time. This prodromal phase lasts up to 10 days, followed by acute symptoms like fever, headache, weakness, and discomfort. These escalate to anxiety, confusion, insomnia, hallucinations, partial paralysis, excessive salivation, and difficulty swallowing. Once acute symptoms manifest, coma and death typically occur within a week.
Rabies claims over 55,000 lives each year, primarily in Africa and Asia, but it is entirely preventable with timely treatment. Modern post-exposure vaccinations no longer involve stomach injections. Instead, patients receive multiple rabies vaccine doses over four days, along with human rabies immune globulin administered at the bite site and intramuscularly elsewhere [source: CDC].
9: Primary Amoebic Meningoencephalitis (PAM)
 Worried about brain-eating amoebas in lakes? Don’t be. Simply hold your nose when diving in.
© John Lund/Drew Kelly/Blend Images/Corbis
Worried about brain-eating amoebas in lakes? Don’t be. Simply hold your nose when diving in.
© John Lund/Drew Kelly/Blend Images/CorbisThe term 'brain-eating amoeba' is as terrifying as it sounds. This refers to Naegleria fowleri, a deadly microorganism that causes meningoencephalitis, a condition akin to bacterial meningitis. With a fatality rate exceeding 97 percent, most victims succumb within days. However, infections are extremely rare, with only 34 cases reported in the U.S. between 2004 and 2013 [source: CDC].
While Naegleria fowleri thrives in warm freshwater and soil across the U.S., infections occur only when contaminated water enters the nasal cavity deeply. This can happen during activities like using neti pots, religious submersion, or swimming and diving in lakes, rivers, or poorly chlorinated pools. Initial symptoms, appearing one to seven days post-infection, mimic bacterial meningitis and include headaches, fever, nausea, and vomiting. These progress to a stiff neck, confusion, hallucinations, balance issues, reduced awareness, and seizures. Once symptoms emerge, the condition deteriorates rapidly, often leading to death within one to 12 days.
Currently, there is no effective treatment for PAM, nor is there a reliable method to detect the amoeba in water [source: CDC]. In two cases, doctors managed partial success using brain-swelling control and miltefosine, an experimental drug for breast cancer and leishmaniasis. However, all other cases have been fatal, leaving the efficacy of such treatments uncertain [sources: CDC; Jacobson].
8: Plague
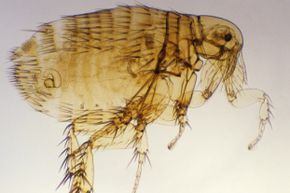 This is the Oriental rat flea (Xenopsylla cheopsis), a key carrier of bubonic plague.
© Dr. Robert Calentine/Visuals Unlimited/Corbis
This is the Oriental rat flea (Xenopsylla cheopsis), a key carrier of bubonic plague.
© Dr. Robert Calentine/Visuals Unlimited/CorbisOur next subject is infamous. Responsible for wiping out 60 percent of Europe’s population in the 14th century, it has shaped history by collapsing empires and spurring societal and technological shifts. Today, it primarily lurks in rural areas of Africa, Asia, and South America, though it also appears in the American West, with an average of seven cases annually from 1900 to 2010 [source: CDC].
The bacteria Yersinia pestis is responsible for three types of plague:
- Bubonic plague, usually transmitted through bites from infected rodent fleas
- Septicemic plague, which can result from flea bites, contact with fluids or carcasses of plague-infected animals, or untreated bubonic plague
- Pneumonic plague, caused by inhaling respiratory droplets from infected cats or humans with pneumonic plague or other forms that have reached the lungs
Bubonic plague patients rapidly develop symptoms like fever, headache, chills, weakness, and painful, swollen lymph nodes called buboes, where the bacteria thrive. Without proper antibiotics, the infection can spread, leading to septicemic or pneumonic plague. Septicemic plague adds abdominal pain, shock, and potential internal bleeding, while pneumonic plague causes severe pneumonia, respiratory failure, and shock.
With the advent of antibiotics, the fatality rate of plague has decreased from 66 percent to 11 percent. However, untreated septicemic and pneumonic plagues remain universally fatal [sources: CDC; WHO].
7: Smallpox
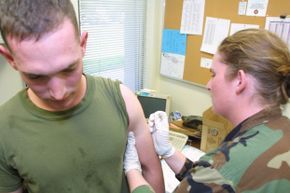 A U.S. Marine stationed at Camp Pendleton receives a smallpox vaccination prior to deployment to the Persian Gulf.
© Tim Rue/Corbis
A U.S. Marine stationed at Camp Pendleton receives a smallpox vaccination prior to deployment to the Persian Gulf.
© Tim Rue/CorbisThe 2014 discovery of misplaced variola samples reignited fears of a potential smallpox outbreak in a population no longer routinely vaccinated. The U.S. holds a strategic reserve of smallpox vaccine, which, if administered within three to four days of exposure, can mitigate infection and significantly reduce mortality. However, concerns about bioterrorism remain, particularly if the virus is genetically modified or weaponized [sources: Aleccia; CDC].
Smallpox manifests in two forms. Variola major, characterized by a widespread rash and high fever, is more severe, while the milder variola minor has a mortality rate of just 1 percent. Variola major is further categorized into ordinary (over 90 percent of cases), modified (a less severe form seen in previously vaccinated individuals), and two rare, severe types: flat-type (malignant) and hemorrhagic. While ordinary variola major has a 30 percent fatality rate, flat and hemorrhagic types are almost always deadly [sources: Inglesby et al.; CDC].
Transmission occurs through prolonged face-to-face contact, direct exposure to infected bodily fluids or contaminated items, or, in rare cases, airborne spread in confined spaces like buses or planes. After a noncontagious incubation period of seven to 17 days, symptoms begin with two to four days of flu-like signs, followed by four days of contagious skin and mouth rashes. Over subsequent weeks, these rashes spread, forming raised bumps filled with thick fluid and featuring distinctive central indentations. Pustules eventually form, scab over, and fall off, leaving pitted scars. Smallpox remains infectious until the last scab detaches [source: CDC].
6: Ebola Virus
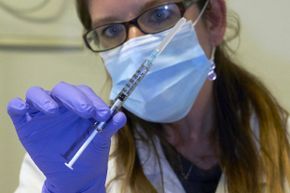 A nurse displays a syringe containing an experimental Ebola vaccine during a media event at Lausanne University Hospital in Switzerland on November 4, 2014.
© Denis Balibouse/Reuters/Corbis
A nurse displays a syringe containing an experimental Ebola vaccine during a media event at Lausanne University Hospital in Switzerland on November 4, 2014.
© Denis Balibouse/Reuters/CorbisThe 2014 Ebola outbreak in West Africa became the deadliest in history, with Guinea, Liberia, and Sierra Leone reporting 14,432 confirmed cases and 9,936 deaths by March 7, 2015. The outbreak also affected Nigeria (20 cases), Senegal (1), Mali (8), Spain (1), the U.K. (1), and the U.S. (4) [source: CDC].
Despite requiring direct contact with infected blood or bodily fluids for transmission (though some cases in Africa may result from handling bushmeat or infected bats), Ebola evokes widespread fear. This is likely due to its high fatality rate, ranging from 25 to 90 percent depending on the outbreak, with an average of 50 percent. The absence of a cure or rapid, reliable diagnostic test exacerbates these fears. The disease's progression, beginning two to 21 days post-exposure (typically eight to 10 days), includes symptoms like unexplained bleeding, fever, severe headache, muscle pain, weakness, diarrhea, vomiting, and abdominal pain. Additionally, fears of the virus mutating into an airborne strain, fueled by media and films, contribute to the panic.
The battle against Ebola is further complicated by the unresolved mystery of its natural reservoir host. While bats are suspected, the lack of definitive knowledge makes it impossible to predict when or where the virus might emerge in humans and trigger an outbreak [source: CDC].
5: Marburg Hemorrhagic Fever
 A newspaper reports on the Marburg virus outbreak in Kampala, Uganda, in October 2014.
© James Akena/Reuters/Corbis
A newspaper reports on the Marburg virus outbreak in Kampala, Uganda, in October 2014.
© James Akena/Reuters/CorbisUnlike Ebola, the reservoir host for Marburg hemorrhagic fever is known: the African fruit bat, Rousettus aegyptiacus. While the exact transmission method from bats to humans remains unclear, scientists believe it occurs in bat-filled mines or caves, where humans may encounter bat droppings or airborne droplets of bat fluids like urine. Once transmitted to humans, it spreads similarly to Ebola, through direct contact with infected bodily fluids. Marburg is primarily found in Africa [source: CDC].
After an incubation period of five to 10 days, symptoms begin abruptly with fever, chills, headache, and muscle pain. Around five days later, a maculopapular rash (raised, spotted lesions) appears, mainly on the torso. This is often accompanied by nausea, vomiting, chest pain, sore throat, abdominal pain, and diarrhea. As the disease progresses, symptoms worsen, leading to jaundice, pancreas inflammation, severe weight loss, delirium, shock, liver failure, massive bleeding, and multi-organ failure [source: CDC].
Similar to Ebola, Marburg HF has no known cure, with fatality rates varying significantly between outbreaks (23-90 percent) [sources: CDC; WHO]. Diagnosing the virus is challenging, as its symptoms mimic those of other infectious diseases like malaria and typhoid fever. While some experimental treatments have shown promise in nonhuman primate studies, they remain unapproved for human use [source: CDC].
4: Anthrax
 Biohazard signs at the American Media Center in Boca Raton, Florida, alert visitors after several employees were exposed to anthrax, one of whom later died.
© Reuters/Corbis
Biohazard signs at the American Media Center in Boca Raton, Florida, alert visitors after several employees were exposed to anthrax, one of whom later died.
© Reuters/CorbisCertain infectious diseases are as widespread as soil and, under normal conditions, relatively harmless. However, when they find a suitable environment—or are weaponized by humans—they can become deadly threats.
Consider Bacillus anthracis, a rod-shaped bacterium found globally in soil. Its spores remain inactive until they enter a host, where they multiply and produce harmful toxins. Domestic and wild animals can inhale or ingest spores from contaminated soil, plants, or water. Though rare, humans can contract anthrax through contact with infected animals or contaminated animal products.
Anthrax infects humans through four primary pathways:
- Cutaneous, through cuts or abrasions while handling infected animals
- Gastrointestinal, from consuming contaminated food or drink
- Injection, primarily affecting heroin users in northern Europe
- Inhalation, from weaponized anthrax or exposure to contaminated animal products like hair, hides, or wool
Each type of anthrax presents distinct symptoms, which may emerge anywhere from one day to over two months after exposure [source: CDC]. Inhalation and gastrointestinal anthrax initially resemble severe flu, but gastrointestinal anthrax also includes swollen lymph nodes and potentially bloody diarrhea or vomiting. Cutaneous anthrax causes blisters and ulcers, while injection anthrax progresses more rapidly, adding fever and chills to the mix.
Untreated anthrax can be fatal, but all forms are preventable and treatable with proper precautions and antibiotics. A vaccine is available, though it is reserved for high-risk adults. Some nations, including the U.S., implement veterinary public health programs to vaccinate animals against anthrax.
3: Clostridium Botulinum Toxin
 A detailed view of Clostridium botulinum
© Visuals Unlimited/Corbis
A detailed view of Clostridium botulinum
© Visuals Unlimited/CorbisOver the last 50 years, medical advancements have reduced botulism's fatality rate from 50 percent to just 3-5 percent. However, the neurotoxin produced by Clostridium botulinum bacteria (and occasionally by Clostridium butyricum and Clostridium baratii) remains highly dangerous.
Naturally present in soil and household surfaces like floors, carpets, and countertops, the bacteria often gains attention through foodborne outbreaks. However, botulism can also manifest in four other forms: wound botulism, infant botulism from ingested bacteria, rare adult intestinal colonization, and overdoses related to therapeutic or cosmetic uses like Botox [source: LDHH]. In the U.S., approximately 145 botulism cases are reported yearly, with 15 percent being foodborne (often linked to home canning), 65 percent infant, and 20 percent wound-related (associated with black-tar heroin use). Since honey can harbor the bacteria, it is advised not to give it to children under 12 months old [source: CDC].
Foodborne botulism symptoms typically appear 18-36 hours after ingestion, including blurred or double vision, drooping eyelids, slurred speech, dry mouth, and difficulty swallowing. Infant botulism presents as lethargy, weak crying, poor muscle tone, constipation, and feeding difficulties. Without treatment, both types can lead to muscle paralysis, spreading to respiratory muscles, limbs, and torso, ultimately causing death from respiratory failure.
Diagnosing botulism is challenging, but it can be treated with an antitoxin. For foodborne cases, treatments like enemas or induced vomiting may be necessary, while wound botulism might require antibiotics. Even for survivors, respiratory failure often necessitates weeks or months on a ventilator. Recovery can take weeks, with lingering weakness potentially lasting years.
2: Hantavirus
 A CDC researcher examines a deer mouse captured during a hantavirus study in New Mexico. The deer mouse is a primary carrier of this lethal virus.
© Karen Kasmauski/Corbis
A CDC researcher examines a deer mouse captured during a hantavirus study in New Mexico. The deer mouse is a primary carrier of this lethal virus.
© Karen Kasmauski/CorbisIn late 2012, the National Park Service confirmed 10 cases of hantavirus among Yosemite National Park visitors, three of which were fatal. This virus, with an average mortality rate of 38 percent, is found across western and central regions of the U.S. and Canada, as well as in Central and South America [source: CDC].
Hantavirus is transmitted through exposure to the urine, feces, or saliva of rodents, particularly the deer mouse (Peromyscus maniculatus), which carries the Sin Nombre strain in North America. While proper cleaning and rodent-proofing can reduce risks, disturbing areas inhabited by mice can release infectious particles into the air.
In the Americas, hantavirus can progress to hantavirus pulmonary syndrome (HPS), marking the onset of severe complications. Symptoms typically appear one to five weeks after exposure and include fatigue, fever, muscle pain, and, in about half of cases, headaches, dizziness, chills, and stomach issues. Within four to 10 days, coughing and shortness of breath develop as fluid accumulates in the lungs. Without a specific cure, treatment focuses on symptom management, often requiring intubation, with a fatality rate of 36 percent [source: CDC].
In other regions, hantavirus can also lead to hemorrhagic fever with renal syndrome (HFRS). Symptoms resembling the flu typically emerge one to two weeks after exposure and may include blurred vision, facial flushing, rashes, or red, inflamed eyes. As the disease progresses, patients may experience low blood pressure, acute shock, vascular leakage, and kidney failure. Treatment remains supportive, with fatality rates ranging from 1 to 15 percent [source: CDC].
For both HPS and HFRS, mortality rates depend on the specific hantavirus strain involved.
1: Variant Creutzfeldt-Jakob Disease (vCJD)
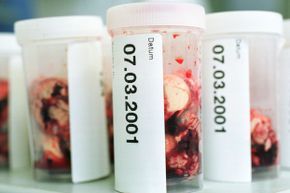 Brain tissue samples from slaughtered cows await testing for mad cow disease in Germany.
Sean Gallup/Newsmakers/Getty Images
Brain tissue samples from slaughtered cows await testing for mad cow disease in Germany.
Sean Gallup/Newsmakers/Getty ImagesA brain disorder linked to dementia might seem an unusual addition to a list of deadly diseases, but among those listed, only variant Creutzfeldt-Jakob disease (vCJD) is invariably fatal. Similar to classic CJD, vCJD causes abnormal folding of brain proteins, resulting in spongy deposits throughout the brain.
Unlike classic CJD, vCJD is believed to originate from the same agent responsible for mad cow disease (bovine spongiform encephalopathy) and is likely contracted through consuming contaminated beef products. Compared to CJD, vCJD typically affects younger individuals and progresses more slowly, taking around 14 months to prove fatal, compared to five months for CJD. It also presents distinct diagnostic features and includes additional psychiatric and sensory symptoms.
In addition to dementia, vCJD patients may experience poor coordination, involuntary muscle movements (myoclonus) or jerks (chorea), and heightened reflex responses (hyperreflexia) within four months of onset. The disease has no cure and inevitably results in progressive brain deterioration and death.
As of June 2014, the CDC reported over 220 vCJD cases worldwide, with the majority occurring in the United Kingdom (177 cases) and France (27 cases). Among the four confirmed cases in the United States, all were linked to exposure outside the country [source: CDC].
