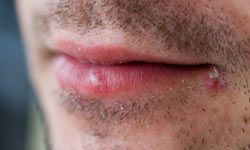
 Although cold sores are a lifelong condition, modern medical advancements have introduced antiviral treatments that can effectively push the virus into a dormant state.
©iStockphoto/Thinkstock
Although cold sores are a lifelong condition, modern medical advancements have introduced antiviral treatments that can effectively push the virus into a dormant state.
©iStockphoto/ThinkstockPainful. Awkward. Unattractive.
Cold sores are often described in many negative ways, and unfortunately, they are caused by a persistent virus that remains in the body for life [source: Mayo Clinic].
Although the unsettling reality is that an outbreak can occur unexpectedly, there is still optimism. While the virus cannot be eradicated from your body, it typically stays inactive for the majority of the time.
While the virus is dormant, there are several triggers you can steer clear of to prevent another outbreak. Moreover, various treatment options are available to reduce both the duration and intensity of an outbreak.
This article explores the common causes of cold sore flare-ups and highlights effective treatments to manage outbreaks when they occur.
10: Cause: Contact with an Infected Person
We begin our exploration of cold sore causes with the most apparent one: Exposure to someone carrying the virus.
Cold sores, also known as fever blisters, cannot develop unless the virus is initially transmitted from another individual [source: Mayo Clinic].
If you do not carry the virus, avoid sharing items that might come into contact with an active sore on someone else. This includes utensils, lip balm, towels, or any object that could touch the affected area [source: Mayo Clinic].
HSV-1, the herpes simplex virus responsible for cold sores, is closely related to HSV-2, which causes genital herpes. While they are not identical, both viruses can spread to the other region through direct contact [source: WebMD].
9: Treatment: Don't Touch
For both individuals experiencing an outbreak and those close to them who are virus-free, the primary rule and "treatment" is straightforward: Avoid touching the sore. Allow the outbreak to resolve on its own.
The herpes simplex virus is transmitted through the fluid from cold sore blisters, and it can spread even when the sore appears mild or unnoticeable [source: Mayo Clinic].
If you carry the virus, you risk spreading it to your eyes, leading to additional complications. Therefore, it’s crucial to wash your hands often and avoid touching the sore [source: McKinley].
8: Cause: Illness
For individuals with the cold sore virus, one common trigger is hinted at in its name—catching a cold.
In some cases, contracting a cold or the flu can lead to the emergence of a cold sore, particularly if accompanied by a fever (hence the term fever blister) [source: Mayo Clinic].
The link lies in the immune system, which plays a crucial role in controlling HSV-1. Individuals with compromised immune systems tend to experience cold sore outbreaks more frequently than those in good health [source: WebMD].
While colds, flu, or fevers can trigger cold sore outbreaks, they aren’t limited to winter. Any time your immune system is weakened, the virus has an opportunity to reactivate.
7: Treatment: Stay Healthy
While it’s impossible to completely prevent cold sore outbreaks, maintaining optimal health can help minimize their occurrence.
Regular exercise is a key factor in supporting a strong immune system, which can help decrease the frequency of cold sore flare-ups.
Additionally, prioritize getting adequate sleep. Rest is equally important as physical activity, so try to avoid pulling all-nighters whenever possible [source: McKinley].
6: Cause: Sunlight
Daily sun exposure is beneficial for overall health, such as aiding in the production of vitamin D. However, for cold sores, sunlight can act as an unwelcome trigger.
Excessive exposure to the sun’s ultraviolet rays can irritate the delicate skin on and around the lips. Even minor skin damage can reactivate the dormant virus, which typically resides in nearby nerve cells [source: McKinley].
Remember this the next time you spend extended periods in the sun.
You can take preventive measures to shield yourself from sun-induced cold sores, similar to how you protect your skin from sunburn. Many lip balms available today come with SPF protection.
5: Treatment: Protection from the Sun
Since excessive sun exposure can reactivate the dormant herpes simplex virus, it’s crucial to monitor how much sunlight your lips and mouth are exposed to.
Sensitivity to sunlight varies from person to person; only you can determine the level of ultraviolet exposure that might trigger a cold sore.
Before spending extended time in the sun, apply sunscreen to your face, especially the delicate skin around your mouth [source: WebMD].
4: Cause: Stress
What if you haven’t caught a cold, don’t have a fever, and haven’t spent much time in the sun, yet still develop a fever blister? The mere possibility might be enough to stress you out.
However, try not to stress. Seriously. Stress is a known trigger for those with HSV-1 [source: McKinley].
It’s not stress itself that directly causes outbreaks, but rather its impact on the body. Similar to illness, excessive stress weakens the immune system, creating an opportunity for cold sores to emerge.
You might have heard these terms but aren’t certain: Are cold sores and canker sores the same? They are not. Canker sores, which are shallow ulcers inside the mouth, may resemble cold sores in some ways, but they are not viral and therefore not contagious [source: WebMD].
3: Treatment: Relaxation Techniques
Just as stress can trigger an outbreak, practicing relaxation techniques can help prevent cold sores.
Everyone experiences stress in their lives, but how you manage it makes all the difference.
Choose methods that calm both your body and mind to lower overall stress levels (and no, we’re not just referring to a post-work glass of wine).
Some individuals find relief through rhythmic deep breathing or relaxation practices such as yoga [source: McKinley].
2: Cause: Menstruation
The final cause on our list is one that’s largely beyond your control, especially if you’re female.
A woman’s menstruation cycle can influence the occurrence of cold sores, though its impact varies from person to person. For some women with HSV-1, menstruation has no effect, while for others, it can trigger outbreaks [source: Mayo Clinic].
There’s no way to predict how it will affect you until it happens, so there’s no need to stress about your next period (especially since stress itself is a trigger).
Internet rumors have linked the drinking game "beer pong" to the spread of cold sores. While some claimed the Centers for Disease Control was studying this connection, the CDC has debunked it as a hoax, confirming no such study exists [source: Centers for Disease Control and Prevention].
1: Treatment: Medication
Our final treatment is one that many would anticipate for an illness, though its effectiveness against viruses is limited.
As previously mentioned, cold sores are caused by HSV-1, a virus that typically remains in the host (the human) for life.
However, modern medical advancements have introduced antiviral medications that can suppress the virus, pushing it back into dormancy. Common treatments for cold sores include acyclovir, valacyclovir, famciclovir, and penciclovir [source: Mayo Clinic].
For additional information on cold sores, refer to the next page for a wealth of details.
