At 23, I began experiencing unexplained vision loss, leaving doctors baffled.
It started subtly with minor issues during a standard eye test. Soon, I was shuffled between optometrists, ophthalmologists, and neuro-ophthalmologists, yet no one could pinpoint the cause. When specialists with complex titles are stumped, you know something’s seriously wrong.
This struggle lasted almost two years, with my sight gradually worsening. Now, at 41, my corrected vision is 20/70. While it’s far from ideal, as this list demonstrates, it could have been much more devastating.
10. Brain Tumor

“Mass lesion.”
The most terrifying phrase I’ve ever seen was scribbled on a medical notepad. I peeked while the optometrist stepped out—perhaps, I imagined, to arrange my final rites. My anxiety spiked because the eye exam had clearly gone poorly; the doctor’s alarming note was accompanied by my visual field test results, revealing significant blind spots, or scotomas, in both eyes.
The blind spots were largely symmetrical. My left eye had major gaps in the upper left quadrant, while the right eye was affected in the upper right. Later, I discovered the optometrist suspected a brain tumor pressing on my optic chiasm—the area where optic nerves intersect at the brain’s base. Pressure from a lesion here could explain the bilateral vision damage I was experiencing.
The visual field test was prompted by my inability to read the 20/20 line even with prescription glasses. While this might be expected in older individuals, it was alarming for someone my age—just 23.
Of course, the optometrist couldn’t confirm this immediately, so “mass lesion” wasn’t a diagnosis but a referral. They scheduled an MRI to check for a tumor causing my vision loss. After what felt like the longest four days of my life, the results finally arrived.
…clear. No tumor. I wasn’t dying, but the cause of my vision loss remained a mystery. The rest of this list includes conditions I might have had, and one I actually do.
9. Retinitis Pigmentosa

Often abbreviated as RP, retinitis pigmentosa is as frightening as it sounds. Essentially, your field of vision gradually narrows, beginning with peripheral blindness that progresses to tunnel vision. Over time, this tunnel further contracts, potentially leading to complete blindness.
The condition gets its name from the deterioration and loss of retinal cells—the light-sensitive tissue at the back of the eye. It stems from mutations in any of over 50 genes crucial for the healthy development of retinal photoreceptors, known as rods and cones due to their shapes. RP is uncommon but not extremely rare, affecting roughly 1 in 4,000 people. Given my visual field test results, those odds suddenly felt uncomfortably close.
In its early stages, RP typically causes night blindness and a slow reduction in the visual field. The rate of progression varies, but most individuals with RP eventually lose a significant portion of their vision, often to the point where daily tasks like reading, driving, walking unaided, or recognizing faces and objects become extremely challenging. What a joy!
An electroretinogram, commonly referred to as an ERG, is one of the diagnostic tools for Retinitis Pigmentosa (RP). It assesses the electrical responsiveness of photoreceptors. A diminished reaction typically indicates fewer cells, a hallmark of RP. In my case, the results were within the normal range, effectively excluding RP as a diagnosis.
8. Macular Degeneration

Macular Degeneration stands as the primary cause of vision impairment, impacting over 10 million individuals in the United States alone—surpassing the combined numbers of cataracts and glaucoma. Unlike cataracts, which are treatable, or glaucoma, which can be managed effectively with treatment, Macular Degeneration remains incurable and largely irreversible.
Macular Degeneration involves the breakdown of the central retina, known as the macula. This area is crucial for central vision, which is essential for detailed tasks. The macula enables activities such as reading, driving, color differentiation, and facial recognition.
The progression of Macular Degeneration can vary widely, sometimes halting without clear reason. Individuals with mild cases might not notice any significant vision loss. However, as the condition advances, symptoms like distorted or blurry vision may appear. In severe cases, central vision can be entirely lost, leaving only peripheral vision—essentially the reverse of tunnel vision.
Macular Degeneration is categorized into two primary forms: 'dry' and 'wet'. The dry type, accounting for 85-90% of cases, is characterized by the buildup of drusen, yellowish deposits beneath the macula, without any fluid leakage. This form typically offers a more favorable outlook, with many patients maintaining relatively good central vision, around 20/40.
Wet Macular Degeneration involves the growth of irregular blood vessels beneath the macula. These vessels leak, causing swelling and potentially leading to swift and significant vision deterioration.
Typically associated with aging, Macular Degeneration manifests later in life. However, Stargardt disease, a rarer variant, affects younger individuals and often results in a less optimistic prognosis for preserving vision. Thankfully, this condition did not apply to me, as my macula were in good health.
7. River Blindness

In cases of unexplained vision loss, physicians often pose specific, sometimes obscure questions to eliminate rare possibilities. One such question is, 'Have you recently traveled to Africa or tropical regions?'
Onchocerciasis, often referred to as River Blindness, is a condition affecting the eyes and skin, caused by microscopic worms transmitted via blackfly bites. These flies typically thrive near fast-moving water sources, giving the disease its colloquial name. Inside the human body, the worms reproduce, releasing countless larvae known as microfilariae that invade the skin and eyes, leading to severe complications.
The death of microfilariae releases a potent toxin, triggering intense itching and eye damage that can result in permanent blindness and severe skin conditions. In certain West African regions, nearly half of the male population over 40 once suffered blindness due to this disease.
Having never visited Africa, Latin America, or other high-risk areas, it was confirmed that my vision loss was not caused by Onchocerciasis. The doctor moved on to the next potential cause.
6. Lead Poisoning

'Have you been exposed to old pipes, paint, or consumed non-fresh water?' was the next question aimed at identifying potential lead exposure.
Asking someone if they’ve been consuming paint chips is hardly a tactful question, yet it’s one that had to be considered.
Doctors needed to eliminate the possibility of lead poisoning, a condition that not only impairs brain function but also wreaks havoc on the nervous system, including the optic nerve responsible for sending visual information to the brain.
Lead poisoning can manifest through various visual disturbances, such as trouble seeing in dim light, blurred vision, and persistent eye discomfort. It also heightens the risk of cataracts, though this was unlikely for someone in their early 20s like me.
The ongoing crisis in Flint, Michigan, highlights how prevalent lead poisoning remains despite being entirely preventable. Historically, lead was used in numerous everyday items like gasoline, paint, art supplies, and plumbing, which explains the doctor’s unsettling query about pipe exposure. Thankfully, widespread lead contamination is uncommon in developed countries.
5. Nonarteritic Anterior Ischemic Optic Neuropathy
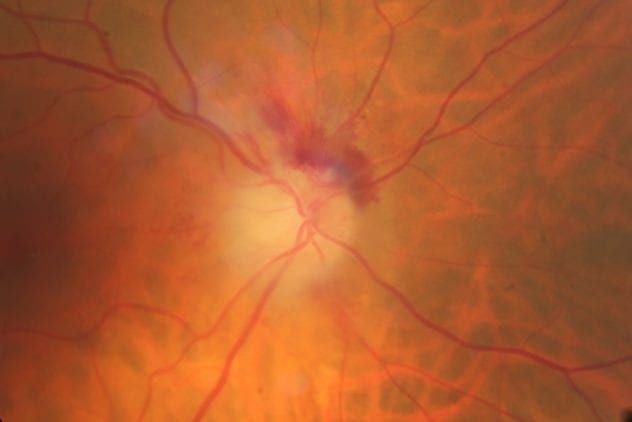
… is a frighteningly complex term for what is essentially an 'ocular stroke.'
An ocular stroke happens when the optic nerve suffers a sudden, significant drop in blood flow, leading to oxygen deprivation. This can occur as part of a broader stroke affecting multiple body systems or as an isolated incident impacting only vision.
Similar to conventional strokes, ocular strokes range widely in intensity. This condition affects roughly 1 in 10,000 people, including Frank Bruni, a well-known New York Times columnist. In February 2018, Bruni shared his experience in a moving article titled 'Am I Going Blind?'
The opening of Bruni’s piece vividly captures the sudden, terrifying nature of the disorder: 'They say death arrives like a thief in the night,' he writes. 'Lesser intruders follow the same pattern. The condition that robbed me of my vision, or at least a significant portion of it, struck as I slept. I went to bed with one view of the world and woke up to a completely different one.'
Bruni likens his vision loss to 'a dense, patchy fog' obscuring the right side of his sight, causing not just severe blurriness but also a disorienting sensation that made him feel 'intoxicated without having consumed alcohol.'
Individuals who experience an ocular stroke not only deal with vision impairment but also carry a persistent fear of recurrence, as one incident significantly increases the risk of another. Bruni revealed that, within the next five years, he faced a 20% chance of a similar event occurring in his unaffected eye, meaning a one in five probability of near-total blindness.
The nature of my vision loss didn’t align with the typical signs of a stroke. Although it remained a potential diagnosis, doctors continued to explore other, more plausible causes.
4. Devic’s Disease
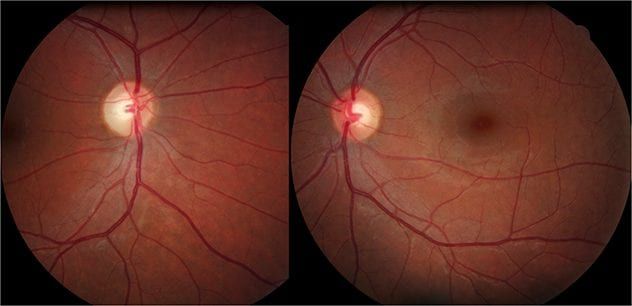
Among the conditions that closely matched my visual symptoms, one stood out as particularly alarming and daunting.
Neuromyelitis optica, or Devic’s Disease, can be likened to an intensified version of multiple sclerosis. While MS usually targets one eye with optic neuritis—periodic attacks on the optic nerve—Devic’s Disease often causes significant blind spots in both eyes simultaneously.
My vision impairment affected both eyes, and a neuro-ophthalmologist noted that my optic nerves were thinner than average. In simpler terms, while my eyes themselves were functioning properly, the connections were damaged, causing significant distortion in what I could see.
Devic’s Disease is, in a word, devastating. Similar to MS, it involves immune system attacks on the optic nerves and spinal cord. However, unlike MS, Devic’s often causes sudden and severe loss of vision and mobility, following a relapse-remission pattern that is more aggressive and debilitating. Symptoms can range from blindness in one or both eyes to limb weakness, paralysis, painful spasms, numbness, uncontrollable vomiting, and issues with bladder or bowel control, depending on which areas of the nervous system are affected.
An MRI of my spine yielded inconclusive results. The subsequent step, a spinal tap, was far more uncomfortable and invasive.
The spinal fluid analysis showed no abnormalities, ruling out MS or Devic’s Disease—at least for the time being. The investigation into the cause of my symptoms continued.
3. Dominant Optic Atrophy
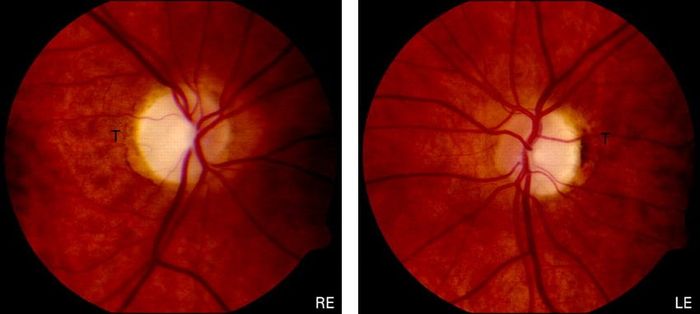
After nearly two years of uncertainty, doctors reached a tentative diagnosis through elimination: Dominant Optic Atrophy.
Often abbreviated as DOA, Dominant Optic Atrophy is a somewhat ambiguous condition marked by the deterioration of the optic nerves. The term 'dominant' refers to its genetic inheritance, a key clue for doctors since my father has experienced mild optic neuritis (inflammation of the optic nerves).
DOA typically manifests in the first ten years of life, with those affected often experiencing moderate vision impairment and color vision deficiencies. The severity varies widely—a common trait among eye disorders that complicates diagnosis—with visual acuity ranging from nearly normal to legally blind (20/200 or worse, even with correction).
Dominant Optic Atrophy remains somewhat enigmatic: it can result from mutations in various genes, some of which are still unidentified. Like many eye conditions, there is currently no prevention or cure.
DOA also carries a 'Sword of Damocles' quality, as it can halt and resume unpredictably. Fortunately, it has been over 15 years since I experienced any noticeable vision loss. However, the possibility of further deterioration will linger in my mind, much like the condition itself, for the rest of my life.
2. Leber’s Syndrome
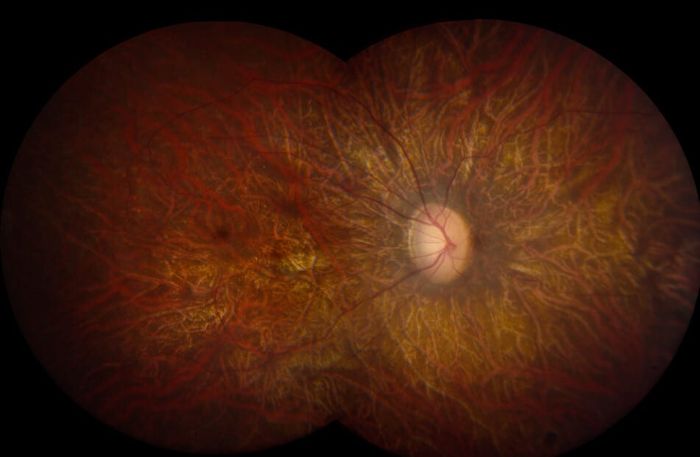
Leber Hereditary Optic Neuropathy, commonly known as Leber’s Syndrome, is a mitochondrial condition that causes the degeneration of retinal ganglion cells and their axons—long, threadlike nerve cells connected to the optic nerve. Although it predominantly affects young men, LHON is maternally inherited, as mitochondria are passed exclusively from the mother’s egg during conception.
Leber’s Syndrome typically begins with sudden vision loss in one eye, followed by the other eye within weeks. However, in 25% of cases, vision loss occurs in both eyes simultaneously. The condition progresses to severe optic atrophy, leading to permanent vision impairment.
During the acute phase, affected eyes show a fluid-like appearance in the nerve fiber layer and abnormalities in the peripapillary blood vessels. A pupillary defect may also develop as the eyes attempt to compensate for reduced light intake.
In addition to bilateral vision loss, I exhibited two other symptoms that closely matched Leber’s: diminished color vision and the specific placement of my scotomas (blind spots). Mine were cecocentral, meaning they expanded from the natural blind spot where the optic nerve meets the eye, growing significantly over time.
If I had been diagnosed with Leber’s Syndrome, I would likely be almost completely blind by now. Fortunately, that was not the case.
1. Coloboma of the Eye
The term 'coloboma,' derived from a Greek word meaning 'curtailed,' refers to a group of conditions where normal eye tissue is absent from birth. This can affect the macula, lens, uvea, optic nerve, or even the eyelids. The severity of visual impairment varies widely, from almost no symptoms to near-total blindness.
If confirmed, my condition would be a moderate case of optic nerve coloboma, characterized by an abnormal, hollowed-out optic pathway. Although present from birth, mild to moderate cases often go undetected until adolescence or early adulthood. As one doctor explained, 'You can only perceive the world through your own eyes.' My poor vision seemed normal to me until failing several eye exams revealed it was significantly worse than average.
The idea of a birth defect seemed plausible, given that my mother experienced preeclampsia—a condition causing dangerously high blood pressure—while pregnant with me. (Tragically, she passed away from it during her second pregnancy three years later.) Preeclampsia can restrict oxygen to the fetus, potentially leading to birth defects.
However, colobomas are more frequently genetic, and there was no indication of them being hereditary in my family. Without a definitive diagnostic test, this condition joined the list of potential diagnoses. It was a reassuring possibility, as colobomas generally do not progress over time.
