Medicine has advanced significantly from the days of garlic-infused masks and strong herbal teas. Even in more recent history, some drugs have had horrifying impacts on the human body. But—here's the important part—they still work, often surprisingly well. Back then, they were the best option, despite their deadly potential.
Today, the regulations imposed by today’s “Big Pharma” are far more rigorous than those in the early to mid-20th century. The drugs featured in this list come from the 12th edition of Grollman and Slaughter’s *Pharmacology and Therapeutics*, a fascinating compilation of strange and unusual old medications.
10. Metrazol

In 1926, F. Hildebrandt conducted experiments on animals with a new drug and discovered two major clinical effects. When administered in high doses, it induced convulsions similar to epilepsy. At lower doses, it acted as a stimulant, boosting heart rate and respiration, particularly in cases of depressant overdose (such as excessive chloroform).
Can you guess the primary use physicians found for it?
If your answer was “as an antidote to poisoning,” you’d be mistaken. (After all, we had pure stimulants for that purpose.) Instead, in 1934, scientist Ladislas J. Meduna introduced its use in humans to trigger convulsions as a treatment for mental illnesses.
Meduna’s main focus was schizophrenia, for which Metrazol became the first officially accepted treatment. However, its use in convulsive therapy also expanded to other psychiatric conditions, including depression. Patients typically received Metrazol in a hospital and waited for its quick effects, often being discharged within hours.
Metrazol was regarded as an effective therapy for psychoses lasting less than three years. Though the side effects were initially minimal, they could be dreadful, including spinal fractures, tuberculosis, and brain damage. Fortunately, Metrazol fell out of favor swiftly and was replaced by the “more efficient” electroconvulsive therapy, which came with fewer physical side effects.
Although Metrazol is notorious for its unsettling effects, it remains in use today, but not within hospitals. Instead, it is employed in laboratories to provoke convulsions or anxiety in rodents for the purpose of testing potential treatments for similar conditions. Recently, there has been a surge of interest in its possible application for Down syndrome, though it is not anticipated to provide a cure.
9. Tribromoethanol

Tribromoethanol, as suggested by the 'ethanol' in its name, shares a connection with the beverage alcohol. While it has comparable effects, it is significantly more potent and carries a wider spectrum of potential side effects. Cushny’s updated work mentions that Willstätter first synthesized it in 1923, with Duisberg later using it as an anesthetic in 1926.
Rectal administration proves to be highly effective. Within just 10 minutes, half of the dose is absorbed, and 95 percent of it is absorbed within 25 minutes. The result is predictable: a deep sleep that typically lasts around two and a half hours.
The one major issue, however, was that it was nearly impossible to alter the hypnotic state once induced. No known drug at the time could reverse the effect. As a result, tribromoethanol was rarely used because it was far too difficult to control.
Other adverse effects included damage to the circulatory system, liver and kidney degeneration, a reduction in metabolic rate (about 15 percent slower), depletion of glycogen reserves, elevated blood sugar levels, and in some cases, even death.
Today, there are no significant clinical uses for the drug. Instead, it is primarily employed to sedate mice in laboratory settings.
8. Bulbocapnine

This intriguing substance was infamously used in the MKUltra program. Structurally similar to apomorphine, bulbocapnine is derived from Corydalis cava. It is one of those fascinating compounds that produces different effects across species. In cold-blooded animals, it mimics morphine by dulling pain sensitivity and causing sedation.
However, in warm-blooded creatures, bulbocapnine induces catalepsy, which is a condition where the muscles stiffen in a fixed posture, and the individual cannot move. The subject becomes immobile.
The condition becomes more pronounced in higher-order animals (humans, apes, dogs, etc.). Additionally, the greater the dose, the more likely narcolepsy will occur. In many instances, bulbocapnine stimulates the intestines, prompting defecation, and triggers the secretion of saliva. Interestingly, this effect only happens in neutered animals.
Fortunately, small doses around 0.1 mg can be tolerated without significant adverse effects. However, bulbocapnine has little to no positive clinical applications. Instead, it is primarily used in laboratory research and in notorious government interrogation programs. Currently, it is being studied for its possible role in treating Alzheimer’s disease.
7. Picrotoxin

A drug is bound to be interesting when it carries the word “toxin” in its name. Picrotoxin is derived from the Anamirta cocculus plant. The symptoms of its use were well-documented but appeared with a delay.
The initial signs of poisoning included vomiting, excessive salivation, rapid breathing, and a slowed heart rate accompanied by palpitations. This was followed by unconsciousness and violent seizures, often paired with respiratory paralysis that would stop after a few moments. Well, most of the time. In some cases, patients succumbed to asphyxia when they were unable to restart their breathing.
Despite its dangerous reputation, picrotoxin has practical uses. It was traditionally employed to treat barbiturate poisoning because it stimulates anesthetized patients. It is thought that picrotoxin works by competing with the neurotransmitters that barbiturates typically target.
Oddly enough, comatose patients can often withstand doses far exceeding the lethal limit without suffering any adverse effects. In most cases, picrotoxin is administered in doses of 1–3 mg at regular intervals. The lethal dose can be as little as 0.357 mg/kg, or 28 mg for someone weighing 80 kilograms (176 pounds).
Interestingly, some comatose patients have received as much as 300 mg over the span of one or two days without any ill effects. In one documented instance, a total of 2.134 grams given over eight days was nonfatal.
6. Thymol

Thymol, a compound derived from the thyme herb, is one that you might recognize, as it is an ingredient in the toothpaste product Euthymol. Traditionally, it has been used to treat infections such as tinea, ringworm, and hookworm in humans.
However, when ingested to treat ringworm, thymol can cause some disturbing side effects. As with most poisons, there are the usual symptoms like nausea, vomiting, and headaches. More alarming effects include profound depression, unexpected giddiness, eventual collapse, and potentially death. The crucial factor is the dosage: 1–2 grams every few hours, followed by a saline purge and bowel evacuation, is typically both effective and safe.
For conditions like tinea and ringworm, thymol is usually mixed in a 1:10 ratio with alcohol and applied directly to the skin. This preparation gradually eliminates the infection, largely due to thymol's potent antimicrobial properties. (This explains its presence in toothpaste.)
That said, thyme isn’t the most powerful of the antimicrobial spices. When ranking herbs by their ability to combat microbes, oregano, clove, coriander, and cinnamon all come before thyme. So, if you're thinking of boosting your immunity with a spicy lunch, a carrot and coriander soup would be a better choice than a cinnamon latte.
5. Isonipecaine

Isonipecaine, developed by Eisted and Schaumann in 1939 as part of the quest for opioid-like painkillers, is perhaps more widely recognized by its alternative name, pethidine. It is commonly used today as a painkiller, especially in maternity wards for women in labor.
While isonipecaine is an effective painkiller with mild respiratory depression (in contrast to morphine) and reduced vomiting reflex, it is also known for its high euphoria rates (up to 90 percent) and the potential for addiction if used long-term.
Overall, its side effects are significantly less severe than those of morphine or other natural opiates. Isonipecaine has minimal impact on respiration, circulation, or metabolic processes.
Unfortunately, isonipecaine has a short duration of action, peaking in 45 minutes and lasting only around two hours. It is also less potent than a standard initial dose of morphine. Furthermore, modern research has revealed that isonipecaine is just as addictive as previously claimed, despite earlier assumptions about its lower addiction potential.
Isonipecaine is highly toxic in overdose situations. If administered in large doses over a short period (3-4 hours), it can cause disorientation, rapid heart rate, and severe respiratory depression.
The use of isonipecaine in labor is well recognized. It has a milder effect on respiration compared to morphine or diamorphine, making it a safer choice for both the infant and the mother.
Isonipecaine also affects smooth muscles, which gives it muscle relaxant properties. This can be beneficial in alleviating tension and pain during contractions. However, the drug does delay labor and impacts the baby.
4. Intocostrin
In addition to Metrazol, another essential drug used in electroconvulsive therapy was introcostrin.
It's interesting to note that introcostrin is derived from curare, a substance historically used by indigenous South Americans to poison the tips of their arrows for hunting. Curare effectively paralyzes all voluntary movements.
As described by Cushny et al.: 'The muscles give way one after another until the animal collapses, completely immobilized... and becomes entirely paralyzed.'
Over time, the poison causes suffocation as the respiratory system fails. Essentially, this results in a fatal version of locked-in syndrome. A curious fact: ingesting it orally is mostly harmless, so you can suck out the poison from a wound and still have a chance to survive.
Curare has limited medicinal use. It only becomes effective when administered in a dose high enough to relax muscles but not impair breathing. This delicate balance is often avoided in favor of intocostrin.
Intocostrin, being easier to control and dose, was primarily used to help patients undergoing convulsive or electroconvulsive therapy. The drug eased the intensity of violent convulsions, which was believed to lower the risk of spinal fractures—a serious concern for such patients. It also helped to alleviate spasms and was used as an adjunct to anesthesia.
3. Santonin
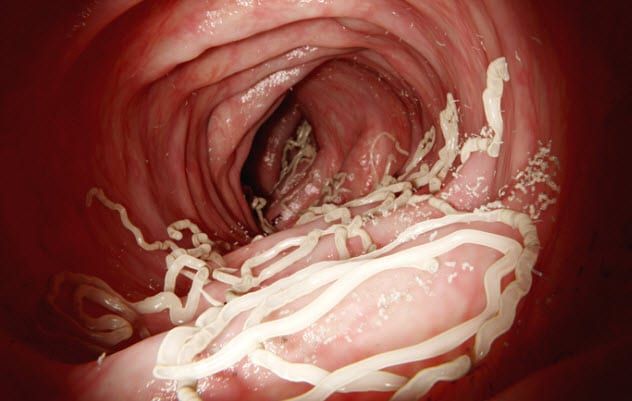
Santonin, a bitter-tasting drug developed in the early 1800s, was once the go-to remedy for treating roundworms and pinworms before being superseded by safer alternatives. It remained in use for a while longer as a treatment for whipworm but was entirely ineffective against tapeworms.
The side effects of santonin were both unpleasant and oddly amusing. For instance, patients noted a change in their vision—not necessarily negative, but everything began to appear with a blue hue.
This effect was short-lived before another visual anomaly took over. Bright objects appeared to have glowing yellow halos, blue turned into green, and the previously blue hues darkened progressively until they became indistinguishable from black. The more santonin ingested, the more vivid and intense these visual effects became.
Additionally, patients suffered from nausea, vomiting, and occasional confusion. Higher doses could trigger convulsions, with the risk of asphyxia. The drug was expelled from the body in nearly every conceivable way: in the feces with the expelled worms, in urine that turned a striking neon yellow, and even in sweat, which took on a yellowish tint.
The way in which santonin eliminates parasites can be summed up succinctly: It takes care of them before it takes care of you.
2. Ergot

Ergot is a notorious fungus that thrives on rye and other grains such as wheat. This fungus is infamous for causing ergotism, also known as 'St. Anthony’s Fire,' a gangrenous condition. The symptoms, which include delirium and psychosis, may have played a role in the witch hunts during the Middle Ages.
Despite its dark reputation, ergot still has valuable medical uses. It is highly effective in inducing uterine contractions, facilitating labor, or even causing abortions.
However, it is important that ergot be administered only after the second stage of labor, once the placenta has been expelled, to avoid the risk of suffocating the baby. When used at this stage, ergot helps reduce bleeding and prevents postpartum hemorrhaging.
Ergot was once believed to be effective in treating all types of internal bleeding because it causes blood vessels to contract, reducing hemorrhaging. However, prolonged use can quickly result in gangrene. Despite these risks, ergot or one of its derivatives may still prove beneficial in treating parkinsonism.
1. Dinitrophenol

Dinitrophenol is one of those drugs that seemed like a brilliant idea at first, but soon revealed serious complications. It was originally discovered during World War I when munitions workers died from exposure to the chemical. You’d think that would have ended its use, but the drug was quickly studied to see if there were any possible medical applications.
When administered at a dose of 3–5 mg per kilogram of body weight, dinitrophenol was found to boost metabolism by 20–30 percent for several days due to an increase in oxygen consumption. This made it look like a promising solution for obesity.
However, as the dosage increased, side effects began to emerge, such as excessive sweating and a rise in body temperature by as much as 3 degrees Celsius (5.4°F). In toxic amounts, these effects were followed by other symptoms, including rapid breathing.
The increasing oxygen demand in this particular case meant that the patient’s respiratory system was unable to meet the body’s oxygen needs. Hypoxia could emerge along with a fever reaching as high as 43°C (109°F) or beyond—and that’s just the beginning. Common side effects, even with standard doses, included various internal and external conditions that could easily lead to death.
Once briefly used to treat obesity, dinitrophenol quickly became unpopular due to its dangerous long-term effects and its potential to trigger fatal conditions. Today, its main use is as a pesticide or as an ingredient in a highly explosive mixture known as shellite.
