Health experts emphasize that another global epidemic of a lethal illness is inevitable. Authorities predict a high likelihood of a rapidly spreading pathogen causing a worldwide crisis within the next decade and a half.
Nearly 100 years have passed since the 1918 Spanish flu pandemic, which took millions of lives. This devastating illness affected more than 500 million individuals and led to tens of millions of fatalities. Despite significant progress in medical science and technology over the past century, the threat of a similar outbreak remains very real. Below are ten reasons why another catastrophic pandemic could be just around the corner.
10. Rising Global Population

At the time of the 1918 Spanish flu, the world's population was under two billion. The pandemic wiped out roughly 2.5% of the global population, equating to about 50 million deaths. With the current global population at 7.6 billion, a similar outbreak today could lead to approximately 190 million fatalities.
Rapid population growth accelerates the transmission of infectious diseases. As more individuals inhabit the same regions, human interaction increases, creating more opportunities for diseases to propagate.
Over half of the global population resides in urban areas, and this figure is steadily rising. Infectious diseases can spread rapidly in large cities. Public transportation brings people into close proximity, living spaces are often overcrowded, and in many nations, densely populated regions include slums with unsanitary conditions that foster the proliferation and spread of harmful bacteria.
9. Antibiotic Resistance
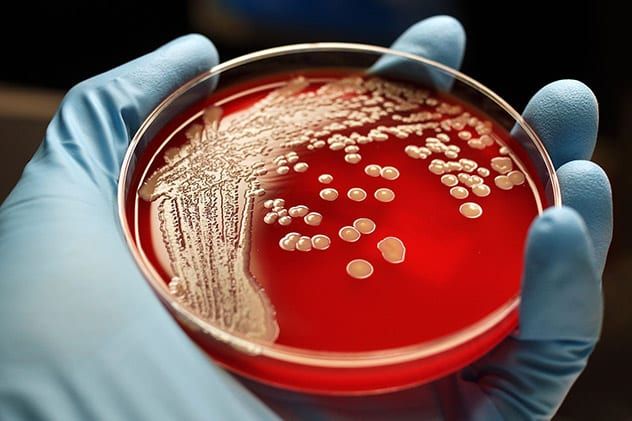
For decades, antibiotics have been the go-to solution for treating bacterial infections. However, their effectiveness is diminishing as bacteria evolve and develop resistance. Infections caused by antibiotic-resistant bacteria are increasingly challenging, and in some cases, untreatable. Tom Frieden, former CDC director, warned in 2014 that antibiotic-resistant bacteria could trigger the next global health crisis.
CRE, a group of carbapenem-resistant bacteria, poses a significant threat. Carbapenems are powerful antibiotics typically used to combat drug-resistant bacteria, but CRE strains defy even these. Earlier this year, the WHO identified 12 priority antibiotic-resistant bacteria, with the top three labeled as 'critical' due to their resistance to carbapenems. These pathogens are responsible for severe illnesses like pneumonia, bloodstream infections, and gonorrhea.
Without addressing the growing issue of antibiotic resistance, many currently treatable infections could become fatal. Sadly, pharmaceutical companies are reluctant to invest in developing new antibiotics due to the high costs of research and development and the limited profitability, as these drugs are typically used for short durations.
8. Ever-Changing Flu Strains

Health experts identify the flu virus as a prime candidate for triggering the next pandemic. However, this awareness does not translate into actionable measures to prevent it.
Predicting and preparing for the flu is notoriously difficult. The seasonal flu vaccine, the best available defense, is far from foolproof. Scientists develop the vaccine months before flu season begins, basing it on predictions of which strains will dominate. The vaccine's effectiveness fluctuates annually. For instance, during the 2015-2016 season, it protected about half of recipients, while in the 2014-2015 season, its effectiveness dropped to just 19%.
While only a few flu strains circulate globally, many more are believed to exist. Each strain undergoes annual mutations, with the extent of these changes determining the virus's threat level. Minor mutations can render the flu unrecognizable to the immune system, challenging vaccine developers. In some years, the flu mutates so significantly that it becomes almost a new virus, leading to pandemics like the 1918 Spanish flu.
7. Rise in Global Travel

Modern travel is faster, more frequent, and more accessible than ever before. With the ability to traverse the globe in a single day, diseases can now spread at an equally rapid pace.
Travel exposes individuals to unfamiliar diseases or new variants of known illnesses. Visitors to foreign regions may unknowingly introduce pathogens that local populations are ill-prepared to combat. For example, the 2014 Ebola outbreak devastated West Africa partly because the region had no prior exposure to the virus. Local healthcare systems lacked experience in treating the disease, and the population had no natural immunity from previous encounters.
Travelers often spend time in environments conducive to disease transmission, such as airplanes and hotels. These confined spaces bring people into close contact, facilitating the spread of germs. During the 2003 SARS outbreak, an infected Chinese doctor stayed at a Hong Kong hotel before succumbing to the illness. The virus spread to other hotel guests, who then carried it to various countries via air travel. Within five months, SARS had infected over 8,000 people across more than 30 nations, resulting in 774 fatalities.
As international travel grows, so does the potential for contagious diseases to spread across borders.
6. Deforestation

Around 75% of emerging infectious diseases are zoonotic, meaning they jump from animals to humans. As human-wildlife interactions increase, so does the likelihood of disease transmission. Deforestation exacerbates the spread of illnesses like Ebola and malaria by disrupting the habitats of animals that carry these pathogens. When their natural environments are destroyed, animals are driven closer to human settlements in search of food and shelter, heightening the risk of infection.
The link between deforestation and disease spread is well-documented.
A study in Peru during the late 1990s revealed that a malaria-carrying mosquito species in deforested areas bit humans nearly 300 times more often than those in undisturbed forests. Similarly, a 2010 study found that clearing just 4% of a Brazilian forest led to a 50% surge in malaria cases. Deforestation also triggered severe droughts in Brazil, prompting people to store water in open containers, which attracted mosquitoes and likely contributed to the Zika virus outbreak.
Mosquitoes aren't the only disease vectors impacted by deforestation. Primates, bats, and rodents also harbor pathogens that can infect humans. As long as human activities continue to encroach on animal habitats, the risk of new, highly contagious, and potentially untreatable diseases will persist.
5. Risks in Scientific Research

In 2014, researchers in the U.S. engineered a virus closely resembling the 1918 Spanish flu. Using reverse genetics, scientists at the University of Wisconsin – Madison reconstructed the virus from segments of avian flu strains found in wild birds. They further modified the virus to become airborne, a trait associated with the most lethal infectious diseases.
Proponents of the study argue that replicating such a dangerous virus is crucial for assessing its potential threat to humanity. However, many experts oppose these experiments, citing the inherent risks to public safety. Even in high-security laboratories, producing deadly pathogens is fraught with danger. Critics contend that there is little evidence these experiments save lives, while they undeniably endanger them. A Harvard School of Public Health professor cautioned that an accidental or intentional release of such a virus could trigger a devastating global pandemic.
4. World Health Organization's Role

The ability to respond swiftly to a highly contagious and rapidly spreading disease will determine the scale of lives lost. Public awareness and precautionary measures are essential, and the World Health Organization (WHO) serves as the primary global health monitor, responsible for issuing alerts during outbreaks. However, the WHO's track record raises concerns about its ability to act promptly in such crises.
The recent Ebola outbreak started in early 2014. However, the WHO did not declare it a public health emergency until August, five months after outbreaks were reported in Guinea and Liberia. An independent panel of global health experts criticized the delay, stating it led to unnecessary suffering and loss of life.
The WHO faced significant backlash for its sluggish response to the Ebola crisis. They pledged to enhance their systems to ensure faster and more effective reactions in the future. However, if they fail to act promptly during the next pandemic, the consequences could be irreversible by the time they acknowledge their delays.
3. Potential for a Current Pandemic

The H7N9 bird flu virus first infected humans in 2013, claiming the lives of two individuals in China. Since then, China has experienced annual outbreaks, with the fifth wave beginning in October 2016 being the most severe. This wave saw more cases than the previous four combined and affected the largest geographic area. The mortality rate for confirmed H7N9 cases is approximately 40%, with 1,622 confirmed cases and 619 deaths reported as of October 25, 2017.
The CDC identifies H7N9 as the flu strain with the highest pandemic potential. While most human infections have been linked to live poultry markets in China, the virus is continuously mutating. This raises concerns that it could soon evolve to spread efficiently between humans, significantly increasing the global threat.
A study conducted last year on a highly pathogenic strain of H7N9 involved ferrets, the preferred animal model for testing flu virus transmissibility in humans. Infected and healthy ferrets were placed in adjacent cages, and the virus spread easily, killing two out of three healthy ferrets. The study confirmed that the virus could be transmitted through airborne respiratory droplets, such as those produced by coughing or sneezing.
Given the significant mutations observed in H7N9 over the past year, the next wave of the virus could become highly contagious among humans and equally lethal. Currently, there is no effective vaccine available for the latest strains of H7N9.
2. Bioterrorism

The next global pandemic could stem from a deliberate act of bioterrorism.
Bill Gates, one of the world's wealthiest individuals, has dedicated the past two decades to funding global health initiatives. Earlier this year, at a security conference in Munich, Gates warned that bioterrorism—the intentional release of viruses or bacteria—could result in the deaths of millions.
The risk of bioterrorism has grown significantly over the past five years. Advances in molecular biology have simplified the creation of biological weapons, making them more accessible. Terrorists can now use genetic engineering to produce viruses like smallpox or engineer highly contagious and deadly flu strains. Intelligence reports indicate that ISIS has been developing bioweapons at their bases in Syria and Iraq.
1. Climate Change

Vector-borne diseases, which are transmitted to humans by organisms like fleas, ticks, and mosquitoes, are on the rise due to global warming. As the planet warms, the prevalence and geographic spread of these diseases have increased.
Mosquitoes, which thrive in warmer climates, are responsible for transmitting deadly diseases such as Malaria, Zika, and Dengue. Malaria, in particular, is the most lethal. Climate change expands the habitats of these insects, allowing them to breed in new regions and extending their active seasons, thereby increasing the risk of disease transmission to humans.
Fleas and ticks, which also flourish in warm environments, carry dangerous illnesses like Congo-Crimean haemorrhagic fever, typhus, and Lyme disease.
