Sleep is an extraordinary experience, but with over 100 known sleep disorders, many individuals struggle to get the quality rest they deserve. While some sleep disorders, like sleep apnea, sleepwalking, sleep talking, teeth grinding (bruxism), narcolepsy, and sleep paralysis, are fairly well-known, there are also less talked about yet equally troubling conditions. Here are a few more that might keep you awake at night.
10. Sleep State Misperception

We’ve all experienced those moments when we’re convinced we haven’t slept. You might be absolutely certain you’ve been awake the whole time, but you could be dealing with sleep state misperception, also known as paradoxical insomnia. This condition refers to individuals who either underestimate their sleep, thinking they’ve been awake, or overestimate it. People with this disorder often claim to have had little or no sleep, but a sleep study in a lab can reveal that their sleep patterns are actually within the normal range.
Sleep research has demonstrated that people are generally poor at accurately gauging the amount of sleep they actually get. Paradoxical insomnia typically affects young and middle-aged men and can lead to depression and anxiety. Treatment options such as sleep restriction therapy and medication can alleviate symptoms. Paradoxical insomnia accounts for approximately 5 percent of individuals seeking treatment for insomnia-related issues.
9. Sleep-Related Painful Erections

While experiencing erections during sleep is a normal and often pleasurable occurrence, some men suffer from intensely painful erections during the night. According to the Principles and Practices of Sleep Medicine, individuals with this disorder experience penile pain during REM sleep, typically affecting middle-aged or older men. These individuals often report frequent awakenings due to partial or full erections accompanied by significant pain, despite having a history of normal, painless erections while awake.
Some men with SRPE believe the condition is linked to inadequate sexual release, but even with regular intercourse or masturbation, these painful nocturnal erections can still occur. Persistent issues with this disorder can result in insomnia, anxiety, irritability, and excessive daytime sleepiness. Over time, the condition may worsen, and while no specific studies have been conducted on its effectiveness, medication has been known to alleviate symptoms for some patients.
8. Short and Long Sleepers

The average adult typically requires seven to eight hours of sleep each night to function well the following day. However, some individuals need 10 hours or more of sleep to feel fully rested, while others can thrive on just five hours. Long sleepers may manage with nine hours of sleep during the workweek, but they often extend their sleep to 12–15 hours on weekends or holidays to recharge.
Research indicates that long sleepers make up only about 2 percent of the population, and they are somewhat more likely to be male. While there is generally nothing medically wrong with long sleepers, they may have a higher risk of experiencing depression and anxiety. Short sleepers, on the other hand, are often male as well and generally have normal personalities, though they may occasionally exhibit hypomanic tendencies.
Despite having the opportunity to sleep more, short sleepers typically maintain their usual five hours of sleep, even on weekends. Both short and long sleepers represent the extremes of typical sleep patterns. These conditions are rare, but they often run in families. Studies suggest that short sleepers tend to die earlier than long sleepers, despite engaging in similar levels of physical activity.
7. Cataplexy

Have you ever laughed so hard or been so frightened that you suddenly lose the ability to move? While this is rare for most people, those with cataplexy experience this phenomenon regularly. When individuals with cataplexy experience strong emotions—whether positive, like joy or laughter, or negative, such as anger or fear—they may lose muscle tone and sometimes seem as though they've fallen asleep. Laughter is typically the most significant trigger for these episodes.
Cataplectic attacks can range in severity, from minor muscle weakness to a complete loss of muscle tone, causing the person to collapse. Many individuals with narcolepsy, a condition characterized by excessive sleepiness and occasional sleep attacks, also experience cataplexy. During these episodes, a person may be unable to move and, if they also have narcolepsy, may even fall asleep. Most cataplectic attacks last only a few minutes and can usually be managed with medication.
6. Nocturnal Sleep-Related Eating Disorder

Most of us have gotten up for a midnight snack at some point, but for some individuals, this habit becomes an extreme. This condition is different from nocturnal eating syndrome (NES), where people binge eat during the night. Those with nocturnal sleep-related eating disorder (NSRED or SRED) are unaware that they are eating while asleep.
Individuals with NSRED may consume a variety of unusual items such as sweets, drinks, raw or spoiled food, glue, wood, and even cigarette butts. They often handle food carelessly, sometimes injuring themselves while cutting or opening cans. Rapid weight gain can occur over a short period, and many with NSRED struggle with obesity. While some medications have helped manage the disorder, they are not universally effective. Certain drugs, like Ambien, can trigger SRED episodes, and life stressors such as divorce or drug abuse can also contribute to the condition.
5. Rhythmic Movement Disorder

It can be distressing for a parent to witness their child repeatedly bang their head against the mattress or headboard while attempting to fall asleep. Children with rhythmic movement disorder (RMD) may engage in activities like head-banging, rocking their bodies, humming, or rolling their heads and bodies during the process of falling asleep. Usually, they are unaware of their actions. These rhythmic movements can occur when the child is drifting off to sleep and may continue or reappear during deeper sleep stages.
These movements are typically observed when the child is lying on their back or stomach, although they can also occur while the child is sitting upright. RMD can sometimes be associated with developmental conditions like autism. It can manifest at any age but is most commonly seen in infants and toddlers. In many cases, it fades as the child grows older and rarely requires medical intervention. For children with more violent movements, padding the bed or crib can help prevent injury.
4. Hypnogogic Arousals

Also referred to as sleep starts or hypnic jerks, these are involuntary movements such as jerks, jumps, or sensations of falling that occur just as a person is about to fall asleep. The sensation of the jerk can be strong enough to cause someone to suddenly wake up and may make it difficult to fall back asleep due to anxiety about experiencing another hypnogogic arousal.
People with irregular sleep schedules, high caffeine consumption, or significant stress in their lives are more likely to experience sleep starts, though 60-70% of people report having at least one. This condition is quite common and generally doesn’t require medical treatment. It's often recommended to reduce stress, cut down on caffeine, and get more sleep to reduce episodes. While experts haven’t yet figured out why sleep starts occur, some believe it could be an evolutionary trait. It may also be linked to other sleep disorders like sleep apnea.
3. Central Sleep Apnea
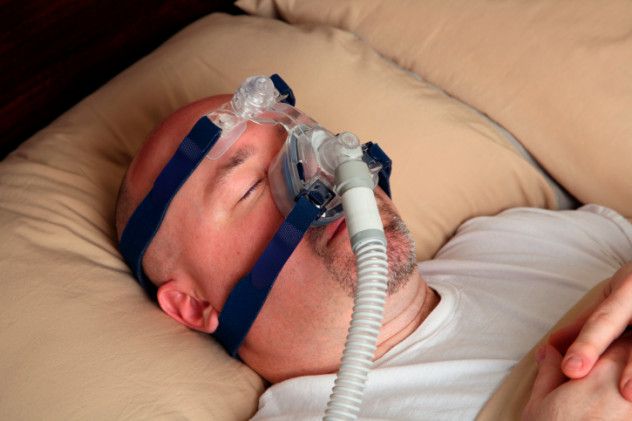
Many people aren’t aware that there are different types of sleep apnea. The most common type is obstructive sleep apnea, where the airway becomes blocked. In central sleep apnea, the brain fails to send a signal to breathe, causing the person to stop breathing. This can happen to individuals who have misused pain medications, suffered head injuries from accidents or strokes, or those with kidney or heart diseases.
While treatment for obstructive sleep apnea typically involves using a CPAP (continuous positive airway pressure) machine, those with central sleep apnea may require a different kind of therapy. This could include BiPAP (which uses different pressures for inhalation and exhalation) or an adaptive servo-ventilation (ASV) machine, which helps maintain regular breathing. Central sleep apnea can be just as dangerous as obstructive sleep apnea, leading to issues like obesity, diabetes, stroke, and even cardiac arrest.
2. Delayed And Advanced Sleep Phase Disorders

Individuals with delayed sleep phase disorder (DSPD) and advanced phase sleep disorder (APSD) are present in many walks of life, often among teenagers and older adults. DSPD is more commonly found in teenagers, whose internal clocks tend to delay their bedtime. Some with DSPD may stay awake for two to four hours before finally falling asleep and often have trouble getting up in the morning. This lack of rest is generally due to staying up late and poor sleep habits. Teenagers, especially, are prone to late-night habits, exacerbated by cell phone use, which prevents them from getting the sleep they need to function properly the next day. It’s no surprise that many individuals with DSPD identify as “night owls.”
In contrast, ASPD typically affects people over the age of 60. Those with ASPD often go to bed much earlier, usually between 6:00 PM and 8:00 PM, and wake up very early, typically between 1:00 AM and 3:00 AM, though never later than 5:00 AM. Mild ASPD is often a natural part of aging, and daytime napping is common among those affected. Individuals with ASPD often consider themselves “early birds.”
1. Alcohol-Dependent Sleep Disorder

Many of us have enjoyed a drink or two to help us wind down at night, but for some, alcohol use as a sleep aid goes beyond occasional use. Individuals with alcohol-dependent sleep disorder rely on alcohol as a sedative to help them fall asleep every night for over a month. While this behavior might seem like a sign of alcoholism, it is not always associated with full-blown alcohol dependency.
Over time, the disorder can lead to alcoholism, as the body becomes accustomed to alcohol for sleep. The initial sedative effects of alcohol wear off, prompting individuals to increase their consumption, which raises their risk of developing a full-blown alcohol addiction. Those with alcohol-dependent sleep disorder often experience interrupted sleep, sweating, headaches, dehydration, and mild withdrawal symptoms. When trying to quit using alcohol to fall asleep, many individuals find it extremely challenging to sleep without their nightly drink.
