Variant Creutzfeldt-Jakob disease (vCJD), the human counterpart of mad cow disease, is an exceptionally rare and chilling illness. Despite ongoing research, scientists still have limited understanding of this condition.
What has been discovered, however, is both intriguing and has prompted stricter regulations in the beef industry. For example, the US Department of Agriculture mandates the removal of all brain and spinal cord materials from cattle deemed to be at high risk. These materials are not allowed in the US food supply.
Even so, the facts surrounding the human form of mad cow disease remain deeply unsettling.
10. It Is A Prion Disease

Prion diseases, also known as transmissible spongiform encephalopathies, are uncommon brain disorders that alter the brain’s structure and can be passed between organisms. These diseases occur in both humans and animals, and vCJD is among the most fatal human types of prion disease.
Humans possess prion proteins in their brains, but scientists have not yet fully figured out their precise role. In vCJD, these normal prion proteins are impacted by an infected prion that enters the victim’s body.
The infected prion attaches to the prion proteins in the victim's brain, changing them into an abnormal shape. These altered prions then destroy brain cells and create holes in brain tissue, giving the brain a spongy appearance. As more prions become infected, the victim experiences further brain damage and a range of psychiatric symptoms.
9. It is transmitted directly from cows
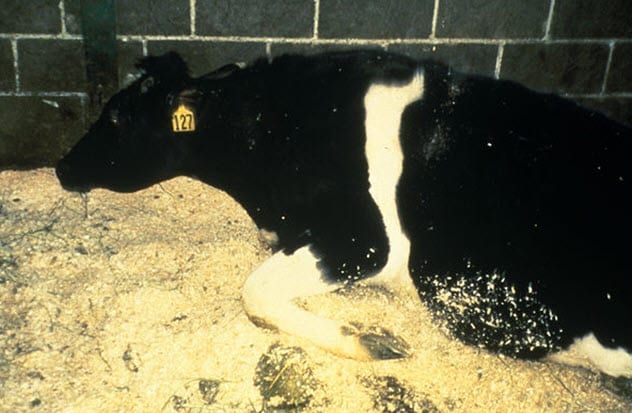
Humans typically acquire the abnormal prion responsible for vCJD through consumption of beef from a cow infected with bovine spongiform encephalopathy (BSE), commonly known as mad cow disease. The prion responsible for BSE in cattle mirrors the one causing vCJD in humans.
The origins of mad cow disease remain unclear, but it is thought to have emerged when cows were fed cattle feed contaminated with meat from sheep infected with scrapie, another prion disease. Researchers believe mad cow disease initially spread in the UK when infected cattle meat was fed to calves. The connection between vCJD and mad cow disease was confirmed after the first cases of vCJD appeared in the UK, where mad cow disease began.
Between 1984 and 1986, UK citizens were most at risk of consuming infected meat. The initial cases of vCJD were recorded between 1994 and 1996, which aligns with the average 10-year incubation period for the prion in both cattle and humans.
In rare instances, vCJD has been contracted through a blood transfusion from an infected individual. However, the majority of cases are due to consumption of meat from cattle affected by mad cow disease.
8. It Represents A Manifestation of A Broader Condition

vCJD is a particular variant of the broader condition known as Creutzfeldt-Jakob disease (CJD). CJD is a disorder triggered by an infectious prion, a protein capable of transferring its abnormal form. This disease is divided into four subtypes, each defined by the method in which the prion is transmitted to humans. vCJD is one such form, while the other three share similar characteristics except for the transmission method.
The most prevalent type of CJD is sporadic Creutzfeldt-Jakob disease (sCJD), though its origins remain elusive. In sCJD, a normal prion protein in the brain of the afflicted individual undergoes a spontaneous transformation into an infectious version. While the precise cause of sCJD is not fully understood, researchers suggest that it may be more frequent in those possessing a specific genetic variation of the prion protein.
Familial CJD is the third form, which arises when an individual inherits a genetic mutation leading to the production of malformed prion proteins. The onset of symptoms typically occurs after the age of 50, which means that parents carrying this genetic mutation may not be aware of it when deciding to have children.
The rarest type of CJD is iatrogenic CJD, which occurs when medical equipment that has not been thoroughly sterilized after being used on a vCJD patient is then reused on another individual, transmitting the infected prion.
Given that all four of these alarming diseases fall under the umbrella of CJD, many experts consider Creutzfeldt-Jakob disease to be one of the most destructive brain conditions known to humanity.
7. It Gave Rise to Another Disease
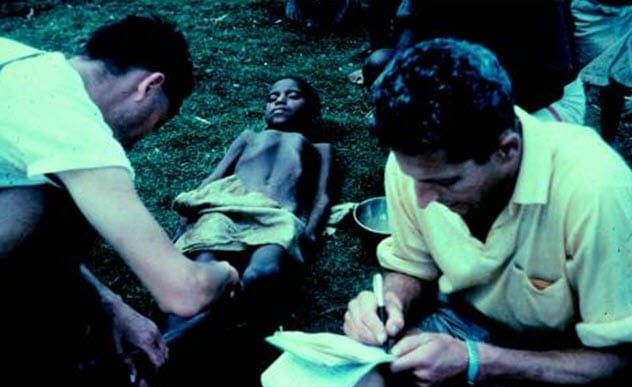
Kuru is another frightening prion disease that spread among the tribal regions of Papua New Guinea. The condition was prevalent in tribes that practiced a form of ritual cannibalism, consuming the brains of deceased family members as an act of reverence.
Though the tribes ceased this practice in the early 1960s, kuru cases persisted due to the disease's lengthy incubation period (at least 10 years). Interestingly, the changes that occur in the brain of a kuru patient are similar to those seen in individuals with vCJD, as both conditions result in the formation of misshapen prions that begin to infect brain proteins.
In their investigation, scientists uncovered that the practice of cannibalism led to prion abnormalities, and they proposed an astonishing hypothesis: the disease kuru stemmed from tribe members consuming the brain of someone afflicted with Creutzfeldt-Jakob disease (CJD). Through comparing kuru prions with those found in all four variants of CJD, researchers confirmed that kuru prions share transmission properties akin to those in CJD.
This suggests that a tribe member in Papua New Guinea who passed away had CJD without anyone being aware. As a result, their brain was consumed, giving rise to a new prion disease. Although scientists have not yet identified the exact form of CJD that affected the deceased tribe member, there's a strong likelihood it was vCJD.
Papua New Guinea has an abundant cattle population with minimal health regulations or controls, which may have led to the tribes consuming cattle infected with mad cow disease.
6. No Effective Treatment Is Available

Sadly, there is no cure for vCJD. Those afflicted with the disease typically live for only about 13 months after the onset of the first symptoms. Although various drugs, such as amantadine and pentosan polysulphate, have been tested on vCJD patients, none have consistently shown positive results.
Despite this, some medications have provided relief to certain individuals with vCJD. For example, in one case, a 22-year-old patient who was treated with pentosan polysulphate (a drug designed to slow the deterioration of brain cells) managed to survive for 51 months after showing the first signs of the disease.
This survival period is significantly longer than the typical 13 months, suggesting that this treatment may offer promise for more patients, pending further studies. However, at present, the focus of treatment remains on ensuring patient comfort and managing the symptoms of vCJD.
5. The Disease Induces Severe Psychiatric Symptoms

The symptoms of vCJD are largely similar to those seen in other forms of CJD. This is because the same abnormal prion is responsible for all the variations; the only distinction lies in the method of transmission between them.
As the vCJD prion damages the brain cells of the patient, it triggers a range of neurological symptoms. Initially, the patient may struggle with muscle coordination, experiencing involuntary jerking movements and muscle spasms.
As the brain continues to deteriorate, the patient may suffer from various symptoms, including hallucinations, memory loss, and even blindness in some cases. Within a year of the first symptoms, the patient will lose the ability to speak or move and may slip into a coma. During this time, many patients develop pneumonia or other infections, which are often the cause of death.
While the symptoms of vCJD bear similarities to other forms of CJD, it is distinct in that it primarily affects younger individuals. The average age of a vCJD victim is 28, whereas sporadic and inherited forms of CJD typically affect older adults, particularly those in middle age or the elderly.
4. Diagnosis Can Only Be Confirmed Posthumously

Given the rarity of vCJD, diagnosing it can be extremely difficult for doctors. If CJD is suspected, the initial step involves conducting routine tests to rule out more common mental disorders. These tests, including spinal taps and MRIs, help identify abnormalities that are typically associated with CJD.
The only reliable method to confirm a CJD diagnosis is through a brain biopsy or autopsy. While a biopsy can be performed while the patient is alive, it is generally not advised for CJD patients due to its potential risks and the fact that it does not always retrieve tissue from the areas of the brain affected by the disease.
Unless a person with CJD is willing to risk undergoing a biopsy, the diagnosis can only be confirmed after the patient's death through an autopsy. Fortunately, scientists are working on new tests that could make it possible to diagnose CJD while the patient is still alive.
For example, the National Institute of Neurological Disorders and Stroke has developed a diagnostic test that looks for a specific protein in the brain that causes nerve degeneration. The test works by analyzing the patient's spinal fluid. With further research, this method could lead to a way to definitively diagnose CJD before the patient passes away.
3. Awareness of the Disease is Growing
Thankfully, both the US and UK have taken important measures to prevent the spread of vCJD. For example, strict regulations have been implemented to ensure that meat from cattle infected with mad cow disease does not enter the human food supply. These regulations include banning certain animal feed and conducting BSE testing on all cattle over 30 months old, as mad cow disease is rare in cattle younger than 30 months.
The Centers for Disease Control and Prevention (CDC) in the United States has implemented various measures to track the spread of vCJD. They examine all CJD cases within the country, analyzing them in an attempt to detect any patterns that could assist researchers in developing new treatments.
In 1997, the CDC established the National Prion Disease Pathology Surveillance Center, which conducts in-depth tests, including brain autopsies, on prion diseases. While vCJD and other forms of CJD have not been eliminated, these efforts by scientists and healthcare professionals have helped reduce the disease's impact.
2. The Disease Has Global Reach

Even though vCJD is a rare disease, it has spread beyond the UK in the last few decades. Of the confirmed cases of vCJD, 178 have been reported in the UK, and four in the US. The remaining 49 cases have been recorded across 10 different countries.
As of 2017, France has reported the highest number of cases with 27, followed by Spain with five, Ireland with four, and three cases each from the Netherlands and Italy. Portugal and Canada have two cases each, and Japan, Saudi Arabia, and Taiwan have one case each.
While the UK currently has the largest number of vCJD cases, this may not remain the case for long. The peak of vCJD cases in the UK occurred in 1999, and the number has been steadily decreasing since then. However, other countries seem to be experiencing the opposite trend.
Despite the UK having a significantly higher number of vCJD cases, Portugal has recently seen a rise in its vCJD rate compared to the number of mad cow–infected cattle. This suggests that Portugal's cattle may have been more frequently contaminated, leading to higher human infections. If the UK's infection rate continues to decline, Portugal might eventually surpass the UK in confirmed cases.
1. A Highly Rare Disease

Globally, CJD affects about three individuals per million people, which already classifies it as an incredibly rare disease. However, this includes all forms of CJD, and vCJD constitutes less than 20 percent of those cases. Since its identification in 1996, only 231 vCJD cases have been reported.
Of the 231 known cases of vCJD, 178 are from the UK, which is expected given that mad cow disease originated there. In the US, only four vCJD cases have been documented. Two of these cases involved individuals who contracted the prion while traveling in the UK.
Out of the 231 documented cases of vCJD, three individuals contracted the prion through blood transfusions. This represents 1.3 percent of all vCJD cases, meaning they were not caused by consuming infected cattle but were transmitted by someone who already had vCJD. Scientists classify this as a rare instance of vCJD combined with iatrogenic CJD and now advise individuals with any form of CJD to refrain from donating blood.
