Allergies arise when the body reacts defensively to substances it deems harmful. While food is a common trigger, they can also be provoked by animals, electronic devices, medications, and even other health conditions.
Many are unaware that allergies can stem from unexpected sources. For example, a chocolate allergy is rarely due to cocoa or other chocolate ingredients. Instead, it’s often caused by traces of cockroach particles found in chocolate. Below are nine more surprising examples, some of which remain unverified by medical experts.
10. Cockroach Residue Triggers Chocolate Allergy

While some individuals report chocolate allergies, the real culprit is often cockroach fragments that inadvertently end up in chocolate products. These particles are finely ground, making them less noticeable but still capable of triggering allergic reactions.
While ground-up cockroaches might seem like a valid reason for the FDA to penalize chocolate manufacturers, the agency actually allows up to 60 insect fragments per 100 grams of chocolate. On average, a standard chocolate bar contains about eight such fragments.
Cockroaches frequently find their way into chocolate during the cocoa bean harvesting process, infiltrating the crops. Farmers already employ various pesticides to control their population, but eliminating them entirely would require even more chemicals. This would result in chocolate being laden with pesticides, posing a greater health risk than the presence of cockroach particles.
In addition to chocolate, cockroach remnants can also cause allergic reactions in foods such as peanut butter, macaroni, popcorn, cheese, wheat, and certain fruits.
9. Vaccines Allegedly Linked to Peanut Allergies

Peanut allergies are prevalent among young children, affecting millions in the US. Some unconventional sources suggest that vaccines are a significant contributor to this issue. The use of refined peanut oil, a key component in vaccines, is cited as the reason. Manufacturers include this oil to stabilize vaccines and help the body combat the weakened pathogens they contain.
While various oils are suitable for vaccine production, manufacturers are said to favor refined peanut oil due to its affordability. However, this oil is believed to trigger hypersensitivity, or serum sickness, in certain children, potentially leading to peanut allergies later in life. It’s important to note that no scientific evidence supports the alleged connection between vaccines and peanut allergies.
8. Another Potential Culprit Behind Wi-Fi Allergies

Electromagnetic hypersensitivity (EHS) is a purported allergy triggered by proximity to devices emitting electromagnetic signals, such as cell phones, computers, and Wi-Fi. However, this condition lacks medical recognition, and its validity remains debated.
The World Health Organization (WHO) maintains that EHS is not a genuine medical condition, despite acknowledging the reality of its symptoms. Dr. James Rubin, a psychologist at King’s College London, suggests that while EHS symptoms are real, they are not caused by electromagnetic fields.
A 2009 review of 46 studies on EHS revealed that participants could not reliably detect whether electromagnetic devices were active or inactive. Despite this, individuals continue to report symptoms like severe headaches, nausea, fatigue, and dizziness, which they claim subside when they move away from the source of electromagnetic signals.
In Massachusetts, a 12-year-old’s parents filed a lawsuit against his private school, alleging that the school’s Wi-Fi triggered EHS symptoms like nosebleeds and heart palpitations in their son. Interestingly, doctors couldn’t confirm the condition, as the symptoms vanished when the boy was away from school.
In France, a woman with EHS relocated to the mountains to avoid electromagnetic signals. Similarly, the parents of a 15-year-old UK girl attributed her suicide to EHS, claiming that Wi-Fi signals at her school caused disorientation and illness, ultimately leading to her tragic decision.
7. Dogs Can Develop Allergies From Repeatedly Eating the Same Food

Dog owners are often puzzled when their pets develop allergies to a food they’ve consumed without issue for years. In reality, dogs can develop allergies from prolonged exposure to the same type of food.
These allergies can arise from consuming the same brand of food or foods with identical protein sources. Repeated exposure to the same ingredients or proteins can trigger food allergies, which is why they are more common in dogs older than two years.
The primary food allergens for dogs include beef, dairy products like milk and cheese, chicken, and wheat. Other potential triggers are eggs, corn, lamb, soy, yeast, spices, and various additives.
6. Airborne Particles Trigger Allergies Misattributed to Air Conditioning

It’s impossible to be allergic to air conditioners themselves. Those who believe they have an air conditioner allergy are actually reacting to airborne particles circulated by the unit. Common culprits include pollen, dust mites, pet dander, mold, toxins, bacteria, viruses, air pollution, or harmful chemicals.
Air conditioners don’t produce these allergens but disperse them throughout the space. Pollen can enter through open doors, windows, or on clothing and shoes. Indoor plants can also be a source. Toxic chemicals often originate from household cleaning products or similar items.
5. Baby Wipes May Be Linked to Food Allergies

Baby wipes have recently been linked to food allergies in infants. Researchers suggest that the soap and similar substances in wipes may disrupt the natural chemicals in the skin’s outer layer, potentially triggering allergic reactions.
Certain children possess genes that make them susceptible to food allergies when exposed to these chemicals. As a result, experts recommend that parents avoid using wipes altogether and opt for water to clean their babies.
However, the findings are not definitive, and some argue that baby wipes do not cause food allergies in children. This skepticism stems from the fact that the widely cited study linking wipes to allergies was conducted on newborn mice, not humans.
4. Allergies to Birds and Dogs Are Often Caused by Dead Skin

Many people claim to be allergic to dogs, but in reality, they are reacting to dander—dead skin cells shed by the animal. Other triggers include the dog’s saliva, urine, or pollen and mold that cling to its fur.
Dander, which is airborne, tends to accumulate in homes or places frequented by dogs. This explains why individuals allergic to dogs often experience reactions in areas where dogs have been, even in the animal’s absence. Studies show that those with dog allergies have an overactive immune system that mistakes dander, urine, or saliva for harmful pathogens and responds aggressively.
Similarly, allergies to birds are not caused by the birds themselves but by the dander on their feathers and the dust mites that thrive on it. These allergens are often dispersed into the air when birds flap their wings.
3. Allergic Eczema Is Connected to Food Allergies in Children
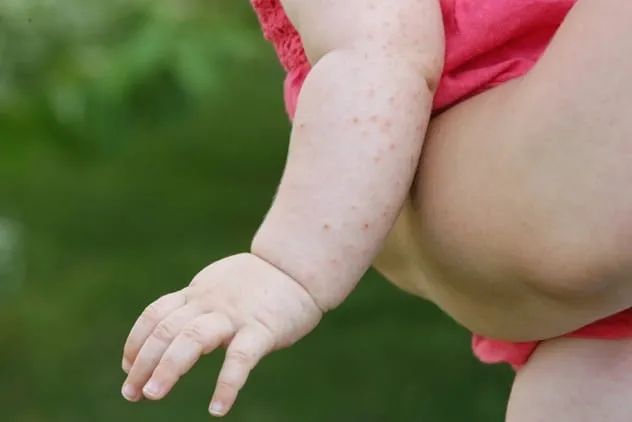
Allergic eczema occurs when the skin comes into contact with an allergen, resulting in a dry, itchy rash that may be painful and sometimes accompanied by blisters.
Recent studies reveal a connection between eczema and food allergies in children. Currently, 20 percent of children are affected by allergic eczema, and notably, 30 percent of these children also suffer from food allergies.
Studies have shown that the skin near eczema patches in children with food allergies often has distinct molecular structures compared to other areas of their skin. In contrast, children without food allergies exhibit no such differences in the skin surrounding their eczema.
Researchers suggest that these molecular differences explain why some children with allergic eczema develop food allergies while others do not. They also believe that analyzing these structures could help identify food allergies in children at an earlier stage.
2. Folic Acid May Trigger Allergies in Unborn Babies

Pregnant women are frequently encouraged to consume various vitamins and minerals to ensure a healthy pregnancy. Folic acid, the synthetic form of vitamin B9, is among the most crucial.
While folic acid is recommended during the first trimester of pregnancy, research from the University of Adelaide’s Robinson Research Institute suggests that consuming it beyond this period may increase the risk of allergies in the developing child.
However, similar to the baby wipe findings, this research was deemed inconclusive as it was conducted solely on sheep. Researchers found that lambs whose mothers consumed folic acid late in pregnancy often developed allergies to dust mites and egg albumen.
1. Parasites Are Responsible for Swimmer’s Itch
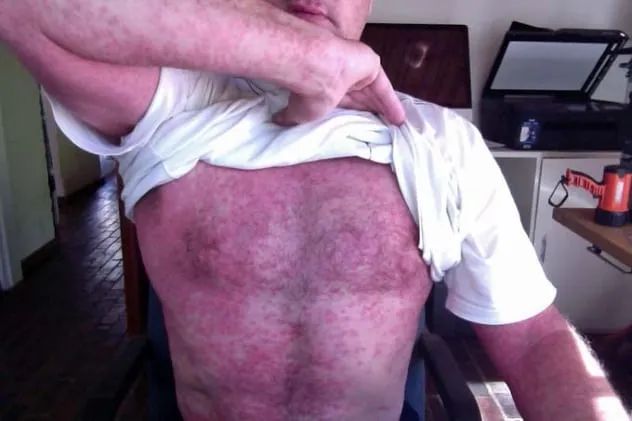
Chlorine rash is frequently mistaken for swimmer’s itch. Although both conditions result from swimming, they cannot occur simultaneously in the same water. Chlorine rash arises from swimming in chlorinated water, while swimmer’s itch occurs in non-chlorinated water.
Swimmer’s itch is an allergic reaction, whereas chlorine rash is not. Humans cannot develop allergies to chlorine but can become sensitive to it. Chlorine rash is caused by prolonged exposure and interaction between the skin and chlorine.
Swimmer’s itch, also called cercarial dermatitis, is triggered by a parasite. It typically occurs after swimming in lakes, ponds, or occasionally saltwater. However, it is rare in swimming pools because chlorine inhibits the parasites’ survival.
The parasites enter the water as eggs through the feces of animals like beavers, muskrats, and waterfowl that inhabit water-adjacent areas. After hatching, they are ingested by a specific type of snail before being released back into the water.
These parasites penetrate the skin of swimmers, leading to an allergic reaction. Fortunately, humans are unsuitable hosts, and the parasites die within a few days.
