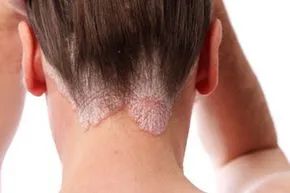
 Certain genetic skin disorders, such as psoriasis, can be quite severe without posing a life-threatening risk. However, some can be deadly. Explore more images of skin conditions.
iStockphoto/Thinkstock
Certain genetic skin disorders, such as psoriasis, can be quite severe without posing a life-threatening risk. However, some can be deadly. Explore more images of skin conditions.
iStockphoto/ThinkstockThe skin, despite its durability and vast coverage, is susceptible to various issues. Sun exposure can harm skin cell DNA, causing sunburn or potentially cancer. Harsh, dry, and windy environments can strip moisture from the skin, resulting in painful, cracked areas. Additionally, blocked sebaceous glands may lead to acne.
While we can adopt preventive measures to shield our skin from environmental harm, some skin conditions originate internally due to genetic mutations inherited from our parents. These inherited skin issues are known as genodermatoses, or genetic dermatological disorders.
Genodermatoses encompass a wide spectrum of conditions. Some, such as psoriasis, may be mild and manageable with topical treatments. Others, like harlequin-type ichthyosis, can be life-threatening. Below are five inherited skin disorders that affect large areas of the skin.
5: Darier-White Disease
 The biological process responsible for fingernail formation can also occur abnormally on the skin, leading to a condition called Darier-White disease.
Pixland/Thinkstock
The biological process responsible for fingernail formation can also occur abnormally on the skin, leading to a condition called Darier-White disease.
Pixland/ThinkstockDarier-White disease, clinically referred to as keratosis follicularis, was first discovered in the late 1800s by dermatologists Ferdinand-Jean Darier and James Clarke White. White recognized it as an inherited skin disorder when a mother and daughter sought his treatment for the condition.
Darier-White disease is marked by the unusual hardening of skin cells on the epidermis, a phenomenon known as keratinization. This process, which typically transforms healthy skin cells into fingernails, occurs abnormally on other parts of the skin in those with Darier-White disease. Studies indicate that sufferers' skin cells lack the binding junctions called desmosomes, potentially increasing the frequency of keratinization [source: Kwok]. The most noticeable signs are clusters of small, oily, yellow-brown, pimple-like papules that develop around sebaceous glands [source: Spitz].
Scientists have identified connections between mutations in the ATP2A2 gene and Darier-White disease, yet no consistent mutation pattern has been established to define the condition. Interestingly, individuals with identical ATP2A2 mutations may exhibit varying symptoms.
4: Epidermolysis Bullosa
 Bullosa causes agonizing blisters to form due to minor temperature changes or pressure.
©iStockphoto/whitemay
Bullosa causes agonizing blisters to form due to minor temperature changes or pressure.
©iStockphoto/whitemayEpidermolysis bullosa (EB) is a severe inherited skin disorder that causes blistering due to minor pressure or temperature variations. Typically, blisters form when the epidermis and dermis separate, creating a fluid-filled cushion to protect and heal the underlying skin.
Individuals with epidermolysis bullosa experience an exaggerated blistering response. Everyday activities like walking, crawling, or being held, as well as slight temperature fluctuations, can trigger painful blisters. Frequent blistering raises the risk of infections, which can lead to severe complications such as amputation.
EB has been associated with mutations in at least 10 different genes. While the condition is usually inherited from parents, it can occasionally arise from spontaneous mutations [source: Mayo Clinic]. Most often, the disorder stems from inherited mutations in genes that produce keratin proteins, which are essential for maintaining the structural integrity and bonding between skin layers [source: Marinkovich].
3: Lamellar Ichthyosis
 In normal skin, fresh skin cells replace older ones, which are then shed. However, individuals with lamellar ichthyosis produce healthy skin cells but cannot shed them, resulting in the formation of scaly plates across their bodies.
Hemera/Thinkstock
In normal skin, fresh skin cells replace older ones, which are then shed. However, individuals with lamellar ichthyosis produce healthy skin cells but cannot shed them, resulting in the formation of scaly plates across their bodies.
Hemera/ThinkstockThe genetic disorder lamellar ichthyosis derives part of its name from the Latin word for fish, ichthys. This is fitting, as those affected by lamellar ichthyosis develop thick, fish-like scales across their skin due to the condition.
In healthy individuals, older skin cells shield newer ones before being shed and replaced. Beneath the stratum corneum (the outermost layer), skin cells called keratinocytes divide to create fresh, healthy cells. As these cells age and die, they harden and move toward the stratum corneum to form a protective layer. Eventually, they are shed as new hardened cells take their place. In lamellar ichthyosis, skin cells develop normally but fail to separate once they reach the stratum corneum, preventing shedding. Over time, these dead cells accumulate, forming the characteristic hard, scaly plates that cover the body [source: WebMD].
This condition is rare. Symptoms typically appear in early childhood or at birth, with scales present from infancy. While symptoms may fade during adulthood, they can reappear later in life [source: Mayo Clinic].
2: Cutaneous Porphyria
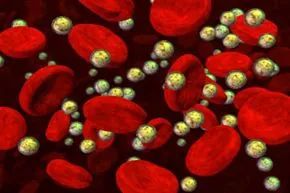 The inherited skin disorder cutaneous porphyria stems from the body's inability to transform porphyrins into heme.
iStockphoto/Thinkstock
The inherited skin disorder cutaneous porphyria stems from the body's inability to transform porphyrins into heme.
iStockphoto/ThinkstockCutaneous porphyrias encompass six distinct types of the inherited disorder porphyria. In each type, individuals lack the enzymes necessary to produce heme, a vital component of red blood cells responsible for oxygen transport. Heme is synthesized from chemicals called porphyrins, which can build up when not converted into heme. This deficiency in heme and accumulation of porphyrins result in the symptoms of porphyria. Cutaneous porphyrias specifically affect the skin.
In cutaneous porphyria, the skin becomes highly sensitive to light. Even brief exposure to sunlight can cause redness, painful irritation, and blistering. Additionally, the skin may swell and darken abnormally when exposed to sunlight [source: American Porphyria Foundation]. Consequently, patients are strongly advised to avoid sunlight.
Children inherit this disorder from one or both parents. There are eight enzymes involved in converting porphyrins to heme, and a mutation in any of the genes responsible for producing these enzymes can lead to porphyria.
1: Mal de Maleda
 Mal de Maleda derives its name from the island of Maleda, located near Croatia, where the condition was first identified.
Adam Jones/Getty Images
Mal de Maleda derives its name from the island of Maleda, located near Croatia, where the condition was first identified.
Adam Jones/Getty ImagesAmong genodermatoses, Mal de Maleda is exceptionally rare. This inherited skin condition primarily affects individuals of Mediterranean ancestry and was named after the Croatian island of Maleda, where initial cases were recorded [source: Goldsmith].
The disorder is a subtype of keratosis palmaris et plantaris, a more common skin condition marked by thickened skin on the palms and soles. This thickening occurs due to enlarged skin cells, resulting in larger palms and soles with a yellowish tint [source: Wrong Diagnosis].
Given that Mal de Maleda is an uncommon genodermatosis, it follows that it is also an autosomal recessive disorder. This implies that two copies of the defective gene, one from each parent, are required for the condition to manifest.
The SLURP1 gene, which plays a role in producing proteins essential for cell binding, has been pinpointed as the cause of Mal de Maleda [source: Spitz].
