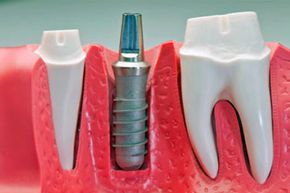
 The phrase "dental implants" refers to the artificial roots that serve as the base for fixed or detachable replacement teeth.
iStockphoto/Thinkstock
The phrase "dental implants" refers to the artificial roots that serve as the base for fixed or detachable replacement teeth.
iStockphoto/ThinkstockFor millions of individuals, replacing teeth would be far simpler if it were as easy as locating new teeth and inserting them. Smile—you're finished. Naturally, whether you choose conventional dentures or dental implants, the process is a bit more complex.
Dentures and bridges are the most popular and cost-effective solutions for tooth replacement, but implants are regarded as the closest alternative to natural teeth [source: JADA]. (The term "dental implants" technically refers to the artificial roots that support fixed or removable teeth, but it is also commonly used to describe the teeth themselves.) Titanium or titanium alloys, which are durable and lightweight metals, are typically used for implants, while the teeth are crafted from porcelain and other composite materials designed to resemble and blend with natural teeth.
Imagine the process of getting dental implants as similar to setting up a fence post. Initially, a hole is dug into the ground to place a supporting beam. This post might be stabilized with cement that requires time to set or packed with soil to provide a solid base, ensuring it stands upright and sturdy enough to hold the fence.
Creating a durable tooth implant follows a comparable procedure. A skilled surgeon drills into the jawbone, and once the implant is in place, the surrounding gum tissue and bone must regenerate around it to fortify the structure. This foundation supports the post, which then holds the artificial crown in place among neighboring teeth. It’s more about structural integrity than aesthetics.
Numerous individuals qualify for dental implants, but a collaborative effort between a dentist, an oral and maxillofacial surgeon, and a periodontist is essential to confirm adequate gum health and bone density for a durable implant. This team conducts detailed examinations, X-rays, and devises a treatment strategy. The implant procedure is not a quick fix; it unfolds over several months [source: Mayo Clinic].
Why opt for surgery when alternatives are available? And even if you’re eligible, is it financially feasible? Next, we’ll explore the key distinctions among artificial tooth solutions.
Artificial Teeth Options
Dental implants serve a crucial purpose, but with costs ranging from $3,000 to $4,500 per implant—and tens of thousands for a partial bridge or full set—why not opt for dentures? Both options have their advantages and disadvantages. Dentures, for instance, can cost between $1,200 and several thousand dollars for a complete set, which is significantly less than implants. However, implants demand far less maintenance and fewer long-term expenses compared to dentures. Additionally, insurance companies often reimburse a higher percentage for dentures and bridges than for implants, though some policies may cover dental implants as well [source: Alderman].
Why are implants more expensive, and should you choose them over dentures? The higher cost is partly due to the surgical nature of the procedure and the involvement of multiple specialists, including dentists, prosthodontists (who handle both natural and artificial teeth), periodontists (who treat the gums), and maxillofacial surgeons (who work with the jawbone and insert the posts). While not every implant procedure requires all these experts, most involve consultations with both surgeons and dentists. Despite the cost, many patients find the comfort and natural look of implants to be worth the investment.
Implants are often a lifelong solution, with fewer than 5 percent of surgeries failing. In contrast, dentures and bridges typically need replacement every five years. Unlike dentures and bridges, implants do not slip, rarely require adjustments to adjacent teeth, and contribute to healthier gums and bones over time [source: Alderman].
Next, we’ll explore how dental implants are placed and why they remain so securely in position.
Parents often face the heartbreak of their children losing permanent teeth due to sports injuries or accidents. While dental implants might seem like an ideal solution, children and young adults are generally poor candidates because their jaws are still developing. Implants in growing jaws can shift, leading to misaligned bites over time. However, in some cases, implants can be successful when combined with orthodontic treatments, so consult your dentist and orthodontist for advice [sources: AAOMS; Brahim].
Placing Dental Implants
Opting for dental implants to replace lost teeth involves a multi-month process. While implants are durable and long-lasting, they also require significant time to properly integrate. Following initial evaluations to check gum and bone health, a team of dental specialists—including a dentist, surgeon, periodontist, and restorative dentist or prosthodontist—will create a surgical and treatment plan tailored to the patient’s oral health and tooth replacement requirements.
If the bone is healthy and dense enough, the procedure can proceed. However, if gum tissue or bone density is insufficient, additional treatments like periodontal care or bone grafting may be required before implantation. (We’ll discuss bone-building options later.) Since dental implantation is a surgical process, patients must also be in good overall health.
The first step in the implant process involves the surgeon cutting into the gum tissue to access the underlying bone. The area is completely numbed to minimize or eliminate pain during the procedure. (Anesthesia options range from general anesthesia to localized numbing agents like Novocain.) A hole is then drilled into the jawbone, and a titanium implant, shaped like a screw, is inserted. The implant is customized to fit the tooth space and adjusted to match the patient’s jawbone thickness, extending slightly above the bone’s surface [source: Mayo Clinic].
Once the implant is placed, it must remain undisturbed to allow the bone to fuse with it through a process called osseointegration. The gum tissue is stitched closed and requires time to heal and tighten around the implant site, emphasizing the importance of healthy gums before surgery. This healing and fusion process can take three to nine months or longer, during which patients usually wear a temporary cosmetic overlay or partial denture in place of permanent teeth [sources: ADA; JADA; Mayo Clinic].
Dr. Ira Cheifetz, former president of the American Association of Oral and Maxillofacial Surgeons, explains that bone growth and healing continue long after the implant procedure because the screw in the jawbone mimics the presence of natural teeth, prompting the body to maintain bone density [source: Alderman].
While the bone-drilling phase is finished, additional procedures may still be required before the new teeth are installed. We’ll explore this further next.
Dental Implant Abutments
 Once the titanium implant is surgically placed into the jawbone, an abutment is attached to it. These abutments serve as the foundation for the custom-designed crowns that are later secured in place.
iStockphoto/Thinkstock
Once the titanium implant is surgically placed into the jawbone, an abutment is attached to it. These abutments serve as the foundation for the custom-designed crowns that are later secured in place.
iStockphoto/ThinkstockDental implant procedures are increasingly performed in two stages, though they can sometimes involve three—often by choice. After the implant is placed into the bone, a post, or abutment, is attached to the titanium implant. This abutment serves as the anchor for the new crown or artificial tooth. While the abutment is often added during the initial implant procedure, it can also be attached in a second, minor surgery where the gums are reopened, and the abutment is secured. The gums then require several weeks to heal around the abutment—but not over it—before proceeding to the next step [source: NIDCR].
Since the abutment protrudes from the implant and through the gums, it remains visible and cannot be easily hidden. The implant itself, however, remains concealed. For this reason, some patients choose to delay the abutment placement to avoid having it exposed during the months-long healing process [source: Mayo Clinic]. In many cases, a temporary crown or denture can be fitted and worn during this period, similar to a one-step procedure.
Whether the procedure is completed in one or two steps, maintaining excellent oral hygiene is crucial. As the bone heals and the gums close around the abutment, a solid foundation is established for the final stage: attaching the dental crown. Once the surgical work is complete, the body responds by regenerating bone and firming up gum tissue to support the new teeth.
Once the gums have fully healed, a dentist or specialist takes impressions of the mouth to create a custom-fitted crown—or implant prosthesis—which is then attached to the abutment and adjusted as needed. For single-tooth replacements, a fixed implant is typically screwed or cemented onto the post. For multiple teeth or full sets, removable implants are an option, functioning similarly to bridges by allowing easy removal for cleaning or repairs. After this final restoration step, the new teeth are ready for use, often lasting a lifetime with proper care [source: Mayo Clinic].
In some cases, additional preparatory work is required before even reaching the initial implant surgery. We’ll explore these preparatory steps and potential complications next.
Jaw Bone Growth and Grafting
Dental implant surgeries boast a high success rate, but their effectiveness and longevity depend on several factors. Adequate bone density at the implant site and the ability of the bone to heal and integrate with the titanium are critical. In some cases, bone grafts are necessary to qualify a patient for the procedure. Rarely, if implants fail, maxillofacial surgeons may perform bone grafts to reinforce the area before attempting the procedure again.
When bone density is insufficient or the bone is too soft, surgeons may extract bone from another area, such as the hip, and transplant it to the jawbone. This grafted bone fuses with the existing jawbone over six to nine months. For minor bone deficiencies, grafts can sometimes be performed during the implant placement, with fusion occurring during the osseointegration phase [source: Mayo Clinic]. Synthetic materials are also an option for augmenting bone mass in certain situations.
While these steps may appear complex, expensive, and time-intensive, they often result in a permanent solution for lost teeth. Implants provide a natural look and feel, and with proper care, they can last a lifetime with minimal maintenance. Smoking and poor oral hygiene are known to reduce the success and durability of implants, but few other issues are documented in medical and dental research.
Implant dentistry offers a reliable alternative to traditional partial bridges and dentures. As its popularity grows, it may lead to better insurance coverage and reduced costs, potentially addressing the dental needs of an aging population in the future.
Next, we’ll explore more about maintaining and enhancing your smile.
Maintaining dental implants is similar to caring for natural teeth. It’s typically advised to brush multiple times daily, floss at least once a day, and schedule regular dental check-ups every six months. If bone grafting or periodontal work is involved, additional care instructions may be included in your oral hygiene routine. For implants supporting removable partial dentures, both the implants and the denture should be cleaned—brushing and flossing the implants, and gently scrubbing and rinsing the denture when removed. Depending on the material of the appliance, your dentist may recommend regular toothpaste or milder options like soap or denture cleaners. While toothpaste is generally safe for permanent implant crowns, always consult your dentist for specific advice.
