 ©iStockphoto.com/creacart
©iStockphoto.com/creacartGlancing in the mirror, you notice a pus-filled breakout on your nose and chin. As you turn around, you spot the cyst-like pimples that have settled on your back, causing significant pain with even the slightest pressure. While it’s not the plague, dealing with acne can make you feel isolated due to the discomfort, pain, and social embarrassment it brings.
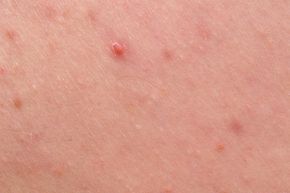
Acne is a skin condition characterized by inflamed breakouts. These occur when the sebaceous glands, responsible for producing sebum (oil) to moisturize skin and hair, get blocked by dead skin cells or excess oil. This blockage can lead to bacterial growth, which triggers inflammation. Commonly referred to as zits, pimples, blackheads, or whiteheads, acne typically falls into two main categories:
- Acne vulgaris: This prevalent type of acne appears as blackheads or whiteheads on the skin.
- Acne cystic: A more severe form, this occurs when blockages are deep within hair follicles, resulting in painful red bumps, pustules, nodules, and cysts that may lead to scarring.
Acne is most common among teenagers due to hormonal changes that activate sebaceous glands, leading to excess sebum production. Although many teens outgrow acne, adults, particularly women before menstruation, can also experience breakouts.
Acne develops in areas with a high concentration of sebaceous glands. Nearly 92 percent of acne sufferers deal with facial acne, while 60 percent report breakouts on their back and chest [source: McCoy].
Back acne, often referred to as "bacne," is typically more severe, causing significant pain, scarring, and even social discomfort. Below, we explore the causes of this severe acne and effective ways to treat it.
Back Acne Causes
While the exact cause of acne remains unclear, doctors have identified several factors that increase susceptibility [source: American Academy of Dermatology]. Hormonal fluctuations, particularly during puberty, can trigger overactive sebaceous glands, leading to excess sebum production and clogged pores. Similarly, adult women may experience breakouts due to hormonal shifts before their menstrual cycle.
Genetics also play a role in acne development. If your parents had acne, you’re more likely to inherit traits that cause excessive sebum production and follicle blockages [source: Fulton].
External factors, such as heat, pressure, or friction, can lead to acne mechanica, a condition where acne forms in areas prone to irritation. Pollution and high humidity exacerbate back acne by creating ideal conditions for clogged pores and breakouts.
Athletes may develop acne mechanica along the hairline from helmets or on skin areas under pressure from tight uniforms. Similarly, musicians who play string instruments can experience chin acne due to prolonged contact with their instruments.
These examples illustrate how acne mechanica can affect the back. Students carrying heavy backpacks, outdoor workers wearing tight clothing in hot weather, and frequent drivers exposed to seat pressure are all at risk of developing back acne.
Many people attribute acne to stress or specific foods like chocolate and fried items, but scientific evidence does not support these claims [source: Mayo Foundation for Medical Education and Research].
Now that we’ve explored the causes of back acne, let’s delve into effective ways to manage and control it.
Oily, irritated skin doesn’t always indicate acne. If the affected area is scaly and flaky instead of bumpy, you might be dealing with seborrheic dermatitis.
Similar to acne, the exact cause of seborrheic dermatitis is unknown, but experts link it to excessive oiliness and yeast-related irritation. Genetics, stress, lack of sleep, harsh weather, or poor hygiene can contribute to this condition. Those with acne may also be prone to seborrheic dermatitis. Treatments include dandruff shampoos, over-the-counter products, or prescription medications with selenium, ketoconazole, or corticosteroids [source: The A.D.A.M. Medical Encyclopedia].
Back Acne Treatments
Home remedies can sometimes help manage bacne, but be cautious of unproven "remedies" that lack scientific backing.
Certain home remedies, such as 5 percent tea tree oil gels, zinc supplements, and glycolic acid, may alleviate back acne pain [source: Gibson]. Wearing loose, breathable clothing can also reduce pressure and friction, allowing the skin to breathe.
Over-the-counter topical and oral treatments can be effective for acne. Cleansers with 2 percent salicylic acid and benzoyl peroxide spot treatments help dry excess oil. Apply these to clean skin, covering the entire affected area, and continue use even after breakouts subside. For hard-to-reach areas, consider a spa back facial or use a loofah sponge or back brush with acne body wash containing salicylic and glycolic acid.
When home treatments fail to clear stubborn acne after four to 12 weeks, or if scarring and self-esteem issues arise, consult a dermatologist. They can assess your skin, diagnose the issue, and prescribe appropriate medication.
With the right care, you can reduce the discomfort and embarrassment of back acne and achieve healthier skin. Continue reading for more acne-related insights.
