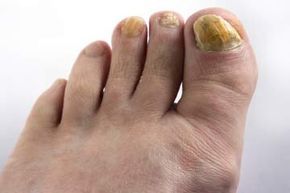
 Fungal infections frequently alter the appearance and feel of your nails. Check out additional images of skin-related issues.
© iStockphoto.com/adrian beesley
Fungal infections frequently alter the appearance and feel of your nails. Check out additional images of skin-related issues.
© iStockphoto.com/adrian beesleyThe term 'fungus' has an inherently unpleasant ring to it. Even without knowing its exact meaning, most people would avoid having it on their bodies. However, up to 14% of Americans suffer from nail fungus, with the percentage rising to 40% among those aged 60 and above [source: PDRhealth]. Thankfully, there are clear indicators of nail fungus to watch for, and effective treatments are available for those affected.
Fungal infections can affect both fingernails and toenails. To identify nail fungus, be aware of its typical symptoms. Notice any shifts in your nails' texture or color. Some fungi cause yellow streaks beneath the nail, while others appear as white spots or streaks on the nail's surface. Depending on the fungus type, your nail may thicken and detach from the nail bed, or it may weaken, crumble, or break while staying attached [source: WebMD].
Beyond changes in color and texture, fungal infections can extend from the nails to the surrounding skin, leading to inflammation, redness, and irritation. In severe cases, these infections may cause significant pain and emit a foul odor.
Nail fungus isn't just unsightly; it can disrupt your daily life [source: PDRhealth]. Fortunately, prevention is possible if you understand its causes. Continue reading to discover when and why nail fungus becomes a problem.
Causes of Nail Fungus
While understanding the causes of nail fungus is helpful, some risk factors are beyond your control. For instance, men are more prone to nail fungus than women [source: Mayo Clinic]. Age also increases susceptibility, particularly for those over 60 [source: PDRhealth]. Additionally, a family history of nail fungus can elevate your risk.
Fungi, plant-like parasites, naturally reside on your body. While yeast can cause nail infections, dermatophytes are the primary offenders, responsible for 90% of toenail fungal infections [source: WebMD]. Your toenails provide an ideal food source for these fungi, as they thrive on keratin, the protein found in skin, hair, and nails [sources: PDRhealth and WebMD].
Fungi thrive in dark, damp environments. Wearing non-breathable socks and tight shoes all day creates an ideal setting for fungal growth. However, avoiding shoes and socks altogether and going barefoot doesn't guarantee protection; walking barefoot in certain areas can still expose you to nail fungus [source: Mayo Clinic]. Even the smallest cut on your foot can provide an entry point for these organisms.
Whether due to unavoidable risk factors or occasional lapses in precautions, developing nail fungus doesn't mean you're stuck with thick, painful nails forever. Several effective treatments are available. Continue reading to explore your options.
Locker rooms, swimming pools, and public showers are hotspots for fungi due to their moist environments. Fungi can also linger on nail clippers and other grooming tools [source: PDRhealth].
Nail Fungus Treatments
Your doctor is the best person to consult for treating nail fungus. Since various fungi can cause infections, your doctor will likely take a nail sample to identify the specific type. Other conditions, like psoriasis and eczema, can mimic fungal symptoms, so an accurate diagnosis is crucial before starting any treatment [source: WebMD].
After a confirmed diagnosis, fungal nail infections can be treated in three primary ways. The first involves oral anti-fungal medications, which are highly effective but may cause side effects like liver damage. Additionally, since these medications work as nails grow, treatment can take four months or longer [source: Mayo Clinic].
Topical treatments, such as anti-fungal creams, offer an alternative to oral medications and are most effective in early stages. For severe or painful infections, surgical removal of the infected nail and surrounding tissue may be necessary. However, fungal infections are notoriously persistent and may return even after successful treatment [source: WebMD].
For those avoiding medical visits or preferring non-invasive treatments, homeopathic remedies are an option. Continue to the next page to explore these alternatives.
Nail biting is an unhealthy habit, particularly if it damages the skin around your nails, creating an entry point for fungal infections. It can also transfer infections from your hands to your mouth. Breaking this habit is essential—consider alternatives like chewing gum or keeping your hands busy [source: Gibson].
Home Remedies for Nail Fungus
For those who prefer a hands-on approach and wish to tackle nail fungus with home remedies, here are some popular options people have tried, often applying them consistently over several months:
- Listerine
- Vinegar and water
- Listerine and vinegar
- Vicks VapoRub
- Oil of oregano
- Tea tree oil
[source: Graedon]
These treatments share two key characteristics. First, users report that it takes several months to see results, similar to prescription medications [source: Graedon]. Fungus is notoriously stubborn, and nails respond slowly to treatment. Second, these remedies are anecdotal—there’s no scientific evidence supporting their effectiveness. Proceed with caution, as untreated infections may worsen and become harder to treat later [source: Mayo Clinic].
The best home remedy is prevention. To avoid nail fungus, keep your feet dry by wearing open-toed shoes, moisture-wicking socks, and changing socks frequently. Use flip-flops in public showers and avoid walking barefoot in communal areas [source: Mayo Clinic].
In certain situations, home remedies are not advisable. Individuals with weakened immune systems or diabetes face a higher risk of severe infections if they develop nail fungus, as the condition can be exacerbated by their underlying health issues. If you fall into this group, seek medical attention promptly [source: Mayo Clinic].
