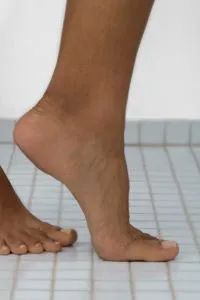
 Tinea, the fungal infection behind athlete's foot, can show up on almost any part of your skin. View more images of skin conditions.
Medioimages/Photodisc/Getty Images
Tinea, the fungal infection behind athlete's foot, can show up on almost any part of your skin. View more images of skin conditions.
Medioimages/Photodisc/Getty ImagesThere's a fungus among us, causing discomfort and frustration. The agent behind this is from the genus Trichophyton, a group of fungi known as dermatophytes. These fungi reside in the epidermis, the outer layer of skin, where they thrive on the protein keratin, a key component of skin, horns, and claws in other animals, which helps defend against germs and other invaders.
Trichophyton is one of the few microorganisms capable of producing the enzyme required to break down the fibrous structure of keratin. Fortunately for the fungus, your body continuously produces new epidermal cells every four weeks, offering it an unlimited supply of food.
Like other fungi, Trichophyton flourishes in warm, moist environments. On the human body, it typically affects the scalp, groin, and feet. The infection caused by Trichophyton is known as tinea, derived from the Latin word for larva. Infected areas can sometimes resemble the damage caused by moth larvae on wool clothing. This similarity gave rise to its common name, ringworm.
Ringworm is known by various names, some even more specific depending on where it appears on the body. A general case is called tinea corporis, ringworm on the body. When it affects the scalp, it's referred to as tinea capitis, ringworm on the head. In the groin or buttocks, it’s called tinea cruris, commonly known as jock itch. If it infects the feet, it’s tinea pedis, better known as athlete's foot.
Despite the name, no worms are involved in ringworm, but it might make you feel like you're being eaten alive by moths. Your skin becomes red and scaly, cracks, peels, and itches. Infected nails may break down and separate from their beds. The scalp can develop bald patches.
How does Trichophyton manage to reach your skin? How can you prevent it from settling in — or, if that fails, how can you get rid of it? What happens if you leave it untreated? Where can you find relief?
Where It Starts, Where It Leads
Although ringworm has nothing to do with worms, you don’t need to be a jock or an athlete to catch it. In fact, some of Trichophyton’s favorite hosts are children, who are just starting to play games like catch.
Why? Trichophyton spreads easily through both direct and indirect contact. Kids at school push and shove in the lunch line. Friends swap pencils and baseball caps. Siblings share living spaces. A single family can infect an entire neighborhood. The fungus also lives in animal skin. Pets like dogs and cats, or even a classroom rabbit, can carry it. Unsurprisingly, children are more likely than adults to get ringworm on their bodies and scalp.
Fungi thrive in humid environments, and dermatophytes love bare skin. These conditions are abundant in gyms, swimming pools, and locker rooms where athletes gather. But even feet that never step into a gym, yet spend time in damp, sweaty socks, are at risk. Men and teenage boys are more likely to get jock itch and athlete's foot.
Some individuals are especially vulnerable to infection. Those with weakened immune systems, such as people living with AIDS or cancer, are at greater risk. If you’re prone to other fungal infections, you're more likely to develop ringworm.
Trichophyton is persistent. Even after you eliminate the main colony using sprays and powders, small growths can hide in hard-to-reach folds and layers of skin.
If ringworm is left untreated, things can escalate quickly. As keratin is broken down, the skin becomes weaker and cracks. This allows bacteria to enter, bringing along the usual symptoms of infection: fever, pus, and increased heat, pain, and swelling. People with poor circulation in their limbs are more prone to these secondary infections. Individuals with diabetes are especially at risk for complications from athlete's foot. Some may even develop fluid-filled, oozing blisters as an allergic reaction to the fungus and the by-products of keratin breakdown.
You’ll likely seek treatment before reaching that point — first stopping by the drugstore, and possibly making a visit to your doctor.
You can catch athlete's foot from a pedicure, too, if the pedicurist doesn't properly sterilize their instruments.
Lines of Treatment
You can steer clear of the troubles caused by Trichophyton by following two simple rules: Stay clean and dry, and maintain good hygiene. For instance:
- Shower or bathe every day. Follow up by applying talcum powder to keep your skin dry.
- Wear fresh clothes, particularly socks, stockings, and underwear.
- Opt for loose, breathable clothing when possible. Check labels for fabrics made from "wicking" microfibers (usually polyester and nylon blends) that help draw moisture away from your body to aid in faster evaporation.
- Don't share shoes, clothing, or personal items like combs and towels.
- Wear waterproof sandals or other protective footwear in public places where you might expose your feet, such as gyms, spas, or college dorm showers.
- If you're getting a pedicure, bring your own tools.
- Ensure rooms are well-ventilated and disinfect your bathroom regularly as part of your cleaning routine.
If an infection occurs, over-the-counter sprays, powders, or shampoos are typically the first line of treatment. These topical remedies contain antifungals that target Trichophyton's cell walls, combined with cortisone to reduce inflammation. It can take several weeks to completely eliminate the fungus from all the hidden areas.
Research suggests some plant extracts also possess antifungal properties. Ointments with tea tree oil or ajoene, a sulfur compound found in garlic, may prove effective.
If ringworm complications arise, a doctor's intervention is necessary. The doctor might examine skin scrapings under a microscope to confirm that Trichophyton is the cause. They may prescribe stronger topical antifungals or oral medications, especially for scalp infections, and possibly antibiotics. Some oral treatments can have unpleasant side effects, such as stomach issues or liver problems. Additionally, other medications you're taking may influence the treatment approach.
If you tend to sweat, live in a humid climate, or work in damp conditions, be extra cautious. For example, substitute antifungal powder for regular body powder. Whenever safe, go barefoot.
