 The improper use of antibiotic prescriptions has resulted in some bacteria gaining resistance to certain drugs. Explore more drug-related images.
Courtesy Joe Raedle/Getty Images
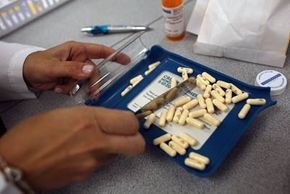
The improper use of antibiotic prescriptions has resulted in some bacteria gaining resistance to certain drugs. Explore more drug-related images.
Courtesy Joe Raedle/Getty ImagesRemember when your doctor prescribed antibiotics and emphasized completing the entire course? You should have heeded that advice. Due to the widespread misuse of antibiotics globally (how many partially used bottles are in your cabinet right now?), the bacteria you aim to eliminate are growing stronger. Some, like the MRSA superbug, have even developed immunity to certain antibiotics.
This occurs through natural selection. Antibiotics are used to eliminate harmful bacteria causing infections. However, stronger bacteria can survive if the antibiotic course isn’t completed, passing on their resistance to future generations.
The rise of drug-resistant bacteria isn't solely due to improper prescription use. Antibacterial and antimicrobial soaps, along with other cleaning products in your home, also play a significant role. Just as antibiotics can be misused, so can antibacterial products. When was the last time you washed your hands for the full 20 seconds recommended by the CDC? It might seem short, but it’s enough time to sing the ABCs once through.
Originally designed to curb infections in hospitals, antibacterial and antimicrobial agents were later marketed to the general public. This widespread use has led to more microbes developing resistance to these agents.
Excessive use of antibacterial products may push bacteria to evolve into stronger, more dangerous forms. This overuse is now a key focus in pharmacoepidemiology, the study of how medications are used by populations.
If antibacterial and antimicrobial products pose a risk to public health, why are they still available? We’ll address that shortly, but first, let’s explore how these products function—or fail to.
Problems with Antibacterials
 A range of bacteria is grown in a lab at Aventis Pasteur, a pharmaceutical company.
Courtesy Aventis Pasteur MSD/Getty Images
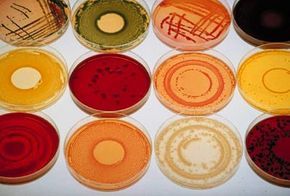
A range of bacteria is grown in a lab at Aventis Pasteur, a pharmaceutical company.
Courtesy Aventis Pasteur MSD/Getty ImagesThrough aggressive marketing, companies persuade consumers that they are under constant threat from microscopic invaders and need specialized antimicrobial products to safeguard their health. However, research indicates that the overuse of these chemicals may be diminishing their efficacy.
Triclosan, a key ingredient in many antibacterial products, disrupts the production of a crucial fatty acid in bacterial cells. However, bacteria that survive exposure to Triclosan can evolve into resistant strains, rendering the chemical ineffective.
How do bacteria develop resistance to antimicrobial agents? According to Dr. Stuart B. Levy of Tufts School of Medicine in Boston, the answer lies in residual traces of the agent left after use. For surviving bacteria, these remnants act as a training ground, prompting mutations and adaptations to counter future attacks. This process, known as selection, allows resistant microbes to thrive and reproduce.
Even more concerning, some antibacterial agents target the same bacterial mechanisms as prescription antibiotics. This means if bacteria develop resistance to an antibacterial agent in a household product, they may also resist similar prescription antibiotics. Scientists refer to this phenomenon as cross-resistance.
Additional research reveals that certain bacteria become more resilient as they adapt. According to Levy's findings, even antibacterial soaps containing 2,500 micrograms of Triclosan may fail to eliminate the most resistant mutated bacteria.
In a study, researchers treated a strain of wild (non-mutated) E. coli — commonly found in raw food — with soap containing 150 micrograms of triclosan. It took two hours to kill 90% of the bacteria. For a mutated strain, two to four times the amount of triclosan was required to achieve the same result.
Adding antimicrobial chemicals to soap may not be effective. In the same study, exposing the same E. coli strain to just six micrograms of pure triclosan killed as many bacteria in the same timeframe [source: Levy].
The excessive use of antibiotics and antimicrobial cleaners might also contribute to a rise in allergies. Continue reading to learn more.
Antibacterial Allergies
 Matsushita's new refrigerator in Japan utilizes a silver ion filter to eradicate 99.9% of bacteria within the appliance.
Courtesy Yoshikazu Tsuno/AFP/Getty Images
Matsushita's new refrigerator in Japan utilizes a silver ion filter to eradicate 99.9% of bacteria within the appliance.
Courtesy Yoshikazu Tsuno/AFP/Getty ImagesA 2005 study revealed that over half of Americans exhibit an allergic reaction to at least one of 10 common allergens [source: AAAAI]. Some microbiologists believe the rise of antibacterial products may be a contributing factor.
From infancy, humans are constantly exposed to microscopic organisms known as environmental flora. These tiny life forms are omnipresent: in soil, on surfaces, in the air, and even within our bodies. While some can cause infections, most are harmless, and some, like lactobacillus, are beneficial, aiding digestion and combating harmful bacteria.
Given the vast number of environmental flora compared to humans, the body has evolved mechanisms to protect against infections and allergies caused by microbes. The T-helper cells in the human body generate an immunoresponse to microbial invasions. There are two types of T-helper cells: T-H1 cells assist other cells in building defenses against microbes, while T-H2 cells manage antibody production, which targets and eliminates foreign microbes.
Together, these helper cells ensure you don’t fall ill from a simple sneeze or a minor cut. They also prevent constant allergic reactions to everyday environmental exposures.
For these cells to function properly, they need exposure to microbes and allergens. Childhood vaccinations introduce weakened or dead microbes, helping the body build defenses against similar strains. In homes overly reliant on antibacterial products, a child’s immune system may miss crucial encounters with allergens, hindering the development of necessary antibodies and defenses.
While parents can maintain a sanitized home, they cannot control the entire world. When a child leaves such an environment, their underdeveloped immune system faces a barrage of microbes and allergens.
Even if you avoid overusing antimicrobial products, you may still encounter them. Antibiotics can be found in the food you consume and the water you drink.
Modern agricultural practices rely on antibiotics to maintain livestock health. These antibiotics persist in the meat consumed by humans. Additionally, runoff from livestock facilities and processing plants can contaminate groundwater and other water sources.
Should antimicrobial agents be banned? It might be too soon to decide. Continue reading to understand why the debate remains unresolved.
Testing Antibacterial Soap
 A 2005 study showed no significant variation in resistant bacteria presence between households using antibacterial products and those using non-antibacterial alternatives.
Courtesy Carl D. Walsh/Aurora/Getty Images
A 2005 study showed no significant variation in resistant bacteria presence between households using antibacterial products and those using non-antibacterial alternatives.
Courtesy Carl D. Walsh/Aurora/Getty ImagesAt the July 2000 Emerging Infectious Diseases Conference in Atlanta, multiple presentations explored the link between antibacterial product use and the rise of resistant bacteria. Stuart B. Levy was among the presenters, sharing a paper titled "Antibacterial Household Products: A Cause for Concern."
In his paper, Levy highlights studies suggesting humanity may be nearing a tipping point where bacteria, fueled by antibacterial product use and antibiotic misuse, could outpace our ability to combat them.
Five years later, Levy collaborated with five peers on a study with contrasting results. They divided 224 households into two groups: one using antibacterial products and the other not. The year-long study focused on families with similar demographics.
The researchers discovered no significant difference in bacterial reduction between antibacterial and regular soap. Additionally, there was no notable rise in resistant bacteria in homes using antibacterial products.
These results were unexpected. The study concluded that antibacterial soap is no more effective than regular soap at killing germs and found no evidence of bacteria mutating into superbugs in antibacterial-using households. However, the study, titled "Antibacterial Cleaning Products and Drug Resistance," noted that one year might be insufficient for definitive conclusions [source: Aiello].
Two years later, researchers from the 2005 study conducted a follow-up experiment. Once again, they found that antibacterial soap offered no superior germ-killing benefits compared to plain soap. However, they also gathered evidence indicating that bacteria are developing cross-resistance due to antibacterial product usage.
Should we be alarmed? The findings remain inconclusive. While microbiologists have observed bacterial mutations in lab settings due to antibacterial agents, real-world evidence is lacking. Nonetheless, scientists believe bacterial mutation is likely inevitable and continue their research.
What’s the most effective way to combat germs? Sometimes, traditional methods remain the best. Continue reading to discover the effectiveness of good old-fashioned soap.
Antibacterial Soap vs Regular Soap
 Dr. Bronner's Magic Soap, an organic soap.
Courtesy Dr. Bronner's
Dr. Bronner's Magic Soap, an organic soap.
Courtesy Dr. Bronner'sSometimes, traditional soap and other proven cleaning methods can be just as effective as modern antibacterial products. Regular soap, though not labeled "antibacterial," still eliminates germs and can sometimes outperform its antibacterial counterparts.
Moreover, soap isn’t the only germ-fighting solution—nature offers many antibacterial agents. Lemon juice, for instance, alters the pH level in bacterial cells, creating an acidic environment that kills microbes. Other natural substances dehydrate bacterial cells, while agents like bleach and certain alcohols destroy bacteria by causing their cells to lyse, or burst.
Why haven’t bacteria developed resistance to bleach, alcohol, or lemon juice? These agents leave no residue, eliminating the chance for bacteria to adapt. As a result, bacteria remain as vulnerable to these substances today as they were a century ago. Skip the targeted antimicrobial approach and opt for these powerful alternatives.
How can we combat superbugs? The basics of cleanliness still hold true. The 2005 study found that frequent handwashing, regardless of soap type, reduced illness in households [source: Aiello]. Good hygiene practices, such as using alcohol-based sanitizers and avoiding sick individuals, remain essential. Stuart Levy also emphasizes that proper antibiotic use can restore environmental flora to its pre-antibiotic and antibacterial era state [source: Levy].
So keep healthy, stay warm and dry, and practice singing your ABCs while washing your hands.
For additional details on antibiotics and related subjects, check out the next page.
