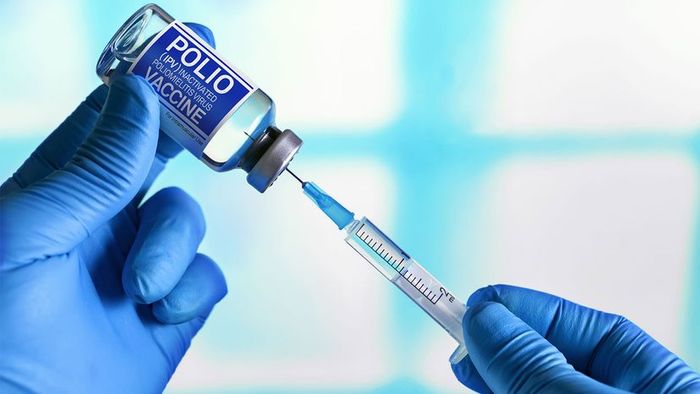
 The inactivated polio vaccine (IPV) is the sole polio vaccine authorized by the U.S. Food and Drug Administration (FDA). angellodeco/Shutterstock
The inactivated polio vaccine (IPV) is the sole polio vaccine authorized by the U.S. Food and Drug Administration (FDA). angellodeco/ShutterstockAs the United States continues to recover from the COVID-19 pandemic and grapples with the recent outbreak of monkeypox, the resurgence of a deadly virus once thought eradicated in the U.S. is the last thing anyone wants to hear.
The Terrifying History of the Polio Virus
During the 1940s and 1950s, polio ranked among the most dreaded viruses, causing over 15,000 paralysis cases annually until vaccines became available starting in 1955. Due to widespread vaccination and robust public health campaigns, wild poliovirus has been absent from the United States for over three decades.
In June 2022, a young, unvaccinated man in his 20s from Rockland County, New York, was confirmed to have contracted vaccine-derived poliovirus. Following this, the New York State Department of Health initiated wastewater surveillance. The CDC confirmed the presence of poliovirus, specifically the paralytic strain, in samples from Rockland County, three additional counties, and New York City.
On September 9, 2022, New York Governor Kathy Hochul declared a state of emergency, urging unvaccinated individuals to get immunized against polio immediately. The World Health Organization also included New York in its list of regions where vaccine-derived polio is actively circulating.
Is polio resurfacing in the United States, and should we be concerned about the risks?
"Currently, the top priority is to ensure you are vaccinated against polio. Most people in the U.S. have been vaccinated unless there's a specific reason they haven't," explains Howard Forman, M.D., a professor of radiology, biomedical imaging, public health, public policy, management, and economics at Yale University. "If you're unvaccinated, get vaccinated. If you're uncertain about your vaccination status and can't verify it through medical records, vaccination is still an option."
How Dangerous Is Polio?
Poliovirus is highly contagious, spreading through direct contact with an infected person's stool or respiratory droplets from sneezes or coughs. Most infected individuals show no symptoms, while about 25% experience mild, flu-like signs such as fever, diarrhea, stomach discomfort, and body aches. Many remain unaware they have contracted polio.
However, approximately 1 in 200 to 1 in 1,000 individuals who contract the virus develop a paralytic form of the disease called poliomyelitis. This condition can vary from mild disability to severe respiratory failure and even death. Dr. Forman emphasizes that those vaccinated against polio face almost no risk of developing paralytic polio.
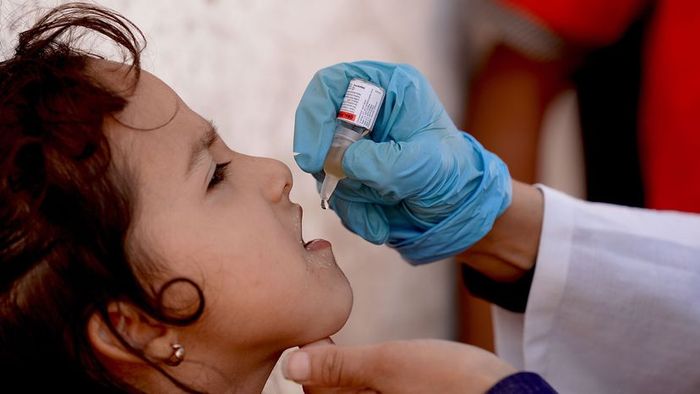 In February 2022, a young girl in Taizz, Yemen, received an oral polio vaccine. Although highly effective, the oral vaccine carries a minimal risk of causing paralytic polio. Due to this risk, the U.S. discontinued its use in 2000, opting exclusively for the inactivated poliovirus vaccine.
Abdulnasser Alseddik/Anadolu Agency/Getty Images
In February 2022, a young girl in Taizz, Yemen, received an oral polio vaccine. Although highly effective, the oral vaccine carries a minimal risk of causing paralytic polio. Due to this risk, the U.S. discontinued its use in 2000, opting exclusively for the inactivated poliovirus vaccine.
Abdulnasser Alseddik/Anadolu Agency/Getty ImagesDespite widespread public health initiatives to immunize all children against polio, certain individuals in the U.S. may not have received either the oral or injectable vaccine or completed the full four-dose regimen. These individuals, including young children, remain vulnerable to contracting polio.
The inactivated polio vaccine (IPV) is the sole polio vaccine authorized by the U.S. Food and Drug Administration (FDA). Administered via injection in the arm or leg, depending on age, the CDC advises that children receive four doses at 2 months, 4 months, 6-18 months, and 4-6 years.
What Is Vaccine-Derived Polio?
While wild poliovirus is the most recognized form, another variant known as circulating vaccine-derived poliovirus (cVDPV) can also spread within communities. Although rare, cVDPV has been on the rise in areas with low vaccination rates. This is the only form of poliovirus observed in the U.S. in recent decades, including the recent cases detected in New York.
Two vaccines have been widely used to prevent polio: the injectable inactivated poliovirus (IPV) and the oral polio vaccine (OPV).
The oral vaccine contains a live, weakened form of the virus, offering enhanced immunity in the gut, where polio replicates. The virus is also shed in stool, enabling its detection in sewage samples. This shedding allows for person-to-person transmission, though vaccinated individuals are not at risk.
In communities with low vaccination rates, the virus can circulate among unvaccinated individuals. Over 12 to 18 months, it can mutate similarly to wild poliovirus, potentially leading to paralytic polio cases.
 Dr. Jonas Salk is pictured in the University of Pittsburgh laboratory where he developed the polio vaccine.
Bettmann/Getty Images
Dr. Jonas Salk is pictured in the University of Pittsburgh laboratory where he developed the polio vaccine.
Bettmann/Getty ImagesAlthough highly effective, the oral vaccine carries a minimal risk of causing paralytic polio. Due to this risk, the U.S. discontinued its use in 2000, opting exclusively for the inactivated poliovirus vaccine.
New York health officials suspect that the young man from Rockland County, diagnosed with paralytic polio last summer, contracted the virus from an international visitor carrying a vaccine-derived strain. Since he was unvaccinated, his body lacked the necessary defenses to combat the virus.
The CDC states, "Most U.S. adults were vaccinated as children, making them likely protected against polio. Unless there's evidence to the contrary, most U.S.-born adults can assume they received the polio vaccine during childhood. Polio vaccination has been a standard part of the U.S. childhood immunization schedule for decades and remains so today. Adults who received any childhood vaccines in the U.S. were almost certainly vaccinated against polio."
Dr. Forman emphasizes, "These vaccines are exceptionally safe. If you're vaccinated, you're protected. If you're not, there's still time to get vaccinated."
Franklin D. Roosevelt, the 32nd U.S. president, contracted paralytic polio in 1921 at age 39, losing the use of his legs. As president, he prioritized eradicating polio by founding the National Foundation for Infantile Paralysis, later renamed the March of Dimes Foundation. In 1954 — nine years after FDR's death — March of Dimes grantee Jonas Salk, M.D., developed a vaccine that nearly eradicated polio globally.
