 This woman has just undergone a successful skin graft procedure. Her visible pain underscores the fact that while skin grafts offer a remedy, they also bring significant discomfort in treating devastating injuries.
Paula Bronstein/Getty Images
This woman has just undergone a successful skin graft procedure. Her visible pain underscores the fact that while skin grafts offer a remedy, they also bring significant discomfort in treating devastating injuries.
Paula Bronstein/Getty ImagesYour skin, the body's largest organ, is crucial for survival. It does so much – from regulating temperature to maintaining hydration and shielding you from harmful bacteria. A scraped knee might heal on its own, but no amount of natural healing can combat the extreme damage caused by fire.
The agony from a severe burn is unimaginable, and so is the devastation it wreaks on your body. Without skin, your body can't fend off infection, regulate temperature, or retain hydration. This often leads to shock. For many years, the most effective solution for severe burns has been a skin graft.
While skin grafts may sound like an ancient form of torture, they are responsible for saving countless lives each year. Over two million people in the U.S. seek burn treatment annually, with three to four thousand succumbing to their injuries [source: Merck Manual].
To carry out a skin graft, surgeons extract healthy skin from a donor site on the patient’s body and place it over the injured area. While scarring is unavoidable and the recovery process may be slow and painful, most patients survive the procedure and are able to resume their everyday lives.
What kinds of injuries and conditions necessitate a skin graft? How is the procedure performed? And what are the recent advances in artificial skin technology? Keep reading for more information.
Why Skin Grafts Are Needed
A skin graft is recommended when an area of skin is so damaged that it cannot regenerate by itself. Various traumatic injuries, medical conditions, and post-surgical complications may require a skin graft as part of the treatment plan.
Severe burns are among the most frequent injuries treated with skin grafts. While minor first-degree burns, which only affect the outermost layer of skin, usually heal on their own, second-degree burns covering more than 10 percent of the body, or third-degree burns covering more than one percent, are considered severe burns [source: Merck Manual].
Why are these burns so critical? In second-degree burns, the injury penetrates the dermis, the second layer of skin. If the affected area is large, the burn struggles to heal naturally and carries a high risk of infection. A third-degree burn affects all three layers of skin, potentially damaging muscle, cartilage, and even bone. Such severe injuries will almost certainly require a skin graft for proper healing.
Pressure ulcers, also known as bedsores, are a dangerous and persistent issue for those who are bedridden or rely on a wheelchair. These ulcers result from prolonged pressure on certain body parts, cutting off circulation. Common sites for pressure ulcers include the buttocks, hips, lower legs, shoulder blades, and even the head. While some ulcers are shallow, a stage IV ulcer -- the most severe type -- can damage underlying muscle and bone [source: Mayo Clinic].
Certain forms of diabetes can cause loss of sensation in the feet, allowing ulcers to form without the patient’s awareness. These ulcers can become severely infected and may eventually lead to amputation. Diabetic ulcers are the leading cause of non-traumatic foot amputation. Skin grafts, sometimes combined with lab-grown skin substitutes, can assist in covering and healing the wound [source: Scanlan].
Cancer patients often need reconstructive cosmetic surgery to replace skin lost during the removal of cancerous tissue. For instance, breast reconstruction after a mastectomy may require the repositioning of the nipple and areola area with a skin graft. If part of the nose is removed during skin cancer surgery, a skin graft from another body area may be used to reconstruct it.
Various Types of Skin Grafts
 A doctor performs a skin graft procedure on a self-immolation survivor in Afghanistan.
Paula Bronstein/Getty Images
A doctor performs a skin graft procedure on a self-immolation survivor in Afghanistan.
Paula Bronstein/Getty ImagesDuring all skin graft surgeries, healthy skin must be harvested from a donor site and grafted onto the injured area. The best source of donor skin is typically the patient’s own body, a procedure known as an autograft. As the immune system would reject foreign skin, autografts are considered the optimal choice for long-term healing.
In certain situations, a patient may be too ill or injured to undergo an autograft immediately. In these cases, doctors may apply a temporary skin covering to the wounded area to prevent infection and allow time for the patient to recover enough for the full procedure.
When skin is taken from another human, usually a cadaver, it is referred to as an allograft. Allografts typically last between seven and ten days before being rejected by the body [source: WCI]. Xenografts, which are temporary skin coverings from animals, usually pigs, last only three to five days [source: BCM]. In some cases, the injury may not be severe enough to require an autograft, and the allograft or xenograft may offer enough coverage for the skin to heal on its own.
When an autograft is needed, there are three primary types to consider: split-thickness grafts, full-thickness grafts, and composite grafts. The depth of the skin loss is the main factor in determining which type to use. Split-thickness grafts are intended for shallow wounds that affect only the epidermis and part of the dermis, and they involve removing only a few layers of skin from the donor site.
Full-thickness grafts involve the removal of all three layers of skin – the epidermis, dermis, and hypodermis – from the donor site. These grafts are often used when the cosmetic appearance of the injured area is crucial, such as on the face. Full-thickness grafts contain hair follicles, sweat glands, and blood vessels, which help the grafted area look and function more naturally. In contrast, split-thickness grafts, lacking these underlying structures, often appear flat and discolored.
A composite graft is used for wounds that involve bone, tendon, cartilage, or muscle loss. For example, in a nose reconstruction, the surgeon would harvest a composite graft that includes both skin layers and supporting cartilage tissue.
An innovative alternative to autografts is lab-created skin, which we'll discuss further later. For now, let’s dive into the challenging process of skin graft surgery.
Steps in Skin Graft Surgery
For the majority of skin graft surgeries, the patient is placed under general anesthesia. However, if the affected area is particularly small, the doctor may opt for a local anesthetic to numb the area and alleviate pain.
The first step is to debride the wound area. In this process, the surgeon carefully cleans the wound, removing damaged skin and tissue. The surgeon may need to use a scalpel to trim away uneven tissue around the wound's edges. The goal is to create a clean, disinfected, and bleeding surface where the donor skin can be attached.
Next, the surgeon carefully measures the exact size of the wound and traces an identical pattern on the donor site. The donor site can be located anywhere on the body, though areas typically hidden by clothing, such as the lower back, buttocks, or inner thigh, are often chosen [source: Medline Plus].
To remove the precise thickness of skin from the donor site, the surgeon uses a specialized tool called a dermatome. While it may sound unsettling, you can think of a dermatome as a surgical version of a cheese slicer.
To make the most of a small amount of donor skin, doctors may opt to mesh it. This involves running the harvested skin through a rolling device that creates hundreds of tiny holes, similar to an old mimeograph machine. The result is a mesh-like texture, and the surgeon can stretch it to cover a larger area of the wound. The perforated skin also allows fluids to drain from the wound more easily, reducing the risk of infection.
In most procedures, the donor skin is placed over the wound and secured with stitches or surgical staples. For very thin split-thickness grafts, stitches may be avoided, and the graft can be held in place with gauze and dressings. For full-thickness grafts, the area will be covered with an antibiotic solution, multiple layers of mesh gauze, additional bandages, elastic netting, and sometimes a cast.
The donor site will also require treatment. For full-thickness grafts, the donor site will need to be sutured back together. Split-thickness grafts generally only need a generous application of antibiotic ointment and clean dressings to help regenerate the new skin layers.
Healing and Complications of Skin Grafts
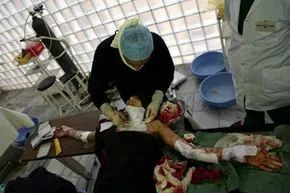 The healing process for a skin graft can take several weeks, depending on both the severity of the wound and the source of the grafted skin.
Paula Bronstein/Getty Images
The healing process for a skin graft can take several weeks, depending on both the severity of the wound and the source of the grafted skin.
Paula Bronstein/Getty ImagesSkin cannot survive without a constant supply of oxygen. The best way to deliver oxygen and other essential nutrients to skin cells is via the bloodstream. Healthy skin is packed with tiny blood vessels that help circulate the body’s blood to nourish and support both new and existing skin cells.
For a skin graft to successfully heal, it must trigger the growth of new blood vessels. In an effective graft, this process of regeneration begins as soon as 36 hours post-surgery [source: Medline Plus].
Given the critical role oxygen plays in the healing process, some doctors recommend hyperbaric oxygen therapy. You might be familiar with a hyperbaric chamber, which resembles a long, glass-walled tube that encases a raised bed. Inside this chamber, the patient breathes pure oxygen at twice the normal atmospheric pressure. These concentrated oxygen bursts can accelerate the healing of skin grafts.
Another treatment method is vacuum-assisted closure (VAC), a post-surgery technique where the grafted area is covered with a porous bandage attached to a vacuum tube. The vacuum helps drain excess fluids and promotes blood circulation to the graft. It also removes any potentially infectious fluids, making disposal easier. Some surgeons are so impressed by its benefits that they leave the VAC tube in place for up to seven days after the surgery without changing the dressing [source: Carson].
The recovery for skin grafts can take time, depending on how severe the wound is, as well as the size and depth of the donor sites. Patients receiving full-thickness grafts may need to remain in the hospital for up to two weeks to ensure the graft stays in place and remains free from infection. On the other hand, those who receive split-thickness grafts might only need a few days of hospitalization.
After returning home, patients must be very cautious with their grafts. They should avoid stretching the skin and refrain from strenuous physical activities for at least a month. Additionally, the donor site will need some weeks to heal as well.
All skin grafts result in scars, both at the donor site and the grafted area. Full-thickness grafts tend to leave less noticeable scars due to their inclusion of functioning blood vessels. In contrast, split-thickness grafts lack sweat glands, hair follicles, and blood vessels, which causes them to be discolored. These grafts require frequent moisturizing to prevent scaling and irritation.
Unfortunately, some skin grafts may become infected in the area where the donor skin meets the wound. Fluid can accumulate beneath the graft, preventing it from properly adhering to the wound. In such cases, the graft is considered a "failure" and must be redone using fresh donor skin.
Artificial Skin Grafts
In severe burn cases, where a significant portion of the body—often 80 to 90 percent—is affected by second- and third-degree burns, there may not be enough healthy donor skin for an autograft. Starting in the late 1970s, medical researchers began experimenting with artificial skin sheets that could be permanently grafted onto patients without any other feasible treatment option.
As discussed in the Mytour.com article, How Lab-grown Skin Works, two surgeons from Boston introduced a groundbreaking artificial skin design in 1981, known as Integra. Interestingly, Integra is not truly "artificial skin." Rather than mimicking the full function of healthy skin, Integra "tricks" living skin cells into growing in the damaged dermis.
Integra acts as an artificial "scaffold" for new skin cells to grow. This scaffold is made from shark cartilage and cow-derived collagen, a protein found in all connective tissue. The bottom layer of the collagen scaffold, which comes into contact with the wound, is coated with a sugar molecule known as glycosaminoglycan. This sticky sugar layer simulates the texture of the lower surface of the dermis [source: NIGMS].
This texture is sufficient to trick certain skin cells, known as fibroblasts, into initiating the production of human collagen. As collagen production increases, the connective tissue gradually climbs up the artificial scaffold, creating a new dermis. Meanwhile, the scaffold dissolves naturally, leaving no trace behind.
Integra does not serve as a replacement for the epidermis. Instead, it features a thin silicon coating that can be peeled away once the dermis has fully regenerated. To restore the epidermis, doctors use lab-grown skin. They take a sample of the patient’s skin and place it in a culture enriched with mouse-derived fibroblasts. Over several weeks, these fibroblasts generate a thin epidermal sheet, which can then be applied to the new dermis.
Recent advancements in artificial skin aim for complete replacements of both the epidermis and dermis, including blood vessels, all produced in the lab. A German company has successfully grown bi-layer skin samples (epidermis and dermis) in the lab, and California researchers have successfully cultivated blood vessels from skin samples [sources: Maugh and ScienceDaily]. Scientists are hopeful that a fully functional, lab-created artificial skin graft will be available soon.
Lot More Information
Related Mytour Articles
- 5 Daily Requirements for Healthy Skin
- 10 Essential Skincare Items You Need Every Day
- Understanding How Lab-Grown Skin Works
- How Face Transplant Procedures Are Performed
- Understanding Bedsores and How They Form
- How to Properly Maintain Your Skin Barrier
- Is Olive Oil Beneficial for Your Skin?
- Is Taking a Daily Shower Too Much for Your Skin?
- Does Taking Daily Aspirin Affect Your Skin Health?
- How Does Weather Impact Your Daily Skincare Routine?
- What Could an "Anti-Aging Molecule" Really Do?
More Useful Resources
- The Massachusetts General Hospital Burn Research Center
- The Johns Hopkins Burn Center
References
- Baylor College of Medicine. "Skin Graft" https://www.thehearthospitalbaylor.com/handler.cfm?event=practice,template&cpid=53325
- Calman, Barney. "The burns victim saved by £60K of 'shark skin.'" The Daily Mail. September 14, 2009 http://www.dailymail.co.uk/health/article-1213003/The-burns-victim-saved-60K-shark-skin.html
- Carson, Stanley N. et al. "Vacuum-Assisted Closure Used for Healing Chronic Wounds and Skin Grafts in the Lower Extremities." Ostomy Wound Management. Volume 50: Issue 3 (October 13, 2009) http://www.o-wm.com/article/2386
- The Massachusetts General Hospital Burn Research Center. "The Development of Artificial Skin" http://www.burnresearchcenter.org/brcpublicwebsite/artificialskin.htm
- Maugh, Thomas H. "Kidney patient's cells used to grow blood vessels in lab." Los Angeles Times. April 25, 2009 http://articles.latimes.com/2009/apr/25/science/sci-kidney25
- Mayo Clinic. "Bedsores (pressure sores)" http://www.mayoclinic.com/health/bedsores/DS00570
- Medline Plus. "Skin graft" http://www.nlm.nih.gov/medlineplus/ency/article/002982.htm
- The Merck Manual Online Medical Library. "Burns" http://www.merck.com/mmhe/sec24/ch289/ch289a.html
- National Institute of General Medical Sciences. "Artificial Skin Fact Sheet" http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3021617/
- Norfolk and Norwich University Hospitals. "Split Thickness Skin Graft." http://www.nnuh.nhs.uk/docs%5Cdocuments%5C37.htm
- Scanlan, Matt. "New skin graft eases diabetic foot ulcers." November 21, 1997 http://www.mc.vanderbilt.edu/reporter/index.html?ID=350
- Science Daily. "Artificial Skin Manufactured in Fully Automated Process." May 19, 2009 http://www.sciencedaily.com/releases/2009/05/090518102959.htm
- Swedish Medical Center. "Skin Graft" http://healthlibrary.epnet.com/GetContent.aspx?token=af362d97-4f80-4453-a175-02cc6220a387&chunkiid=14862
- Indian Journal of Plastic Surgery. "Biologic and Synthetic Skin Substitutes: An overview" http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3038402/
