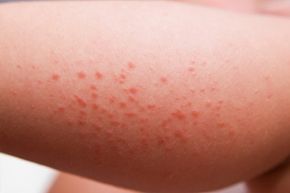
 Sun rash results from an allergic response to sunlight. Explore our image gallery for more insights on achieving radiant skin.
©iStockphoto.com/Karen Mower
Sun rash results from an allergic response to sunlight. Explore our image gallery for more insights on achieving radiant skin.
©iStockphoto.com/Karen MowerIt's widely known that excessive sun exposure is harmful. Beyond painful sunburns, it increases the risk of skin cancer. For some, however, the sun can trigger a different painful issue: sun rash.
Sun rash stems from an allergic reaction to sunlight. The most frequent cause is polymorphous light eruption (PMLE), where rashes form after minimal sun exposure. Other triggers include hereditary PMLE, common among Native Americans, and solar urticaria, a rare condition causing hives, primarily in young women.
Some medications can trigger sun-induced allergic reactions, termed photoallergic reactions. These occur due to the interaction of sunlight with specific components in the drugs. Medications like birth control, antibiotics, and antidepressants are common culprits.
The symptoms of PMLE vary but often include small bumps, redness, and itching. In some cases, burning, blistering, or swelling may also occur. This rash commonly appears on the neck and chest but can also affect the arms and thighs. Additional symptoms may include chills, headaches, and nausea.
PMLE affects approximately 10 to 15 percent of the population, impacting individuals of all racial and ethnic backgrounds [source: Intelihealth]. Symptoms typically recur annually, often in spring or early summer when sun exposure begins.
Continue reading to discover more about sun rash and effective treatment methods.
Sun Rash Causes
Individuals who develop sun rash are photosensitive, meaning they have heightened sensitivity to sunlight. While the exact reason for this sensitivity remains unclear, ultraviolet light is known to trigger the rash [source: Mayo Clinic].
Sunlight consists of three types of ultraviolet (UV) radiation: UVA, UVB, and UVC. UVC rays are irrelevant to sun rash as they don't reach the Earth. UVA rays are the primary cause of PMLE, though some individuals react to UVB rays or a mix of both. Tanning beds, which emit UV radiation, can also provoke allergic reactions in those with PMLE.
For those with PMLE in northern climates, the first sun exposure in spring or early summer often triggers a rash due to prolonged lack of sunlight. Winter vacations to sunny destinations can have the same effect. Fortunately, repeated sun exposure typically reduces UV sensitivity, allowing many PMLE sufferers to enjoy the sun rash-free by summer's end.
PMLE can affect anyone, but common risk factors include being female, under 30, fair-skinned, living in northern regions, or having a family history of the condition [source: Mayo Clinic].
Now that you understand the causes of sun rash, continue reading to explore treatment and prevention strategies.
Hereditary PMLE is a genetic condition predominantly found in Native American families in the Western Hemisphere. Unlike typical PMLE, which lasts two to three days and affects both genders equally, hereditary PMLE can persist throughout the summer and is twice as common in women as in men [source: American Osteopathic College of Dermatology].
Treating Sun Rash
Sun rash typically appears one to two hours after sun exposure. While it often fades within two to three days, it can persist for over a week. Thankfully, these rashes seldom leave lasting scars.
Effective home treatments for sun rash include using cold compresses, applying hydrocortisone cream, taking antihistamines to alleviate allergic reactions, or using anti-inflammatory medications like aspirin or ibuprofen to reduce redness and swelling. If blisters form, cover them with gauze and avoid breaking them [source: Mayo Clinic].
Consult a doctor if the sun rash spreads beyond the neck, chest, arms, or thighs, or if it causes painful blisters or a high fever. Also, seek medical advice if you suspect your medications are causing a photoallergic reaction. A doctor may prescribe stronger antihistamines or suggest hardening, a method that gradually increases your skin's tolerance to sunlight [source: American Osteopathic College of Dermatology]. Phototherapy, involving controlled exposure to artificial UV light, may also be recommended.
After spending hours outdoors, you might find yourself hot, sweaty, and with an unexpected rash. But is it sun rash or heat rash? Heat rash arises when sweat gets trapped under the skin due to blocked sweat glands. Unlike sun rash, heat rash typically appears in skin folds, such as the inner elbows and knees. It primarily affects newborns, individuals in tropical climates, and those who have just finished a strenuous workout [source: Mayo Clinic].
Preventing Sun Rash
For those sensitive to sunlight, avoiding the sun is the best way to prevent sun rash. If sun exposure is unavoidable, take steps to protect yourself from PMLE and other sun allergies. Limit your time in the sun, especially if you've had PMLE before. Consult your doctor about phototherapy or hardening techniques. Gradually increase your sun exposure in spring and early summer, and avoid being outdoors between 10 a.m. and 4 p.m., when the sun is strongest [source: American Osteopathic College of Dermatology].
When outdoors during peak sun hours, wear lightweight clothing that covers most of your skin. Use sunscreen with an SPF of at least 15, reapplying every two hours and after swimming or sweating. Choose a sunscreen that blocks both UVA and UVB rays, and don’t forget to apply it on cloudy days. Protect your eyes with sunglasses and use lip balm containing SPF to shield against UV damage.
Even if you don’t have a sun allergy, following these preventive measures can safeguard your skin from harmful UV rays while still letting you enjoy the sunshine.
Broad-spectrum sunscreens offer protection against both UVA and UVB rays and include active ingredients like oxybenzone, sulisobenzone, dioxybenzone, avobenzone, zinc oxide, titanium dioxide, and menthyl anthranilate [source: AAD].
